Abstract
Context
Central obesity in polycystic ovary syndrome (PCOS) is associated with increased inflammatory markers and increased risk for type 2 diabetes.
Objective
To evaluate if improved body composition during treatment with metformin (M) vs. oral contraceptive pills (OCP) was associated with changes in circulating adiponectin, interleukin (IL)-6, and monocyte chemoattractant protein (MCP)-1.
Patients and interventions
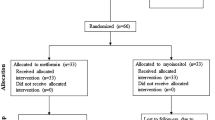
Ninety patients with PCOS were randomized to 12-month treatment with M (2 g/day), M + OCP (150 mg desogestrel + 30 microgram ethinylestradiol) or OCP. Adiponectin, IL-6, MCP-1, whole body DXA scans, and clinical evaluations were performed before and after the intervention period in the 65 study completers.
Main outcome measures
Changes in inflammatory markers and changes in total and regional fat mass estimates.
Results
Adiponectin, IL-6, and MCP-1 levels were unchanged during the three types of medical intervention. Treatment with M and M + OCP was superior to OCP regarding decreased regional fat mass. Baseline adiponectin and IL-6 were associated with BMI, waist, and trunk fat mass. Changes in trunk fat were significantly associated with changes in IL-6 and MCP-1 during M + OCP.
Conclusions
Long-term treatment with M alone or in combination with OCP was associated with improved body composition compared to OCP, whereas inflammatory markers were unchanged. OCP was not associated with increased inflammatory markers despite a small but significant weight gain.
Similar content being viewed by others
References
Glintborg D, Andersen M (2010) An update on the pathogenesis, inflammation, and metabolism in hirsutism and polycystic ovary syndrome. Gynecol Endocrinol 4:281–296
Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group (2004) Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril 1:19–25
Salley KE, Wickham EP, Cheang KI et al (2007) Position statement: glucose intolerance in polycystic ovary syndrome A position statement of the androgen excess Society. J Clin Endocrinol Metab 12:4546–4556
Douchi T, Ijuin H, Nakamura S et al (1995) Body fat distribution in women with polycystic ovary syndrome. Obstet Gynecol 4(Pt 1):516–519
Kirchengast S, Huber J (2001) Body composition characteristics and body fat distribution in lean women with polycystic ovary syndrome. Hum Reprod 6:1255–1260
Libby P, Ridker PM, Maseri A (2002) Inflammation and atherosclerosis. Circulation 9:1135–1143
Eckel RH, Grundy SM, Zimmet PZ (2005) The metabolic syndrome. Lancet 9468:1415–1428
Fasshauer M, Paschke R (2003) Regulation of adipocytokines and insulin resistance. Diabetologia 12:1594–1603
Weisberg SP, McCann D, Desai M et al (2003) Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 12:1796–1808
Bruun JM, Lihn AS, Pedersen SB, Richelsen B (2005) Monocyte chemoattractant protein-1 release is higher in visceral than subcutaneous human adipose tissue (AT): implication of macrophages resident in the AT. J Clin Endocrinol Metab 4:2282–2289
Dandona P, Aljada A, Ghanim H et al (2004) Increased plasma concentration of macrophage migration inhibitory factor (MIF) and MIF mRNA in mononuclear cells in the obese and the suppressive action of metformin. J Clin Endocrinol Metab 10:5043–5047
Diez JJ, Iglesias P (2003) The role of the novel adipocyte-derived hormone adiponectin in human disease. Eur J Endocrinol 3:293–300
Li S, Shin HJ, Ding EL, van Dam RM (2009) Adiponectin levels and risk of type 2 diabetes: a systematic review and meta-analysis. JAMA 2:179–188
Kern PA, Ranganathan S, Li C, Wood L, Ranganathan G (2001) Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance. Am J Physiol Endocrinol Metab 5:E745–E751
Bruun JM, Lihn AS, Verdich C et al (2003) Regulation of adiponectin by adipose tissue-derived cytokines: in vivo and in vitro investigations in humans. Am J Physiol Endocrinol Metab 3:E527–E533
Sell H, Eckardt K, Taube A et al (2008) Skeletal muscle insulin resistance induced by adipocyte-conditioned medium: underlying mechanisms and reversibility. Am J Physiol Endocrinol Metab 6:E1070–E1077
Glintborg D, Andersen M, Hagen C et al (2006) Evaluation of metabolic risk markers in polycystic ovary syndrome (PCOS). Adiponectin, ghrelin, leptin and body composition in hirsute PCOS patients and controls. Eur J Endocrinol 2:337–345
Glintborg D, Frystyk J, Hojlund K et al (2008) Total and high molecular weight (HMW) adiponectin levels and measures of glucose and lipid metabolism following pioglitazone treatment in a randomized placebo-controlled study in polycystic ovary syndrome. Clin Endocrinol (Oxf) 2:165–174
Glintborg D, Andersen M, Richelsen B, Bruun JM (2009) Plasma monocyte chemoattractant protein-1 (MCP-1) and macrophage inflammatory protein-1α are increased in patients with polycystic ovary syndrome (PCOS) and associated with adiposity, but unaffected by pioglitazone treatment. Clin Endocrinol (Oxf) 5:652–658
Azziz R, Carmina E, Dewailly D et al (2009) The androgen excess and PCOS Society criteria for the polycystic ovary syndrome: the complete task force report. Fertil Steril 2:456–488
Bjorntorp P (1996) The android woman––a risky condition. J Intern Med 2:105–110
Cosma M, Swiglo BA, Flynn DN et al (2008) Clinical review: insulin sensitizers for the treatment of hirsutism: a systematic review and metaanalyses of randomized controlled trials. J Clin Endocrinol Metab 4:1135–1142
Bates GW, Legro RS (2013) Longterm management of Polycystic Ovarian Syndrome (PCOS). Mol Cell Endocrinol 1–2:91–97
Ravn P, Haugen AG, Glintborg D (2013) Overweight in polycystic ovary syndrome. An update on evidence based advice on diet, exercise and metformin use for weight loss. Minerva Endocrinol 1:59–76
Shrestha B, Eden J, Sjoblom P, Johnson N (2007) Insulin-sensitising drugs versus the combined oral contraceptive pill for hirsutism, acne and risk of diabetes, cardiovascular disease, and endometrial cancer in polycystic ovary syndrome. Cochrane Database Syst Rev 1:CD005552
Palomba S, Falbo A, Zullo F, Orio F Jr (2009) Evidence-based and potential benefits of metformin in the polycystic ovary syndrome: a comprehensive review. Endocr Rev 1:1–50
Halperin IJ, Kumar SS, Stroup DF, Laredo SE (2011) The association between the combined oral contraceptive pill and insulin resistance, dysglycemia and dyslipidemia in women with polycystic ovary syndrome: a systematic review and meta-analysis of observational studies. Hum Reprod 1:191–201
Sirmans SM, Pate KA (2013) Epidemiology, diagnosis, and management of polycystic ovary syndrome. Clin Epidemiol 6:1–13
Glintborg D, Altinok ML, Mumm H, et al (2014) Body composition is improved during 12 months treatment with metformin alone or combined with oral contraceptives compared to treatment with oral contraceptives in polycystic ovary syndrome. J Clin Endocrinol Metab, jc20141135
Glintborg D, Henriksen JE, Andersen M et al (2004) Prevalence of endocrine diseases and abnormal glucose tolerance tests in 340 Caucasian premenopausal women with hirsutism as the referral diagnosis. Fertil Steril 6:1570–1579
Morin-Papunen LC, Vauhkonen I, Koivunen RM et al (2000) Endocrine and metabolic effects of metformin versus ethinyl estradiol-cyproterone acetate in obese women with polycystic ovary syndrome: a randomized study. J Clin Endocrinol Metab 9:3161–3168
Morin-Papunen L, Vauhkonen I, Koivunen R et al (2003) Metformin versus ethinyl estradiol-cyproterone acetate in the treatment of nonobese women with polycystic ovary syndrome: a randomized study. J Clin Endocrinol Metab 1:148–156
Glintborg D, Andersen M, Hagen C, Hermann AP (2005) Higher bone mineral density in Caucasian, hirsute patients of reproductive age. Positive correlation of testosterone levels with bone mineral density in hirsutism. Clin Endocrinol (Oxf) 6:683–691
Nielsen TL, Hagen C, Wraae K et al (2007) Visceral and subcutaneous adipose tissue assessed by magnetic resonance imaging in relation to circulating androgens, sex hormone-binding globulin, and luteinizing hormone in young men. J Clin Endocrinol Metab 7:2696–2705
Ciaraldi TP, Aroda V, Mudaliar SR, Henry RR (2013) Inflammatory cytokines and chemokines, skeletal muscle and polycystic ovary syndrome: effects of pioglitazone and metformin treatment. Metabolism 11:1587–1596
Trolle B, Lauszus FF, Frystyk J, Flyvbjerg A (2010) Adiponectin levels in women with polycystic ovary syndrome: impact of metformin treatment in a randomized controlled study. Fertil Steril 6:2234–2238
Madsen EL, Rissanen A, Bruun JM et al (2008) Weight loss larger than 10 % is needed for general improvement of levels of circulating adiponectin and markers of inflammation in obese subjects: a 3-year weight loss study. Eur J Endocrinol 2:179–187
Herder C, Peltonen M, Svensson PA, et al (2014) Adiponectin and bariatric surgery: associations with diabetes and cardiovascular disease in the Swedish obese subjects study. Diabetes Care
Lim SS, Norman RJ, Davies MJ, Moran LJ (2013) The effect of obesity on polycystic ovary syndrome: a systematic review and meta-analysis. Obes Rev 2:95–109
Kriplani A, Periyasamy AJ, Agarwal N et al (2010) Effect of oral contraceptive containing ethinyl estradiol combined with drospirenone vs. desogestrel on clinical and biochemical parameters in patients with polycystic ovary syndrome. Contraception 2:139–146
Luque-Ramirez M, Alvarez-Blasco F, Escobar-Morreale HF (2009) Antiandrogenic contraceptives increase serum adiponectin in obese polycystic ovary syndrome patients. Obesity (Silver Spring) 1:3–9
Domecq JP, Prutsky G, Mullan RJ et al (2013) Adverse effects of the common treatments for polycystic ovary syndrome: a systematic review and meta-analysis. J Clin Endocrinol Metab 12:4646–4654
Escobar-Morreale HF, Luque-Ramirez M, Gonzalez F (2011) Circulating inflammatory markers in polycystic ovary syndrome: a systematic review and metaanalysis. Fertil Steril 3:1048–1058
Dardzinska JA, Rachon D, Kuligowska-Jakubowska M et al (2014) Effects of metformin or an oral contraceptive containing cyproterone acetate on serum c-reactive protein, interleukin-6 and soluble vascular cell adhesion molecule-1 concentrations in women with polycystic ovary syndrome. Exp Clin Endocrinol Diabetes 2:118–125
Domecq JP, Prutsky G, Mullan RJ et al (2013) Lifestyle modification programs in polycystic ovary syndrome: systematic review and meta-analysis. J Clin Endocrinol Metab 12:4655–4663
Karjane NW, Cheang KI, Mandolesi GA, Stovall DW (2012) Persistence with oral contraceptive pills versus metformin in women with polycystic ovary syndrome. J Womens Health (Larchmt) 6:690–694
Acknowledgments
The authors thank Lenette Pedersen, Pia Hornbek, Anette Riis Madsen, Lotte Hørlyck, Steffanie Anthony Christensen, Jane Nielsen, Donna Arbuckle-Lund, Elizabeth Hanmann, Jeannette Fogh Lindegaard, Mette Brøchner Hansen, Anne Mette Hangaard, Susanne Møller Pedersen, Geraldine Rasmussen and Thon Kowall Andersen for excellent technical assistance. Financial grants for the studies were supported by Jacob Madsen’s and Olga Madsen’s Foundation, Institute of Clinical Research, Odense University Hospital, Kolding Hospital, AP Møller’s Foundation, Bernhard and Marie Kleins Foundation, The Novo Nordisk Foundation, The Danish Medical Association. Oral contraceptive pills and metformin tablets were sponsored by Sandoz.
Conflict of interest
None of the authors have any conflict of interest that could be perceived as prejudicing the impartiality of the research reported. Sandoz sponsored tablets, but were otherwise not involved in the projects’ economy, planning or writing of article.
Author information
Authors and Affiliations
Corresponding author
Additional information
http://www.clinicaltrials.gov, Registration Number NCT004515 68.
Rights and permissions
About this article
Cite this article
Glintborg, D., Mumm, H., Altinok, M.L. et al. Adiponectin, interleukin-6, monocyte chemoattractant protein-1, and regional fat mass during 12-month randomized treatment with metformin and/or oral contraceptives in polycystic ovary syndrome. J Endocrinol Invest 37, 757–764 (2014). https://doi.org/10.1007/s40618-014-0103-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-014-0103-8