Abstract
Purpose
Narcolepsy is a lifelong condition affecting one person per every 2000 worldwide. It is widely underrecognized and most are not diagnosed until 10–15 years after initial symptom onset. The purpose of this review was to provide an overview on the factors that contribute to the diagnostic delay of narcolepsy along with associated implications for clinicians.
Methods
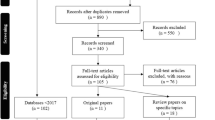
A search of the literature in electronic databases was conducted examining data related to a diagnosis of narcolepsy. Keywords used for the search included ‘diagnosing narcolepsy,’ ‘delayed diagnosis of sleep disorders,’ etc. Of approximately 50 articles, 15 were included in this review for their relevancy and evidence, based on the Strength of Recommendation Taxonomy (SORT) system.
Results
On average, the duration in diagnostic delay was reported to be 7 years. Contributing factors included the absence of cataplexy, lack of awareness and underrecognition, presence of comorbidities and medications, limitations of and lack of consistency in current diagnostic methods, and age of onset.
Conclusions
This review highlighted major contributing factors of the diagnostic delay of narcolepsy. Recommendations for clinicians included the following: (1) learn and disseminate information about narcolepsy and (2) what narcolepsy is NOT, and; (3) employ evidence-based diagnostic procedures and/or refer to specialist.
Similar content being viewed by others
References
Black J, Reaven NL, Funk SE, et al. The burden of narcolepsy disease (bond) study: health-care utilization and cost findings. Sleep Med. 2014;15(5):522–9. https://doi.org/10.1016/j.sleep.2014.02.001 PubMed PMID: 24768358.
Thorpy MJ, Krieger AC. Delayed diagnosis of narcolepsy: characterization and impact. Sleep Med. 2014;15(5):502–7. https://doi.org/10.1016/j.sleep.2014.01.015 PubMed PMID: 24780133.
Overeem S, Reading P, Bassetti CL. Narcolepsy. Sleep Med Clin. 2012;7(2):263–81. https://doi.org/10.1016/j.jsmc.2012.03.013.
Carter LP, Acebo C, Kim A. Patients’ journeys to a narcolepsy diagnosis: a physician survey and retrospective chart review. Postgrad Med. 2014;126(3):216–24. https://doi.org/10.3810/pgm.2014.05.2769 PubMed PMID: 24918805.
Jennum P, Ibsen R, Petersen ER, et al. Health, social, and economic consequences of narcolepsy: a controlled national study evaluating the societal effect on patients and their partners. Sleep Med. 2012;13(8):1086–93. https://doi.org/10.1016/j.sleep.2012.06.006 PubMed PMID: 22841027.
Nevsimalova S, Pisko J, Buskova J, et al. Narcolepsy: clinical differences and association with other sleep disorders in different age groups. J Neurol. 2013;260(3):767–75. https://doi.org/10.1007/s00415-012-6702-4 PubMed PMID: 23070467.
American Academy of Sleep Medicine (AASM). The international classification of sleep disorders-third edition (ICSD-3). Darien: American Academy of Sleep Medicine; 2014.
Ruoff C, Rye D. The ICSD-3 and DSM-5 guidelines for diagnosing narcolepsy: clinical relevance and practicality. Curr Med Res Opin. 2016;32(10):1611–22.
Krahn LE, Hershner S, Loeding LD, et al. Quality measures for the care of patients with narcolepsy. J Clin Sleep Med. 2015;11(3):335. https://doi.org/10.5664/jcsm.4554.
American Psychiatric Association (APA). Diagnostic and statistical manual of mental disorders. 5th ed. VA: American Psychiatric Association; 2013.
Ebell MH, Siwek J, Weiss BD, et al. Strength of recommendation taxonomy (SORT): a patient-centered approach to grading evidence in the medical literature. J Am Board Fam Pract. 2004;17(1):59–67.
Weiss BD. SORT-strength of recommendation taxonomy. Fam Med. 2004;36(2):141–3.
Frauscher B, Ehrmann L, Mitterling T, et al. Delayed diagnosis, range of severity, and multiple sleep comorbidities: a clinical and polysomnographic analysis of 100 patients of the innsbruck narcolepsy cohort. J Clin Sleep Med. 2013;9(8):805–12. https://doi.org/10.5664/jcsm.2926.
Maski K, Steinhart E, Williams D, et al. Listening to the patient voice in narcolepsy: diagnostic delay, disease burden, and treatment efficacy. J Clin Sleep Med. 2017;13(3):419.
Morrish E, King MA, Smith IE, et al. Factors associated with a delay in the diagnosis of narcolepsy. Sleep Med. 2004;5(1):37–41.
Taddei RN, Werth E, Poryazova R, et al. Diagnostic delay in narcolepsy type 1: combining the patients’ and the doctors’ perspectives. J Sleep Res. 2016;25(6):709–15. https://doi.org/10.1111/jsr.12420.
Ueki Y, Hayashida K, Komada Y, et al. Factors associated with duration before receiving definitive diagnosis of narcolepsy among japanese patients affected with the disorder. Int J Behav Med. 2014;21(6):966–70.
Baumann CR, Mignot E, Lammers GJ, et al. Challenges in diagnosing narcolepsy without cataplexy: a consensus statement. Sleep. 2014;37(6):1035–42. https://doi.org/10.5665/sleep.3756.
Rosenberg R, Kim AY. The AWAKEN survey: knowledge of narcolepsy among physicians and the general population. Postgrad Med. 2014;126(1):78–86. https://doi.org/10.3810/pgm.2014.01.2727 PubMed PMID: 24393754.
Dunne L, Patel P, Maschauer EL, et al. Misdiagnosis of narcolepsy. Sleep Breath. 2016;20(4):1277–84. https://doi.org/10.1007/s11325-016-1365-5.
Jennum P, Ibsen R, Knudsen S, et al. Comorbidity and mortality of narcolepsy: a controlled retro- and prospective national study. Sleep. 2013;36(6):835–40. https://doi.org/10.5665/sleep.2706.
Jara CO, Popp R, Zulley J, et al. Determinants of depressive symptoms in narcoleptic patients with and without cataplexy. J Nerv Ment Dis. 2011;199(5):329–34. https://doi.org/10.1097/nmd.0b013e3182174fd3 PubMed PMID: 21543952.
Black J, Reaven NL, Funk S, et al. High rates of medical comorbidity in narcolepsy: findings from the burden of narcolepsy disease (BOND) study of 9,312 patients in the United States. Sleep. 2013;36:A249.
Bayard S, Croisier Langenier M, Cochen De Cock V, et al. Executive control of attention in narcolepsy. PLoS One. 2012;7(4):e33525. https://doi.org/10.1371/journal.pone.0033525.
National Institute of Neurological Disorders and Stroke (NINDS). Narcolepsy fact sheet. MD: National Institutes of Health; 2015.
Vignatelli L, Plazzi G, Peschechera F, et al. A 5-year prospective cohort study on health-related quality of life in patients with narcolepsy. Sleep Med. 2011;12(1):19–23. https://doi.org/10.1016/j.sleep.2010.07.008 PubMed PMID: 20851047.
Hughes S, Finnegan T, Ullman S, et al. Online medical education improves knowledge and competence in the management of clinically challenging cases of narcolepsy among neurologists (P3. 063). Neurology. 2017;88(16 Supplement):P3–063.
Ohayon MM. Narcolepsy is complicated by high medical and psychiatric comorbidities: a comparison with the general population. Sleep Med. 2013;14(6):488–92. https://doi.org/10.1016/j.sleep.2013.03.002 PubMed PMID: 23643648.
Walters AS, Silvestri R, Zucconi M, et al. Review of the possible relationship and hypothetical links between attention deficit hyperactivity disorder (ADHD) and the simple sleep related movement disorders, parasomnias, hypersomnias, and circadian rhythm disorders. J Clin Sleep Med. 2008;4:591–600.
Thorpy MJ, Dauvilliers Y. Clinical and practical considerations in the pharmacologic management of narcolepsy. Sleep Med. 2015;16(1):9–18. https://doi.org/10.1016/j.sleep.2014.10.002 PubMed PMID: 25458251.
Ahmed I, Thorpy M. Clinical features, diagnosis and treatment of narcolepsy. Clin Chest Med. 2010;31(2):371–81. https://doi.org/10.1016/j.ccm.2010.02.014 PubMed PMID: 20488294.
Flygare J, Parthasarathy S. Narcolepsy: let the patient’s voice awaken us! Am J Med. 2015;128(1):10–3. https://doi.org/10.1016/j.amjmed.2014.05.037.
Kim LJ, Coelho FM, Hirotsu C, et al. Frequencies and associations of narcolepsy-related symptoms: a cross-sectional study. J Clin Sleep Med. 2015;11(12):1377.
Funding
There are no funding sources to report for this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed in a significant way to the manuscript and have read and approved the final version.
Corresponding author
Ethics declarations
Conflict of Interest
The authors report no conflicts of interest.
Rights and permissions
About this article
Cite this article
Bhattarai, J., Sumerall, S.W. Diagnostic Delay of Narcolepsy: Contributing Factors and Implications for Clinicians. Sleep Vigilance 2, 103–109 (2018). https://doi.org/10.1007/s41782-018-0046-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41782-018-0046-9