Abstract
Introduction
Many current guidelines on optimal target blood pressure (BP) for chronic kidney disease (CKD) patients are largely based on studies in diabetic and hypertensive patients. However, there have been few studies in patients with glomerular diseases.
Methods
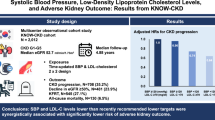
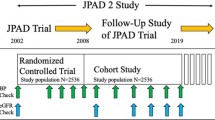
We retrospectively studied the longitudinal association between BP and CKD progression in 1,066 biopsy-proven patients diagnosed with primary glomerular diseases, including IgA nephropathy, membranous nephropathy (MN), and focal segmental glomerulosclerosis (FSGS), between 2005 and 2017. The main predictor was time-updated systolic blood pressure (SBP) at every clinic visit. The primary outcome was a composite one including ≥ 50% decrease in estimated glomerular filtration rate (eGFR) from the baseline, and end-stage kidney disease (ESKD).
Results
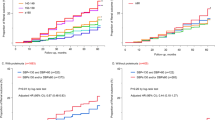
During 5009 person-years of follow-up, the primary outcome occurred in 157 (14.7%) patients. In time-varying Cox model, the adjusted hazard ratios (HRs) (95% confidence interval (CI)) for the primary outcome were 1.48 (0.96–2.29), 2.07 (1.22–3.52), and 2.53 (1.13–5.65) for SBP of 120–129, 130–139, and ≥ 140 mmHg, respectively, compared with SBP < 120 mmHg. This association was particularly evident in patients with elevated proteinuria. However, there was no association between baseline SBP and adverse kidney outcomes. Finally, prediction models failed to show the improvement of predictive performance of SBP compared with that of remission status. Moreover, patients with remission and less controlled SBP had better kidney outcomes than those with non-remission and well-controlled SBP.
Conclusion
Among patients with glomerular disease, higher time-updated SBP was significantly associated with higher risk of CKD progression. However, the clinical significance of blood pressure was less powerful than remission status.
Graphic abstract




Similar content being viewed by others
References
Becker GJ, Wheeler DC, De Zeeuw D, Fujita T, Furth SL, Holdaas H et al (2012) Kidney disease: improving global outcomes (KDIGO) blood pressure work group. KDIGO clinical practice guideline for the management of blood pressure in chronic kidney disease. Kidney Int Suppl 2(5):337–414
Schrier RW, Abebe KZ, Perrone RD, Torres VE, Braun WE, Steinman TI et al (2014) Blood pressure in early autosomal dominant polycystic kidney disease. N Engl J Med 371(24):2255–2266
Troyanov S, Wall CA, Miller JA, Scholey JW, Cattran DC (2005) Focal and segmental glomerulosclerosis: definition and relevance of a partial remission. J Am Soc Nephrol 16(4):1061–1068
Ponticelli C, Zucchelli P, Passerini P, Cesana B, Locatelli F, Pasquali S et al (1995) A 10-year follow-up of a randomized study with methylprednisolone and chlorambucil in membranous nephropathy. Kidney Int 48(5):1600–1604
Ponticelli C, Zucchelli P, Passerini P, Cagnoli L, Cesana B, Pozzi C et al (1989) A randomized trial of methylprednisolone and chlorambucil in idiopathic membranous nephropathy. N Engl J Med 320(1):8–13
Pozzi C, Andrulli S, Del Vecchio L, Melis P, Fogazzi GB, Altieri P et al (2004) Corticosteroid effectiveness in IgA nephropathy: long-term results of a randomized, controlled trial. J Am Soc Nephrol 15(1):157–163
Orofino L, Quereda C, Lamas S, Orte L, Gonzalo A, Mampaso F et al (1987) Hypertension in primary chronic glomerulonephritis: analysis of 288 biopsied patients. Nephron 45(1):22–26
Kheder MA, Maiz HB, Abderrahim E, El Younsi F, Moussa FB, Safar ME et al (1993) Hypertension in primary chronic glomerulonephritis analysis of 359 cases. Nephron 63(2):140–144
Johnston PA, Davison AM (1993) Hypertension in adults with idiopathic glomerulonephritis and normal serum creatinine. A report from the MRC glomerulonephritis registry. Nephrol Dial Transplant 8(1):20–24
Ridao N, Luño J, de Vinuesa SG, Gómez F, Tejedor A, Valderrábano F (2001) Prevalence of hypertension in renal disease. Nephrol Dial Transplant 16(Suppl 1):70–73
Joffe M, Hsu CY, Feldman HI, Weir M, Landis JR, Hamm LL (2010) Variability of creatinine measurements in clinical laboratories: results from the CRIC study. Am J Nephrol 31(5):426–434
Levey AS, Coresh J, Greene T, Marsh J, Stevens LA, Kusek JW et al (2007) Expressing the modification of diet in renal disease study equation for estimating glomerular filtration rate with standardized serum creatinine values. Clin Chem 53(4):766–772
Levey AS, Stevens LA, Schmid CH, Zhang Y, Castro AF, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Harrell FE, Califf RM, Pryor DB, Lee KL, Rosati RA (1982) Evaluating the yield of medical tests. JAMA J Am Med Assoc 247(18):2543–2546
Group KDIGO (KDIGO) GW (2012) KDIGO clinical practice guideline for glomerulonephritis. Kidney Int Suppl 2(2):139–274
Sethna CB, Meyers KEC, Mariani LH, Psoter KJ, Gadegbeku CA, Gibson KL et al (2017) Blood pressure and visit-to-visit blood pressure variability among individuals with primary proteinuric glomerulopathies. Hypertension 70(2):315–323
Ihm CG (2015) Hypertension in chronic glomerulonephritis. Electrolyte Blood Press 13(2):41–45
Ljutic D (2003) The role of arterial hypertension in the progression of non-diabetic glomerular diseases. Nephrol Dial Transplant 18(90005):28v–230
Anderson AH, Yang W, Townsend RR, Pan Q, Chertow GM, Kusek JW et al (2015) Time-updated systolic blood pressure and the progression of chronic kidney disease: a cohort study. Ann Intern Med 162(4):258–265
Hiki Y, Odani H, Takahashi M, Yasuda Y, Nishimoto A, Iwase H et al (2001) Mass spectrometry proves under-O-glycosylation of glomerular IgA1 in IgA nephropathy. Kidney Int 59(3):1077–1085
Tomana M, Matousovic K, Julian BA, Radl J, Konecny K, Mestecky J (1997) Galactose-deficient IgA1 in sera of IgA nephropathy patients is present in complexes with IgG. Kidney Int 52(2):509–516
Tomana M, Novak J, Julian BA, Matousovic K, Konecny K, Mestecky J (1999) Circulating immune complexes in IgA nephropathy consist of IgA1 with galactose-deficient hinge region and antiglycan antibodies. J Clin Invest 104(1):73–81
Wei C, El Hindi S, Li J, Fornoni A, Goes N, Sageshima J et al (2011) Circulating urokinase receptor as a cause of focal segmental glomerulosclerosis. Nat Med 17(8):952–960
Beck LH, Bonegio RGB, Lambeau G, Beck DM, Powell DW, Cummins TD et al (2009) M-type phospholipase A2 receptor as target antigen in idiopathic membranous nephropathy. N Engl J Med 361(1):11–21
Hoxha E, Thiele I, Zahner G, Panzer U, Harendza S, Stahl RAK (2014) Phospholipase A2 receptor autoantibodies and clinical outcome in patients with primary membranous nephropathy. J Am Soc Nephrol 25(6):1357–1366
Ramachandran R, Yadav AK, Kumar V, Inamdar N, Nada R, Gupta KL et al (2018) Temporal association between PLA2R antibodies and clinical outcomes in primary membranous nephropathy. Kidney Int Reports 3(1):142–147
Nam KH, Kie JH, Lee MJ, Chang TI, Kang EW, Kim DW et al (2014) Optimal proteinuria target for renoprotection in patients with IgA nephropathy. PLoS ONE 9(7):e0101935. https://doi.org/10.1371/journal.pone.0101935
Reich HN, Troyanov S, Scholey JW, Cattran DC (2007) Remission of proteinuria improves prognosis in IgA nephropathy. J Am Soc Nephrol 18(12):3177–3183
Polanco N, Gutiérrez E, Covarsí A, Ariza F, Carreñ OA, Vigil A et al (2010) Spontaneous remission of nephrotic syndrome in idiopathic membranous nephropathy. J Am Soc Nephrol 21(4):697–704
Troyanov S, Wall CA, Miller JA, Scholey JW, Cattran DC (2004) Idiopathic membranous nephropatliy: definition and relevance of a partial remission. Kidney Int 66(3):1199–1205
Chun MJ, Korbet SM, Schwartz MM, Lewis EJ (2004) Focal segmental glomerulosclerosis in nephrotic adults: presentation, prognosis, and response to therapy of the histologic variants. J Am Soc Nephrol 15(8):2169–2177
Vischer AS, Burkard T (2017) Principles of blood pressure measurement—current techniques, office vs ambulatory blood pressure measurement. Adv Exp Med Biol 956:85–96
Chen T, Li X, Li Y, Xia E, Qin Y, Liang S et al (2019) Prediction and risk stratification of kidney outcomes in IgA nephropathy. Am J Kidney Dis 74(3):300–309
Sood MM, Akbari A, Manuel D, Ruzicka M, Hiremath S, Zimmerman D et al (2017) Time-varying association of individual BP components with eGFR in late-stage CKD. Clin J Am Soc Nephrol 12(6):904–911
Alencar de Pinho N, Levin A, Fukagawa M, Hoy WE, Pecoits-Filho R, Reichel H et al (2019) Considerable international variation exists in blood pressure control and antihypertensive prescription patterns in chronic kidney disease. Kidney Int 96(4):983–994
Fuiano G, Mazza G, Comi N, Caglioti A, De Nicola L, Iodice C et al (2000) Current indications for renal biopsy: a questionnaire-based survey. Am J Kidney Dis 35(3):448–457
Acknowledgements
This research was supported by the Research of Korea Centers for Disease Control and Prevention (2019ER690101).
Funding
None.
Author information
Authors and Affiliations
Consortia
Contributions
SHH and HWK contributed to the research idea and study design; S-WK, T-HY, SHH, HJC, D-RR, EWK, TIC, JTP, and HWK were involved in data acquisition; SHH and HWK were responsible for data analysis/interpretation; SHH, YSJ, SCK, JYL, SL, and HWK contributed to statistical analysis; JTP, TIC, EWK, T-HY, HJC, S-WK, and SHH were responsible for data analysis/interpretation supervision or mentorship. Each author contributed important intellectual content during manuscript drafting or revision and accepts accountability for the overall work by ensuring that questions pertaining to the accuracy or integrity of any portion of the work are appropriately investigated and resolved. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
The study was performed in accordance with the Declaration of Helsinki principles, and the institutional review board of Yonsei University Health System approved this retrospective study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The Korean GlomeruloNEphritis Study (KoGNET) Group.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, H.W., Park, J.T., Joo, Y.S. et al. Systolic blood pressure and chronic kidney disease progression in patients with primary glomerular disease. J Nephrol 34, 1057–1067 (2021). https://doi.org/10.1007/s40620-020-00930-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-020-00930-x