Abstract
Introduction
Spinal measurements play an integral role in surgical planning for a variety of spine procedures. Full-length imaging eliminates distortions that can occur with stitched images. However, these images take radiologists significantly longer to read than conventional radiographs. Artificial intelligence (AI) image analysis software that can make such measurements quickly and reliably would be advantageous to surgeons, radiologists, and the entire health system.
Materials and methods
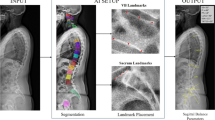
Institutional Review Board approval was obtained for this study. Preoperative full-length standing anterior–posterior and lateral radiographs of patients that were previously measured by fellowship-trained spine surgeons at our institution were obtained. The measurements included lumbar lordosis (LL), greatest coronal Cobb angle (GCC), pelvic incidence (PI), coronal balance (CB), and T1-pelvic angle (T1PA). Inter-rater intra-class correlation (ICC) values were calculated based on an overlapping sample of 10 patients measured by surgeons. Full-length standing radiographs of an additional 100 patients were provided for AI software training. The AI algorithm then measured the radiographs and ICC values were calculated.
Results
ICC values for inter-rater reliability between surgeons were excellent and calculated to 0.97 for LL (95% CI 0.88–0.99), 0.78 (0.33–0.94) for GCC, 0.86 (0.55–0.96) for PI, 0.99 for CB (0.93–0.99), and 0.95 for T1PA (0.82–0.99). The algorithm computed the five selected parameters with ICC values between 0.70 and 0.94, indicating excellent reliability. Exemplary for the comparison of AI and surgeons, the ICC for LL was 0.88 (95% CI 0.83–0.92) and 0.93 for CB (0.90–0.95). GCC, PI, and T1PA could be determined with ICC values of 0.81 (0.69–0.87), 0.70 (0.60–0.78), and 0.94 (0.91–0.96) respectively.
Conclusions
The AI algorithm presented here demonstrates excellent reliability for most of the parameters and good reliability for PI, with ICC values corresponding to measurements conducted by experienced surgeons. In future, it may facilitate the analysis of large data sets and aid physicians in diagnostics, pre-operative planning, and post-operative quality control.




Similar content being viewed by others
References
Hirsch BP, Vaynrub M, Siow M et al (2021) Visualization of the cervicothoracic junction with EOS imaging is superior to conventional lateral cervical radiographs. Global Spine J 11(6):925–930
Grover P, Siebenwirth J, Caspari C et al (2022) Can artificial intelligence support or even replace physicians in measuring sagittal balance? A validation study on preoperative and postoperative full spine images of 170 patients. Eur Spine J 31(8):1943–1951
Orosz LD, Bhatt FR, Jazini E et al (2022) Novel artificial intelligence algorithm: an accurate and independent measure of spinopelvic parameters. J Neurosurg Spine 37(6):893–901
Löchel J, Putzier M, Dreischarf M et al (2021) Evaluation of artificial intelligence based image analysis of sagittal profile. Eur Spine J 30:3328–3414
Vogt S, Scholl C, Grover P et al (2022) Validation of a novel artificial intelligence-based algorithm for the automatic measurement of cervical sagittal balance parameters on pre-and post-operative radiographs. Brain Spine 2:100968
Berlin C, Adomeit S, Grover P et al (2023) Novel ai-based algorithm for the automated computation of coronal parameters in adolescent idiopathic scoliosis patients: a validation study on 100 preoperative full spine X-rays. Glob Spine J 28:21925682231154544
Martin CT, Polly DW, Holton KJ et al (2021) Acute failure of S2-alar-iliac screw pelvic fixation in adult spinal deformity: novel failure mechanism, case series, and review of the literature. J Neurosurg Spine 36(1):53–61
He K, Gkioxari G, Dollár P, et al (2017) Mask r-cnn. In: Proceedings of the IEEE international conference on computer vision 2017. pp. 2961–2969
Ronneberger O, Fischer P, Brox T (2015) U-net: convolutional networks for biomedical image segmentation. In: medical image computing and computer-assisted intervention—MICCAI 2015: 18th International Conference, Munich, Germany, October 5–9, 2015, Proceedings, Part III 18 2015. Springer International Publishing, pp. 234–241
Zhang H, Cisse M, Dauphin YN, et al (2017) mixup: beyond empirical risk minimization. arXiv preprint arXiv:1710.09412
Contributors PS (2020) Model zoo. https://pytorch.org/serve/model_zoo.html. Accessed 18 Aug 2023
Cicchetti DV (1994) Guidelines, criteria, and rules of thumb for evaluating normed and standardized assessment instruments in psychology. Psychol Assess 6(4):284
Yamada K, Aota Y, Higashi T et al (2015) Accuracies in measuring spinopelvic parameters in full-spine lateral standing radiograph. Spine 40:E640–E646
Lee CM, Liu RW (2022) Comparison of pelvic incidence measurement using lateral x-ray, standard CT versus CT with 3d reconstruction. Eur Spine J 31(2):241–247
İplikçioğlu AC, Karabağ H (2022) Validity and reliability of spinopelvic parameters measured on computed tomography. Int J Spine Surg 16(5):875–880
Gupta M, Henry JK, Schwab F et al (2016) Dedicated spine measurement software quantifies key spino-pelvic parameters more reliably than traditional picture archiving and communication systems tools. Spine 41(1):E22–E27
Legaye J (2007) The femoro-sacral posterior angle: an anatomical sagittal pelvic parameter usable with dome-shaped sacrum. Eur Spine J 16(2):219–225
Chen HF, Mi J, Zhang HH, Zhao CQ (2019) Pelvic incidence measurement using a computed tomography data-based three-dimensional pelvic model. J Orthop Surg Res 14(1):13
Lee HD, Jeon CH, Chung NS, Kwon HJ (2017) Comparative analysis of three imaging modalities for evaluation of cervical sagittal alignment parameters: a validity and reliability study. Spine 42(24):1901–1907
Park SA, Kwak DS, Cho HJ, Min DU (2017) Changes of spinopelvic parameters in different positions. Arch Orthop Trauma Surg 137(9):1223–1232
Funding
The authors disclose no receipt of financial support for the data collection, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
JJH Made contributions to the design of the work, and the acquisition of data. PBS, MD, KO: Made substantial contributions to the acquisition, analysis, or interpretation of data. Drafted the work and revised it critically for important intellectual content. PG Made substantial contributions to the analysis, and interpretation of data. Drafted the work and revised it critically for important intellectual content. NRH, KEJ, CTM, JNS, DWPJr: Made substantial contributions to the conception of the work and reviewed the work critically for important intellectual content. JJH, PBS, PG, MD, KO, NRH, KEJ, CTM, JNS, DWPJr: Approved the version to be published and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
CM has consultancies to Medtronic, institutional research support from SI-Bone, and industry funding to travel to cadaveric surgical training sessions from Medtronic, NuVasive, and Accutech, and KF Degenerative committee member for AO Spine. KJ has consultancies with SI Bone and Medtronic. JS receives support of non-study-related clinical or research effort from Orthofix, NuVasive, and AO Spine. DP has consultancies with SI-Bone, Springer textbook (royalties), Medtronic (royalties), and Globus Medical (royalties) and has received research support from MizuhoOSI and Medtronic. NH, JH, PS, PG, JH, and MD have nothing to disclose.
Ethical approval/review
Institutional review board (IRB) approval for this project was obtained from the University of Minnesota.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Haselhuhn, J.J., Soriano, P.B.O., Grover, P. et al. Spine surgeon versus AI algorithm full-length radiographic measurements: a validation study of complex adult spinal deformity patients. Spine Deform 12, 755–761 (2024). https://doi.org/10.1007/s43390-024-00825-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-024-00825-y