Abstract
Background
Although discontinuation of antiplatelet agents at least 5 days before kidney biopsy is commonly recommended, the evidence behind this practice is of low level. Indeed, few non-randomized studies previously showed an equivalent risk of bleeding in patients receiving aspirin therapy.
Methods
We conducted a single center retrospective study comparing the risk of complications after percutaneous native kidney biopsy in patients who received low-dose aspirin (ASA) within 5 days from biopsy and those who did not. The main outcome was the difference in the incidence of major complications (red blood cell transfusion, need for selective arterial embolization, surgery, nephrectomy). Secondary outcomes included difference in minor complications, comparison between patients who received ASA within 48 h or within 3–5 days, identification of independent factors predictive of major complications.
Results
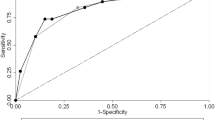
We analyzed data on 750 patients, of whom 94 received ASA within 5 days from biopsy. There were no significant differences in the proportion of major complications in patients receiving or not receiving ASA (2.59% and 3.19%, respectively, percentage point difference 1%, 95% CI − 3 to 4%, p = 0.74). Groups were also comparable for minor complications; among patients receiving ASA, there were no differences in major bleeding between those who received ASA within 48 h or 3–5 days from biopsy. Significant baseline predictors of major bleeding in our cohort were platelet count lower than 120*103/microliter, higher diastolic blood pressure and higher blood urea.
Conclusions
Treatment with low-dose ASA within 5 days from kidney biopsy did not increase the risk of complications after the procedure.
Graphical abstract



Similar content being viewed by others
References
Halimi J-M, Gatault P, Longuet H et al (2020) Major bleeding and risk of death after percutaneous native kidney biopsies. Clin J Am Soc Nephrol. https://doi.org/10.2215/cjn.14721219
Kumar V, Mitchell MD, Umscheid CA, Berns JS, Hogan JJ (2018) Risk of complications with use of aspirin during renal biopsy: a systematic review. Clin Nephrol 89(2):67–74. https://doi.org/10.5414/CN109274
Mackinnon B, Fraser E, Simpson K, Fox JG, Geddes C (2008) Is it necessary to stop antiplatelet agents before a native renal biopsy? Nephrol Dial Transplant 23(11):3566–3570. https://doi.org/10.1093/ndt/gfn282
Lees JS, McQuarrie EP, Mordi N, Geddes CC, Fox JG, Mackinnon B (2017) Risk factors for bleeding complications after nephrologist-performed native renal biopsy. Clin Kidney J. https://doi.org/10.1093/ckj/sfx012
Biondi-Zoccai GGL, Lotrionte M, Agostoni P et al (2006) A systematic review and meta-analysis on the hazards of discontinuing or not adhering to aspirin among 50,279 patients at risk for coronary artery disease. Eur Heart J 27(22):2667–2674. https://doi.org/10.1093/eurheartj/ehl334
Awtry EH, Loscalzo J (2000) Aspirin. Circulation 101(10):1206–1218. https://doi.org/10.1161/01.CIR.101.10.1206
Rollino C, Giacchino F, Savoldi S et al (2012) Restrospective analysis of the renal biopsy activity in Piedmont. G Ital Nefrol 29(4):473–483
Bollée G, Martinez F, Moulin B et al (2010) Renal biopsy practice in France: results of a nationwide study. Nephrol Dial Transplant 25(11):3579–3585. https://doi.org/10.1093/NDT/GFQ254
MacGinley R, Champion De Crespigny PJ, Gutman T et al (2019) KHA-CARI Guideline recommendations for renal biopsy. Nephrology 24(12):1205–1213. https://doi.org/10.1111/nep.13662
Hogan JJ, Mocanu M, Berns JS (2016) The native kidney biopsy: update and evidence for best practice. Clin J Am Soc Nephrol 11(2):354–356. https://doi.org/10.2215/CJN.05750515
Ferrari E, Benhamou M, Cerboni P, Marcel B (2005) Coronary syndromes following aspirin withdrawal: a special risk for late stent thrombosis. J Am Coll Cardiol 45(3):456–459. https://doi.org/10.1016/J.JACC.2004.11.041
Corapi KM, Chen JLT, Balk EM, Gordon CE (2012) Bleeding complications of native kidney biopsy: a systematic review and meta-analysis. Am J Kidney Dis 60(1):62–73. https://doi.org/10.1053/J.AJKD.2012.02.330
Baffour FI, Hickson LTJ, Stegall MD et al (2017) Effects of aspirin therapy on ultrasound-guided renal allograft biopsy bleeding complications. J Vasc Interv Radiol 28(2):188–194. https://doi.org/10.1016/J.JVIR.2016.10.021
Mejía-Vilet JM, Márquez-Martínez MA, Cordova-Sanchez BM, Ibargüengoitia MC, Correa-Rotter R, Morales-Buenrostro LE (2018) Simple risk score for prediction of haemorrhagic complications after a percutaneous renal biopsy. Nephrology (Carlton) 23(6):523–529. https://doi.org/10.1111/NEP.13055
Manno C, Strippoli GFM, Arnesano L et al (2004) Predictors of bleeding complications in percutaneous ultrasound-guided renal biopsy. Kidney Int 66(4):1570–1577. https://doi.org/10.1111/J.1523-1755.2004.00922.X
Korbet SM, Gashti CN, Evans JK, Whittier WL (2018) Risk of percutaneous renal biopsy of native kidneys in the evaluation of acute kidney injury. Clin Kidney J 11(5):610–615. https://doi.org/10.1093/CKJ/SFY048
Muñoz AT, Valdez-Ortiz R, González-Parra C, Espinoza-Dávila E, Morales-Buenrostro LE, Correa-Rotter R (2011) Percutaneous renal biopsy of native kidneys: efficiency, safety and risk factors associated with major complications. Arch Med Sci 7(5):823–831. https://doi.org/10.5114/AOMS.2011.25557
Andrulli S, Rossini M, Gigliotti G et al (2022) The risks associated with percutaneous native kidney biopsies: a prospective study. Nephrol Dial Transplant. https://doi.org/10.1093/NDT/GFAC177
Monahan H, Gunderson T, Greene E, Schmit G, Atwell T, Schmitz J (2019) Risk factors associated with significant bleeding events after ultrasound-guided percutaneous native renal biopsies: a review of 2204 cases. Abdom Radiol (New York) 44(6):2316–2322. https://doi.org/10.1007/S00261-019-01962-Z
Ali H, Murtaza A, Anderton J, Ahmed A (2015) Post renal biopsy complication rate and diagnostic yield comparing hands free (ultrasound-assisted) and ultrasound-guided biopsy techniques of renal allografts and native kidneys. Springerplus. https://doi.org/10.1186/S40064-015-1292-0
Acknowledgements
The study was approved by the local Ethical Committee “Comitato Etico dell’Area Vasta Emilia Nord”.
Funding
No funding was required for the present study.
Author information
Authors and Affiliations
Contributions
FF conceived and designed the study; SC, FG, FB, SG, GL collected the data; FF and GA analyzed the data; FF wrote the manuscript; GM, RM, GC, GD critically revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The Authors declare no conflict of interest for the present study; the results presented in this paper have not been published previously in whole or part, except in abstract format.
Ethics approval
The study was approved by the appropriate institutional research ethics committee (“Comitato Etico dell’Area Vasta Emilia Nord”) and was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fontana, F., Cazzato, S., Giaroni, F. et al. Risk of bleeding after percutaneous native kidney biopsy in patients receiving low-dose aspirin: a single-center retrospective study. J Nephrol 36, 475–483 (2023). https://doi.org/10.1007/s40620-022-01441-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-022-01441-7