Abstract
Deteriorated functioning is a part of the clinical-high risk (CHR) criteria for psychosis. Diminished social, educational and occupational functioning in the phase of late adolescence and early adulthood are associated with long-term social, economic and health consequences, which stresses the importance of early intervention to stimulate functioning. This pilot study examines the effectiveness and feasibility of the choose-get-keep model of Supported Education and Supported Employment (SEE) to improve educational and occupational functioning of individuals at CHR for a psychosis. A single blind randomized controlled pilot study combined SEE with treatment as usual (TAU) versus TAU among adolescents and early adults at CHR. School performance and job status as well as global functioning scales were assessed at twelve months. Of the 78 eligible participants, 20 individuals consented to participate in this study. At follow-up, participants in the intervention condition (n = 9) did not start an education more often than the participants in the control condition (n = 11) and the school results for both conditions were similar. However, in the intervention condition there were no school dropouts, more participants gained a job and worked longer hours. Two participants quit the intervention. This pilot study provides preliminary evidence that a SEE intervention is effective and feasible in sustaining and improving the level of both educational and occupational functioning of individuals at CHR for psychosis by supporting them in attaining, keeping and elaborating of their education or employment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Early or first-episode psychosis exists when a person first meets the full criteria for a psychotic episode (Nordic Alliance on Mental Illnesses 2016). In the past decades, cumulative evidence has shown that people at heightened risk for psychosis can be detected before the onset of a psychotic episode (Yung et al. 2005). Individuals at Clinical High Risk for Psychosis (CHR-P) are between 14 and 35 years old and either have a genetic risk (a first-degree relative with a psychotic disorder or a schizoid personality disorder), display subclinical psychotic symptoms, or have experienced a brief psychotic episode with spontaneous remission within one week. A second criterion for CHR-P is a deterioration in social, educational, and occupational functioning in the past twelve months or a sustained low level of functioning of at least one year measured with the Social and Occupational Functioning Scale (Yung et al. 2005; Goldman et al. 1992). Social, educational, and occupational engagement is an important outcome variable in CHR-P, given its relationship with future social economic status and health problems (Gutiérrez-García et al. 2017). A longitudinal study involving 111 individuals with a mean age of 18 years (SD = 4.9) revealed that the level of social, educational, and occupational engagement of individuals at CHR-P, who do not develop a psychotic episode at 1- and 2-year follow-up, remained lower than the mean level of social, educational, and occupational engagement in the general population (Addington et al. 2011).
In line with this finding, several studies state that prolonged impairment in social, educational, and occupational engagement is one of the main issues in the treatment of individuals at CHR-P, regardless of transition to psychosis (Cotter et al. 2014; Jang et al. 2011).
Social, educational, and occupational engagement relates to different roles in life. In the 14–35 age group, choosing, getting, and keeping education or a job are essential (Humensky et al. 2019). The NICE guideline for psychotic disorders recommends that mental health services should assist CHR-P individuals to engage with employment or education, however there is no indication about which intervention should routinely be employed (NICE 2014). Tognin and colleagues compared the current practice around of the provision of education and employment support at the Outreach and Support in South London (OASIS) Service, one of the oldest and largest EDP services in Europe and worldwide, to the NICE guidelines and the IPS principles (Tognin et al. 2019). They concluded that the focus should be broadened to include interventions that selectively target vocational and educational recovery. Interventions like Individual Placement and Support may be helpful in order to help young people with their vocational goals (Killackey et al. 2017).
Although the NICE guidelines recommend to offer interventions that stimulate participation for people with a CHR-P, there are only a few studies available on the implementation of evidence based interactions in order to improve vocational and education engagement. Since many early detection teams are searching for appropriate interventions in order to improve vocational and education engagement in CHR-P individuals, this study aims to describe the acceptability and feasibility, as well as the results of a pilot study on Supported Education and Supported Employment.
Supported Education and Supported Employment (SEE)
Several Supported Education and Supported Employment interventions (SEE intervention) (i.e. Individual Placement and Support) particularly target to improve educational and occupational engagement (Danley et al. 1992; Drake et al. 2012; Ellison et al. 2018; Kane et al. 2016; Killackey et al. 2019; Mowbray et al. 2005; Mueser et al. 2015; Sullivan et al. 1993; Unger 1998; Humensky et al. 2019). The SEE intervention of Boston Psychiatric Rehabilitation Approach (PRA) was introduced in the Dutch Mental Health Care system in 1992 and has been widely used since then (Swildens et al. 2011). The principles of the SEE intervention are the same as Individual Placement and Support (IPS) (Drake et al. 2016). Both interventions support people in their efforts to achieve steady and meaningful employment in mainstream competitive job.
The SEE intervention is the process of assisting students/clients to acquire and to use the skills, support, and resources necessary to be successful and satisfied in the educational or occupational environment of their choice (Anthony et al. 2002). The SEE intervention has been implemented and investigated in older participants (i.e. middle adulthood) with prolonged severe mental illnesses, such as schizophrenia and mood disorders (Unger 1998). However interventions that stimulate educational and occupational development are particularly important for individuals in their late adolescence or early adulthood. It is to be expected that a population with relatively mild mental disorders, such as individuals at CHR-P, who have not completely dropped out of school or only recently withdrew from their job, may therefore profit from an intervention such as SEE to prevent further social decline (NICE 2014). The aim of this pilot study is to investigate the effectiveness and feasibility of the SEE intervention for maintaining and improving academic and occupational development in young individuals at CHR-P.
Method
Setting
This study was conducted at the Early Detection service of the community mental health centre Friesland Mental Health Care Service in the Netherlands, funded by Dutch health insurance companies. Annually, around 60 individuals are treated at the Early Detection service, mainly Caucasian people between 14 and 35 years old. Clients were offered the SEE intervention right from the start of the treatment for CHR-P.
The medical ethics committee granted dispensation (METc2013/468), because the SEE intervention was in addition to the treatment as usual (TAU), and recommended by clinical guidelines (NICE Guidelines 2014; Veling et al. 2017). Written informed consent was obtained from the participants by a research assistant, as well as parental or guardian’s consent for participants under the age of sixteen. The study was registered in the Dutch trial register (NTR3669).
SEE Intervention
The SEE intervention is an individualized instruction and support program delivered by a vocational therapist, who assists people with psychiatric disorder to obtain educational and employment goals (Hofstra and Korevaar 2016; Korevaar 2015; Sullivan et al. 1993; Unger 1998). The vocational therapists, who were trained in the intervention, were not involved in the TAU interventions. Therefore, they were not part of the multidisciplinary team meetings.
The SEE intervention consists of three phases: choose, get, and keep. The aim of the ‘choosing phase’ is to select an education, training programme, or employment that is compatible with the participant’s values, skills, and learning needs. The ‘getting phase’ aims to secure admission to a preferred educational or vocational training program or employment. The aim of the ‘keeping phase’ is to remain in school or employed and to increase the participants’ success and satisfaction through enhancement of the participant’s skills and by providing support.
At the start of the intervention, the participant enters into the phase which is relevant for their own situation. The key element of the intervention is that the participant is in the lead with regard to the pace (i.e. frequency of sessions, time spent in each phase) and route of the process. The vocational therapists act as facilitator and offers support if needed (Sanches et al. 2018). Progression to the next phase follows when the goal of the current phase is achieved. The SEE intervention assumes customization, the intervention can be as intensive as needed and also as long as needed (Hofstra and Korevaar 2016; Korevaar 2015; Sullivan et al. 1993; Unger 1998).
Treatment as Usual
TAU was given by the Early Intervention of Psychosis team, a multidisciplinary team with 15 team members for people with CHR-P. TAU contained monitoring of the subclinical psychotic symptoms and psycho education. Moreover, every three months, supportive counselling was provided by a nurse, focusing on encouraging the participants to remain in or restart an education or a job. The vocational therapists had no role in the treatment as usual.
Optionally, participants received indicated Cognitive Behavioural Therapy for people with a Clinical High Risk, targeting subclinical psychotic symptoms (Van Der Gaag et al. 2013).
Design
The study was a single blind randomized controlled pilot study of the SEE intervention, focussing on Supported Education and Supported Employment combined with TAU versus TAU. A research nurse, blind to the participant’s treatment, conducted the assessments at baseline and at the twelve-month follow-up.
Eligibility and Recruitment
Regardless of their initial reasons to seek help, all new referrals (who were between 14–35 years old) of Friesland Mental Health were routinely screened with the Prodromal Questionnaire (PQ-16) (Ising et al. 2012), a 16-item self-assessment screening scale for subclinical psychotic symptoms. Individuals who scored above the cut-off of six or higher received an in-depth assessment with the semi-structured Comprehensive Assessment of At Risk Mental State interview (CAARMS; Yung et al. 2005) to determine whether they met the criteria for CHR-P. Supplementary to the treatment for their primary mental disorder, individuals at CHR-P received add-on symptom monitoring, psychoeducation and the indicated CHR-P intervention of Cognitive Behavioural Therapy (CBT-CHR) (NICE Guidelines 2014). Inclusion criteria were: (1) CHR-P status; (2) age 14–35; (3) sufficient mastery of the Dutch language; (4) a wish for enrolment in an educational program or attainment of employment; and (5) difficulties with education or employment. The inclusion enrolment period was between January 2013 and December 2014.
Description of Measures
CAARMS and SOFAS
The Comprehensive Assessment of At Risk Mental State interview (CAARMS) is a semi-structured interview that predominantly assesses the intensity and frequency of subclinical psychotic symptoms to identify people with a Clinical High Risk for Psychosis (CHR-P) (Yung et al. 2005). An individual meets the criteria for CHR-P in case of either subclinical psychotic symptoms, a brief psychotic episode with spontaneous remission within a week, or a genetic risk for psychosis, each combined with a deterioration in functioning in the past year. Functioning was determined by the Social and Occupational Functioning Assessment Scale (SOFAS), a scale that assesses the impact of physical and mental impairments on multiple areas of social functioning, such as education, employment, family and friends (Goldman et al. 1992). The scale ranges from 1 (extreme severe dysfunction) to 100 (superior functioning), and a score of 50 or lower is considered significant impaired functioning. The CAARMS and SOFAS are the gold standards to determine an CHR-P status in the Netherlands (Veling et al. 2017).
Global Functioning- Social and Global Functioning Role Scale (GF-S and GF-R)
Particularly developed for individuals at CHR-P, the Global Functioning–Social (GF-S) and Global Functioning–Roles scales (GF-R) (Cornblatt et al. 2007) assess social and global engagement on a more detailed level. The GF-R assesses an individual’s primary role, which can be either as an employee, student, or housewife. The GF-S rates an individual’s social functioning. Both scales range scores from 1 to 10, with 1 indicating severe functional impairment and 10 representing superior functioning. A score of 5 or lower indicates serious impairment. The reported inter-rater reliabilities are high, both scoring above 0.75 (P < 0.01) (Cornblatt et al. 2007).
Key Behavioural Indicators
At baseline and at follow-up, the participant’s then education and occupation was examined. Educational results (i.e. completed (almost) all subjects, attended classes yet failed exams, or did not attend classes at all and failed exams) and/or type of occupation (i.e. regular, supported, voluntary), as well as number of working hours per week were recorded by the therapists.
Therapists
The two vocational therapists both worked in the early intervention psychosis team, which the early detection team that treats individuals with CHR-P is a part of. Until then, both therapists only treated clients with first-episode psychosis in order to improve their occupation and had no experience in treating people with CHR-P. Both therapists are trained Boston PRA rehabilitation experts. They received an additional SGK training (16 h) and supervision (72 h).
The SEE fidelity assessment, using the Psychiatric Rehabilitation Fidelity Questionnaire (Luyten et al. 2004), was applied to assess the treatment fidelity. At the end of the study, each vocational therapist was interviewed by a research assistant about one randomly selected participant who received at least three sessions of SEE intervention. The research assistant rated the therapists’ execution of the intervention on 25 items regarding specific elements of the intervention (e.g. goal setting, functional, and resource assessment plus interventions), as well as general elements (e.g. contact with participant, rehabilitation plan). Each item was scored either a zero (not applied), a one (partly applied), or a two (completely and correctly applied). Total scores per therapist ranged from 0 to 30 (insufficient), 30 to 40 (fair), and 40 to 50 (good application).
Analyses
Descriptive Analyses
Feasibility was studied in concordance with the framework of feasibility studies described by the UK National Health Care Institute (Eldridge et al. 2016), which contains examination of the number of eligible participants, the follow-up rates of the intervention and drop-out, and the follow-up response rates to assessments.
Quantitative Analyses
Treatment outcome data were analysed using in SPSS 25.0 (Corp. 2015). Considering the pilot nature of the study, the analysis concentrated on confidence intervals and effect sizes, rather than statistical significance of findings. Using an effect size calculator (Becker 2000) we computed Pearson’s correlation coefficient (rYλ = d/√ (d2 + 4)) to assess the strength of the effect of the SEE intervention. It is widely accepted that an r value of 0.10 indicates a small effect, 0.30 a medium effect, and 0.50 a large effect (Field 2013). However, Cohen’s d is often reported in psychosocial intervention literature, therefore we estimated both r and d (d = M1–M2/σpooled, where σpooled = √[(σ12 + σ22)/2]).
Results
Baseline Data
A total of 20 individuals at CHR-P were included in the study, all of Caucasian origin, 19 females (95%), one male (see Table 1. for the baseline characteristics of the sample). The participant’s mean age was 21.7 years old (SD = 6.3).
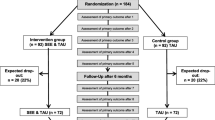
Nine participants were randomized to the SEE intervention, and the other eleven participants received TAU. All participants received one or two CHR for psychosis-focused psychoeducation sessions, yet none of the individuals desired indicated CBT-CHR for psychosis. A flowchart of the study is presented in Fig. 1.
Participation
Initially, 78 eligible subjects were approached for participation in the study, mainly female (60%) with a mean age of 23,4 years (SD 6.9). 49.4% (n = 39) did not participate due to external factors (out of care (n = 14), participation declined by therapist (n = 1), participation declined by parents (n = 1), not meeting the UHR criteria anymore (n = 15), transition to psychosis (n = 5), erroneous inclusion (n = 3)), 24.3% (n = 19) actively declined participation, and the remaining 25.6% (N = 20) agreed to participate (see Fig. 1).
The individuals randomized to the SEE intervention attended a mean number of 12.8 one-hour sessions (SD 9.4). Individuals that remained in school received support in the ‘keeping phase’ for two months up to one year. These participants were slightly younger than those who wanted to keep or get a job. Most of the participants completed the SEE intervention (67%) and the assessments (65%).
Two participants dropped out of the intervention after the initial session and, despite several attempts to contact them, both their reasons for quitting as well as functional outcome remained unknown.
One individual took a time-out from the intervention because she started a reintegration program on her own at her previous occupation. After quitting the intervention, she soon contacted the therapist with a request to restart in order to keep her occupation. In the TAU condition, 64% (n = 7) completed the assessments. Reasons for dropping out were out of care, unwillingness to proceed, and loss of contact.
Fidelity
Both occupational therapists scored 39 and 42 points on the fidelity scale, indicating fair application of the intervention (Luyten et al. 2004).
Effectiveness of the SEE Intervention
Starting Phase
All participants with an occupation also explored whether there were options for attaining a higher level of education or making a career switch. However, due to financial issues, debts, and job hunt requirements to secure the eligibility of welfare, enrolment and attainment of an education was not feasible for three participants. For these three, the focus of the intervention therefore was on finding or keeping a job.
Some participants started in the ‘choosing phase’: investigating a new education or occupation, whereas others began in the ‘keeping phase’ in order to keep their education or occupation. Interestingly, as part of the intervention all individuals in the SEE intervention condition started at investigating and finding additional (part-time) occupations. Consequently, at follow-up, there was no increase in educational participation in the SEE intervention condition and the educational results were comparable in both conditions.
Education
In the TAU condition, two individuals (40%) quit their education, whereas all participants in the intervention condition continued their education (100%) (see Table 2).
Employment
Regarding employment, also shown in Table 2, in the TAU condition, both the occupational participation and amount of working time decreased between baseline and follow-up from eight to seven hours a week. However, the occupational participation in regular work of individuals in the SEE intervention increased by 66% after the intervention from 9.7 to 16.2 h a week. Moreover, the number of working hours at follow-up in the intervention condition increased with 67% in comparison to baseline measurement.
Role, Social, and General Engagement
The participants in both conditions had comparable scores at baseline regarding role, social, and general engagement and all subjects show an improvement of engagement at follow-up (see Table 3). This improvement was most remarkable in the assessment of role functioning, whereby participants in the SEE intervention condition scored higher than in the TAU condition (r = 0.392), indicating a moderate effect. Assessment of social (r = 0.313, d = 0.613) and global functioning (r.297, d = 0.613) show a similar, yet less marked, improvement.
Discussion
To our knowledge, this is the first pilot study examining the effectiveness and feasibility of a specific SEE intervention for individuals at CHR for psychosis. This study shows that individuals at risk for a psychotic episode can profit from a SEE intervention, resulting in an improved occupational and a sustained educational level of engagement. However, the small sample size does call for a careful interpretation.
In comparison to participants in the TAU condition, participants receiving a SEE intervention were more often employed and worked for longer hours. Regarding education, fewer participants quit their education in the SEE intervention condition, although the SEE intervention did not result in higher educational attendance.
In general, all participants showed an increase in engagement in work and school activities at follow-up, assessed with both general and specific measurements, which could be explained by the fact that in both conditions there is specific attention for (re)gaining the educational and occupational roles. During the supportive counselling sessions, the participants in the TAU condition were only encouraged to remain in or restart school or work. However, compared to the TAU condition, the participants who received the SEE intervention exhibit a higher level of engagement in work and school activities, especially with regard to role functioning, at twelve months follow-up. It could be stated that support and advice itself can motivate and help individuals at CHR for psychosis to invest in regaining their social roles, an aspect that is very important during this phase of life (Korevaar and Hofstra 2017). However, a specific intervention such as SEE can help individuals to reach a higher level of educational and vocational engagement. Since the CHR-P individuals are young and likely to be in education or in the process of securing their first (paid) job, they are experiencing less cognitive and clinical symptoms than people who have experienced a first episode of psychosis and an intervention. As SEE can address risk factors that impact clinical outcomes, they are the ideal target group for this intervention (Davies et al. 2018). In doing so, it is important that it is an intervention that is tailored to the individual and his developmental phase, just as this has been done with IPS (Ellison et al. 2015).
According to current CHR-P criteria, either a period of lower functioning of more than twelve months or a functional deterioration in the past year for at least one month is required (Yung et al. 2005). As a result, all engaged participants were engaged in school and work activities at a relatively low level at the inclusion of the study and, as such, a so-called regression to the mean effect can occur. This effect refers to the tendency of second measures to be closer to the average when the initial assessments were extreme, which can confound the potential effects of an intervention. Nevertheless, even though the included participants all were engaged in school and work activities at a low level, the improvement of engagement is more striking in the participants who received the SEE intervention.
A specific intervention such as SEE can help individuals to reach a higher level of functioning. The point of a multidisciplinary integrated approach like the SEE intervention in this study is to prevent young people from being left behind. This is of great importance, as many individuals at CHR-P functioning remain impaired, regardless of symptomatic remission or transition to full-threshold psychosis (Addington et al. 2011). By keeping young people actively engaged in vocational roles and career exploration, managing stress and distress effectively, they keep hope for the future regarding their career and further perspective. This might even potentially prevent the onset of psychosis, since impairment of social and role function is known to appear before the active psychosis onset (Lee et al. 2017).
Although the follow-up period is rather short, limiting the investigation of the long-term impact of the intervention on attaining a regular academic qualification or achieving a job with an adequate income, preliminary results are hopeful. Studies have shown that, in the general population, missing out on social roles in late adolescence and early adulthood, such as education and employment, have an effect on subsequent economic, health, and psychosocial situations (Gutiérrez-García et al. 2017). This is particularly the case in individuals who are vulnerable to dropping out of social roles because of psychiatric problems (Rodwell et al. 2017). Therefore, any improvement in functioning is valuable.
Feasibility
The increased focus on identifying and treating CHR-P clients is relatively novel. Since a decline in social functioning in the past year is part of the classification of CHR-P and social functioning in the areas of vocational and career development are of great importance during the adolescence and early adulthood, it was a useful opportunity to test the utility of interventions like SEE in this client group.
The SEE intervention in individuals at CHR for psychosis seems feasible, proven by the ratio of eligible versus participating subjects and the low dropout rate for both the intervention and the assessments. Because the dropouts in the intervention both took place after the initial session, it might be advisable to investigate the clients’ expectation of the intervention and to monitor their motivation regularly. The moderate acceptability of the intervention is noteworthy. Reasons for declining participation were not collected, however a study of Ben-David et al. revealed that for CHR individuals personal, social, cultural and provider factors influence treatment engagement. Future research is needed to examine how these factors influence interventions like these (Ben-David et al. 2019). External factors which affected the participation rate are out of care, declining participation by own therapist of parents, transition to psychosis, or erroneous inclusion. Lessons that can be learned from this pilot for future implementation are that the intervention needs to take place directly after enrollment in the public health service and the need to thoroughly inform parents and other caregivers about the importance of the intervention. In future implementation, this intervention should be piloted with younger youth, paying specific attention to their needs in terms of career interests, skill development, and the need for support for this. Also, with regard to supported education a solid collaboration between the vocational therapists, the individual’s family and school or university disability offices.
An aspect that requires thorough revision in further research is the ‘keeping phase’, specifically for participants that had to maintain an occupation: participants reported they needed less support in this phase, because their goal of acquiring an occupation had already been achieved. It can be argued that these particular individuals in this particular phase should be motivated to continue the intervention.
Maintaining an occupation is challenging and requires specific skills that cannot be trained in advance and specified support is needed. In comparison to the participants with prolonged severe mental illnesses, for whom the intervention was originally developed, individuals at CHR for psychosis in general have a relatively mild level of disturbed engagement in work and school activities and therefore these individuals are better able to acquire an occupation by themselves.
Clinical Implications
The results of this pilot study (indirectly) emphasize the need to heighten awareness of the level of engagement in work and school activities and of (re)enrolment in education and occupation in individuals at CHR for psychosis. This is in line with the Dutch clinical guideline for psychosis (Veling et al. 2017), as well as the NICE guidelines (NICE 2014) which recommends indicated interventions aimed at educational and occupational functioning.
The SEE intervention is a low-threshold positive intervention that can be provided by a skilled vocational therapist, who receives an additional training of 3 × 6 h plus 24 h of supervision (Korevaar and Hofstra 2017). This makes the intervention very accessible for both clients and staff members. Attention to positive things, like study and work, are essential for young people, especially in times when they are in danger of losing their grip on things as a result of mental health problems like CHR-P.
Limitations
The first limitation of this pilot study is its small sample size and its associated lack of power. However, in contrast to randomized controlled trials that study effects more thoroughly, pilot studies aim to investigate the feasibility and preliminary effects and are thus allowed to have a small sample size.
Another limitation is the period until the follow-up, which is limited to one year. Participants remained in education or acquired an occupation, however the short follow-up period does not allow research into whether individuals completed courses, received diplomas, or expanded their working hours.
Conclusion
This pilot study shows preliminary results that a SEE intervention can be effective in improving and sustaining the level of both educational and occupational engagement of individuals at CHR for psychosis. These positive results justify a larger-scale evaluation of the efficacy of a SEE intervention in the CHR for psychosis phase. Moreover, this study demonstrates the feasibility of a SEE intervention, although it also points out the need for flexibility and easy accessibility of vocational therapists to deliver a tailor-made intervention, to meet the needs of the participants in all phases of the intervention.
Data Availability
The datasets generated during and/or analysed during the current study are not publicly available due to patient confidentiality but are available from the corresponding author on reasonable request.
Code Availability
I19 Other.
References
Addington, J., Cornblatt, B. A., Cadenhead, K. S., Cannon, T. D., McGlashan, T. H., Perkins, D. O., … Heinssen, R. (2011). At clinical high risk for psychosis: Outcome for nonconverters. American Journal of Psychiatry, 168(8), 800–805. https://doi.org/10.1176/appi.ajp.2011.10081191
Becker, L. (2000). Effect size calculators. Retrieved from https://www.uccs.edu/lbecker/index.html
Ben-David S, Cole AR, Brucato G, Girgis R, Munson MR. (2019). A conceptual model of mental health service utilization among young adults at clinical high-risk for developing psychosis. Psychiatric Rehabilitation Journal, 42(1), 17-25. doi: https://doi.org/10.1037/prj0000336.
Cornblatt, B. A., Auther, A. M., Niendam, T., Smith, C. W., Zinberg, J., Bearden, C. E., & Cannon, T. D. (2007). Preliminary findings for two new measures of social and role functioning in the prodromal phase of schizophrenia. Schizophrenia Bulletin, 33(3), 688–702. https://doi.org/https://doi.org/10.1093/schbul/sbm029
Corp., I. (2015). IBM SPSS Statistics for Windows. Armonk, NY: IBM Corp.
Cotter, J., Drake, R. J., Bucci, S., Firth, J., Edge, D., & Yung, A. R. (2014). What drives poor functioning in the at-risk mental state? A systematic review. Schizophrenia Research, 159(2–3), 267–277. https://doi.org/https://doi.org/10.1016/j.schres.2014.09.012
Danley, K. S., Sciarappa, K., & MacDonald-Wilson, K. (1992). Choose-get-keep: a psychiatric rehabilitation approach to supported employment. New Directions for Mental Health Services, 53, 87–96. https://doi.org/https://doi.org/10.1002/yd.23319925310
Davies C, Cipriani A, Ioannidis JPA, Radua J, Stahl D, Provenzani U, et al. ‘Lack of evidence to favor specific preventive interventions in psychosis: a network meta-analysis’. World Psychiatry (2018) 17:196–209. doi: https://doi.org/10.1002/wps.20526
Drake RE, Bond GR, Goldman HH, Hogan MF, Karakus M; Individual Placement And Support Services Boost Employment For People With Serious Mental Illnesses, But Funding Is Lacking. Health Aff (Millwood). 2016 Jun 1; 35(6):1098-105.
Drake, R. E., Bond, G. R., & Becker, D. R. (2012). Individual Placement and Support - Am evidence-based approach to supported employment. New York: Oxford University Press.
Eldridge, S. M., Lancaster, G. A., Campbell, M. J., Thabane, L., Hopewell, S., Coleman, C. L., & Bond, C. M. (2016). Defining feasibility and pilot studies in preparation for randomised controlled trials: Development of a conceptual framework. PLoS ONE, 11(3), 1–22. https://doi.org/https://doi.org/10.1371/journal.pone.0150205
Ellison, M. L., Reilly, E. D., Mueller, L., Schultz, M. R., & Drebing, C. E. (2018). A Supported Education Service Pilot for Returning Veterans With Posttraumatic Stress Disorder. Psychological Services, 15(2), 200–207. https://doi.org/https://doi.org/10.1037/ser0000180
Ellison ML, Klodnick VV, Bond GR, Krzos IM, Kaiser SM, Fagan MA, Davis M. (2015) Adapting supported employment for emerging adults with serious mental health conditions. Journal of Behavoir Health Services and Research, 42(2), 206-22. doi: https://doi.org/10.1007/s11414-014-9445-4. PMID: 25391357.
Field, A. (2013). Discovering Statistics Using SPSS. SAGE Publications (Vol. 4). London: Sage.
Goldman, H. H., Skodol, A. E., & Lave, T. R. (1992). Revising axis V for DSM-IV: A review of measures of social functioning. American Journal of Psychiatry, 149(9), 1148–1156. https://doi.org/https://doi.org/10.1176/ajp.149.9.1148
Gutiérrez-García, R. A., Benjet, C., Borges, G., Méndez Ríos, E., & Medina-Mora, M. E. (2017). NEET adolescents grown up: eight-year longitudinal follow-up of education, employment and mental health from adolescence to early adulthood in Mexico City. European Child and Adolescent Psychiatry, 26(12), 1459–1469. https://doi.org/https://doi.org/10.1007/s00787-017-1004-0
Hofstra, J., & Korevaar, L. (2016). Toolkit Supported Education. Rotterdam: Erasmus: ImpulSE.
Humensky JL, Nossel I, Bello I, Dixon LB. Supported Education and Employment Services for Young People with Early Psychosis in OnTrackNY. J Ment Health Policy Econ. 2019 Sep 1;22(3):95–108. PMID: 31811753; PMCID: PMC6902640.
Ising, H. K., Veling, W., Loewy, R. L., Rietveld, M. W., Rietdijk, J., Dragt, S., … Van Der Gaag, M. (2012). The validity of the 16-item version of the prodromal questionnaire (PQ-16) to screen for ultra high risk of developing psychosis in the general help-seeking population. Schizophrenia Bulletin, 38(6), 1288–1296. https://doi.org/10.1093/schbul/sbs068
Jang, J. H., Shin, N. Y., Shim, G., Park, H. Y., Kim, E., Jang, G.-E., … Kwon, J. S. (2011). Longitudinal patterns of social functioning and conversion to psychosis in subjects at ultra-high risk. Australian and New Zealand Journal of Psychiatry, 45, 763–770. https://doi.org/10.3109/00048674.2011.595684
Kane, J. M., Robinson, D. G., Schooler, N. R., Kim, T., Penn, D. L., Rosenheck, R. A., … Heinssen, R. K. (2016). Comprehensive Versus Usual Community Care For First Episode Psychosis: Two-Year Outcomes From The NIMH RAISE Early Treatment Program. Amarican, 173(4), 362–372. https://doi.org/10.1176/appi.ajp.2015.15050632.Comprehensive
Killackey E, Allott K, Woodhead G, Connor S, Dragon S, Ring J. Individual placement and support, supported education in young people with mental illness: an exploratory feasibility study. Early Interv Psychiatry (2017). 11(6):526–531. doi: https://doi.org/10.1111/eip.12344
Killackey, E., Allott, K., Jackson, H. J., Scutella, R., Tseng, Y. P., Borland, J., … Cotton, S. M. (2019). Individual placement and support for vocational recovery in first-episode psychosis: Randomised controlled trial. British Journal of Psychiatry, 214(2), 76–82. https://doi.org/10.1192/bjp.2018.191
Korevaar, L. (2015). Handboek begeleid leren: het ondersteunen van jongeren met psychische beperkingen bij het kiezen, verkrijgen en behouden van een reguliere opleiding. Utrecht: Stichting Rehabilitatie ’92.
Korevaar, E.L. & J. Hofstra (2017). Databank effectieve jeugdinterventies: beschrijving ‘Begeleid Leren'. Utrecht: Nederlands Jeugdinstituut.
Lee, S. J., Kim, K. R., Lee, S. Y., & An, S. K. (2017). Impaired Social and Role Function in Ultra-High Risk for Psychosis and First-Episode Schizophrenia: Its Relations with Negative Symptoms. Psychiatry investigation, 14(5), 539–545. https://doi.org/https://doi.org/10.4306/pi.2017.14.5.539
Luyten, E., Busschbach, J., Swildens, W., & Kdjfal. (2004). Psychiatric rehabilitation fidelity in the Netherlands: questionnaire. Assen/Rotterdam: Dutch Foundation for Psychiatric Rehabilitation.
Mowbray, C. T., Collins, M. E., Bellamy, C. D., Megivern, D. A., Bybee, D., & Szilvagyi, S. (2005). Supported education for adults with psychiatric disabilities: An innovation for social work and psychosocial rehabilitation practice. Social Work, 50(1), 7–20. https://doi.org/https://doi.org/10.1093/sw/50.1.7
Mueser, K. T., Penn, D., Addington, J., Brunette, M. F., Gingerich, S., Lynde, D. W., … McGurk, S. R. (2015). The NAVIGATE Program for First Episode Psychosis: Rationale, Overview, and Description of Psychosocial Components. Psychiatric Services, 66(7), 680–690. https://doi.org/10.1176/appi.ps.201400413
NICE Guidelines. (2014). NICE Guidelines: Psychosis and schizophrenia in adults: prevention and management. Retrieved from https://www.nice.org.uk/guidance/CG178
Nordic Alliance on Mental Illnesses. (2016). Psychosis. Retrieved from https://www.nami.org/NAMI/media/NAMI-Media/Images/FactSheets/What-is-Early-and-First-Episode-Psychosis.pdf
Rodwell, L., Romaniuk, H., Nilsen, W., Carlin, J. B., Lee, K. J., & Patton, G. C. (2017). Adolescent mental health and behavioural predictors of being NEET: a prospective study of young adults not in employment, education, or training. Psychological Medicine, 1–11. https://doi.org/https://doi.org/10.1017/S0033291717002434
Sanches, S. A., Van Busschbach, J. T., Michon, H. W. C., Van Weeghel, J., & Swildens, W. E. (2018). The role of working alliance in attainment of personal goals and improvement in quality of life during psychiatric rehabilitation. Psychiatric Services, 69(8), 903–909. https://doi.org/https://doi.org/10.1176/appi.ps.201700438
Sullivan, A. P., Nicolellis, D. L., & MacDonald-Wilson, K. (1993). Choose-Get-Keep: A Psychiatric Rehabilitation Approach to Supported Education. Psychosocial Rehabilitation Journal, 17, 55–68.
Swildens, W., Van Busschbach, J. T., Michon, ; Harry, Kroon, H., Maarten, ;, Koeter, W. J., … Van Os, J. (2011). Effectively Working on Rehabilitation Goals: 24-Month Outcome of a Randomized Controlled Trial of the Boston Psychiatric Rehabilitation Approach. The Canadian Journal of Psychiatry, 56(12), 751–760.
Unger, K. (1998). Handbook on Supported Education: Providing Services for Students with Psychiatric Disabilities. Baltimore: Paul H. Brookes Publishing.
Van Der Gaag, M., Nieman, D. H., & Van Der Berg, D. (2013). CBT for those at risk of a first episode psychosis.Evidence-based Psychotherapy for People With an “At Risk Mental State.” (1st ed.). London: Routeledge.
Veling, W., Lansen, M., Rosema, B. S., Kleiwegt, H., de Pater, M., Gijsman, H., … Castelein, S. (2017). Zorgstandaarden Psychose. Retrieved October 27, 2017, from https://www.ggzstandaarden.nl/zorgstandaarden/psychose
Yung, A. R., Yuen, H. P., Mcgorry, P. D., Phillips, L. J., Kelly, D., Dell ’olio, M., … Buckby, J. (2005). Mapping the onset of psychosis: the Comprehensive Assessment of At-Risk Mental States. Australian and New Zealand Journal of Psychiatry , 39, 964–971.
Acknowledgements
We thank the participants and the vocational therapists Mrs. M. Oosterkamp and Mrs. M. Koree for their effort to execute in this study.
Funding
Mrs. R. Nieboer and N. Boonstra, PhD, received a grant from the province of Friesland to execute this study, registration number 01029272.
Author information
Authors and Affiliations
Contributions
NB, RN and LK contributed to the study conception and design. Material preparation was done by RN. Data collection was performed by RN and van der BP. Data analysis and the first draft of the manuscript was written by AM and all other authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Consent to Participate
Informed consent was obtained, as well as parental or guardian’s consent of participants under the age of sixteen.
Consent for Publication
By subscribing the informed consent to participate in the study, all participants also gave their consent for publication of the study.
Ethics Approval
Ethical approval was waived by the medical ethics committee of University Medical Centre Groningen (METc2013/468) in view of the intervention being performed as a part of the routine care.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Malda, A., Kuis, D.J., Nieboer, R. et al. Supported Education and Supported Employment for Individuals at Clinical-High Risk of Psychosis: A Pilot Study. J. Psychosoc. Rehabil. Ment. Health 10, 331–343 (2023). https://doi.org/10.1007/s40737-022-00312-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40737-022-00312-5