Abstract
The prevalence of non-alcoholic fatty liver disease (NAFLD) differs between various stages of the female lifespan. The aim of this review is to summarize current evidence on the association of NAFLD and circulating sex hormones and to explore the pathogenesis of NAFLD within the context of (1) sex hormone changes during the reproductive, post-reproductive female life and beyond and (2) the in vitro and in vivo evidence on pharmacological modulation in women on menopausal hormone treatment (MHT) or endocrine therapy after breast cancer. The fluctuation in estrogen concentrations, the relative androgen excess, and the age-related reduction in sex hormone-binding globulin are related to increased NAFLD risk. Moreover, the peri-menopausal changes in body composition and insulin resistance might contribute to the increased NAFLD risk. Whether MHT prevents or improves NAFLD in this population remains an open question. Studies in women with breast cancer treated with tamoxifen or non-steroidal aromatase inhibitors point to their adverse effects on NAFLD development, although a more pronounced effect of tamoxifen is reported. Future studies focusing on the underlying pathogenesis should identify subgroups with the highest risk of NAFLD development and progression into more aggressive forms, as well as elucidate the role of hormone therapies, such as MHT.

Similar content being viewed by others
References
Dewidar B et al (2020) Metabolic liver disease in diabetes—from mechanisms to clinical trials. Metabolism 111S:154299
Pafili K, Maltezos E, Papanas N (2018) Ipragliflozin and sodium glucose transporter 2 inhibitors to reduce liver fat: will the prize we sought be won? Expert Opin Pharmacother 19(3):185–187
Gunn NT, Shiffman ML (2018) The use of liver biopsy in nonalcoholic fatty liver disease: when to biopsy and in whom. Clin Liver Dis 22(1):109–119
Pafili K, Roden M (2020) Nonalcoholic fatty liver disease (NAFLD) from pathogenesis to treatment concepts in humans. Mol Metab 50:101122
Kahl S et al (2014) Comparison of liver fat indices for the diagnosis of hepatic steatosis and insulin resistance. PLoS ONE 9(4):e94059
Long MT, Gandhi S, Loomba R (2020) Advances in non-invasive biomarkers for the diagnosis and monitoring of non-alcoholic fatty liver disease. Metabolism 111S:154259
Polyzos SA, Mantzoros CS (2016) Nonalcoholic fatty future disease. Metabolism 65(8):1007–1016
Gouni-Berthold I, Papanas N, Maltezos E (2014) The role of oral antidiabetic agents and incretin mimetics in type 2 diabetic patients with non-alcoholic fatty liver disease. Curr Pharm Des 20(22):3705–3715
Zaharia OP et al (2019) Risk of diabetes-associated diseases in subgroups of patients with recent-onset diabetes: a 5-year follow-up study. Lancet Diabetes Endocrinol 7(9):684–694
Clayton JA, Collins FS (2014) Policy: NIH to balance sex in cell and animal studies. Nature 509(7500):282–283
Kur P et al (2020) Sex hormone-dependent physiology and diseases of liver. Int J Environ Res Public Health 17(8):2620
Fernandez-Perez L et al (2014) Lipid profiling and transcriptomic analysis reveals a functional interplay between estradiol and growth hormone in liver. PLoS ONE 9(5):e96305
Davis SR et al (2015) Menopause. Nat Rev Dis Primers 1:15004
Markopoulos MC et al (2015) Hyperandrogenism after menopause. Eur J Endocrinol 172(2):R79-91
Lonardo A et al (2019) Sex differences in nonalcoholic fatty liver disease: state of the art and identification of research gaps. Hepatology 70(4):1457–1469
Ryu S et al (2015) Age at menarche and non-alcoholic fatty liver disease. J Hepatol 62(5):1164–1170
Yi KH et al (2017) Early menarche is associated with non-alcoholic fatty liver disease in adulthood. Pediatr Int 59(12):1270–1275
Lu J et al (2017) Age at menarche is associated with the prevalence of non-alcoholic fatty liver disease later in life. J Diabetes 9(1):53–60
Wang J et al (2021) Associations between reproductive and hormone-related factors and risk of nonalcoholic fatty liver disease in a multiethnic population. Clin Gastroenterol Hepatol 19(6):1258-1266e1
Mueller NT et al (2015) Earlier menarche is associated with fatty liver and abdominal ectopic fat in midlife, independent of young adult BMI: the CARDIA study. Obesity (Silver Spring) 23(2):468–474
Ajmera VH et al (2016) Gestational diabetes mellitus is strongly associated with non-alcoholic fatty liver disease. Am J Gastroenterol 111(5):658–664
Lavrentaki A et al (2019) Increased risk of non-alcoholic fatty liver disease in women with gestational diabetes mellitus: A population-based cohort study, systematic review and meta-analysis. J Diabetes Complicat 33(10):107401
Kubihal S et al (2021) Prevalence of non-alcoholic fatty liver disease and factors associated with it in Indian women with a history of gestational diabetes mellitus. J Diabetes Investig 12(5):877–885
Forbes S et al (2011) Increased prevalence of non-alcoholic fatty liver disease in European women with a history of gestational diabetes. Diabetologia 54(3):641–647
Endres LK et al (2015) Postpartum weight retention risk factors and relationship to obesity at 1 year. Obstet Gynecol 125(1):144–152
Paschou SA et al (2020) Nonalcoholic fatty liver disease in women with polycystic ovary syndrome. Endocrine 67(1):1–8
Polyzos SA et al (2014) Non-alcoholic fatty liver disease in women with polycystic ovary syndrome: assessment of non-invasive indices predicting hepatic steatosis and fibrosis. Hormones (Athens) 13(4):519–531
Vassilatou E et al (2010) Increased androgen bioavailability is associated with non-alcoholic fatty liver disease in women with polycystic ovary syndrome. Hum Reprod 25(1):212–220
Lambrinoudaki I et al (2011) Sex hormones in postmenopausal women receiving low-dose hormone therapy: the effect of BMI. Obesity (Silver Spring) 19(5):988–993
Moghetti P et al (1996) The insulin resistance in women with hyperandrogenism is partially reversed by antiandrogen treatment: evidence that androgens impair insulin action in women. J Clin Endocrinol Metab 81(3):952–960
Sarkar M et al (2017) Testosterone levels in pre-menopausal women are associated with nonalcoholic fatty liver disease in midlife. Am J Gastroenterol 112(5):755–762
Park JM et al (2019) Serum testosterone level within normal range is positively associated with nonalcoholic fatty liver disease in premenopausal but not postmenopausal women. J Womens Health (Larchmt) 28(8):1077–1082
Sarkar MA et al (2021) Testosterone is associated with nonalcoholic steatohepatitis and fibrosis in premenopausal women with NAFLD. Clin Gastroenterol Hepatol 19(6):1267-1274e1
Dilimulati D et al (2021) correlation between sex hormones and non-alcoholic fatty liver disease before and after laparoscopic sleeve gastrectomy. Obes Surg 31(11):4901–4910
Matsuo K et al (2016) Surgical menopause and increased risk of nonalcoholic fatty liver disease in endometrial cancer. Menopause 23(2):189–196
Sarrel PM, Sullivan SD, Nelson LM (2016) Hormone replacement therapy in young women with surgical primary ovarian insufficiency. Fertil Steril 106(7):1580–1587
Lefebvre P, Staels B (2021) Hepatic sexual dimorphism - implications for non-alcoholic fatty liver disease. Nat Rev Endocrinol 17(11):662–670
Palmisano BT, Zhu L, Stafford JM (2017) Role of estrogens in the regulation of liver lipid metabolism. Adv Exp Med Biol 1043:227–256
Mueller NT et al (2020) Sex hormone relations to histologic severity of pediatric nonalcoholic fatty liver disease. J Clin Endocrinol Metab 105(11):3496–3504
Jaruvongvanich V et al (2017) Testosterone, sex hormone-binding globulin and nonalcoholic fatty liver disease: a systematic review and meta-analysis. Ann Hepatol 16(3):382–394
Kojima S et al (2003) Increase in the prevalence of fatty liver in Japan over the past 12 years: analysis of clinical background. J Gastroenterol 38(10):954–961
Florio AA et al (2019) Oophorectomy and risk of non-alcoholic fatty liver disease and primary liver cancer in the Clinical Practice Research Datalink. Eur J Epidemiol 34(9):871–878
Bao T et al (2020) Association between serum uric acid and nonalcoholic fatty liver disease in nonobese postmenopausal women: a cross-sectional study. Sci Rep 10(1):10072
Hong SH et al (2020) Comparison of anthropometric indices for the screening of nonalcoholic fatty liver disease in pre- and postmenopausal women. Menopause 27(1):88–94
Kim HB, Lee YJ (2020) Association of resting heart rate with nonalcoholic fatty liver disease in postmenopausal women. Medicine (Baltimore) 99(14):e19529
Chen Y et al (2019) Association between serum uric acid and non-alcoholic fatty liver disease according to different menstrual status groups. Can J Gastroenterol Hepatol 2019:2763093
Chung GE et al (2015) The influence of metabolic factors for nonalcoholic fatty liver disease in women. Biomed Res Int 2015:131528
Gutierrez-Grobe Y et al (2010) Prevalence of non alcoholic fatty liver disease in premenopausal, posmenopausal and polycystic ovary syndrome women. The role of estrogens. Ann Hepatol 9(4):402–409
Moon SS (2013) Relationship between serum uric acid level and nonalcoholic fatty liver disease in pre- and postmenopausal women. Ann Nutr Metab 62(2):158–163
Ryu S et al (2015) Menopausal stages and non-alcoholic fatty liver disease in middle-aged women. Eur J Obstet Gynecol Reprod Biol 190:65–70
Volzke H et al (2007) Menopausal status and hepatic steatosis in a general female population. Gut 56(4):594–595
Suzuki A et al (2010) Regional anthropometric measures and hepatic fibrosis in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol 8(12):1062–1069
Greendale GA et al (2019) Changes in body composition and weight during the menopause transition. JCI Insight 4(5):e124865
Lambrinoudaki I et al (2018) The metabolic syndrome is associated with carotid atherosclerosis and arterial stiffness in asymptomatic, nondiabetic postmenopausal women. Gynecol Endocrinol 34(1):78–82
Davis SR et al (2012) Understanding weight gain at menopause. Climacteric 15(5):419–429
Tchernof A et al (1998) Menopause, central body fatness, and insulin resistance: effects of hormone-replacement therapy. Coron Artery Dis 9(8):503–511
Brochu M et al (2000) Visceral adipose tissue is an independent correlate of glucose disposal in older obese postmenopausal women. J Clin Endocrinol Metab 85(7):2378–2384
Signorelli SS et al (2006) Behaviour of some indicators of oxidative stress in postmenopausal and fertile women. Maturitas 53(1):77–82
Bourgonje AR et al (2020) Systemic oxidative stress is increased in postmenopausal women and independently associates with homocysteine levels. Int J Mol Sci 21(1):314
Kara A et al (2014) Ultra-structural changes and apoptotic activity in cerebellum of post-menopausal-diabetic rats: a histochemical and ultra-structural study. Gynecol Endocrinol 30(3):226–231
Hamaguchi M et al (2012) Aging is a risk factor of nonalcoholic fatty liver disease in premenopausal women. World J Gastroenterol 18(3):237–243
Veronese N et al (2018) Menopause does not affect fatty liver severity in women: a population study in a Mediterranean area. Endocr Metab Immune Disord Drug Targets 18(5):513–521
Zhou H et al (2019) Prevalence of cardiovascular risk factors in non-menopausal and postmenopausal inpatients with type 2 diabetes mellitus in China. BMC Endocr Disord 19(1):98
Klair JS et al (2016) A longer duration of estrogen deficiency increases fibrosis risk among postmenopausal women with nonalcoholic fatty liver disease. Hepatology 64(1):85–91
Yang JD et al (2014) Gender and menopause impact severity of fibrosis among patients with nonalcoholic steatohepatitis. Hepatology 59(4):1406–1414
Yoneda M et al (2014) The influence of menopause on the development of hepatic fibrosis in nonobese women with nonalcoholic fatty liver disease. Hepatology 60(5):1792
Lazo M et al (2015) Association Between Endogenous Sex Hormones and Liver Fat in a Multiethnic Study of Atherosclerosis. Clin Gastroenterol Hepatol 13(9):1686–1693
Polyzos SA et al (2013) Sex steroids and sex hormone-binding globulin in postmenopausal women with nonalcoholic fatty liver disease. Hormones (Athens) 12(3):405–416
Wang N et al (2016) Combined association of vitamin d and sex hormone binding globulin with nonalcoholic fatty liver disease in men and postmenopausal women: a cross-sectional study. Medicine (Baltimore) 95(4):e2621
Flechtner-Mors M et al (2014) Associations of fatty liver disease and other factors affecting serum SHBG concentrations: a population based study on 1657 subjects. Horm Metab Res 46(4):287–293
Rosner W et al (2013) Challenges to the measurement of estradiol: an endocrine society position statement. J Clin Endocrinol Metab 98(4):1376–1387
Chartampilas E (2018) Imaging of nonalcoholic fatty liver disease and its clinical utility. Hormones (Athens) 17(1):69–81
Wang X et al (2020) Serum SHBG is associated with the development and regression of nonalcoholic fatty liver disease: a prospective study. J Clin Endocrinol Metab 105(3):dgz244
Venetsanaki V, Polyzos SA (2019) Menopause and non-alcoholic fatty liver disease: a review focusing on therapeutic perspectives. Curr Vasc Pharmacol 17(6):546–555
Simo R et al (2012) Potential role of tumor necrosis factor-alpha in downregulating sex hormone-binding globulin. Diabetes 61(2):372–382
Luo J et al (2018) Association of sex hormone-binding globulin with nonalcoholic fatty liver disease in Chinese adults. Nutr Metab (Lond) 15:79
Polyzos SA, Kountouras J, Mantzoros CS (2017) Adipose tissue, obesity and non-alcoholic fatty liver disease. Minerva Endocrinol 42(2):92–108
Shen M, Shi H (2015) Sex hormones and their receptors regulate liver energy homeostasis. Int J Endocrinol 2015:294278
Larsson H, Ahren B (1996) Androgen activity as a risk factor for impaired glucose tolerance in postmenopausal women. Diabetes Care 19(12):1399–1403
Nikolaou N et al (2015) Regulation of lipogenesis in human hepatocytes by androgens, glucocorticoids, and 5[alpha]-reductase. Endocr Abstr. https://doi.org/10.1530/endoabs.37.GP.04.04
Galmes-Pascual BM et al (2020) 17beta-estradiol ameliorates lipotoxicity-induced hepatic mitochondrial oxidative stress and insulin resistance. Free Radic Biol Med 150:148–160
Galmes-Pascual BM et al (2017) 17beta-estradiol improves hepatic mitochondrial biogenesis and function through PGC1B. J Endocrinol 232(2):297–308
Zhu L et al (2013) Estrogen treatment after ovariectomy protects against fatty liver and may improve pathway-selective insulin resistance. Diabetes 62(2):424–434
Cortes E et al (2019) Tamoxifen mechanically deactivates hepatic stellate cells via the G protein-coupled estrogen receptor. Oncogene 38(16):2910–2922
Itagaki T et al (2005) Opposing effects of oestradiol and progesterone on intracellular pathways and activation processes in the oxidative stress induced activation of cultured rat hepatic stellate cells. Gut 54(12):1782–1789
McKenzie J et al (2006) Effects of HRT on liver enzyme levels in women with type 2 diabetes: a randomized placebo-controlled trial. Clin Endocrinol (Oxf) 65(1):40–44
Florentino GS et al (2013) Nonalcoholic fatty liver disease in menopausal women. Arq Gastroenterol 50(3):180–185
Yang JD et al (2017) Patient sex, reproductive status, and synthetic hormone use associate with histologic severity of nonalcoholic steatohepatitis. Clin Gastroenterol Hepatol 15(1):127–131
Nishino M et al (2003) Effects of tamoxifen on hepatic fat content and the development of hepatic steatosis in patients with breast cancer: high frequency of involvement and rapid reversal after completion of tamoxifen therapy. AJR Am J Roentgenol 180(1):129–134
Bruno S et al (2005) Incidence and risk factors for non-alcoholic steatohepatitis: prospective study of 5408 women enrolled in Italian tamoxifen chemoprevention trial. BMJ 330(7497):932
Yan M et al (2017) The relationship between tamoxifen-associated nonalcoholic fatty liver disease and the prognosis of patients with early-stage breast cancer. Clin Breast Cancer 17(3):195–203
Hong N et al (2017) Different patterns in the risk of newly developed fatty liver and lipid changes with tamoxifen versus aromatase inhibitors in postmenopausal women with early breast cancer: a propensity score-matched cohort study. Eur J Cancer 82:103–114
Lee JI et al (2019) Aromatase inhibitors and newly developed nonalcoholic fatty liver disease in postmenopausal patients with early breast cancer: a propensity score-matched cohort study. Oncologist 24(8):e653–e661
Acknowledgements
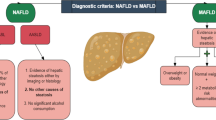
Cartoons in Figure 1 were created with BioRender.com.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
Conceptualization: IL, SAPa. Data investigation: KP, EA. Data interpretation: KP, EA, SAPo, SAPa, DG, IL. Draft preparation: KP. Revision: KP, EA, SAPo, SAPa, DG, IL. Approval of submission: KP, EA, SAPo, SAPa, DG, IL.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethics approval
This study has been approved by the Ethics department of the Aretaieio Hospital, National and Kapodistrian University of Athens.
Informed consent
For this type of study, consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pafili, K., Paschou, S.A., Armeni, E. et al. Non-alcoholic fatty liver disease through the female lifespan: the role of sex hormones. J Endocrinol Invest 45, 1609–1623 (2022). https://doi.org/10.1007/s40618-022-01766-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-022-01766-x