Abstract
Objectives
Endothelial dysfunction, the earliest vascular alteration, is a consequence of metabolic disorders associated with obesity. However, it is still unclear whether a proportion of obese individuals without metabolic alterations associated with obesity, defined as “metabolically healthy obesity (MHO)”, exhibit better endothelial function. We therefore aimed to investigate the association of different metabolic obesity phenotypes with endothelial dysfunction.
Methods
The obese participants without clinical cardiovascular disease from the MESA (Multi-Ethnic Study of Atherosclerosis) were allocated to the different metabolic obesity phenotypes based on their metabolic status, including MHO and metabolically unhealthy obesity (MUO). Associations of metabolic obesity phenotypes with the biomarkers of endothelial dysfunction, including soluble intercellular adhesion molecule-1 (sICAM-1) and soluble E-selectin (sE-selectin), were evaluated using multiple linear regression models.
Results
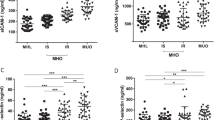
Plasma levels of sICAM-1 and sE-selectin were respectively measured in 2371 and 968 participants. Compared to the non-obese participants, those with MUO were associated with higher concentrations of sICAM-1 (β 22.04, 95% CI 14.33–29.75, P < 0.001) and sE-selectin (β 9.87, 95% CI 6.00–13.75, P < 0.001) after adjusting for confounders. However, no differences were found for the concentrations of sICAM-1 (β 0.70, 95% CI − 8.91 to 10.32, P = 0.886) and sE-selectin (β 3.69, 95% CI − 1.13 to 8.51, P = 0.133) in the participants with MHO compared to the non-obese participants.
Conclusions
Individuals with MUO were associated with elevated biomarkers of endothelial dysfunction, but the association with endothelial dysfunction was not found in those with MHO, indicating that the individuals with MHO might exhibit better endothelial function.




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
World Health Organization. Facts in Pictures: Obesity. https://www.who.int/news-room/facts-in-pictures/detail/6-facts-on-obesity. Accessed 10 Dec 2022
Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, Lee A et al (2017) Health effects of overweight and obesity in 195 countries over 25 years. New Engl J Med 377:13–27
Khan SS, Ning H, Wilkins JT, Allen N, Carnethon M, Berry JD et al (2018) Association of body mass index with lifetime risk of cardiovascular disease and compression of morbidity. Jama Cardiol 3:280–287
Powell-Wiley TM, Poirier P, Burke LE, Després JP, Gordon-Larsen P, Lavie CJ et al (2021) Obesity and cardiovascular disease: a scientific statement from the american heart association. Circulation 143:e984–e1010
Neeland IJ, Poirier P, Després JP (2018) Cardiovascular and metabolic heterogeneity of obesity: clinical challenges and implications for management. Circulation 137:1391–1406
Van Gaal LF, Mertens IL, De Block CE (2006) Mechanisms linking obesity with cardiovascular disease. Nature 444:875–880
Koenen M, Hill MA, Cohen P, Sowers JR (2021) Obesity, adipose tissue and vascular dysfunction. Circ Res 128:951–968
Kwaifa IK, Bahari H, Yong YK, Noor SM (2020) Endothelial dysfunction in obesity-induced inflammation: molecular mechanisms and clinical implications. Biomolecules 10:291
Graupera M, Claret M (2018) Endothelial cells: new players in obesity and related metabolic disorders. Trends Endocrin Met 29:781–794
Caballero AE (2003) Endothelial dysfunction in obesity and insulin resistance: a road to diabetes and heart disease. Obes Res 11:1278–1289
Pi X, Xie L, Patterson C (2018) Emerging roles of vascular endothelium in metabolic homeostasis. Circ Res 123:477–494
Brandão I, Martins MJ, Monteiro R (2020) Metabolically healthy obesity-heterogeneity in definitions and unconventional factors. Metabolites 10(2):48
Stefan N, Häring HU, Hu FB, Schulze MB (2013) Metabolically healthy obesity: epidemiology, mechanisms, and clinical implications. Lancet Diabetes Endo 1:152–162
Bild DE, Bluemke DA, Burke GL, Detrano R, Diez RA, Folsom AR et al (2002) Multi-ethnic study of atherosclerosis: objectives and design. Am J Epidemiol 156:871–881
Levey AS, Coresh J, Greene T, Stevens LA, Zhang YL, Hendriksen S et al (2006) Using standardized serum creatinine values in the modification of diet in renal disease study equation for estimating glomerular filtration rate. Ann Intern Med 145:247–254
Expert Panel on Detection evaluation and others (2001) Executive summary of the third report of the national cholesterol education program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). J Am Med Assoc 285:2486–2497
Stefan N, Häring HU, Schulze MB (2018) Metabolically healthy obesity: the low-hanging fruit in obesity treatment? Lancet Diabetes Endo 6:249–258
Zhou Z, Macpherson J, Gray SR, Gill J, Welsh P, Celis-Morales C et al (2021) Are people with metabolically healthy obesity really healthy? A prospective cohort study of 381,363 UK Biobank participants. Diabetologia 64:1963–1972
Caleyachetty R, Thomas GN, Toulis KA, Mohammed N, Gokhale KM, Balachandran K et al (2017) Metabolically healthy obese and incident cardiovascular disease events among 3.5 million men and women. J Am Coll Cardiol 70:1429–1437
Hamer M, Stamatakis E (2012) Metabolically healthy obesity and risk of all-cause and cardiovascular disease mortality. J Clin Endocr Metab 97:2482–2488
Soriguer F, Gutiérrez-Repiso C, Rubio-Martín E, García-Fuentes E, Almaraz MC, Colomo N et al (2013) Metabolically healthy but obese, a matter of time? Findings from the prospective Pizarra study. J Clin Endocr Metab 98:2318–2325
Camhi SM, Must A, Gona PN, Hankinson A, Odegaard A, Reis J et al (2019) Duration and stability of metabolically healthy obesity over 30 years. Int J Obesity 43:1803–1810
Hamer M, Bell JA, Sabia S, Batty GD, Kivimäki M (2015) Stability of metabolically healthy obesity over 8 years: the English longitudinal study of ageing. Eur J Endocrinol 173:703–708
Gao M, Lv J, Yu C, Guo Y, Bian Z, Yang R et al (2020) Metabolically healthy obesity, transition to unhealthy metabolic status, and vascular disease in Chinese adults: a cohort study. Plos Med 17:e1003351
Kouvari M, Panagiotakos DB, Yannakoulia M, Georgousopoulou E, Critselis E, Chrysohoou C et al (2019) Transition from metabolically benign to metabolically unhealthy obesity and 10-year cardiovascular disease incidence: the ATTICA cohort study. Metabolism 93:18–24
Mongraw-Chaffin M, Foster MC, Anderson C, Burke GL, Haq N, Kalyani RR et al (2018) Metabolically healthy obesity, transition to metabolic syndrome, and cardiovascular risk. J Am Coll Cardiol 71:1857–1865
Rask-Madsen C, King GL (2007) Mechanisms of Disease: endothelial dysfunction in insulin resistance and diabetes. Nat Clin Pract Endocrinol Metab 3:46–56
Sun Y, Rawish E, Nording HM, Langer HF (2021) Inflammation in metabolic and cardiovascular disorders-role of oxidative stress. Life (Basel) 11(7):672
Padilla J, Vieira-Potter VJ, Jia G, Sowers JR (2015) Role of perivascular adipose tissue on vascular reactive oxygen species in type 2 diabetes: a give-and-take relationship. Diabetes 64:1904–1906
Maruhashi T, Higashi Y (2021) Pathophysiological association between diabetes mellitus and endothelial dysfunction. Antioxidants (Basel) 10(8):1306
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ et al (2019) 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American college of cardiology/American heart association task force on clinical practice guidelines. Circulation 140:e596–e646
Wharton S, Lau DCW, Vallis M, Sharma AM, Biertho L, Campbell-Scherer D et al (2020) Obesity in adults: a clinical practice guideline. CMAJ 192(31):E875–E891
Xu S, Ilyas I, Little PJ, Li H, Kamato D, Zheng X et al (2021) Endothelial dysfunction in atherosclerotic cardiovascular diseases and beyond: from mechanism to pharmacotherapies. Pharmacol Rev 73:924–967
Ashor AW, Lara J, Siervo M, Celis-Morales C, Oggioni C, Jakovljevic DG et al (2015) Exercise modalities and endothelial function: a systematic review and dose-response meta-analysis of randomized controlled trials. Sports Med 45:279–296
Oesterle A, Laufs U, Liao JK (2017) Pleiotropic effects of statins on the cardiovascular system. Circ Res 120:229–243
Rahadian A, Fukuda D, Salim HM, Yagi S, Kusunose K, Yamada H et al (2020) Canagliflozin prevents diabetes-induced vascular dysfunction in ApoE-deficient mice. J Atheroscler Thromb 27:1141–1151
Smith GI, Mittendorfer B, Klein S (2019) Metabolically healthy obesity: facts and fantasies. J Clin Invest 129:3978–3989
Meigs JB, Hu FB, Rifai N, Manson JE (2004) Biomarkers of endothelial dysfunction and risk of type 2 diabetes mellitus. Jama-J Am Med Assoc 291:1978–1986
Kershaw KN, Lane-Cordova AD, Carnethon MR, Tindle HA, Liu K (2017) Chronic stress and endothelial dysfunction: the multi-ethnic study of atherosclerosis (MESA). Am J Hypertens 30:75–80
Acknowledgements
The authors thank the other investigators, the staff, and the participants of the MESA study for their valuable contributions. A full list of participating MESA investigators and institutions can be found at http://www.mesa-nhlbi.org.
Funding
The MESA study used in this analysis was supported by contracts HHSN268201500003I, N01-HC-95159, N01-HC-95160, N01-HC-95161, N01-HC-95162, N01-HC-95163, N01-HC-95164, N01-HC-95165, N01-HC-95166, N01-HC-95167, N01-HC-95168, and N01-HC-95169 from the National Heart, Lung, and Blood Institute and by grants UL1-TR-000040, UL1-TR-001079, and UL1-TR-001420 from the National Center for Advancing Translational Sciences (NCATS). This study was also supported by the National Natural Science Foundation of China (81870195, 82070384 to X.Liao; 81900329 to Y.Guo), Guangdong Basic and Applied Basic Research Foundation (2021A1515011668 to X.Liao; 2019A1515011098, 2022A1515010416 to Y.Guo; 2022A1515111181 to ML) and China Postdoctoral Science Foundation (2022M723635 to ML).
Author information
Authors and Affiliations
Contributions
The study was designed by ML with contributions from PW, YG, and XZ. ML, PW, PX, XX, LH, XC, SZ, YL, and YH: participated in data cleaning. PX, XX, LH, and XC: were responsible for data analysis. WX, LW, and XL: were responsible for data interpretation. ML and PW: wrote the original draft. YG and XZ: verified the data. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Research involving human participants and/or animals
The study was conducted following the Declaration of Helsinki and was approved by the corresponding Institutional Ethics Committee.
Informed consent
All participants gave informed consent to the use of their records for research purpose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, M., Wang, P., Xie, P. et al. Expression of ICAM-1 and E-selectin in different metabolic obesity phenotypes: discrepancy for endothelial dysfunction. J Endocrinol Invest 46, 2379–2389 (2023). https://doi.org/10.1007/s40618-023-02094-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-023-02094-4