Abstract
Objective
The objective of this study was to assess whether in-hospital morbidity or mortality differed by race/ethnicity for preterm neonates admitted to the neonatal intensive care unit (NICU).
Study Design
In a retrospective cohort study, preterm infants, < 37 weeks, were admitted to the NICU from 1994 to 2009. Exclusions included structural anomalies and aneuploidy. Primary outcome was in-hospital mortality (IHM). Secondary outcomes were respiratory distress syndrome (RDS), interventricular hemorrhage (IVH), necrotizing enterocolitis (NEC), and retinopathy of prematurity (ROP). Sub-analysis of very preterm (VPT) infants, < 28 weeks, was performed. Five racial/ethnic groups (REGs) were compared: White, Black, Hispanic, Asian, and Mixed. Associations were modeled by logistic regression. White neonates (WNs) were the referent group. Unadjusted and adjusted odds ratios and 95% confidence intervals for remaining REGs were reported. p value was significant at 5% for overall tests and at Bonferroni-corrected level < 0.0125 for between-race comparisons with WNs.
Results
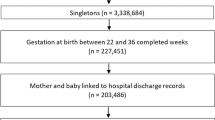
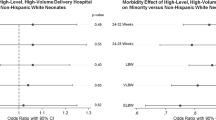
Four thousand nine hundred fifty-five preterm neonates were identified; 153 were excluded leaving 4802 for analysis. After controlling covariates that were chosen a priori, there was no difference across REGs for IHM (all between-race comparison p values > 0.0125). There was a significant difference in RDS among Black neonates (BNs) (aOR 0.57, 95% CI 0.45–0.73; p < 0.001) and Hispanic neonates (HNs) (aOR 0.67, 95% CI 0.50–0.89; p = 0.005) compared to WNs. The risk of ROP was significantly different across REGs with HNs having a 70% increase in ROP (aOR 1.70, 95% CI 1.15–2.49; p = 0.008) and Mixed neonates (MNs) experiencing a 55% reduction (aOR 0.45, 95% CI 0.29–0.68; p < 0.001) compared to WNs. There was no difference in IVH or NEC across REGs (all p values > 0.0125). In the VPT cohort sub-analysis, BNs experienced a significant 59% reduction in IHM compared to WNs (BNs aOR 0.41, 95% CI 0.22–0.73; p = 0.003). MNs experienced a 46% reduction in ROP compared to WNs (aOR 0.54, 95% CI 0.35–0.81; p = 0.004). There was no difference in RDS, IVH, or NEC in very preterm infants across REGs (all between comparison p values > 0.0125).
Conclusion
In preterm neonates, in-hospital mortality does not significantly differ across racial and ethnic groups. However, in very preterm infants, in-hospital mortality for Black neonates is improved. There are morbidity differences (RDS, ROP) seen among racial/ethnic groups.
Similar content being viewed by others
Abbreviations
- RDS:
-
respiratory distress syndrome
- IVH:
-
interventricular hemorrhage
- NEC:
-
necrotizing enterocolitis
- ROP:
-
retinopathy of prematurity
- NICU:
-
neonatal intensive care unit
- VPT:
-
very preterm
- IHM:
-
in-hospital mortality
- REGs:
-
racial and ethnic groups
- WNs:
-
White neonates
- BNs:
-
Black neonates
- CCMC:
-
Connecticut Children’s Medical Center
- aOR:
-
adjusted odds ratio
- CI:
-
confidence intervals
References
Frieden TR, Jaffe HW, Moolenaar RL, Casey CG, Johnson DC, Boyd MF, et al. CDC Health Disparities and Inequalities Report—United States, 2013. MMWR. 2013;62(3):1–2.
Hamilton BE, Martin JA, Osterman MJKS. Births: preliminary data for 2015. Natl Vital Stat Rep. 2015;65(3):1–19.
Martin JA, Hamilton BE, Osterman MJKS, Curtin SC, Mathews TJ. Births: final data for 2013. Natl Vital Stat Rep. 2013;64(1):1–68.
Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller A-B, Narwal R, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379(9832):2162–72.
Mathews TJ, Macdorman MF. Infant mortality statistics from 2010 period linked birth/infant death data set. Natl Vital Stat Rep. 2013;62(8):1–31.
Collins JW, Hawkes EK. Racial differences in post-neonatal mortality in Chicago: what risk factors explain the black infant’s disadvantage? Ethn Health. 2010;2(1–2):117–25.
McGrady GA, Sung JF, Rowley DL, Hogue CJ. Preterm delivery and low birth weight among first-born infants of black and white college graduates. Am J Epidemiol. 1992;136(6):266–76.
Schoendorf KC, Hogue CJ, Kleinman JC, Rowley D. Mortality among infants of black as compared with white college-educated parents. N Engl J Med. 1992;326(23):1522–6.
Boyle RJ, Oh W. Respiratory distress syndrome. Clin Perinatol. 1978;5(2):283–97.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92(4):529–34.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L, et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg. 1978;187(1):1–7.
An International Classification of Retinopathy of Prematurity. Arch Ophthalmol. 1984;102(8):1130–34. https://doi.org/10.1001/archopht.1984.01040030908011.
Ecker JL, Kaimal A, Mercer BM, Blackwell SC, DeRegnier RAO, Farrell RM, et al. ACOG/SMFM consensus #3: periviable birth. Am J Obstet Gynecol. 2015;213(5):604–14.
Petrova A, Mehta R, Anwar M, Hiatt M, Hegyi T. Impact of race and ethnicity on the outcome of preterm infants below 32 weeks gestation. J Perinatol. 2003;23(5):404–8.
Wallace ME, Mendola P, Kim SS, Epps N, Chen Z, Smarr M, et al. Racial/ethnic differences in preterm perinatal outcomes. Am J Obstet Gynecol. 2017;216(3):306.e1–e12.
Bruckner TA, Saxton KB, Anderson E, Goldman S, Gould JB. From paradox to disparity: trends in neonatal death in very low birth weight non-Hispanic black and white infants, 1989-2004. J Pediatr. 2009;155(4):482–487.e1.
Gold KJ, DeMonner SM, Lantz PM, Hayward RA. Prematurity and low birth weight as potential mediators of higher stillbirth risk in mixed black/white race couples. J Womens Health. 2010;19(4):767–73. https://doi.org/10.1089/jwh.2009.1561.
Brandon GD, Adeniyi-Jones S, Kirkby S, Webb D, Culhane JF, Greenspan JS. Are outcomes and care processes for preterm neonates influenced by health insurance status? Pediatrics. 2009;124(1):122–7.
Fassett MJ, Wing DA, Getahun D. Temporal trends in chorioamnionitis by maternal race/ethnicity and gestational age (1995–2010). Int J Reprod Med. 2013;2013:906467. https://doi.org/10.1155/2013/906467.
Lee HC, Lyndon A, Blumenfeld YJ, Dudley RA, Gould JB. Antenatal steroid administration for premature neonates in California. Obstet Gynecol. 2011;117(3):603–9.
Doyle LW, Crowther CA, Middleton P, Marret S, Rouse D. Magnesium sulphate for women at risk of preterm birth for neuroprotection of the fetus. In: Doyle LW, editor. Cochrane database of systematic reviews. John Wiley & Sons, Ltd: Chichester, UK; 2009.
Saunders RA, Donahue ML, Christmann LM, Pakalnis AV, Tung B, Hardy RJ, et al. Racial variation in retinopathy of prematurity. Arch Ophthalmol. 1997;115(5):604.
Eliason KJ, Dane Osborn J, Amsel E, Richards SC. Incidence, progression, and duration of retinopathy of prematurity in Hispanic and white non-Hispanic infants. J Am Assoc Pediatr Ophthalmol Strabismus. 2007;11(5):447–51.
United States Census Bureau: QuickFacts Connecticut, 2015. [Online]. Available: http://www.census.gov/quickfacts/table/PST045215/09. [Accessed: 30-Jul-2016].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Townsel, C., Keller, R., Kuo, CL. et al. Racial/Ethnic Disparities in Morbidity and Mortality for Preterm Neonates Admitted to a Tertiary Neonatal Intensive Care Unit. J. Racial and Ethnic Health Disparities 5, 867–874 (2018). https://doi.org/10.1007/s40615-017-0433-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-017-0433-2