Abstract
Introduction
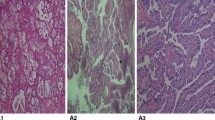
Serous ovarian carcinomas (SOCs) are the commonest epithelial ovarian carcinomas (EOCs). EOCs are subdivided into low-grade serous ovarian carcinomas (LGSOCs) or type 1 and high-grade serous ovarian carcinomas (HGSOCs) or type 2. LGSOC are less common, occur at a younger age, have a better prognosis and are relatively chemoresistant. LGSOC have a higher expression of estrogen receptors (ER) and progesterone receptors (ER-PgR) and are said to be hormone sensitive. Studies have shown higher PgR positivity in LGSOC than in HGSOC. Literature states that the number of ER reduces in ovaries immediately after menopause, whereas PgR receptors persist for some time.
Method
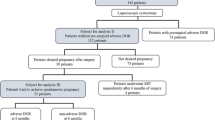
Receptor (ER-PgR) profile of 157 women (out of 202 women with diagnosed or suspected ovarian malignancy) with EOC (both LGSOC and HGSOC) who were treated at a tertiary care cancer hospital over a period of two years was retrospectively collected and analyzed. The ER-PgR profile of these women was also studied in relation to early and late menopausal period.
Result
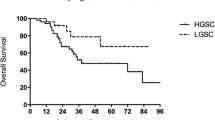
Analysis showed that ER-PgR profile was different for LGSOC and HGSOC. It was also found that the profile of hormone receptors and their ratio was different in early and late menopausal period keeping other variables constant.
Conclusion
LGSOC occurs in comparatively younger women and is mostly diagnosed in early postmenopause, i.e., within five years of menopause. Apart from showing a definite pattern, the ER-PgR ratio is also altered during this period. It can therefore be concluded that the altered ER-PgR ratio might be responsible for pathogenesis of LGSOC rather than absolute numbers or percentages of estrogen and progesterone receptors. This can lead to an alteration in the hormone therapy protocol for management of LGSOC if proven in further research.



Similar content being viewed by others
References
Brodowska A, Starczewski A, Laszczyñska M, Szydowska I. Ovarian androgenesis in women after menopause. Pol Merkuriusz Lek. 2005;19:90–3.
Konstantinos P, Mara S, Agni P, Ri Anna, Petroula T, Nikolaos N, et al. A case series on natural conceptions resulting in ongoing pregnancies in menopausal and prematurely menopausal women following platelet-rich plasma treatment. Cell Transp. 2019;28(9–10):1333–40. https://doi.org/10.1177/0963689719859539.
Fang S, Xuyin Z, Yiqun Z, Jingxin D, Qi C. Hormone receptors expression in ovarian cancer taking into account menopausal status: a retrospective study in Chinese population. Oncotarget. 2017;8(48):84019–27. https://doi.org/10.18632/oncotarget.20251.
Slotman BJ, Nauta JJ, Rao BR. Survival of patients with ovarian cancer apart from stage and grade, tumor progesterone receptor content is a prognostic indicator. Cancer. 1990;665:40–744.
David MG, Diane CB, Robert LC, Karen HL, Anais M, Charlotte CS. Hormonal maintenance therapy for women with low-grade serous cancer of the ovary or peritoneum. J Clin Oncol. 2017;35(10):1103–11. https://doi.org/10.1200/JCO.2016.71.0632.
Peey-S K, Philip B, Rachel L, Peter G, Tony B, James S. PARAGON (ANZGOG-0903): a phase 2 study of anastrozole in asymptomatic patients with estrogen and progesterone receptor-positive recurrent ovarian cancer and CA125 progression. J Gynecol Oncol. 2019;30(5): e86. https://doi.org/10.3802/jgo.2019.30.e86.
Jorge E, Alexander CK, Michelle D, Pamela C, Jill GN, Gregg SN. Quantification of ER/PR expression in ovarian low-grade serous carcinoma. Gynecol Oncol. 2013;128(2):371–6. https://doi.org/10.1016/j.ygyno.2012.10.013.
Fernandez ML, et al. Hormone receptor expression and outcomes in low-grade serous ovarian carcinoma. Gynecol Oncol. 2020;157(1):12–20.
Matthew H, Marian MD, Frank Mc C, Martin MM. Targeting RAF kinases for cancer therapy: BRAF mutated melanoma and beyond. Nat Rev Cancer Nat Rev Cancer. 2014;14(7):455–67. https://doi.org/10.1038/nrc3760.
Harding M, Cowan S, Hole D, Cassidy L, Kitchener H, Davis J, Leake R. Estrogen and progesterone receptors in ovarian cancer. Cancer. 1990;65(3):486–91.
Marta LF, Amy D, Hannah K, Nicole L, Holly R, Maegan B. Hormone receptor expression and outcomes in low-grade serous ovarian carcinoma. Gynecol Oncol. 2020;157(1):12–20. https://doi.org/10.1016/j.ygyno.2019.11.029.
Brett MR, Jennifer BP, Thomas AS. Epidemiology of ovarian cancer: a review. Cancer Biol Med. 2017;14(1):9–32. https://doi.org/10.20892/j.issn.2095-3941.2016.0084.
Voutsadakis IA. A systematic review and meta-analysis of hormone receptor expression in low-grade serous ovarian carcinoma. Eur J Obstet Gynecol Reprod Biol. 2021;256:172–8.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
patni, R., sethi, N. Low Grade Serous Ovarian Cancer: Is disturbed Receptor Ratio (ER: PgR) an Etiogenic Factor?. Indian J Gynecol Oncolog 19, 94 (2021). https://doi.org/10.1007/s40944-021-00556-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40944-021-00556-2