Abstract
Background
Sympathetic over-activity is a hallmark of end stage renal disease (ESRD). Left ventricular (LV) disorders and volume overload are pervasive in ESRD and sympathetic over-activity may be a relevant mediator of the cardiovascular (CV) risk by these alterations in this population.
Design
We investigated the relationship between a combined biomarker of LV disorders and volume excess, atrial natriuretic peptide (ANP), and the plasma concentration of nor-epinephrine (NE) in 227 ESRD patients without heart failure at baseline and modelled the risk for incident CV events by these biomarkers over a 3.5 years follow-up.
Results
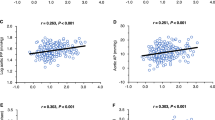
Plasma NE was strongly and independently related to ANP (β = 0.31, P < 0.001). In a multivariate Cox’s regression analysis, ANP was an independent predictor of these events [HR (1-SD) 1.25, 95 % CI 1.01–1.54]. However, when NE was introduced into the multivariate model, HR by ANP reduced substantially (1.14, 95 % CI 0.91–1.42) and was no longer significant (P = 0.25) while the CV risk signalled by NE was clinically relevant (HR 1.29, 95 % CI 1.05–1.59) and statistically significant (P = 0.02).
Conclusions
In ESRD patients without heart failure, NE is strongly and independently related to ANP. The predictive power of ANP for CV events is largely captured by NE in a statistical model including both biomarkers. These data suggest that sympathetic over-activity may be a relevant mediator of the high risk of CV events triggered by LV disorders and volume excess in this population. However, further mechanistic and intervention studies are needed to prove the nature (causal/non causal) of these findings.


Similar content being viewed by others
References
Baigent C, Landray MJ, Reith C, Emberson J, Wheeler DC, Tomson C, Wanner C, Krane V, Cass A, Craig J, Neal B, Jiang L, Hooi LS, Levin A, Agodoa L, Gaziano M, Kasiske B, Walker R, Massy ZA, Feldt-Rasmussen B, Krairittichai U, Ophascharoensuk V, Fellstrom B, Holdaas H, Tesar V, Wiecek A, Grobbee D, de Zeeuw D, Gronhagen-Riska C, Dasgupta T, Lewis D, Herrington W, Mafham M, Majoni W, Wallendszus K, Grimm R, Pedersen T, Tobert J, Armitage J, Baxter A, Bray C, Chen Y, Chen Z, Hill M, Knott C, Parish S, Simpson D, Sleight P, Young A, Collins R, Investigators S (2011) The effects of lowering LDL cholesterol with simvastatin plus ezetimibe in patients with chronic kidney disease (Study of Heart and Renal Protection): a randomised placebo-controlled trial. Lancet 377(9784):2181–2192
de Jager DJ, Grootendorst DC, Jager KJ, van Dijk PC, Tomas LM, Ansell D, Collart F, Finne P, Heaf JG, De Meester J, Wetzels JF, Rosendaal FR, Dekker FW (2009) Cardiovascular and noncardiovascular mortality among patients starting dialysis. JAMA 302(16):1782–1789
Zoccali C, Mallamaci F, Tripepi G (2003) Traditional and emerging cardiovascular risk factors in end-stage renal disease. Kidney Int Suppl 85:S105–S110
Zoccali C, Benedetto FA, Mallamaci F, Tripepi G, Giacone G, Cataliotti A, Seminara G, Stancanelli B, Malatino LS (2004) Prognostic value of echocardiographic indicators of left ventricular systolic function in asymptomatic dialysis patients. J Am Soc Nephrol 15(4):1029–1037
Pecoits-Filho R, Gonçalves S, Barberato SH, Bignelli A, Lindholm B, Riella MC, Stenvinkel P (2004) Impact of residual renal function on volume status in chronic renal failure. Blood Purif 22(3):285–292
Agarwal R (2010) Hypervolemia is associated with increased mortality among hemodialysis patients. Hypertension 56(3):512–517. doi:10.1161/HYPERTENSIONAHA.110.154815
Vink EE, Blankestijn PJ (2012) Evidence and consequences of the central role of the kidneys in the pathophysiology of sympathetic hyperactivity. Front Physiol 3:29. doi:10.3389/fphys.2012.00029
Benedict CR, Shelton B, Johnstone DE, Francis G, Greenberg B, Konstam M, Probstfield JL, Yusuf S (1996) Prognostic significance of plasma norepinephrine in patients with asymptomatic left ventricular dysfunction. SOLVD Investigators. Circulation 94(4):690–697
Abhayaratna WP, Seward JB, Appleton CP, Douglas PS, Oh JK, Tajik AJ, Tsang TS (2006) Left atrial size: physiologic determinants and clinical applications. J Am Coll Cardiol 47(12):2357–2363
Paoletti E, Zoccali C (2013) A look at the upper heart chamber: the left atrium in chronic kidney disease. Nephrol Dial Transplant. doi:10.1093/ndt/gft482
Tripepi G, Mattace-Raso F, Mallamaci F, Benedetto FA, Witteman J, Malatino L, Zoccali C (2009) Biomarkers of left atrial volume: a longitudinal study in patients with end stage renal disease. Hypertension 54(4):818–824
Zoccali C, Mallamaci F, Benedetto FA, Tripepi G, Parlongo S, Cataliotti A, Cutrupi S, Giacone G, Bellanuova I, Cottini E, Malatino LS, Creed I (2001) Cardiac natriuretic peptides are related to left ventricular mass and function and predict mortality in dialysis patients. J Am Soc Nephrol 12(7):1508–1515
Zoccali C, Mallamaci F, Parlongo S, Cutrupi S, Benedetto FA, Tripepi G, Bonanno G, Rapisarda F, Fatuzzo P, Seminara G, Cataliotti A, Stancanelli B, Malatino LS (2002) Plasma norepinephrine predicts survival and incident cardiovascular events in patients with end-stage renal disease. Circulation 105(11):1354–1359
Cice G, Ferrara L, D’Andrea A, D’Isa S, Di Benedetto A, Cittadini A, Russo PE, Golino P, Calabro R (2003) Carvedilol increases two-year survivalin dialysis patients with dilated cardiomyopathy: a prospective, placebo-controlled trial. J Am Coll Cardiol 41(9):1438–1444
Agarwal R, Sinha AD, Pappas MK, Abraham TN, Tegegne GG (2014) Hypertension in hemodialysis patients treated with atenolol or lisinopril: a randomized controlled trial. Nephrol Dial Transplant 29(3):672–681
Tripepi G, Jager KJ, Dekker FW, Zoccali C (2008) Testing for causality and prognosis: etiological and prognostic models. Kidney Int 74(12):1512–1515
Greenland S, Pearl J, Robins JM (1999) Causal diagrams for epidemiologic research. Epidemiology 10(1):37–48
Pecoits-Filho R, Bucharles S, Barberato SH (2012) Diastolic heart failure in dialysis patients: mechanisms, diagnostic approach, and treatment. Semin Dial 25(1):35–41
Tripepi G, Benedetto FA, Mallamaci F, Tripepi R, Malatino L, Zoccali C (2006) Left atrial volume in end-stage renal disease: a prospective cohort study. J Hypertens 24(6):1173–1180
Tripepi G, Benedetto FA, Mallamaci F, Tripepi R, Malatino L, Zoccali C (2007) Left atrial volume monitoring and cardiovascular risk in patients with end-stage renal disease: a prospective cohort study. J Am Soc Nephrol 18(4):1316–1322
Mancia G, Grassi G, Giannattasio C, Seravalle G (1999) Sympathetic activation in the pathogenesis of hypertension and progression of organ damage. Hypertension 34(4):724–728
Zoccali C, Mallamaci F, Tripepi G, Parlongo S, Cutrupi S, Benedetto FA, Cataliotti A, Malatino LS, CREED Investigators (2002) Norepinephrine and concentric hypertrophy in patients with end-stage renal disease. Hypertension 40(1):41–46
Rozanski A, Blumenthal JA, Kaplan J (1999) Impact of psychological factors on the pathogenesis of cardiovascular disease and implications for therapy. Circulation 99(16):2192–2217
Converse RL Jr, Jacobsen TN, Toto RD, Jost CM, Cosentino F, Fouad-Tarazi F, Victor RG (1992) Sympathetic overactivity in patients with chronic renal failure. N Engl J Med 327(27):1912–1918
Mian M, Paradis P, Schiffrin E (2014) Innate immunity in hypertension. Curr Hypertens Rep 16(2):1–9. doi:10.1007/s11906-013-0413-9
Austin AW, Wissmann T, von Kanel R (2013) Stress and hemostasis: an update. Semin Thromb Hemost 39(8):902–912
Wizemann V, Wabel P, Chamney P, Zaluska W, Moissl U, Rode C, Malecka-Masalska T, Marcelli D (2009) The mortality risk of overhydration in haemodialysis patients. Nephrol Dial Transplant 24(5):1574–1579
Long CS, Ordahl CP, Simpson PC (1989) Alpha 1-adrenergic receptor stimulation of sarcomeric actin isogene transcription in hypertrophy of cultured rat heart muscle cells. J Clin Invest 83(3):1078–1082
Acknowledgments
Samar Abd ElHafeez has been granted ERA-EDTA fellowship at CNR-IFC/IBIM Clinical Epidemiology and Physiopathology of Renal Disease and Hypertension of Reggio Calabria, Italy.
Conflict of interest
All authors declare no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Abd ElHafeez, S., Tripepi, G., Stancanelli, B. et al. Norepinephrine, left ventricular disorders and volume excess in ESRD. J Nephrol 28, 729–737 (2015). https://doi.org/10.1007/s40620-015-0182-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-015-0182-4