Abstract
Objective
Surgical intervention for primary spontaneous pneumothorax (PSP) involves thoracoscopic bullectomy with or without adjunct procedures such as mechanical or chemical pleurodesis aimed at preventing recurrence. We aimed to access our recurrence rate following thoracoscopic bullectomy and staple line coverage only, in children.
Methods
We retrospectively reviewed all cases of children with PSP managed with thoracoscopic bullectomy in our institution between 2013 and 2021.
Results
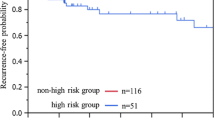
17 thoracoscopic bullectomies were performed on 10 patients over the 9-year period. Apart from coverage of the staple line with fibrin glue, no adjunct procedure was done in the first instance. There were nine males and one female with a median age of 14 years (12–16 years). Median post-operative length of stay was 2 days (2–5 days). No immediate peri-operative complication was seen. There were 3 (18%) recurrences seen during a median follow-up duration 15 months (3–48 months). The median time to developing recurrence was 10 months (1.5–15 months). All recurrent cases had thoracoscopic subtotal pleurectomy and chest drain insertion, and recovered uneventfully.
Conclusion
From our series, thoracoscopic bullectomy with staple line coverage alone appears to be a safe and effective option for children with PSP in the first instance, as it is associated with less morbidity and minimal hospital stay. We recommend subtotal pleurectomy for patients with recurrence.

Similar content being viewed by others
Data availability
Derived data supporting the findings of this study are available from the corresponding author upon request.
Abbreviations
- PSP:
-
Primary spontaneous pneumothorax
- VATS:
-
Video-assisted thoracoscopic surgery
References
MacDuff A, Arnold A, Harvey J (2010) Management of spontaneous pneumothorax: British Thoracic Society pleural disease guideline 2010. Thorax 65:i18–i31. https://doi.org/10.1136/THX.2010.136986
Williams K, Lautz TB, Leon AH, Oyetunji TA (2018) Optimal timing of video-assisted thoracoscopic surgery for primary spontaneous pneumothorax in children. J Pediatr Surg 53:1858–1861. https://doi.org/10.1016/j.jpedsurg.2017.11.047
Roberts ME, Rahman NM, Maskell NA et al (2023) British Thoracic Society Guideline for pleural disease. Thorax 78:s1–s42. https://doi.org/10.1136/thorax-2022-219784
Imperatori A, Rotolo N, Spagnoletti M et al (2015) Risk factors for postoperative recurrence of spontaneous pneumothorax treated by video-assisted thoracoscopic surgery. Interact Cardiovasc Thorac Surg 20:647–652. https://doi.org/10.1093/ICVTS/IVV022
Bialas RC, Weiner TM, Phillips JD (2008) Video-assisted thoracic surgery for primary spontaneous pneumothorax in children: is there an optimal technique? J Pediatr Surg 43:2151–2155. https://doi.org/10.1016/j.jpedsurg.2008.08.041
Soccorso G, Anbarasan R, Singh M et al (2015) Management of large primary spontaneous pneumothorax in children: radiological guidance, surgical intervention and proposed guideline. Pediatr Surg Int 31:1139–1144. https://doi.org/10.1007/S00383-015-3787-8
Wilson PM, Rymeski B, Xu X, Hardie W (2021) An evidence-based review of primary spontaneous pneumothorax in the adolescent population. J Am Coll Emerg Physicians Open. https://doi.org/10.1002/EMP2.12449
Cerchia E, Conighi ML, Bleve C et al (2020) Feasibility of a standardized management for primary spontaneous pneumothorax in children and adolescents: a retrospective multicenter study and review of the literature. J Laparoendosc Adv Surg Tech 30:841–846. https://doi.org/10.1089/lap.2019.0493
Bauman MH, Strange C, Heffner JE et al (2001) Management of spontaneous pneumothorax: an American College of Chest Physicians Delphi Consensus Statement. Chest 119:590–602. https://doi.org/10.1378/CHEST.119.2.590
Furia S, Breda C (2019) Primary spontaneous pneumothorax in children and adolescents: a systematic review. Pediatr Med. https://doi.org/10.21037/PM.2019.04.01/COIF
Muramatsu T, Nishii T, Takeshita S et al (2010) Preventing recurrence of spontaneous pneumothorax after thoracoscopic surgery: a review of recent results. Surg Today 40:696–699. https://doi.org/10.1007/S00595-009-4208-1
Ling ZG, Wu YB, Ming MY et al (2015) The effect of pleural abrasion on the treatment of primary spontaneous pneumothorax: a systematic review of randomized controlled trials. PLoS ONE 10:e0127857. https://doi.org/10.1371/JOURNAL.PONE.0127857
Jeon HW, du Kim Y, Kye YK, Kim KS (2016) Air leakage on the postoperative day: powerful factor of postoperative recurrence after thoracoscopic bullectomy. J Thorac Dis 8:93–97. https://doi.org/10.3978/J.ISSN.2072-1439.2016.01.38
Asghar Nawaz M, Apparau D, Zacharias J, Shackcloth M (2019) Approach to pneumothorax surgery: a national survey of current UK practice. Asian Cardiovasc Thorac Ann 27:180–186. https://doi.org/10.1177/0218492319825943
Gaunt A, Martin-Ucar AE, Beggs L et al (2008) Residual apical space following surgery for pneumothorax increases the risk of recurrence. Eur J Cardiothorac Surg 34:169–173. https://doi.org/10.1016/J.EJCTS.2008.03.049
Yeung F, Chung PHY, Hung ELY et al (2017) Surgical intervention for primary spontaneous pneumothorax in pediatric population: when and why? J Laparoendosc Adv Surg Tech 27:841–844. https://doi.org/10.1089/lap.2016.0163
Jheon S, Lee S, Kim HR et al (2014) Staple line coverage after bullectomy for primary spontaneous pneumothorax: a randomized trial. Ann Thorac Surg 98:2005–2011. https://doi.org/10.1016/j.athoracsur.2014.06.047
Min X, Huang Y, Yang Y et al (2014) Mechanical pleurodesis does not reduce recurrence of spontaneous pneumothorax: a randomized trial. Ann Thorac Surg 98:1790–1796. https://doi.org/10.1016/J.ATHORACSUR.2014.06.034
Williams K, Baumann L, Grabowski J, Lautz TB (2019) Current practice in the management of spontaneous pneumothorax in children. J Laparoendosc Adv Surg Tech A 29:551–556. https://doi.org/10.1089/LAP.2018.0629
Funding
No funding support.
Author information
Authors and Affiliations
Contributions
All authors attest that they meet the current ICMJE criteria for authorship.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing interests.
Ethical approval
Data was collected in accordance to Institutional guidelines.
Rights and permissions
About this article
Cite this article
Emordi, V., Aslam, A. Surgical management of spontaneous pneumothorax in children. J Ped Endosc Surg 6, 7–11 (2024). https://doi.org/10.1007/s42804-024-00219-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42804-024-00219-x