Abstract
Introduction
We present herein a 7-year single-surgeon case series describing the experience and learning from managing paediatric gastro-oesophageal reflux disease (GORD) and the laparoscopic Nissen’s fundoplication (LNF) procedure.
Methods
Retrospectively, data encompassing all patients subjected to LNF from 2014 to 2021 was compiled. Our surgical paradigm centred on optimising restrained dissection at the diaphragmatic hiatus and a lax gastric wrap. Patient demographics, preoperative medical particulars, investigative findings, and postoperative outcomes were systematically collected to facilitate subsequent analysis.
Results
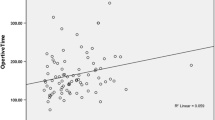
Across the study’s duration, 43 laparoscopic Nissen’s fundoplication were completed. Operative time reduced from 121 min in the first 10 cases to 69 min in the final 10 cases reflecting a learning curve. A total of six cases were converted to open fundoplication (14%). In our cohort, 2 patients required redo operations for technical failure, one was operated on at another centre (5%), 28 patients had resolution of symptoms with surgery alone (65%), one improved with further dilatation (2%) and 14 improved with additional medical therapy (32%), including prokinetics and antihistamines. In this cohort, ten patients had concomitant neurological diagnosis, with five improving post-fundoplication, four improving with pharmacological treatment and one after redo-surgery.
Discussion
Our series highlights 7 years of a surgeon’s progression in their technical proficiency with GORD surgery, showing the learning curve for this surgery. This was evident in shortening of operative times. More importantly, careful patient selection led to clinical resolution of symptoms in many cases (89.1%). We share this clinical journey, along with insightful video supplements, offering learning points for aspiring minimally invasive surgeons. These insights lay the groundwork for the next generation, dedicated to improving the lives of children with GORD.
Similar content being viewed by others
Data availability
Derived data supporting the findings of this study are available from the corresponding author upon request
References
Arcos-Machancoses JV, Ruiz Hernández C, Martin de Carpi J, PinillosPisón S (2018) A systematic review with meta-analysis of the prevalence of gastroesophageal reflux in congenital diaphragmatic hernia pediatric survivors. Dis Esophagus 31. https://doi.org/10.1093/dote/dox158
Capito C, Leclair MD, Piloquet H, Plattner V, Heloury Y, Podevin G (2008) Long-term outcome of laparoscopic Nissen-Rossetti fundoplication for neurologically impaired and normal children. Surg Endosc 22:875–880
Iwanaka T, Kanamori Y, Sugiyama M, Komura M, Tanaka Y, Kodaka T, Ishimaru T (2010) Laparoscopic fundoplication for gastroesophageal reflux disease in infants and children. Surg Today 40:393–397
Langer JC (2003) The failed fundoplication. Semin Pediatr Surg 12:110–117
Lauriti G, Lisi G, Lelli Chiesa P, Zani A, Pierro A (2018) Gastroesophageal reflux in children with neurological impairment: a systematic review and meta-analysis. Pediatr Surg Int 34:1139–1149
Leung AK, Hon KL (2019) Gastroesophageal reflux in children: an updated review. Drugs Context 8:212591
Livingston MH, Shawyer AC, Rosenbaum PL, Jones SA, Walton JM (2015) Fundoplication and gastrostomy versus percutaneous gastrojejunostomy for gastroesophageal reflux in children with neurologic impairment: a systematic review and meta-analysis. J Pediatr Surg 50:707–714
Martin K, Deshaies C, Emil S (2014) Outcomes of pediatric laparoscopic fundoplication: a critical review of the literature. Can J Gastroenterol Hepatol 1:97–102
Quitadamo P, Thapar N, Staiano A, Borrelli O (2016) Gastrointestinal and nutritional problems in neurologically impaired children. Eur J Paediatr Neurol 20:810–815
Rosen R, Vandenplas Y, Singendonk M, Cabana M, DiLorenzo C, Gottrand F, Gupta S, Langendam M, Staiano A, Thapar N, Tipnis N (2018) Pediatric gastroesophageal reflux clinical practice guidelines: joint recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition. J Pediatr Gastroenterol Nutr 66:516–554
Ruigómez A, Wallander MA, Lundborg P, Johansson S, Rodriguez LA (2010) Gastroesophageal reflux disease in children and adolescents in primary care. Scand J Gastroenterol 45:139–146
Slater BJ, Rothenberg SS (2017) Gastroesophageal reflux. Semin Pediatr Surg 26:56–60. https://doi.org/10.1053/j.sempedsurg.2017.02.007
Srivastava R, Downey EC, O’Gorman M, Feola P, Samore M, Holubkov R, Mundorff M, James BC, Rosenbaum P, Young PC, Dean JM (2009) Impact of fundoplication versus gastrojejunal feeding tubes on mortality and in preventing aspiration pneumonia in young children with neurologic impairment who have gastroesophageal reflux disease. Pediatrics 123:338–345
Stone B, Hester G, Jackson D, Richardson T, Hall M, Gouripeddi R, Butcher R, Keren R, Srivastava R (2017) Effectiveness of fundoplication or gastrojejunal feeding in children with neurologic impairment. Hosp Pediatr 7:140–148
Funding
No funding or grant support.
Author information
Authors and Affiliations
Contributions
All authors attest that they meet the current ICMJE criteria for authorship.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this manuscript.
Ethical approval
Data was collected in accordance to Institutional guidelines.
Rights and permissions
About this article
Cite this article
Abdelbary, M., Berezowska, A., Cao, K. et al. That’s a wrap: a 7-year case series of paediatric laparoscopic Nissen’s fundoplication. J Ped Endosc Surg 6, 21–24 (2024). https://doi.org/10.1007/s42804-024-00218-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42804-024-00218-y