Abstract
Introduction
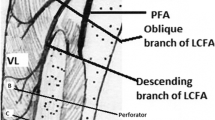
Soft tissue defects due to trauma with crush injuries and post-tumor excision are large in size. Free anterolateral flap provides a stable and durable coverage of soft tissue defects and leads to good functional outcomes.
Materials and Methods
Between January 2017 and January 2019, eight males and six female patients with soft tissue defects were operated upon using a free anterolateral thigh flaps. The defects in ten patients were due to post-tumor extirpation and in four patients due to wound breakdown following post-tumor extirpation.
Results
The average flap dimension was 14 cm × 12 cm. The mean follow-up was 11 months (4–28 months). All the flaps survived well except in one patient who with an upper limb defect, had flap necrosis owing to which patient needed to undergo abdominal flap coverage. Two patients with sarcoma developed local recurrence and had to undergo above‑knee amputation.
Conclusion
The method of reconstruction depends on the size of defect and area to be covered and need of post-surgery mobilization and need for radiotherapy. The free anterolateral thigh flap has varied uses in orthopedics with very good extent of coverage and provides very potent coverage of neurovascular structures, bones, tendons, and implants.













Similar content being viewed by others
References
Song, Y. G., Chen, G. Z., & Song, Y. L. (1984). The free thigh flap: A new free flap concept based on the septocutaneous artery. British Journal of Plastic Surgery, 37(2), 149–159.
Kimata, Y., Uchiyama, K., Ebihara, S., et al. (1997). Versatility of the free anterolateral thigh flap for reconstruction of head and neck defects. Archives of Otolaryngology - Head and Neck Surgery, 123(12), 1325–1331.
Lee, Y.-C., Chiu, H.-Y., & Shieh, S.-J. (2011). The clinical application of anterolateral thigh flap. Plastic Surgery International, 2011, 127353.
Xu, A.C., Koshima, I. (1996). The Anterolateral thigh flap. In: Saunders, W.B. (ed) Donald Serafin’s Atlas of Microsurgical composite tissue transplantation (1st edn, pp. 421–432). London: Elsevier Health Sciences.
Begue, T., & Masquelet, A. C. (2009). Anterolateral thigh flap. In: Grabb’s Encyclopedia of Flaps (3rd ed., pp. 1495–1497). Philadelphia: Lippincott Williams & Wilkins.
Agostini, T., Lazerri, D., & Spinelli, G. (2014). Anterolateral thigh flap thinning. Techniques and complications. Annals of Plastic Surgery, 72(2), 246–252.
Barclay, T. L., Cardoso, E., & Sharpe, D. T. (1983). Cross leg fasciocutaneous flaps. Plastic Reconstructive Surgery, 72, 847.
Wettstein, R., Schurch, R., Banic, A., Erni, D., & Harder, Y. (2008). Review of 197 consecutive free flaps in the lower extremity. Journal of Plastic, Reconstructive and Aesthetic Surgery, 61(7), 772–776.
Agarwal, P., & Raza, H. K. T. (2008). Cross Leg Flap: Its role in salvage. Indian Journal of Orthopaedics, 42(4), 439–443.
Krishnamoorthy, R., & Karthikeyan, G. (2011). Degloving injuries of the hand. Indian Journal of Plastic Surgery., 4(2), 227–236.
Pai, V., Puri, A., Epali, S., & Gulia, A. (2015). Iatrogenic implantation of soft tissue sarcoma at skin graft donor site: Delayed manifestation of an avoidable complication. South Asian Journal of Cancer, 4(2), 100–101.
Demirtas, Y., Kehlametoglu, O., & Cifci, M. (2010). Comparison of free anterolateral thigh flaps and free muscle-musculocutaneous flaps in soft tissue reconstruction of lower extremity. Microsurgery, 30(1), 24–31.
Gedebou, T. M., Wei, F. C., & Lin, C. H. (2002). Clinical experience of 1284 free anterolateral thigh flaps. Handchirurgie Mikrochirurgie Plastische Chirurgie, 34(4), 239–244.
Özkan, Ö., Coskunfirat, O. K., & Özgentas, H. E. (2004). The use of free anterolateral thigh flap for reconstructing soft tissue defects of the lower extremities. Annals of Plastic Surgery, 53(5), 455–461.
Keshk, T. F., El Kashty, S. M., Taalab, A. A., & El-Nahas, M. A. (2018). Reconstruction of complex soft tissue defects in the lower extremities with free anterolateral thigh perforator flap. Menoufia Medical Journal, 31(4), 1386.
Demirtas, Y., Kelahmetoglu, O., Cifci, M., Tayfur, V., Demir, A., & Guneren, E. (2010). Comparison of free anterolateral thigh flaps and free muscle-musculocutaneous flaps in soft tissue reconstruction of lower extremity. Microsurgery: Official Journal of the International Microsurgical Society and the European Federation of Societies for Microsurgery, 30(1), 24–31.
Diamond, S., et al. (2018). Outcomes of subfascial, suprafascial, and super-thin anterolateral thigh flaps: Tailoring thickness without added morbidity. Journal of Reconstructive Microsurgery, 34(3), 176–184.
Seth, A. K., & Iorio, M. L. (2017). Super-thin and suprafascial anterolateral thigh perforator flaps for extremity reconstruction. Journal of Reconstructive Microsurgery, 33(7), 466–473.
Townley, W. A., Royston, E. C., & Karmiris, N. (2011). Critical assessment of the anterolateral thigh flap donor site. Journal of Plastic, Reconstructive and Aesthetic Surgery, 64(12), 1621–1626.
Addison, P. D., Lannon, D., & Neligan, P. C. (2008). Compartment syndrome after closure of the anterolateral thigh flap donor site: A report of two cases. Annals of Plastic Surgery, 60(6), 635–638.
Rodriguez, E. D., et al. (2007). Does fascia lata repair facilitate closure and does it affect compartment pressures of the anterolateral thigh flap donor site? Plastic and Reconstructive Surgery, 120(5), 1300–1304.
Agostini, T., Lazzeri, D., & Spinelli, G. (2013). Anterolateral thigh flap: Systematic literature review of specific donor-site complications and their management. Journal of Cranio-Maxillofacial Surgery, 41(1), 15–21.
Pisters, P. W., Leung, D. H., Woodruff, J., Shi, W., & Brennan, M. F. (1996). Analysis of prognostic factors in 1041 patients with localized soft tissue sarcomas of the extremities. Journal of Clinical Oncology, 14, 1679.
American Joint Committee on Cancer. (2010). Soft tissues. In I. D. Fleming, J. S. Cooper, & D. E. Henson (Eds.), AJCC cancer staging manual. 7 (pp. 149–156). Philadelphia: Lippincott-Raven.
Lehnardt, M., Kuhnen, C., Drücke, D., Homann, H. H., Joneidi Jafari, H., & Steinau, H. U. (2004). Liposarcoma of the extremities: Recent developments in surgical therapy/analysis of 167 patients. Chirurg, 75(12), 1182–1190. https://doi.org/10.1007/s00104-004-0900-2.
López, J. F., Hietanen, K. E., Kaartinen, I. S., Kääriäinen, M. T., Pakarinen, T. K., Laitinen, M., et al. (2015). Primary flap reconstruction of tissue defects after sarcoma surgery enables curative treatment with acceptable functional results: a 7-year review. BMC Surgery, 15(1), 71.
Ng, R. W., Chan, J. Y., & Mok, V. (2008). A modification of technique to cover a large posterior thigh defect using an anterolateral thigh flap. Annals of Plastic Surgery, 61, 201–203.
Radtke, C., Panzica, M., Dastagir, K., Krettek, C., & Vogt, P. M. (2015). Soft tissue coverage of the lower limb following oncological surgery. Frontiers in Oncology, 5, 303. https://doi.org/10.3389/fonc.2015.00303.
Azadgoli, B., Carre, A. L., Perrault, D. P., & Wong, A. K. (2018). Complex reconstruction of the lower extremity following sarcoma resection: a literature review. Plastic and Aesthetic Research, 5, 3. https://doi.org/10.20517/2347-9264.2017.32.
Funding
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Standard Statement
This article does not contain any studies with human or animal subjects performed by the any of the authors.
Informed Consent
For this type of study informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sahijwani, H., Salunke, A.A., Warikoo, V. et al. Use of Free Anterolateral Thigh Flap in Reconstruction of Soft Tissue Defects in Orthopedic Oncology: What are the Outcomes?. JOIO 55 (Suppl 1), 246–255 (2021). https://doi.org/10.1007/s43465-020-00208-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-020-00208-1