Key summary points
We investigated the relationship between walking speed and unexpected hospitalization in community-dwelling older adults with disabilities in activities of daily living.
AbstractSection FindingsIn community-dwelling older people with disabilities in activities of daily living, the amount of change in walking speed over a 3-month period was more strongly associated with unexpected hospitalization than the walking speed at a single time point.
AbstractSection MessageWhen assessing the risk of unexpected hospitalization by walking speed in community-dwelling older adults with disabilities in activities of daily living, it is important to evaluate not only a single point in time, but also changes over time.
Abstract
Purpose
Walking speed is a useful predictor of hospitalization for community-dwelling older people. However, whether it is an effective predictor for disabled older people has not been clarified. This study aimed to investigate the association of walking speed with unexpected hospitalizations in community-dwelling, disabled, older people.
Methods
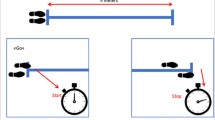
The participants were ambulatory, community-dwelling older adults aged ≥ 65 years with disabilities. Comfortable and maximum walking speeds were measured at two timepoints, baseline and 3 months later. Furthermore, the change over time at 3 months in walking speed was also calculated. If the change in walking speed decreased more than 0.1 m/s, it was defined as walking speed decreased. The primary outcome was unexpected hospitalization during 4-year follow-up. The associations among baseline walking speed, walking speed decline, and hospitalization were analyzed using Cox regression analysis adjusted for potential confounding factors.
Results
A total of 93 people (age 81.8 ± 7.0 years, 64 female) were included, and unexpected hospitalization occurred in 47 people during 4-year follow-up. On Cox regression analysis adjusted for potential confounding factors, only the maximum walking speed decrease was significantly associated with hospitalization (hazard ratio = 2.53, 95% confidence interval: 1.23–5.21), not baseline walking speed and comfortable walking speed decrease.
Conclusion
As for the assessment of walking speed for the prediction of unexpected hospitalization in disabled people, measurement at a single timepoint is not useful, whereas change over time is. Monitoring of change over time in maximum walking speed appears to be one of the indicators for the health management of disabled people.

Similar content being viewed by others
Data availability
The data that support the results of this study are available at reasonable request from the corresponding author.
References
Murakami K, Asayama K, Satoh M, Inoue R, Tsubota-Utsugi M, Hosaka M et al (2017) Risk Factors for stroke among young-old and old-old community-dwelling adults in Japan: the Ohasama study. J Atheroscler Thromb 24(3):290–300. https://doi.org/10.5551/jat.35766
Lloyd-jones DM, Larson MG, Leip EP, Beiser A, D’Agostino RB, Kannel WB et al (2002) Lifetime risk for developing cognitive heart failure: the Framingham heart study. Circulation 106(24):3068–3072. https://doi.org/10.1161/01.cir.0000039105.49749.6f
Lipowsli JZ (1987) Delirium (acute confusional states). JAMA 258:1789–1792
Mizuno M, Kajimoto K, Sato N, Yumino D, Minami Y, Murai K et al (2016) Clinical profile, management, and mortality in very-elderly patients hospitalized with acute decompensated heart failure: an analysis from the ATTEND registry. Eur J Intern Med 27:80–85. https://doi.org/10.1016/j.ejim.2015.08.015
Covinsky KE, Pierluissi E, Johnston CB (2011) Hospitalization-associated disability: “she was probably able to ambulate, but I’m not sure.” JAMA 306(16):1782–1793. https://doi.org/10.1001/jama.2011.1556
Takabayashi K, Iwatsu K, Ikeda T, Morikami Y, Ichinohe T, Yamamoto T et al (2020) Clinical characteristics and outcomes of heart failure patients with long-term care insurance—insights from the Kitakawachi clinical background and outcome of heart failure registry. Circ J 84(9):1528–1535. https://doi.org/10.1253/circj.CJ-20-0017
Freid LP, Guralink JM (1997) Disability in older adults: evidence regarding significance, etiology, and risk. J Am Geriatr Soc 45(1):92–100. https://doi.org/10.1111/j.1532-5415.1997.tb00986.x
Cesari M, Kritchevsky SB, Penninx BWHJ, Nicklas BJ, Simonsick EM, Newman AB et al (2005) Prognostic value of usual gait speed in well-functioning older people—results from the health, aging and body composition study. J Am Geriatr Soc 53(10):1675–1680. https://doi.org/10.1111/j.1532-5415.2005.53501.x
Sabia S, Dumurgier J, Tavernier B, Head J, Tzourio C, Elbaz A (2014) Change in fast Walking speed preceding death: Results from a prospective longitudinal cohort study. J Gerontol A Biol Sci Med Sci 69(3):354–362. https://doi.org/10.1093/gerona/glt114
van Danique Gulick JJ, Sander Perry IB, van der Marike L, van Jolan Beek GM, Cees L, Martijn Stuiver M (2022) A prediction model for falls in community-dwelling older adults in podiatry practices. Gerontology 68(11):1214–1223. https://doi.org/10.1159/000520962
Woo J, Ho SC, Yu AL (1999) Walking speed and stride length predicts 36 months dependency, mortality, and institutionalization in Chinese aged 70 and older. J Am Geriatr Soc 47(10):1257–1260. https://doi.org/10.1111/j.1532-5415.1999.tb05209.x
Hardy SE, Perera S, Roumani YF, Chandler JM, Studenski SA (2007) Improvement in usual gait speed predicts better survival in older adults. J Am Geriatr Soc 55(11):1727–1734. https://doi.org/10.1111/j.1532-5415.2007.01413.x
Dumurgier J, Elbaz A, Ducimetière P, Tavernier B, Alpérovitch A, Tzourio C (2009) Slow walking speed and cardiovascular death in well functioning older adults: prospective cohort study. BMJ 10(339):b4460. https://doi.org/10.1136/bmj.b4460
Perera S, Mody SH, Woodman RC, Studenski SA (2006) Meaningful change and responsiveness in common physical performance measures in older adults. J Am Geriatr Soc 54(5):743–749. https://doi.org/10.1111/j.1532-5415.2006.00701.x
Suzuki Y, Kamide N, Kitai Y, Ando M, Sato H, Shiba Y, Sakamoto M (2019) Absolute reliability of measurements of muscle strength and physical performance measures in older people with high functional capacities. Eur Geriatr Med 10(5):733–740. https://doi.org/10.1007/s41999-019-00218-9
Chen LK, Woo J, Assentachai P, Auyeung TW, Chou MY, Iijima K et al (2020) Asian Working Group for Sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J Am Med Dir Assoc 21(3):300-307.e2. https://doi.org/10.1016/j.jamda.2019.12.012
Satake S, Arai H (2020) The revised Japanese version of the cardiovascular health study criteria (revised J-CHS criteria). Geriatr Gerontol Int 20(10):992–993. https://doi.org/10.1111/ggi.14005
Bohannon RW (1997) Comfortable and maximum walking speed of adults aged 20–79 years: Reference values and determinants. Age Ageing 26(1):15–19. https://doi.org/10.1093/ageing/26.1.15
Callisaya ML, Launay CP, Srikanth VK, Verghese J, Allali G, Beauchet O (2017) Cognitive status, fast walking speed and walking speed reserve—the Gait and Alzheimer interactions tracking (GAIT) study. Geroscience 39(2):231–239. https://doi.org/10.1007/s11357-017-9973-y
Callisaya ML, Blizzard L, McGinley JL, Srikanth VK (2012) Risk of falls in older people during fast-walking—the TASCOG study. Gait Posture 36(3):10–15. https://doi.org/10.1016/j.gaitpost.2012.05.003
Kim HJ, Park I, Lee HJ, Lee O (2016) The reliability and validity of gait speed with different walking pace and distances against general health, physical function, and chronic disease in aged adults. J Exerc Nutrition Biochem. 20(3):46–50. https://doi.org/10.20463/jenb.2016.09.20.3.7
Bohannon RW, Andrews AW, Thomas MW (1996) Walking speed: reference values and correlates for older adults. J Orthop Sports Phys Ther 24(2):86–90. https://doi.org/10.2519/jospt.1996.24.2.86
García AN, Ródenas IH, Molina RG, Grao MCR, Céspedes AA, Víctor ME et al (2020) Gait plasticity impairment as an early frailty biomarker. Exp Gerontol 142:111137. https://doi.org/10.1016/j.exger.2020.111137
Glittenberg CS, Lehmann S, Okada M, Rosen D, Brewer K, Bay RC (2014) Variables explaining health-related quality of life in community-dwelling older adults. J Geriatr Phys Ther 37(2):83–91. https://doi.org/10.1519/JPT.0b013e3182a4791b
Jochem C, Leitzmann M, Volaklis K, Aune D, Strasser B (2019) Association between muscular strength and mortality in clinical populations: a systematic review and meta-analysis. J Am Med Dir Assoc 20(10):1213–1223. https://doi.org/10.1016/j.jamda.2019.05.015
Hermoso AG, Redondo IC, Vélez RR, Ruiz JR, Ortega FB, Lee DC et al (2018) Muscular strength as a predictor of all-cause mortality in an apparently healthy population: a systematic review and meta-analysis of data from approximately 2 million men and women. Arch Phys Med Rehabil 99(10):2100-2113.e5. https://doi.org/10.1016/j.apmr.2018.01.008
Acknowledgements
The authors would like to express their deepest gratitude to the staff of the Department of Rehabilitation at Kitasato Institute Hospital for their support.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures that involved human participants in this study were performed in accordance with the ethical standards of Kitasato Institute Hospital Research Ethics Committee (approval no. 18034) and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained on an opt-out basis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hirai, T., Kamide, N. & Shigeta, K. Decrease in maximum paced walking speed predicts hospitalization in community-dwelling older people with disabilities. Eur Geriatr Med 14, 961–968 (2023). https://doi.org/10.1007/s41999-023-00801-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-023-00801-1