Abstract
Purpose
Patients with neuromuscular scoliosis undergoing posterior instrumented spinal fusion can be underweight, malnourished, and have higher complication rates. A nutrition consult is common in this population and it is unclear if weight gain occurs from the consult or surgery. The purpose of the study was to determine if nutrition consultation in the year prior to spinal fusion resulted in significant differences in weight gain or percentile on the CP growth chart. The secondary aim was to determine if there would be deformity progression during that time.
Methods
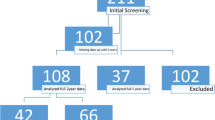
Retrospective chart and radiograph review was performed for all patients with neuromuscular spinal deformity treated with posterior instrumented spinal fusion at one institution between January 1, 2009 and August 1, 2015. Inclusion criteria included < 20 years old, diagnosis of neuromuscular scoliosis, and 1-year pre-operative percentile on the CP growth chart < 50. Patient demographics, GMFCS level, weight, percentile on appropriate CP growth chart, major curve and pelvic obliquity at 1 year pre-operatively and at surgery were recorded.
Results
Sixty-eight patients met inclusion criteria. Thirty-seven patients had a nutrition appointment within 1 year pre-operatively, 31 patients did not. There were no significant differences between the groups when comparing increase in weight (p = 0.9), percentile on CP growth charts (p = 0.3), major deformity (p = 0.1), and pelvic obliquity (p = 0.2). Overall, there was a mean 3.2 kg weight gain, 5.2% increase on CP growth charts, 40° increase in major curve, and 5° worsening of pelvic obliquity in the year before surgery. There was an average overall increase in the pre-operative albumin value, but this was not different between groups (p = 0.6). Children who were tube fed gained on average 10.8 percentiles on the CP growth chart, whereas children without gained only 0.5 percentiles (p = 0.002).
Conclusions
Nutrition consultations in the year preceding posterior instrumented spinal fusion do not lead to weight optimization prior to surgery in comparison to patients without nutrition consults. Gastrostomy tubes were found to be helpful for weight optimization and should be considered as an alternative nutrition option in pre-operative planning in underweight patients.
Level of evidence
III—therapeutic study: retrospective comparative study.



Similar content being viewed by others
References
Vialle R, Thévenin-Lemoine C, Mary P (2013) Neuromuscular scoliosis. Orthop Traumatol Surg Res. https://doi.org/10.1016/j.otsr.2012.11.002 (Published online)
Jevsevar DS, Karlin LI (1993) The relationship between preoperative nutritional status and complications after an operation for scoliosis in patients who have cerebral palsy. J Bone Jt Surg Ser A. https://doi.org/10.2106/00004623-199306000-00008 (Published online)
Sponseller PD, LaPorte DM, Hungerford MW, Eck K, Bridwell KH, Lenke LG (2000) Deep wound infections after neuromuscular scoliosis surgery: A multicenter study of risk factors and treatment outcomes. Spine (Phila Pa 1976). https://doi.org/10.1097/00007632-200010010-00007 (Published online)
Bowen RE, Abel MF, Arlet V et al (2012) Outcome assessment in neuromuscular spinal deformity. J Pediatr Orthop. https://doi.org/10.1097/BPO.0b013e318273ab5a (Published online)
Miller DJ, Flynn JM, Pasha S et al (2020) Improving health-related quality of life for patients with nonambulatory cerebral palsy: who stands to gain from scoliosis surgery? J Pediatr Orthop. https://doi.org/10.1097/BPO.0000000000001424 (Published online)
Suk KS, Baek JH, Park JO et al (2015) Postoperative quality of life in patients with progressive neuromuscular scoliosis and their parents. Spine J. https://doi.org/10.1016/j.spinee.2014.09.030 (Published online)
Watanabe K, Lenke LG, Daubs MD et al (2009) Is spine deformity surgery in patients with spastic cerebral palsy truly beneficial?: a patient/parent evaluation. Spine (Phila Pa 1976). https://doi.org/10.1097/BRS.0b013e3181948c8f (Published online)
Ramo BA, Roberts DW, Tuason D et al (2014) Surgical site infections after posterior spinal fusion for neuromuscular scoliosis: a thirty year experience at a single institution. J Bone Jt Surg Am Vol. https://doi.org/10.2106/JBJS.N.00277 (Published online)
Pahys JM, Samdani A, Kelly M et al (2016) Are severely underweight patients with cerebral palsy at a higher risk for complications and poorer outcomes following posterior spinal fusion for scoliosis? In: 23rd International meeting on advanced spinal techniques, Washington, DC
Baldwin KD, Cahill PJ, Sponseller PD et al (2020) BMI change following spinal fusion for neuromuscular scoliosis surgery. Spine Deform. https://doi.org/10.1007/s43390-020-00109-1 (Published online)
DeFrancesco CJ, Miller DJ, Cahill PJ, Spiegel DA, Flynn JM, Baldwin KD (2018) Releasing the tether: weight normalization following corrective spinal fusion in cerebral palsy. J Orthop Surg. https://doi.org/10.1177/2309499018782556 (Published online)
Adogwa O, Martin JR, Huang K et al (2014) Preoperative serum albumin level as a predictor of postoperative complication after spine fusion. Spine (Phila Pa 1976). https://doi.org/10.1097/BRS.0000000000000450 (Published online)
Brooks J, Day S, Shavelle R, Strauss D (2011) Low weight, morbidity, and mortality in children with cerebral palsy: new clinical growth charts. Pediatrics. https://doi.org/10.1542/peds.2010-2801 (Published online)
Jain A, Sponseller PD, Shah SA et al (2016) Subclassification of GMFCS level-5 cerebral palsy as a predictor of complications and health-related quality of life after spinal arthrodesis. J Bone Jt Surg Am Vol. https://doi.org/10.2106/JBJS.15.01359 (Published online)
Osebold WR, Mayfield JK, Winter RB, Moe JH (1982) Surgical treatment of paralytic scoliosis associated with myelomeningocele. J Bone Jt Surg Ser A. https://doi.org/10.2106/00004623-198264060-00006 (Published online)
Cross MB, Yi PH, Thomas CF, Garcia J, Della Valle CJ (2014) Evaluation of malnutrition in orthopaedic surgery. J Am Acad Orthop Surg. https://doi.org/10.5435/JAAOS-22-03-193 (Published online)
Courtney PM, Rozell JC, Melnic CM, Sheth NP, Nelson CL (2016) Effect of malnutrition and morbid obesity on complication rates following primary total joint arthroplasty. J Surg Orthop Adv. https://doi.org/10.3113/jsoa.2016.0099 (Published online)
Tsantes AG, Papadopoulos DV, Lytras T et al (2019) Association of malnutrition with periprosthetic joint and surgical site infections after total joint arthroplasty: a systematic review and meta-analysis. J Hosp Infect. https://doi.org/10.1016/j.jhin.2019.04.020 (Published online)
Belthur M, Bosch L, Wood W, Boan C, Miller F, Shrader MW (2019) Perioperative management of patients with cerebral palsy undergoing scoliosis surgery: survey of surgeon practices. J Pediatr Rehabil Med. https://doi.org/10.3233/PRM-170504 (Published online)
Sullivan PB, Juszczak E, Bachlet AME et al (2005) Gastrostomy tube feeding in children with cerebral palsy: a prospective, longitudinal study. Dev Med Child Neurol. https://doi.org/10.1017/S0012162205000162 (Published online)
Coppock JH, Ridolfi DR, Hayes JF, St. Paul M, Wilfley DE (2014) Current approaches to the management of pediatric overweight and obesity. Curr Treat Options Cardiovasc Med. https://doi.org/10.1007/s11936-014-0343-0 (Published online)
Nishnianidze T, Bayhan IA, Abousamra O et al (2016) Factors predicting postoperative complications following spinal fusions in children with cerebral palsy scoliosis. Eur Spine J. https://doi.org/10.1007/s00586-015-4243-0 (Published online)
Hollenbeck SM, Yaszay B, Sponseller PD et al (2019) The pros and cons of operating early versus late in the progression of cerebral palsy scoliosis. Spine Deform. https://doi.org/10.1016/j.jspd.2018.09.002 (Published online)
Funding
This study had no external funding source.
Author information
Authors and Affiliations
Contributions
Conception or design of work: ATM, MRL, KDB. Acquisition, analysis, or interpretation of data for the work: ATM, MRL, DAS, PJC, JBA, KDB. Drafting of work or revising it critically for important intellectual content: ATM, MRL, DAS, PJC, JBA, KDB. Final approval of version to be published:: ATM, MRL, DAS, PJC, JBA, KDB.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meltzer-Bruhn, A.T., Landrum, M.R., Spiegel, D.A. et al. Does nutrition consultation in the year leading up to neuromuscular scoliosis surgery result in significant weight gain, or just a larger magnitude curve?. Spine Deform 10, 151–158 (2022). https://doi.org/10.1007/s43390-021-00401-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-021-00401-8