Key summary points
To evaluate to what extent the standardized concept of need-based care on Behavioural and Psychological Symptoms of Dementia (BPSD), and formal caregiver distress, is superior when compared to spending more time or standard care with residents with BPSD.
AbstractSection FindingsNeed-based interventions had a significant effect on residents’ levels of pain behaviour. In the need-based care group, scores on overall BPSD (agitation and aggression, depression, euphoria, irritability, sleep and night-time behaviour) improved significantly from baseline when compared to other timepoints.
AbstractSection MessageTailored non-pharmacological interventions in the residential care for people with dementia reduce the level of BPSD and formal caregivers’ distress.
Abstract
Purpose
To evaluate to what extent the standardized concept of need-based care on Behavioural and Psychological Symptoms of Dementia (BPSD), and formal caregiver distress, is superior when compared to spending more time or standard care with residents with BPSD.
Methods
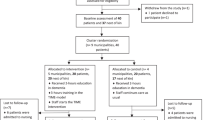
A longitudinal cluster randomized controlled study in 23 nursing homes in Belgium with 3 parallel groups was set up. A total of 481 residents with dementia participated. Formal caregivers in the need-based care group treated residents who displayed agitated or aggressive behaviour with a non-pharmacological intervention, tailored to unmet needs, twice a week with re-evaluation every 8 weeks. In the time group, formal caregivers spent ‘extra time’. In the standard care group, it was ‘care as usual’. Outcomes were measured at four different time points with the Doloplus-2 (to assess pain behaviour), Cohen-Mansfield Agitation Inventory (CMAI) for agitation, the Neuropsychiatric Inventory (NPI-NH) for BPSD and formal caregivers’ distress.
Results
Need-based interventions had a significant effect on residents’ levels of pain behaviour. In the need-based care group, scores on overall BPSD (agitation and aggression, depression, euphoria, irritability, sleep and night-time behaviour) improved significantly from baseline when compared to other timepoints. No significant different interactions over time were found between all three groups for categorized versions of NPI scores (ever versus never).
Conclusion
Need-based care reduced the level of BPSD in residents with dementia as well as formal caregivers’ distress. The study supports the importance of tailored non-pharmacological interventions in the residential care for people with dementia.
Trial Registry
Trial registration number B300201942084 (18/11/2019).


Similar content being viewed by others
Data availability
Data sets generated during the current study are available from the corresponding author on reasonable request.
References
Zwijsen SA et al (2014) Coming to grips with challenging behavior: a cluster randomized controlled trial on the effects of a multidisciplinary care program for challenging behavior in dementia. J Am Med Dir Assoc 15(7):531.e1-531.e10. https://doi.org/10.1016/j.jamda.2014.04.007
Strand LI, Gundrosen KF, Lein RK et al (2019) Body movements as pain indicators in older people with cognitive impairment: a systematic review. Eur J Pain 23:669–685. https://doi.org/10.1002/ejp.1344
Edberg AK, Bird M, Richards DA, Woods R, Keeley P, Davis-Quarrell V (2008) Strain in nursing care of people with dementia: nurses’ experience in Australia, Sweden and United Kingdom. Aging Ment Health 12(2):236–243. https://doi.org/10.1080/13607860701616374
Gitlin LN et al (2018) Targeting behavioural symptoms and functional decline in dementia: a randomized clinical trial. J Am Geriatr Soc 66(2):339–345. https://doi.org/10.1111/jgs.15194
Burley C, Burns K, Brodaty H (2022) Pharmacological and nonpharmacological approaches to reduce disinhibited behaviors in dementia: a systematic review. Int Psychogeriatr 34(4):335–351. https://doi.org/10.1017/S1041610222000151
Dyer S, Harrison S, Laver K, Whitehead C, Crotty M (2018) An overview of systematic reviews of pharmacological and non-pharmacological interventions for the treatment of behavioral and psychological symptoms of dementia. Int Psychogeriatr 30(3):295–309. https://doi.org/10.1017/S1041610217002344
Na R et al (2019) A systematic review and meta-analysis of nonpharmacological interventions for moderate to severe dementia. Psychiatry Investig 16(5):325–335. https://doi.org/10.30773/pi.2019.02.11.2
O’Sullivan J et al (2022) A tablet-based intervention for activating nursing home residents with dementia: Results from a cluster-randomized controlled trial. Int Psychogeriatr 34(2):129–141. https://doi.org/10.1017/S1041610221000818
Saragih ID, Suarilah I, Son NT, Lee B-O (2022) Efficacy of non-pharmacological interventions to reduce pain in people with dementia: a systematic review and meta-analysis. J Clin Nurs 00:1–14. https://doi.org/10.1111/jocn.16444
Meng X et al (2021) Effectiveness of caregiver non-pharmacological interventions for behavioural and psychological symptoms of dementia: an updated meta-analysis. Ageing Res Rev 71:101448. https://doi.org/10.1016/j.arr.2021.101448
Cohen-Mansfield J (2018) Non-pharmacological interventions for persons with dementia: what are they and how should they be studied? Int Psychogeriatr 30(3):281–283. https://doi.org/10.1017/S104161021800039X
Black BS et al (2019) Unmet needs in community-living persons with dementia are common, often non-medical and related to patient and caregiver characteristics. Int Psychogeriatr 31(11):1643–1654. https://doi.org/10.1017/S1041610218002296
Cunningham C, Macfarlane S, Brodaty H (2019) Language paradigms when behaviour changes with dementia: #BanBPSD. Int J Geriatr Psychiatry 34(8):1109–1113. https://doi.org/10.1002/gps.5122
Wolverson E, Birtles H, Moniz-Cook E, James I, Brooker D, Duffy F (2019) Naming and framing the behavioural and psychological symptoms of dementia (BPSD) paradigm: professional stakeholder perspectives. OBM Geriatrics 3(4):1–1. https://doi.org/10.21926/obm.geriatr.1904080
Michelet M, The Actifcare Consortium (2022) Associations between unmet needs for daytime activities and company and scores on the Neuropsychiatric Inventory-Questionnaire in people with dementia: a longitudinal study. Aging Ment Health 26(4):725–734. https://doi.org/10.1080/13607863.2021.1910792
Cohen-Mansfield J, Thein K, Marx MS, Dakheel-Ali M, Freedman L (2012) Efficacy of nonpharmacologic interventions for agitation in advanced dementia: a randomized, placebo-controlled trial. J Clin Psychiatry 73(9):6057
Gillis K, Lahaye H, Dom S, Lips S, Arnouts H, Van Bogaert P (2019) A person-centred team approach targeting agitated and aggressive behaviour amongst nursing home residents with dementia using the senses framework. Int J Older People Nurs. https://doi.org/10.1111/opn.12269
Berger V, Bour L, Carter K et al (2021) A roadmap to using randomization in clinical trials. BMC Med Res Methodol 21:168. https://doi.org/10.1186/s12874-021-01303-z
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12(3):189–198. https://doi.org/10.1016/0022-3956(75)90026-6
Kat MG, de Jonghe JF, Aalten P, Kalisvaart CJ, Dröes RM, Verhey FR (2002) Neuropsychiatrische symptomen bij dementie: psychometrische aspecten van de Nederlandse Neuropsychiatric Inventory (NPI) [Neuropsychiatric symptoms of dementia: psychometric aspects of the Dutch Neuropsychiatric Inventory (NPI)]. Tijdschr Gerontol Geriatr 33(4):150–155
Cohn MD, Smyer MA, Horgas AL (1994) The AB-C’s of behavior change: skills for working with behavior problems in nursing homes. Venture Pub, State College, PA
Nolan, M.R., Brown, J., Davies, S., Nolan, J. and Keady, J. (2006). The Senses Framework: improving care for older people through a relationship-centred approach. Getting Research into Practice (GRiP) Report No 2. Project Report. University of Sheffield.
Kenda M, Kočevar Glavač N, Nagy M, Sollner Dolenc M (2022) Medicinal plants used for anxiety, depression, or stress treatment: an update. Molecules 27(18):6021. https://doi.org/10.3390/molecules27186021
Mannucci C et al (2018) Clinical Pharmacology of citrus aurantium and citrus sinensis for the treatment of anxiety. Evid-Based Complement Alternat Medicine 2018:18. https://doi.org/10.1155/2018/3624094
Zuidema SU, de Jonghe JF, Verhey FR, Koopmans RT (2007) Agitation in Dutch institutionalized patients with dementia: factor analysis of the Dutch version of the cohen-mansfield agitation inventory. Dement Geriatr Cogn Disord 23(1):35–41. https://doi.org/10.1159/000096681
Wary B (1999) Collectif Doloplus. Doloplus, une échelle pour évaluer la douleur. Soins Gérontologie 19:25–27
Maust D (2022) Ending choose-your-own-adventure care for agitation in dementia. Int Psychogeriatr 34(10):867–869. https://doi.org/10.1017/S104161022200059X
Smith TO, Harvey K (2022) Psychometric properties of pain measurements for people living with dementia: a COSMIN systematic review. Eur Geriatr Med 13:1029–1045. https://doi.org/10.1007/s41999-022-00655-z
Cummings J (2020) The neuropsychiatric inventory: development and applications. J Geriatr Psychiatry Neurol 33(2):73–84. https://doi.org/10.1177/0891988719882102
Belgisch Centrum voor Farmacotherapeutische Informatie (2022) Gecommentarieerd geneesmiddelenrepertorium Federaal Agentschap voor Geneesmiddelen en gezondheidsproducten, Brussel. https://www.bcfi.be/nl
R Core Team (2021) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria
Bao Z, Landers M (2022) Non-pharmacological interventions for pain management in patients with dementia: a mixed-methods systematic review. J Clin Nurs 31(7–8):1030–1040. https://doi.org/10.1111/jocn.15963
Azermai M, Elseviers M, Petrovic M, Van Bortel L, Vander Stichele R (2011) Geriatric drug utilisation of psychotropics in Belgian nursing homes. Hum Psychopharmacol 26(1):12–20. https://doi.org/10.1002/hup.1160
Kirkham J et al (2017) Antipsychotic use in dementia. Can J Psychiatry 62(3):170–181. https://doi.org/10.1177/0706743716673321
Geng F, Stevenson DG, Grabowski DC (2019) Daily nursing home staffing levels highly variable, often below CMS expectations. Health Aff 38(7):1095–1100. https://doi.org/10.1377/hlthaff.2018.05322
Stackpoole M, Hockley J, Thompsell A, Simard J, Volicer L (2015) The namaste care programme can reduce behavioural symptoms in care home residents with advanced dementia. Int J Geriatr Psychiatry 30:702–709. https://doi.org/10.1002/gps.4211
Pélissier C, Charbotel B, Fassier JB, Fort E, Fontana L (2018) Nurses’ occupational and medical risks factors of leaving the profession in nursing homes. Int J Environ Res Public Health 15(9):1850. https://doi.org/10.3390/ijerph15091850
Acknowledgements
The authors thank Dirk Jacobs for the methodological advises, Liesbet Decuypere and Kate Meier for the translation of the non-pharmacological treatments’ definitions and Leen Verduyckt and Sandra Vande Voorde for practical support during data collection. Special thanks to all caregivers from the 23 nursing homes for their extraordinary commitment.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare to have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gillis, K., van Diermen, L., Lahaye, H. et al. Effect of need-based care on behavioural and psychological symptoms in residents with dementia and formal caregivers’ distress in nursing homes: a three-arm cluster randomized controlled trial. Eur Geriatr Med 14, 1083–1096 (2023). https://doi.org/10.1007/s41999-023-00825-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-023-00825-7