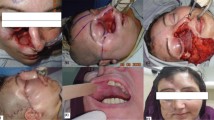
Abstract
Advances in oncological head and neck surgery evidenced in the last decades have been linked to the progression in the reconstruction capacity of the defects resulting from resection of advanced tumors, allowing the improvement of both esthetic and functional results, as well as decrease the rate of postoperative complications in rescue surgery. To understand the situation of head and neck reconstruction across the country. a questionnaire about the current state of head and neck reconstructive surgery in Spain in otorhinolaryngology and head and neck surgery departments was distributed via email. Eighty (25.5%) of 313 ENT departments in Spain carry out some type of reconstruction in oncological surgery of the head and neck. Forty-four (55%) departments use regional pedicled flaps as a single reconstruction strategy, while 36 (45%) departments also employed the use of microvascular free flaps. Fifty-six (70%) departments perform 10 or less regional pedicled flaps per year, while 21 (29.6%) perform 10 or more flaps per year, with an average of 9.91 ± 11.73 flaps/year (min. 2, max. 40). Seven (8.75%) departments perform 10 or more free flaps a year, while the other 29 (36.25%) perform 10 or less, with an average of 4.96 ± 5.1 free flaps microvascular year (min. 2, max 20). In our country, head and neck cancer surgeries are performed in a tertiary level hospital and patients benefit from the reconstruction of post-surgical defects, through the use of regional pedicled or microvascular free flaps.

Similar content being viewed by others
References
Lorch JH, Goloubeva O, Haddad RI, Cullen K, Sarlis N, Tishler R, et al. TAX 324 Study Group. Induction chemotherapy with cisplatin and fluorouracil alone or in combination with docetaxel in locally advanced squamous-cell cancer of the head and neck: Long-term results of the TAX 324 randomised phase 3 trial. Lancet Oncol. 2011;12:153–9.
León X, Agüero A, López M, García J, Farré N, López-Pousa A, et al. Salvage surgery after local recurrence in patients with head and neck carcinoma treated with chemoradiotherapy or bioradiotherapy. Auris Nasus Larynx. 2015;42:145–9.
Corbitt C, Skoracki RJ, Yu P, Hanasono MM. Free flap failure in head and neck reconstruction. Head Neck. 2014;36:1440–5.
Ligh CA, Nelson JA, Wink JD, Gerety PA, Fischer JP, Wu LC, et al. An analysis of early oncologic head and neck free flap reoperations from the 2005–2012 ACS–NSQIP dataset. J Plast Surg Hand Surg. 2016;50:85–92.
Bahl V, Shuman AG, Hu HM, Jackson CR, Pannucci CJ, Alaniz C, et al. Chemoprophylaxis for venous thromboembolism in otolaryngology. JAMA Otolaryngol Head Neck Surg. 2014;140:999–1005.
Cannady SB, Hatten KM, Bur AM, Brant J, Fischer JP, Newman JG, et al. Use of free tissue transfer in head and neck cancer surgery and risk of overall and serious complication(s): an American College of Surgeons-National Surgical Quality Improvement Project analysis of free tissue transfer to the head and neck. Head Neck. 2017 Apr;39:702–7.
Chim H, Salgado CJ, Seselgyte R, Wei FC, Mardini S. Principles of head and neck reconstruction: an algorithm to guide flap selection. Semin Plast Surg. 2010;24:148–54.
Vila PM, Rich JT, Desai SC. Defining quality in head and neck reconstruction. Otolaryngol–Head Neck Surg. 2017;157:545–7.
O'Connell DA, Barber B, Klein MF, Soparlo J, Al-Marzouki H, Harris JR, et al. Algorithm based patient care protocol to optimize patient care and inpatient stay in head and neck free flap patients. J Otolaryngol Head Neck Surg. 2015;44:45.
Whitaker IS, Gulati V, Ross GL, Menon A, Ong TK. Variations in the postoperative management of free tissue transfers to the head and neck in the United Kingdom. Br J Oral Maxillofac Surg. 2007;45:16–8.
Mücke T, Müller AA, Kansy K, Hallermann W, Kerkmann H, Schuck N, et al. Microsurgical reconstruction of the head and neck--current practice of maxillofacial units in Germany, Austria, and Switzerland. J Craniomaxillofac Surg. 2011;39:449–52.
Kansy K, Mueller AA, Mücke T, Koersgen F, Wolff KD, Zeilhofer HF, et al. Microsurgical reconstruction of the head and neck region: current concepts of maxillofacial surgery units worldwide. J Craniomaxillofac Surg. 2015;43:1364–8.
Kim H, Jeong WJ, Ahn SH. Results of free flap reconstruction after ablative surgery in the head and neck. Clin Exp Otorhinolaryngol. 2015;8:167–73.
Tornero J, Cruz-Toro P, Farré A, Vega-Celiz J, Skufca J, Nogués J, et al. Free radial forearm flap in head and neck: our experience. Acta Otorrinolaringol Esp. 2014;65:27–32.
Wong CH, Wei FC. Microsurgical free flap in head and neck reconstruction. Head Neck. 2010;32:1236–45.
Liu M, Liu W, Yang X, Guo H, Peng H. Pectoralis major myocutaneous flap for head and neck defects in the era of free flaps: harvesting technique and indications. Sci Rep. 2017;7:46256.
Croce A, Moretti A, D’Agostino L, Neri G. Continuing validity of pectoralis major muscle flap 25 years after its first application. Acta Otorhinolaryngol Ital. 2003;23:297–304.
Liu R, Gullane P, Brown D, Irish J. Pectoralis major myocutaneous pedicled flap in head and neck reconstruction: retrospective review of indications and results in 244 consecutive cases at the Toronto General Hospital. J Otolaryngol. 2001;30:34–40.
Vartanian JG, Carvalho AL, Carvalho SM, Mizobe L, Magrin J, Kowalski LP. Pectoralis major and other myofascial/myocutaneous flaps in head and neck cancer reconstruction: experience with 437 cases at a single institution. Head Neck. 2004;26:1018–23.
Virós Porcuna D, León Vintró X, López Vilas M, Pujol Olmo A, Masià Ayala J, Quer AM. Pectoralis major flaps. Evolution of their use in the age of microvascularized flaps. Acta Otorrinolaringol Esp. 2008;59:263–8.
Kanazawa T, Sarukawa S, Fukushima S, Takeoda S, Kusaka G, Ichimura K. Current reconstructive techniques following head and neck cancer resection using microvascular surgery. Ann Vasc Dis. 2011;4:189–95.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
Ethical approval from the Spanish Society of Otorhinolaryngology—Head and Neck Surgery was obtained.
Informed Consent
Personal informed consent was sent with the questionnaire to all participants.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Surgery
Rights and permissions
About this article
Cite this article
Chiesa-Estomba, C.M., González-García, J.Á., Sistiaga-Suárez, J.A. et al. Reconstructive Head and Neck Surgery in Spanish Otorhinolaryngology—Head and Neck Surgery Departments: Current State of the Art. SN Compr. Clin. Med. 1, 473–478 (2019). https://doi.org/10.1007/s42399-019-00063-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42399-019-00063-8