Abstract
Background
Recent decade has seen a significant increase in the average age at which couples first produce, thus it becomes essential to study and understand how age affects fertility in humans.
Methodology
Age-dependent variations in human seminal plasma proteome were identified by two- dimensional differential gel electrophoresis (2D-DiGE) followed by mass spectrometric analysis.
Results
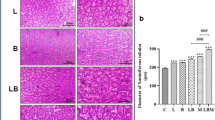
Overall, 10 differentially expressed proteins were identified, viz. glutaredoxin domain-containing cysteine-rich protein-2, clusterin, serum albumin, translation initiation factor IF-2 like, alternative protein RRT-34, ecto-ADP-ribosyltransferase 4, protein Unc-119 homolog A, CB1 cannabinoid receptor-interacting protein 1 and serotransferrin. Expression of clusterin was found upregulated in older age samples, which was further validated by western blotting analysis. It is evident from available literature that higher expression of clusterin is associated with poor semen quality.
Conclusion
Based on this, our study for some extent concludes and supports the fact that semen quality declines with increasing age.



Similar content being viewed by others
Abbreviations
- CBB:
-
Coomassie brilliant blue
- DiGE:
-
Differential gel electrophoresis
- ROS:
-
Reactive oxygen species
References
Agarwal A, Makker K, Sharma R (2008) Clinical relevance of oxidative stress in male factor infertility: an update. Am J Reprod Immunol 59:2–11
Agarwal A, Ayaz A, Samanta L, Sharma R, Assidi M, Abuzenadah AM, Sabanegh E (2015) Comparative proteomic network signatures in seminal plasma of infertile men as a function of reactive oxygen species. Clin Proteomics 12:23
Ahuja HS, Tenniswood M, Zakeri ZF (1996) Differential expression of clusterin in the testis and epididymis of postnatal and germ cell deficient mice. J Androl 17:491–501
Aitken RJ (2014) Age, the environment and our reproductive future: bonking baby boomers and the future of sex. Reproduction 147:S1–S11
Aitken RJ, De Iuliis GN (2010) On the possible origins of DNA damage in human spermatozoa. Mol Hum Reprod 16:3–13
Alam M, Selladurai M, Nagpal S, Tomar AK, Saraswat M, Raziuddin M, Mittal S, Singh TP, Yadav S (2010) Sample complexity reduction aids efficient detection of low-abundant proteins from human amniotic fluid. J Sep Sci 33:1723–1729
Bailey R, Griswold MD (1999) Clusterin in the male reproductive system: localization and possible function. Mol Cell Endocrinol 151:17–23
Belloc S, Cohen-Bacrie P, Benkhalifa M, Cohen-Bacrie M, De Mouzon J, Hazout A, Menezo Y (2008) Effect of maternal and paternal age on pregnancy and miscarriage rates after intrauterine insemination. Reprod Biomed Online 17:392–397
Bieniek JM, Drabovich AP, Lo KC (2016) Seminal biomarkers for the evaluation of male infertility. Asian J Androl 18:426–433
Cadavid JA, Alvarez A, Markert UR, Cardona Maya W (2014) Differential protein expression in seminal plasma from fertile and infertile males. J Hum Reprod Sci 7(3):206–211
Cocuzza M, Athayde KS, Agarwal A, Sharma R, Pagani R, Lucon AM, Srougi M, Hallak J (2008) Age-related increase of reactive oxygen species in neat semen in healthy fertile men. Urology 71:490–494
Cooper TG, Noonan E, von Eckardstein S, Auger J, Baker HW, Behre HM, Haugen TB, Kruger T, Wang C, Mbizvo MT, Vogelsong KM (2010) World Health Organization reference values for human semen characteristics. Hum. Reprod. Update 16:231–245
Cross NL (1998) Role of cholesterol in sperm capacitation. Biol Reprod 59:7–11
Davalieva K, Kiprijanovska S, Noveski P, Plaseski T, Kocevska B, Broussard C, Plaseska-Karanfilska D (2012) Proteomic analysis of seminal plasma in men with different spermatogenic impairment. Andrologia 44:256–264
Del Giudice PT, Belardin LB, Camargo M, Zylbersztejn DS, Carvalho VM, Cardozo KH, Bertolla RP, Cedenho AP (2016) Determination of testicular function in adolescents with varicocoele—a proteomics approach. Andrology 4:447–455
Drabovich AP, Jarvi K, Diamandis EP (2011) Verification of male infertility biomarkers in seminal plasma by multiplex selected reaction monitoring assay. Mol Cell Proteom 10(M110):004127
Drabovich AP, Saraon P, Jarvi K, Diamandis EP (2014) Seminal plasma as a diagnostic fluid for male reproductive system disorders. Nat Rev Urol 11:278–288
Elzanaty S, Erenpreiss J, Becker C (2007) Seminal plasma albumin: origin and relation to the male reproductive parameters. Andrologia 39:60–65
Ganguly S, Unisa S (2010) Trends of infertility and childlessness in India: findings from NFHS data. Facts Views Vis Obgyn 2(2):131–138
Gilany K, Minai-Tehrani A, Savadi-Shiraz E, Rezadoost H, Lakpour N (2015) Exploring the human seminal plasma proteome: an unexplored gold mine of biomarker for male infertility and male reproduction disorder. J Reprod Infertil 16:61–71
Gray S, Huggins C (1942) Electrophoretic analysis of human semen. Proc Soc Exp Biol Med 50:351–353
Griffiths GS, Galileo DS, Aravindan RG, Martin-DeLeon PA (2009) Clusterin facilitates exchange of glycosyl phosphatidylinositol-linked SPAM1 between reproductive luminal fluids and mouse and human sperm membranes. Biol Reprod 81:562–570
Herwig R, Knoll C, Planyavsky M, Pourbiabany A, Greilberger J, Bennett KL (2013) Proteomic analysis of seminal plasma from infertile patients with oligoasthenoteratozoospermia due to oxidative stress and comparison with fertile volunteers. Fertil Steril 100(355–366):e352
Humm KC, Sakkas D (2013) Role of increased male age in IVF and egg donation: is sperm DNA fragmentation responsible? Fertil Steril 99:30–36
Intasqui P, Camargo M, Antoniassi MP, Cedenho AP, Carvalho VM, Cardozo KHM, Zylbersztejn DS, Bertolla RP (2016) Association between the seminal plasma proteome and sperm functional traits. Fertil Steril 105:617–628
Johnson SL, Gemmell NJ (2012) Are old males still good males and can females tell the difference? Do hidden advantages of mating with old males off-set costs related to fertility, or are we missing something else? BioEssays 34:609–619
Johnson SL, Dunleavy J, Gemmell NJ, Nakagawa S (2015) Consistent age-dependent declines in human semen quality: a systematic review and meta-analysis. Ageing Res Rev 19:22–33
Kong A, Frigge ML, Masson G, Besenbacher S, Sulem P, Magnusson G, Gudjonsson SA, Sigurdsson A, Jonasdottir A, Jonasdottir A, Wong WS, Sigurdsson G, Walters GB, Steinberg S, Helgason H, Thorleifsson G, Gudbjartsson DF, Helgason A, Magnusson OT, Thorsteinsdottir U, Stefansson K (2012) Rate of de novo mutations and the importance of father’s age to disease risk. Nature 488:471–475
Koppers AJ, De Iuliis GN, Finnie JM, McLaughlin EA, Aitken RJ (2008) Significance of mitochondrial reactive oxygen species in the generation of oxidative stress in spermatozoa. J Clin Endocrinol Metab 93:3199–3207
Kuhnert B, Nieschlag E (2004) Reproductive functions of the ageing male. Hum Reprod Update 10:327–339
Li Y, Lin H, Li Y, Cao J (2011) Association between socio-psycho-behavioral factors and male semen quality: systematic review and meta-analyses. Fertil Steril 95:116–123
Maheshwari A, Hamilton M, Bhattacharya S (2008) Effect of female age on the diagnostic categories of infertility. Hum Reprod 23:538–542
Milardi D, Grande G, Vincenzoni F, Messana I, Pontecorvi A, De Marinis L, Castagnola M, Marana R (2012) Proteomic approach in the identification of fertility pattern in seminal plasma of fertile men. Fertil Steril 97:67–73
Milardi D, Grande G, Vincenzoni F, Castagnola M, Marana R (2013) Proteomics of human seminal plasma: identification of biomarker candidates for fertility and infertility and the evolution of technology. Mol Reprod Dev 80:350–357
Mostafa T, Anis T, El Nashar A, Imam H, Osman I (2012) Seminal plasma reactive oxygen species-antioxidants relationship with varicocele grade. Andrologia 44:66–69
Pilch B, Mann M (2006) Large-scale and high-confidence proteomic analysis of human seminal plasma. Genome Biol 7(5):R40
Reinhardt K (2007) Evolutionary consequences of sperm cell aging. Q Rev Biol 82:375–393
Salehi M, Akbari H, Heidari MH, Molouki A, Murulitharan K, Moeini H, Novin MG, Aabed F, Taheri H, Fadaei F, Mohsenzadeh M, Jafari M, Pirouzi A, Heidari R (2013) Correlation between human clusterin in seminal plasma with sperm protamine deficiency and DNA fragmentation. Mol Reprod Dev 80(9):718–724
Saraswat M, Joenvaara S, Jain T, Tomar AK, Sinha A, Singh S, Yadav S, Renkonen R (2017) Human spermatozoa quantitative proteomic signature classifies normo- and asthenozoospermia. Mol Cell Proteom 16:57–72
Sartorius GA, Nieschlag E (2010) Paternal age and reproduction. Hum Reprod Update 16:65–79
Siva-Jothy MT (2000) The young sperm gambit. Ecol Lett 3:172–174
Song GJ, Lewis V (2008) Mitochondrial DNA integrity and copy number in sperm from infertile men. Fertil Steril 90:2238–2244
Strocchi P, Smith MA, Perry G, Tamagno E, Danni O, Pession A, Gaiba A, Dozza B (2006) Clusterin up-regulation following sub-lethal oxidative stress and lipid peroxidation in human neuroblastoma cells. Neurobiol Aging 27:1588–1594
Sylvester SR, Morales C, Oko R, Griswold MD (1991) Localization of sulfated glycoprotein-2 (clusterin) on spermatozoa and in the reproductive tract of the male rat. Biol Reprod 45:195–207
Tomar AK, Sooch BS, Raj I, Singh S, Singh TP, Yadav S (2011) Isolation and identification of Concanavalin A binding glycoproteins from human seminal plasma: a step towards identification of male infertility marker proteins. Dis Mark 31:379–386
Tomar AK, Sooch BS, Singh S, Yadav S (2012) Differential proteomics of human seminal plasma: a potential target for searching male infertility marker proteins. Proteom Clin Appl 6:147–151
Tomar AK, Kumar S, Chhillar S, Kumaresan A, Singh S, Yadav S (2016) Human serum albumin and prolactin inducible protein complex enhances sperm capacitation in vitro. J. Proteins Proteom 7:107–113
Wang J, Wang J, Zhang HR, Shi HJ, Ma D, Zhao HX, Lin B, Li RS (2009) Proteomic analysis of seminal plasma from asthenozoospermia patients reveals proteins that affect oxidative stress responses and semen quality. Asian J Androl 11:484–491
Jodar M, Soler-Ventura A, Oliva R, Molecular Biology of R. and Development Research G. (2017) Semen proteomics and male infertility. J Proteom 162:125–134
Yamakawa K, Yoshida K, Nishikawa H, Kato T, Iwamoto T (2007) Comparative analysis of interindividual variations in the seminal plasma proteome of fertile men with identification of potential markers for azoospermia in infertile patients. J Androl 28:858–865
Acknowledgements
This work was supported by research grant received from Indian Council for Medical Research (ICMR), Government of India, New Delhi. KK also acknowledges ICMR for his fellowship.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors of this manuscript declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kant, K., Tomar, A.K., Singh, S. et al. Ageing associated proteomic variations in seminal plasma of Indian men. J Proteins Proteom 10, 83–89 (2019). https://doi.org/10.1007/s42485-019-00013-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42485-019-00013-x