Abstract
Background
There is no clear consensus on the optimal type of fixation in intercalary allograft reconstruction. In this study, we aimed to compare the rate of most common complications following the plate and nail fixation of the intercalary allograft.
Materials and Methods
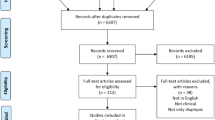
We searched PubMed, EMBASE, Web of Science, Scopus, and Cochrane Library. Studies in which the complication rate of the single bridging plate and intramedullary nail fixation was extractable were included. Studies that used extra procedures such as cementation and fibular vascular graft augmentation were excluded. The primary outcome was the fixation-specific rate of nonunion. Secondary outcomes were the fixation-specific rate of fracture, infection, and local recurrence.
Results
In total, 13 studies with 431 reconstructions (352 reconstructions in the plate group and 79 reconstructions in the intramedullary nailing group) were included in this study. In the plate fixation, the rate of nonunion, fracture, infection and local recurrence was 12%, 11%, 11%, and 3%, respectively. In the intramedullary nail fixation, the rate of nonunion, fracture, infection, and local recurrence was 37%, 5%, 4%, and 0%, respectively. The rate of nonunion was significantly higher in the intramedullary nail group (OR = 6.34; 95% CI 2.98–13.49, P < 0.001). The rate of fracture, infection, and local recurrence was not significantly different between the two fixation methods.
Conclusions
Intramedullary nail is associated with a significantly higher rate of nonunion. Since the rate of other complications was not significantly different between the two osteosynthesis types, plate fixation could be considered as a better type of fixation.








Similar content being viewed by others
References
Bielack, S. S., Kempf-Bielack, B., Gn, D., Exner, G. U., Flege, S., Helmke, K., et al. (2002). Prognostic factors in high-grade osteosarcoma of the extremities or trunk: an analysis of 1702 patients treated on neoadjuvant cooperative osteosarcoma study group protocols. Journal Clinical Oncology, 20(3), 776–790.
Panagopoulos, G. N., Mavrogenis, A. F., Mauffrey, C., Lesenský, J., Angelini, A., Megaloikonomos, P. D., et al. (2017). Intercalary reconstructions after bone tumor resections: A review of treatments. European Journal of Orthopaedic Surgery & Traumatology, 27(6), 737–746.
Virkus W, Henshaw RM, Miller B, Girelis S (2014) Use of allografts and segmental prostheses for reconstruction of segmental bone defects Operative Technique in Orthopaedic Surgical Oncology 1st ed Philadelphia. Lippincott Williams and Wilkins 2012: 288–305.
Houdek, M., Bayne, C., Bishop, A., & Shin, A. (2017). The outcome and complications of vascularised fibular grafts. Bone Joint J., 99(1), 134–138.
Emori, M., Kaya, M., Irifune, H., Takahashi, N., Shimizu, J., Mizushima, E., et al. (2017). Vascularised fibular grafts for reconstruction of extremity bone defects after resection of bone and soft-tissue tumours: A single institutional study of 49 patients. Bone Joint J., 99(9), 1237–1243.
Capanna, R., Campanacci, D. A., Belot, N., Beltrami, G., Manfrini, M., Innocenti, M., et al. (2007). A new reconstructive technique for intercalary defects of long bones: the association of massive allograft with vascularized fibular autograft. Long-term results and comparison with alternative techniques. Orthopedic Clinics of North America, 38(1), 51–60.
Ruggieri, P., Mavrogenis, A. F., Bianchi, G., Sakellariou, V. I., Mercuri, M., & Papagelopoulos, P. J. (2011). Outcome of the intramedullary diaphyseal segmental defect fixation system for bone tumors. Journal of Surgical Oncology, 104(1), 83–90.
Ahlmann, E., & Menendez, L. (2006). Intercalary endoprosthetic reconstruction for diaphyseal bone tumours. Journal of Bone and Joint Surgery. British Volume, 88(11), 1487–1491.
Khattak, M. J., Umer, M., & Umar, M. (2006). Autoclaved tumor bone for reconstruction: An alternative in developing countries. Clinical Orthopaedics and Related Research, 447, 138–144.
Sabo, D., Brocai, D., Eble, M., Wannenmacher, M., & Ewerbeck, V. (2000). Influence of extracorporeal irradiation on the reintegration of autologous grafts of bone and joint: Study in a canine model. Journal of Bone and Joint Surgery. British Volume, 82(2), 276–282.
Tsuchiya, H., Abdel-Wanis, M., Sakurakichi, K., Yamashiro, T., & Tomita, K. (2002). Osteosarcoma around the knee: Intraepiphyseal excision and biological reconstruction with distraction osteogenesis. Journal of Bone and Joint Surgery. British Volume, 84(8), 1162–1166.
Fuchs, B., Ossendorf, C., Leerapun, T., & Sim, F. (2008). Intercalary segmental reconstruction after bone tumor resection. European Journal of Surgical Oncology, 34(12), 1271–1276.
Liberati, A., Altman, D. G., Tetzlaff, J., Mulrow, C., Gøtzsche, P. C., Ioannidis, J. P., et al. (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. Journal of Clinical Epidemiology, 62(10), e1–e34.
Gupta, S., Kafchinski, L., Gundle, K., Saidi, K., Griffin, A., Wunder, J., et al. (2017). Intercalary allograft augmented with intramedullary cement and plate fixation is a reliable solution after resection of a diaphyseal tumour. Bone Joint J., 99(7), 973–978.
Chang, D. W., & Weber, K. L. (2005). Use of a vascularized fibula bone flap and intercalary allograft for diaphyseal reconstruction after resection of primary extremity bone sarcomas. Plast Reconstruc Surgery, 116(7), 1918–1925.
Bus, M., Dijkstra, P., Van de Sande, M., Taminiau, A., Schreuder, H., Jutte, P., et al. (2014). Intercalary allograft reconstructions following resection of primary bone tumors: a nationwide multicenter study. J Bone Joint Surgery., 96(4), e26.
Deijkers, R. L., Bloem, R., Kroon, H., Van Lent, J., Brand, R., & Taminiau, A. H. (2005). Epidiaphyseal versus other intercalary allografts for tumors of the lower limb. Clinical Orthopaedics and Related Research, 439, 151–160.
Slim, K., Nini, E., Forestier, D., Kwiatkowski, F., Panis, Y., & Chipponi, J. (2003). Methodological index for non-randomized studies (minors): Development and validation of a new instrument. ANZ Journal of Surgery, 73(9), 712–716.
Soler, F., Mocini, F., Djemeto, D. T., Cattaneo, S., Saccomanno, M. F., & Milano, G. (2021). No differences between conservative and surgical management of acromioclavicular joint osteoarthritis: A scoping review. Knee Surgery, Sports Traumatology, Arthroscopy, 29(7), 2194–2201.
Aponte-Tinao, L., Farfalli, G. L., Ritacco, L. E., Ayerza, M. A., & Muscolo, D. L. (2012). Intercalary femur allografts are an acceptable alternative after tumor resection. Clinical Orthopaedics and Related Research, 470(3), 728–734.
Muscolo, D. L., Ayerza, M. A., Aponte-Tinao, L., Ranalletta, M., & Abalo, E. (2004). Intercalary femur and tibia segmental allografts provide an acceptable alternative in reconstructing tumor resections. Clinical Orthopaedics and Related Research, 426, 97–102.
Brunet, O., Anract, P., Bouabid, S., Babinet, A., Dumaine, V., Toméno, B., et al. (2011). Intercalary defects reconstruction of the femur and tibia after primary malignant bone tumour resection A series of 13 cases. Orthopaedics & Traumatology, Surgery & Research, 97(5), 512–519.
Farfalli, G. L., Aponte-Tinao, L., Lopez-Millán, L., Ayerza, M. A., & Muscolo, D. L. (2012). Clinical and functional outcomes of tibial intercalary allografts after tumor resection. Orthopedics, 35(3), e391–e396.
Frisoni, T., Cevolani, L., Giorgini, A., Dozza, B., & Donati, D. (2012). Factors affecting outcome of massive intercalary bone allografts in the treatment of tumours of the femur. Journal of Bone and Joint Surgery. British Volume, 94(6), 836–841.
Han, G., Wang, Y., Bi, W., Jia, J., Wang, W., Xu, M., et al. (2015). Reconstruction using massive allografts after resection of extremity osteosarcomas the study design: A retrospective cohort study. International Journal of Surgery, 21, 108–111.
Brien, E. W., Terek, R. M., Healey, J. H., & Lane, J. M. (1994). Allograft reconstruction after proximal tibial resection for bone tumors An analysis of function and outcome comparing allograft and prosthetic reconstructions. Clinical Orthopaedics and Related Research, 303, 116–127.
Giannini, C., Sambri, A., Dalla Rosa, M., Zucchini, R., Bochiccio, V., Fiore, M., et al. (2020). Intercalary bone graft of the tibia: Case series and review of the literature. European Journal of Orthopaedic Surgery & Traumatology, 30(8), 1421–1427.
Voggenreiter, G., Klaes, W., Assenmacher, S., & Schmit-Neuerburg, K. (1995). Massive intercalary bone allografts in the treatment of primary and secondary bone tumors. Archives of Orthopaedic and Trauma Surgery, 114(6), 308–318.
Erol, B., Basci, O., Topkar, M. O., Caypinar, B., Basar, H., & Tetik, C. (2015). Mid-term radiological and functional results of biological reconstructions of extremity-located bone sarcomas in children and young adults. Journal of Pediatric Orthopedics. Part B, 24(5), 469–478.
Gebhardt, M. C., Lord, F., Rosenberg, A., & Mankin, H. (1987). The treatment of adamantinoma of the tibia by wide resection and allograft bone transplantation. Journal of Bone and Joint Surgery. American Volume, 69(8), 1177–1188.
Sanders, P., Spierings, J., Albergo, J., Bus, M., Fiocco, M., Farfalli, G., et al. (2020). Long-term clinical outcomes of intercalary allograft reconstruction for lower-extremity bone tumors. Journal of Bone and Joint Surgery. American Volume, 102(12), 1042–1049.
Ortiz-Cruz, E., Gebhardt, M. C., Jennings, L. C., Springfield, D. S., & Mankin, H. J. (1997). The results of transplantation of intercalary allografts after resection of tumors. A long-term follow-up study. Journal Bone Joint Surgery, 79(1), 97–106.
Jamshidi, K., Shirazi, M. R., Bagherifard, A., & Mirzaei, A. (2019). Curettage, phenolization, and cementation in paediatric Ewing’s sarcoma with a complete radiological response to neoadjuvant chemotherapy. International Orthopaedics, 43(2), 467–473.
Jamshidi, K., Mirkazemi, M., Gharedaghi, M., Izanloo, A., Mohammadpour, M., Pisoudeh, K., et al. (2020). Bipolar hemiarthroplasty versus total hip arthroplasty in allograft-prosthesis composite reconstruction of the proximal femur following primary bone tumour resection. Bone Joint Journal, 102(4), 524–529.
Jamshidi, K., Zandrahimi, F., Bozorgi, M. H. A., Arefpour, A. M., Bagherifard, A., Al-Baseesee, H. H., et al. (2021). Extended curettage versus en bloc resection for the treatment of grade 3 giant cell tumour of the knee with pathologic fracture: A retrospective study. International Orthopaedics, 45(1), 289–297.
Jamshidi, K., Najd-Mazhar, F., & Ahangar, F. A. (2017). The effect of cement augmentation and anteromedial plating on proximal humerus allograft reconstruction. Journal of Orthopaedic Science, 22(1), 69–74.
McNamara, E. R., & Scales, C. D., Jr. (2011). Role of systematic reviews and meta-analysis in evidence-based clinical practice. Indian Journal of Urology, 27(4), 520.
Hornicek, F., Jr., Mnaymneh, W., Lackman, R., Exner, G., & Malinin, T. (1998). Limb salvage with osteoarticular allografts after resection of proximal tibia bone tumors. Clinical Orthopaedics and Related Research, 352, 179–186.
Donati, D., Di Liddo, M., Zavatta, M., Manfrini, M., Bacci, G., Picci, P., et al. (2000). Massive bone allograft reconstruction in high-grade osteosarcoma. Clinical Orthopaedics and Related Research, 377, 186–194.
San-Julian, M., & Canadell, J. (1998). Fractures of allografts used in limb preserving operations. International Orthopaedics, 22(1), 32–36.
Enneking, W. F., & Campanacci, D. A. (2001). Retrieved human allografts : A clinicopathological study. Journal of Bone and Joint Surgery. American Volume, 83(7), 971–986.
Hu, L., Xiong, Y., Mi, B., Panayi, A. C., Zhou, W., Liu, Y., et al. (2019). Comparison of intramedullary nailing and plate fixation in distal tibial fractures with metaphyseal damage: A meta-analysis of randomized controlled trials. Journal of Orthopaedic Surgery and Research, 14(1), 1–11.
Vallier, H. A., Cureton, B. A., & Patterson, B. M. (2011). Randomized, prospective comparison of plate versus intramedullary nail fixation for distal tibia shaft fractures. Journal of Orthopaedic Trauma, 25(12), 736–741.
Vallier, H. A. (2016). Current evidence: Plate versus intramedullary nail for fixation of distal tibia fractures in 2016. Journal of Orthopaedic Trauma, 30, S2–S6.
Wang, J., Yang, Y., Yang, R., Tang, X., & Guo, W. (2019). Does intramedullary nailing improve the union rate or decrease mechanical complications for patients with extremity sarcoma after biological reconstruction? Injury, 50(3), 777–783.
Zekry, K. M., Yamamoto, N., Hayashi, K., Takeuchi, A., Alkhooly, A. Z. A., Abd-Elfattah, A. S., et al. (2019). Reconstruction of intercalary bone defect after resection of malignant bone tumor. Journal of Orthopaedic Surgery, 27(1), 2309499019832970.
Enneking, W. F., & Campanacci, D. A. (2001). Retrieved human allografts: A clinicopathological study. Journal of Bone and Joint Surgery. American Volume, 83(7), 971–986.
Enneking, W., & Mindell, E. (1991). Observations on massive retrieved human allografts. Journal of Bone and Joint Surgery. American Volume, 73(8), 1123–1142.
Kowalczyk, B., Miklaszewski, K., & Felus, J. (2017). Spontaneous healing of fractures and osteotomy within intercalary allograft reconstruction after distal femur osteosarcoma resection in a child. Journal of Pediatric Orthopedics. Part B, 26(6), 570–574.
Funding
None.
Author information
Authors and Affiliations
Contributions
KJ, Study design and supervision; MB, Data analysis; AKB, Data analysis; AB, Reviewing the manuscript critically; AM, Study design and drafting the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
Manuscript has been read and approved by all the authors, represents honest work, and not been submitted elsewhere.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jamshidi, K., Bahardoust, M., Karimi Behnagh, A. et al. How the Choice of Osteosynthesis Affects the Complication Rate of Intercalary Allograft Reconstruction? A Systematic Review and Meta-analysis. JOIO 56, 547–558 (2022). https://doi.org/10.1007/s43465-021-00563-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-021-00563-7