Abstract
Introduction
Many refugees that resettled into the United States (US) arrive with psychological and physical distress. Their health needs are often met with inadequate healthcare. A variety of barriers negatively affect their healthcare access. Knowledge of demographic and social predictors related to key healthcare access components among refugees is limited. This study examines potential predictors of interrupted healthcare coverage—one key component of healthcare access—among refugees living in the US.
Methods
Using the 2016 Annual Survey of Refugees (ASR)nation-wide data collected from 4037 refugees, multiple logistic regression methods were utilized to identify socio-demographic predictors of interrupted healthcare coverage. Interrupted healthcare coverage was defined as one or more months in the past 12 months without coverage by Refugee Medical Assistance (RMA), Medicaid, or private health insurance.
Results
The following five socio-demographic factors were associated with a higher likelihood of interrupted healthcare coverage: Male gender, 20–49 years of age, lack of marriage, resettlement into the south or Midwest, and poor or no current English proficiency. Refugees with no job were less likely to have interrupted coverage compared to employed refugees.
Discussion
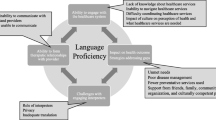
The increased likelihood of interrupted coverage among refugees with poor or no English proficiency supports the belief that limited English proficiency is a barrier to healthcare insurance enrollment. The increased likelihood of interrupted coverage for refugees resettled in the South is consistent with prior literature. In view of clear regional differences, further consideration of the effect of policy differences on refugees living in the US is worthwhile. The findings may help early refugee contacts risk stratify and more effectively allocate limited resources and assist policy makers as they amend and update programs linked to refugee healthcare access (e.g., RMA).
Similar content being viewed by others
Data Availability
The original data source can be obtained at the following DOI: https://doi.org/10.3886/E104642V4.
Code Availability
The entire SAS code used to obtain all statistical results can be obtained by request to the corresponding author.
References
Krogstad J., & Radford J. 2017 Key facts about refugees to the U.S. Pew Research Center. https://www.pewresearch.org/fact-tank/2017/01/30/key-facts-about-refugees-to-the-u-s/. Published January 30, 2017.
Guess MA, Tanabe KO, Nelson AE, Nguyen S, Hauck FR, Scharf RJ. Emergency department and primary care use by refugees compared to non-refugee controls. J Immigr Minor Health. 2019;21(4):793–800.
Pavli, A., & Maltezou, H. (2017). Health problems of newly arrived migrants and refugees in Europe J Travel Med, 2017-07, Vol.24 (4).
Mangrio E, Sjögren Forss K. Refugees’ experiences of healthcare in the host country: a scoping review. BMC Health Serv Res. 2017;17(1):814.
Fazel M, Wheeler J, Danesh J. Prevalence of serious mental disorder in 7000 refugees resettled in western countries: a systematic review. Lancet (British Edition). 2005;365(9467):1309–14.
Kiss V, Pim C, Hemmelgarn BR, Quan H. Building knowledge about health services utilization by refugees. J Immigr Minor Health. 2011;15(1):57–67.
Agrawal P, Venkatesh AK. Refugee resettlement patterns and state-level health care insurance access in the United States. Am J Public Health. 2016;106(4):662–3.
Douangmala CS, Hayden SA, Young LE, Rho J, Schnepper LL. Factors influencing healthcare utilization within a free community clinic. J Immigr Minor Health. 2012;14(4):698–705.
Su D, Wang H, Michaud T, Toure D, Do K, Tak HJ. Acculturation and unmet health needs among refugees in Omaha, Nebraska. J Immigr Minor Health. 2018;21(1):73–9.
Vermette D, Shetgiri R, Al Zuheiri H, Flores G. Healthcare access for Iraqi refugee children in Texas: persistent barriers, potential solutions, and policy implications. J Immigr Minor Health. 2015;17(5):1526–36.
Urban Institute. (2016). 2016 annual survey of refugees. Ann Arbor, MI: inter-university consortium for political and social research [distributor], https://doi.org/10.3886/E104642V4.
Triplett T, & Vilter C. 2016 ASR annual survey of refugees data file user's guide: A technical research manual. Urban Institute, U.S. Department of Health & Human Services. 2018. https://www.openicpsr.org/openicpsr/project/104642/.
Pawlowski B, Atwal R, Dunbar RIM. Sex differences in everyday risk-taking behavior in humans. Evol Psychol. 2008;6(1):29–42.
Lang L. Unmarried older women are twice as likely to lack health insurance. Gastroenterology (New York, NY 1943). 2010;138(7):2195.
Wyn R, Peckham E. Health and health care access among California women ages 50-64. Policy Brief UCLA Cent Health Policy Res. 2010 Feb.
Stephens, J., Artiga, S., Paradise, J. (2018, November 13). Health Coverage and Care in the South in 2014 and Beyond. Retrieved from https://www.kff.org/disparities-policy/issue-brief/health-coverage-and-care-in-the-south-in-2014-and-beyond/
Liaw W, Jetty A, Petterson S, Bazemore A, Green L. Trends in the types of usual sources of care: a shift from people to places or nothing at all. Health Serv Res. 2018;53(4):2346–67.
Arnett MJ, Thorpe RJ, Gaskin DJ, Bowie JV, LaVeist TA. Race, medical mistrust, and segregation in primary care as usual source of care: findings from the exploring health disparities in integrated communities study. J Urban Health. 2016;93(3):456–67.
Shi L, Lebrun LA, Tsai J. The influence of English proficiency on access to care. Ethn Health. 2009;14(6):625–42.
Acknowledgements
I thank Sudha Jayaraman MD, MSc, FACS for her critical review of the original manuscript. I thank Shuo Yu Lin MS for his insight regarding the original statistical analysis revision.
Funding
No funding was obtained.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Kyle Baumann designed and coded the statistical analysis with critical oversight and revision by Tilahun Adera. Kyle Baumann wrote the original draft with critical revision by Tilahun Adera.
Corresponding author
Ethics declarations
Ethics Approval
Since the study does not meet regulatory criteria for human subjects research, Edward Via College of Osteopathic Medicine IRB determined full review and approval unnecessary.
Consent to Participate
Not applicable.
Consent for Publication
All authors give full consent for the publication of this manuscript.
Conflict of Interest
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Baumann, K.J., Adera, T. Predictors of Interrupted Healthcare Coverage in a National Sample of US Refugees. J. Racial and Ethnic Health Disparities 9, 2090–2097 (2022). https://doi.org/10.1007/s40615-021-01147-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-021-01147-9