Abstract
Aconite and cinnamon can treat many diseases. The study aimed to assess the effectiveness and mechanism of aconite, cinnamon, and aconite-cinnamon in bone formation-bone resorption. The co-culture system was treated with serum containing aconite, cinnamon, and aconite-cinnamon, and the effects on osteoblast and osteoclast differentiation were evaluated through ALP activity, ALP staining, alizarin red staining, TRAP activity detection, TRAP staining, and F-actin staining. The study also examined the effects of aconite-cinnamon on intercellular factors using ELISA kits, and the effects on different genes were detected through RT-qPCR and Western blotting. Results showed that aconite-cinnamon improved osteoblast differentiation and activity, reduced the release of RANKL, inhibited osteoclast differentiation and activity, and activated the AMPK/SIRT1 signaling pathway in both osteoblasts and osteoclasts. Therefore, aconite-cinnamon can improve osteogenic differentiation activity and reducing osteoclast differentiation and activity, while activating the AMPK/SIRT1 signaling pathway in both osteoblasts and osteoclasts.
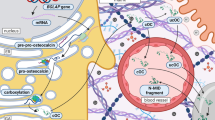
Graphical Abstract






Similar content being viewed by others
Data Availability
All data generated or analyzed during this study are included in this published article. The datasets used and/or analyzed during the present study are available from the corresponding author on reasonable request.
References
Borciani G, Montalbano G, Baldini N, Cerqueni G, Vitale-Brovarone C, Ciapetti G (2020) Co-culture systems of osteoblasts and osteoclasts: simulating in vitro bone remodeling in regenerative approaches. Acta Biomater 108:22–45. https://doi.org/10.1016/j.actbio.2020.03.043
Boyce BF, Xing L (2007) Biology of RANK, RANKL, and osteoprotegerin. Arthritis Res Ther 9(Suppl 1):S1. https://doi.org/10.1186/ar2165
Chen YH, Hsueh KK, Chu PW, Chen SK (2022) AMP-activated protein kinase mediates lipopolysaccharide-induced proinflammatory responses and elevated bone resorption in differentiated osteoclasts. J Cell Biochem 123:275–288. https://doi.org/10.1002/jcb.30165
Darnay BG, Besse A, Poblenz AT, Lamothe B, Jacoby JJ (2007) TRAFs in RANK signaling. Adv Exp Med Biol 597:152–159. https://doi.org/10.1007/978-0-387-70630-6_12
Demontiero O, Vidal C, Duque G (2012) Aging and bone loss: new insights for the clinician. Ther Adv Musculoskelet Dis 4:61–76. https://doi.org/10.1177/1759720X11430858
Fukuyasu S, Kayashima H, Moribayashi A, Matsuoka S, Nagasaki A, Okawa H, Yatani H, Saeki M, Egusa H (2022) Cell-based double-screening method to identify a reliable candidate for osteogenesis-targeting compounds. Biomedicines 10:426. https://doi.org/10.3390/biomedicines10020426
Garcia D, Shaw RJ (2017) AMPK: mechanisms of cellular energy sensing and restoration of metabolic balance. Mol Cell 66:789–800. https://doi.org/10.1016/j.molcel.2017.05.032
Gruenwald J, Freder J, Armbruester N (2010) Cinnamon and health. Crit Rev Food Sci Nutr 50:822–834. https://doi.org/10.1080/10408390902773052
Guo J, Zeng X, Miao J, Liu C, Wei F, Liu D, Zheng Z, Ting K, Wang C, Liu Y (2019) MiRNA-218 regulates osteoclast differentiation and inflammation response in periodontitis rats through Mmp9. Cell Microbiol 21:e12979. https://doi.org/10.1111/cmi.12979
Hapidin H, Hashim NM, Kasiram MZ, Abdullah H (2022) The effects of polyphenol, tannic acid, or tannic acid in combination with pamidronate on human osteoblast cell line metabolism. Molecules 27:451. https://doi.org/10.3390/molecules27020451
He J, Li X, Wang Z, Bennett S, Chen K, Xiao Z, Zhan J, Chen S, Hou Y, Chen J, Wang S, Xu J, Lin D (2019) Therapeutic anabolic and anticatabolic benefits of natural Chinese Medicines for the treatment of osteoporosis. Front Pharmacol 10:1344. https://doi.org/10.3389/fphar.2019.01344
Hsiao YM, Hu CC, Chen MF, Chang CH, Chiu YT, Chang Y (2021) Serum insufficiency induces RANKL-independent osteoclast formation during developing ischemic ONFH. Biomedicines 9:685. https://doi.org/10.3390/biomedicines9060685
Hwang SY, Putney JW (2012) Orai1-mediated calcium entry plays a critical role in osteoclast differentiation and function by regulating activation of the transcription factor NFATc1. FASEB J 26:1484–1492. https://doi.org/10.1096/fj.11-194399
Jann J, Gascon S, Roux S, Faucheux N (2020) Influence of the TGF-β superfamily on osteoclasts/osteoblasts balance in physiological and pathological bone conditions. Int J Mol Sci 21:7597. https://doi.org/10.3390/ijms21207597
Kim DY, Kim EJ, Jang WG (2018) Piperine induces osteoblast differentiation through AMPK-dependent Runx2 expression. Biochem Biophys Res Commun 495:1497–1502. https://doi.org/10.1016/j.bbrc.2017.11.200
Kim JM, Lin C, Stavre Z, Greenblatt MB, Shim JH (2020) Osteoblast-steoclast communication and bone homeostasis. Cells 9:2073. https://doi.org/10.3390/cells9092073
Komori T (2019) Regulation of proliferation, differentiation and functions of osteoblasts by Runx2. Int J Mol Sci 20:1694. https://doi.org/10.3390/ijms20071694
Lagouge M, Argmann C, Gerhart-Hines Z, Meziane H, Lerin C, Daussin F, Messadeq N, Milne J, Lambert P, Elliott P, Geny B, Laakso M, Puigserver P, Auwerx J (2006) Resveratrol improves mitochondrial function and protects against metabolic disease by activating SIRT1 and PGC-1alpha. Cell 127:1109–1122. https://doi.org/10.1016/j.cell.2006.11.013
Lewiecki EM (2018) New and emerging concepts in the use of denosumab for the treatment of osteoporosis. Ther Adv Musculoskelet Dis 10:209–223. https://doi.org/10.1177/1759720X18805759
Lim HJ, Park EJ, Won YS, Bak SG, Cheong SH, Lee SW, Lee S, Lee SJ, Rho MC (2021) Anti-osteoporotic effects of n-trans-hibiscusamide and its derivative alleviate ovariectomy-induced bone loss in mice by regulating RANKL-induced signaling. Molecules 26:6820. https://doi.org/10.3390/molecules26226820
Liu T, Gao Y, Sakamoto K, Minamizato T, Furukawa K, Tsukazaki T, Shibata Y, Bessho K, Komori T, Yamaguchi A (2007) BMP-2 promotes differentiation of osteoblasts and chondroblasts in Runx2-deficient cell lines. J Cell Physiol 211:728–735. https://doi.org/10.1002/jcp.20988
Macías I, Alcorta-Sevillano N, Rodríguez CI, Infante A (2020) Osteoporosis and the potential of cell-based therapeutic strategies. Int J Mol Sci 21:1653. https://doi.org/10.3390/ijms21051653
Ma J, Wang Z, Zhao J, Miao W, Ye T, Chen A (2018) Resveratrol attenuates lipopolysaccharides (LPS)-induced inhibition of osteoblast differentiation in MC3T3-E1 Cells Med Sci Monitor 24:2045–2052. https://doi.org/10.12659/msm.905703
Marycz K, Turlej E, Kornicka-Garbowska K, Zachanowicz E, Tomaszewska A, Kulpa-Greszta M, Pązik R (2021) Co0.5Mn0.5Fe2O4@PMMA nanoparticles promotes preosteoblast differentiation through activation of OPN-BGLAP2-DMP1 axis and modulates osteoclastogenesis under magnetic field conditions. Materials 14:5010. https://doi.org/10.3390/ma14175010
Nyirimigabo E, Xu Y, Li Y, Wang Y, Agyemang K, Zhang Y (2015) A review on phytochemistry, pharmacology and toxicology studies of Aconitum. J Pharm Pharmacol 67:1–19. https://doi.org/10.1111/jphp.12310
Ping Z, Wang Z, Shi J, Wang L, Guo X, Zhou W, Hu X, Wu X, Liu Y, Zhang W, Yang H, Xu Y, Gu Y, Geng D (2017) Inhibitory effects of melatonin on titanium particle-induced inflammatory bone resorption and osteoclastogenesis via suppression of NF-κB signaling. Acta Biomater 62:362–371. https://doi.org/10.1016/j.actbio.2017.08.046
Soltanoff CS, Yang S, Chen W, Li YP (2009) Signaling networks that control the lineage commitment and differentiation of bone cells. In: Stein GS, Stein JL, Lian JB (eds) Crit Rev Eukaryot Gene Expr 19:1–46. https://doi.org/10.1615/critreveukargeneexpr.v19.i1.10
Takayanagi H (2007) The role of NFAT in osteoclast formation. Ann N Y Acad Sci 1116:227–237. https://doi.org/10.1196/annals.1402.071
Wang MY, Shen C, An MF, Xie CQ, Wu X, Zhu QQ, Sun B, Huang YP, Zhao YL, Wang XJ, Sheng J (2018) Combined treatment with Dendrobium candidum and black tea extract promotes osteoprotective activity in ovariectomized estrogen deficient rats and osteoclast formation. Life Sci 200:31–41. https://doi.org/10.1016/j.lfs.2018.03.025
Wang Q, Xie X, Zhang D, Mao F, Wang S, Liao Y (2022) Saxagliptin enhances osteogenic differentiation in MC3T3-E1 cells, dependent on the activation of AMP-activated protein kinase α (AMPKα)/runt-related transcription factor-2 (Runx-2). Bioengineered 13:431–439. https://doi.org/10.1080/21655979.2021.2008667
Wang T, Liu Q, Tjhioe W, Zhao J, Lu A, Zhang G, Tan RX, Zhou M, Xu J, Feng HT (2017) Therapeutic potential and outlook of alternative medicine for osteoporosis. Curr Drug Targets 18:1051–1068. https://doi.org/10.2174/1389450118666170321105425
Watanabe A, Kumagai M, Mishima T, Ito J, Otoki Y, Harada T, Kato T, Yoshida M, Suzuki M, Yoshida I, Fujita K, Watai M, Nakagawa K, Miyazawa T (2015) Toddaculin, isolated from of Toddalia asiatica (L.) Lam., inhibited osteoclastogenesis in RAW 264 cells and enhanced osteoblastogenesis in MC3T3-E1 cells. PLoS ONE 10:e0127158. https://doi.org/10.1371/journal.pone.0127158
Xiong J, Cawley K, Piemontese M, Fujiwara Y, Zhao H, Goellner JJ, O’Brien CA (2018) Soluble RANKL contributes to osteoclast formation in adult mice but not ovariectomy-induced bone loss. Nat Commun 9:2909. https://doi.org/10.1038/s41467-018-05244-y
Xu G, Hu X, Han L, Zhao Y, Li Z (2021) The construction of a novel xenograft bovine bone scaffold, (DSS)6-liposome/CKIP-1 siRNA/calcine bone and its osteogenesis evaluation on skull defect in rats. J Orthop Translat 28:74–82. https://doi.org/10.1016/j.jot.2021.02.001
Yao Z, Getting SJ, Locke IC (2021) Regulation of TNF-induced osteoclast differentiation. Cells 11:132. https://doi.org/10.3390/cells11010132
Yan J, Herzog JW, Tsang K, Brennan CA, Bower MA, Garrett WS, Sartor BR, Aliprantis AO, Charles JF (2016) Gut microbiota induce IGF-1 and promote bone formation and growth. Proc Natl Acad Sci USA 113:E7554–E7563. https://doi.org/10.1073/pnas.1607235113
Zainabadi K, Liu CJ, Caldwell ALM, Guarente L (2017) SIRT1 is a positive regulator of in vivo bone mass and a therapeutic target for osteoporosis. PLoS ONE 12:e0185236. https://doi.org/10.1371/journal.pone.0185236
Zeng Z, Fei L, Yang J, Zuo J, Huang Z, Li H (2022) MiR-27a-3p targets GLP1R to regulate differentiation, autophagy, and release of inflammatory factors in pre-osteoblasts via the AMPK signaling pathway. Front Genet 12:783352. https://doi.org/10.3389/fgene.2021.783352
Acknowledgements
We appreciate the support from the Public Research Platform of the Academy of Chinese Medical Sciences, Zhejiang Chinese Medical University.
Funding
This work was supported by National Natural Science Foundation Youth Project of China (No. 82004247), Zhejiang Provincial Natural Science Foundation of China under Grant No. LQ21H270002, and Natural Science Foundation of Chongqing No. CSTB2022NSCQ-MSX0652.
Author information
Authors and Affiliations
Contributions
LQ, LZ, and QZ participated in the design of the experiment; LY and PS did experiments and data analysis; the draft of the manuscript was written by LY. All the authors read and approved the final manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding authors
Ethics declarations
Ethical Approval and Consent to Participate
Animals were purchased and raised from Animal Experimental Center of Zhejiang University of Traditional Chinese Medicine (License No.: 20180006004067).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yao, L., Zhang, Q., Sun, P. et al. Effect of Cinnamon and Aconite on Bone Formation-Bone Absorption Coupling in Bone Microenvironment. Rev. Bras. Farmacogn. 34, 511–521 (2024). https://doi.org/10.1007/s43450-023-00504-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43450-023-00504-5