Abstract
This article, co-authored by a psoriatic arthritis (PsA) patient and a physician who regularly encounters and treats PsA patients, discusses the patient’s experience of living with the disease, from diagnosis through living with the disease day-to-day and other people’s reactions to their treatment experiences and responses. The physician adds to this by providing his experiences in treating PsA with biologics, and the importance of patients working together with their rheumatologists to maximize the efficacy of treatments and improve patients’ quality of life.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Patient’s Experience
Growing up in a small town in Texas, I heard the phrases “Push through the pain” and “Walk it off” many times. At that time, the source of the pain was some rigorous task or a sports injury. I am now 42 years old and I have to mentally repeat those phrases to myself daily. However, the source of the pain has now changed to psoriatic arthritis (PsA).
I was diagnosed with severe plaque psoriasis at the age of 7 after recovering from chickenpox. I have been on just about every medication available since 1980. I have used coal tar creams, light therapy, sulfur-based oral pills, steroid creams, immunosuppressive biologic injections, and, most recently, anti-inflammatory oral medication.
My first bad flare-up of PsA happened 5 years ago and was likely delayed because of the biologic medication used to treat my skin. My skin was almost clear and my dermatologist and I decided to transition back to a topical treatment. It was about a month after that transition that I noticed my hips were starting to get stiff and sore. My hands, knees, and ankles soon developed the same pain and stiffness. My co-workers started making comments that I had a noticeable limp and wanted to know if everything was okay. A rheumatologist confirmed that I have PsA and suggested that I return to using biologics.
Life with PsA has been a struggle, to say the least. Stereotypically, arthritis is supposed to be something that people over 60 have to deal with, not people in their thirties. I now understand and appreciate the TV commercials for over-the-counter medications with arthritis-friendly caps. I can usually do as much walking as I want, but strenuous exercise is not possible. I recently visited the Texas State Fair and noticed that after taking around 15,000 steps, my joints started to burn, swell, and get stiff.
I have always been a strong man. Words like “can’t” and “unable” are not in the dictionary to describe myself. My parents have always told me that I can do anything if I have the desire and drive to do so. Now, a pickle jar is one of my worst enemies and I often have to ask for help. I know I cannot get out in the yard with my nephews and play football. I volunteer for several different organizations in my town and I have to give serious consideration before I accept any request for physical assistance. That is not how I would prefer to live. I can accept and deal with the emotional baggage that comes with my own physical limitations. However, the part that is the hardest is having people call me lazy because I cannot keep up with them or have to turn down their request for help. They do not understand the pain and what my limitations are. After explaining why I cannot help or keep up, some understand and are nice about it but never ask for my help again. Others are just rude and continue to call me lazy because “you just don’t want to help” or “you’re faking it.” As someone who has been so self-sufficient and independent my entire life, that hurts me deeper than anything. I would love to help everyone with everything, but my “new normal” with PsA keeps me from doing so.
Many readers with arthritis will most likely be able to connect with all I have written. I also acknowledge that many of you have had exponentially more difficult struggles. I would like to encourage those of you in this category to keep fighting. Please educate those around you about your own struggles. When someone offers to help, please let them do so. I would also encourage you to become your doctor’s biggest cheerleader. If you notice that your treatment is helping, even though you may not be back to 100 %, send them a note or call and thank them. Your doctor is also a person and cares enough about you that they went to school to have the chance to treat your condition. I can say with certainty that my dermatologist and I are a team when it comes to my treatment. I am always looking for new treatments and she is open to discuss anything I bring to her. If after her own research she does not think the treatment would be best for me, she explains why instead of just saying no.
For the doctors reading this, I say thank you. You may see patients every day who act like they do not care, but what you do matters. I pray that each one of you never arrives at a point where you are so busy and burned out that you become callous and stop caring. Many of us who struggle with PsA only pour out our aches and pains because you are the source of our relief. We may not tell or trust anyone else to understand. Finally, put the iPad or chart aside, smile, and listen to your patients. We greatly appreciate it. You will find us all to be much happier when we feel we have been heard.
Physician’s Perspective
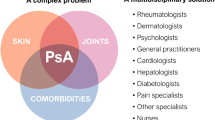
The patient’s experience brings up a great number of salient points worth further discussion. PsA occurs in an estimated 15–35 % of patients with psoriasis and typically, as in this patient, occurs years after the onset of the psoriatic lesions. Whether the development of this patient’s arthritis component was delayed because of his use of biological therapy is unclear; it may have been, as the patient suggests, depending on the type of biologic therapy used (not all biologic therapy is very effective for PsA) or he could have experienced the natural history of disease. Involvement of the hips as the first manifestation of PsA is somewhat unusual: the patient may well have had entheseal involvement, rather than true joint involvement, as the first manifestation of systemic involvement of PsA (rather than synovitis) which is not uncommon.
As the patient points out, the stereotype of “arthritis” is that it occurs almost exclusively in older patients who are considered senior citizens. While this may be somewhat true of osteoarthritis, although many patients with this disorder are younger than 60, it is not true of patients with inflammatory arthritis or systemic rheumatic diseases such as PsA, ankylosing spondylitis, systemic lupus erythematosus, rheumatoid arthritis, scleroderma, gout, etc., which typically have their first manifestations in younger individuals initially occurring at any time from their teens into their fifties.
It is imperative that a patient with PsA this active sees a rheumatologist for management of their PsA. It is not uncommon for a dermatologist and rheumatologist to co-treat a patient, but, the rheumatologist is usually much more aggressive with respect to treatment of the systemic manifestations of disease, including the joints.
The patient describes very well what I hear every day as a rheumatologist; the major difficulties that patients have with their systemic inflammatory arthritis is not necessarily the pain and stiffness in joints but the frustrations with their inability to do normal activities of daily living and the inability of others to understand why they are limited; this can be the most depressing part of their arthritis.
This patient makes a very valuable point to individuals with inflammatory arthritis which all should take to heart: patients with disabilities secondary to an inflammatory arthritis, who refuse to let the discomfort and disability control them, but who do as much as they can in spite of their discomfort and limitations, are much more productive, accomplish more, are more self-sufficient and are happier than those who let their limitations and pain control them.
Almost all rheumatologists are very vested in treating patients with inflammatory arthritis and have great satisfaction when their patients do well. Most rheumatologists would like to dispense with having to work on the computer or iPad and be able to look at the patient during their visit; this has been a major change in the practice of medicine over the past 5 years in the United States. It has led to a marked loss of efficiency by the physician and a loss in face-to-face contact of the patient and physician with some deterioration of patient–physician relationship. These changes have been forced on physicians by our elected officials and the insurance industry and are now Federal law. As much as many physicians would like to go back to the days when there was a true patient–physician relationship, with no interference of computers, this is unlikely to happen as we have gone down the road too far. In spite of this, almost all physicians still listen as well as they did previously; it just is not as obvious to the patient.
PsA can be treated and patients with PsA can be productive members of society. It is a partnership.
Acknowledgments
The patient would like to thank the National Psoriasis Foundation for their efforts. Technical assistance with editing and styling of the manuscript for submission was provided by Complete Healthcare Communications, LLC, and was funded by Novartis Pharmaceuticals Corporation who had no influence on the content. Dr Fleischmann has no acknowledgments and did not receive technical assistance. The authors are fully responsible for all content and editorial decisions and received no financial support or other form of compensation related to the development of this manuscript. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published. The opinions expressed in the manuscript are those of the authors. No funding was received for publication of this article.
Disclosures
Alan Simmons and Roy Fleischmann have nothing to disclose.
Compliance with Ethics Guidelines
This article does not contain any new studies with human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Simmons, A., Fleischmann, R. Living with Psoriatic Arthritis: A Patient’s and Physician’s Perspective. Rheumatol Ther 3, 1–4 (2016). https://doi.org/10.1007/s40744-015-0024-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40744-015-0024-9