Abstract
Objective
Since 2002, the Klingenstein Third Generation Foundation (KTGF) has supported a network of medical student mentorship programs (MSMPs) across the USA with the explicit aim of enhancing interest in, and eventual recruitment into the field of child and adolescent psychiatry (CAP). The authors conducted a multisite, retrospective cohort analysis to examine the impact of the program on career selection, as reflected by graduation match rates into psychiatry or pediatrics.
Methods
The authors collected graduating match information (2008–2019) from fourteen participating medical schools (Exposed) and thirteen non-participating schools (Control). Control schools were selected based on region, comparable student body and faculty size, national standing, and rank in NIH funding. Match rates into psychiatry and pediatrics were compared between Exposed and Control groups.
Results
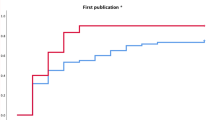
Exposed schools had significantly higher match rates into psychiatry as compared to unexposed schools (6.1% and 4.8%, respectively; OR [95%CI] = 1.29 [1.18, 1.40]; X2 = 32.036, p < 0.001). In contrast, during the same time period, exposed schools had significantly lower match rates into pediatrics than unexposed ones (11.6 and 10.5%, respectively; OR [95%CI] = 0.89 (0.83, 0.95); X2 = 12.127, p < 0.001). These findings persisted even after adjustment for secular trends in match rates.
Conclusions
Seventeen years after its inception, the KTGF medical student mentorship program network has had a positive impact on match rates into general psychiatry. Future studies will address whether these results translate to trainees’ eventual selection of careers in CAP.
Similar content being viewed by others
References
Satiani A, Niedermier J, Satiani B, Svendsen DP. Projected workforce of psychiatrists in the United States: a population analysis. Psychiatr Serv. 2018;69(6):710–3.
Levin SM. The psychiatric workforce now and in the future. Psychiatr Serv. 2018;69(6):714–5.
National Resident Matching Program: main residency match data and reports. http://www.nrmp.org/main-residency-match-data/. Last accessed October 29, 2019.
Agapoff JR, Olson DJ. Challenges and perspectives to the fall in psychiatry fellowship applications. Acad Psychiatry. 2019;43(4):425–8.
Spollen JJ, Beck Dallaghan GL, Briscoe GW, Delanoche ND. Medical school factors associated with higher rates of recruitment into psychiatry. Acad Psychiatry. 2017;41(2):233–8.
Warnke I, Gamma A, Buadze M, et al. Predicting medical students’ current attitudes toward psychiatry, interest in psychiatry, and estimated likelihood of working in psychiatry: a cross-sectional study in four European countries. Frontiers in Psychiatry. 2018;9:49.
Reardon CL, Dottl S, Krahn D. Psychiatry student interest groups: what they are and what they could be. Acad Psychiatry. 2013;37(6):175–8.
Koppelman J. The provider system for children’s mental health: workforce capacity and effective treatment. National Health Policy Forum Issue Brief. 2004;26(801):1–18.
Thomas C, Holzer C. The continuing shortage of child and adolescent psychiatrists. J Am Acad Child Adolesc Psychiatry. 2006;45(9):1023–31.
Findling RL, Stepanova E. The workforce shortage of child and adolescent psychiatrists: is it time for a different approach? J Am Acad Child Adolesc Psychiatry. 2019;57(5):300–1.
Kay C. Child psychiatry recruitment and medical student education. Acad Psychiatry. 1989;13(4):208–12.
Stein JA, Althoff R, Anders T, Davison Y, Edwards S, Frosch E, et al. Does early mentorship in child and adolescent psychiatry make a difference? The Klingenstein Third Generation Foundation Medical Student Fellowship Program. Acad Psychiatry. 2013;37:321–4.
Kishore A, Sun KL, Guth SE, Kolevzon A, Martin A. Child and adolescent psychiatry perceptions and career preference: participation in a national medical student conference improves outcomes. Journal of the American Academy of Child and Adolescent Psychiatry. 2020;59(1):3–7.
Martin A, Bloch M, Stubbe D, Pruett K, Belitsky R, Ebert M, et al. From too little too late to early and often: child psychiatry education during medical school (and before and after). Child and Adolescent Psychiatric Clinics of North America. 2007;16(1):17–43.
Best Medical Schools: Research. U.S. News & World Report Best Graduate Schools Rankings 2019. https://www.usnews.com/best-graduate-schools/top-medical-schools/research-rankings. Last accessed October 21, 2019.
Moran M: Match results show psychiatry remains on upward trend. Psychiatric News. Published online April 7, 2016. https://doi.org/10.1176/appi.pn.2016.4b20. Last accessed October 29, 2019.
Prince S: Is psychiatry cool again? More residents choosing the specialty could mean good news for statewide shortage. Texas Medicine. November 2018. https://www.texmed.org/PsychiatryCoolAgain/. Last accessed October 29, 2019.
What does the psychiatry match data look like? Medical School Headquarters. Podcast Session 59. https://medicalschoolhq.net/ss-59-what-does-the-psychiatry-match-data-look-like/. Last accessed October 29, 2019.
Schlozman SC, Beresin EV. Frustration and opportunity: teaching child and adolescent psychiatry throughout medical education. Acad Psychiatry. 2010;34(3):172–4.
Dean J. Increasing recruitment into child and adolescent psychiatry: a resident’s perspective. Academic Psychiatry. 2017;41:243–5.
Volpe T, Boydell K, Pignatiello A. Choosing child and adolescent psychiatry: factors influencing medical students. Journal of the Canadian Academy of Child and Adolescent Psychiatry. 2013;22(4):260–7.
Lempp T, Neuhoff N, Renner T, Vloet TD, Fischer H, Stegemann T, et al. Who wants to become a child psychiatrist? Lessons for future recruitment strategies from a student survey at seven German medical schools. Academic Psychiatry. 2012;36(3):246–51.
Acknowledgments
An earlier version of this work was presented as a scientific poster at the 66th Annual Conference of the American Academy of Child and Adolescent Psychiatry, Chicago, IL October 16, 2019.
Members of the Klingenstein Third Generation Foundation’s Medical Student Network who contributed to this effort include:
Russell Himmelstein and Sarah Guth (Robert Larner College of Medicine, University of Vermont); Alex Kolevzon (Icahn School of Medicine at Mount Sinai); Michael Enenbach (University of California Los Angeles David Geffen School of Medicine); Geri Fox (University of Illinois at Chicago); Mary Margaret Gleason, Myo Thwin Myint, and Loretta Sonnier (Tulane University); Anne L. Glowinski (Washington University in Saint Louis); Erica Greenberg (Harvard Medical School); Robert Horst (University of California Davis); Anita Kishore and Shashank Joshi (Stanford School of Medicine); Erin Malloy (University of North Carolina at Chapel Hill); Lisell Pérez Rogers (American Academy of Child and Adolescent Psychiatry); Hanna Stevens (University of Iowa); Jennifer Vande Voort (Mayo Clinic Alix School of Medicine); Gerrit van Schalkwyk (Warren Alpert Medical School at Brown); and James F. Leckman and Andrés Martin (Child Study Center, Yale School of Medicine).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Considerations
This study was deemed exempt by the Yale Human Research Protection Program’s Human Investigations Committee (protocol #2000026782).
Funding Sources
Supported by the Klingenstein Third Generation Foundation, which had no role in the analysis or drafting of this report. Additional support provided by the Riva Ariella Ritvo Endowment at the Yale School of Medicine, and by NIMH R25 MH077823, ‘Research Education for Future Physician-Scientists in Child Psychiatry’.
Disclosures
Dr. Glowinski reports funding support from the National Institute of Mental Health and is a member of the ACGME Psychiatry Residency Review Committee. Dr. Kolevzon receives research support from AMO Pharma and has consulted to Ovid Therapeutics, Takeda, 5 AM Ventures, LabCorp, sema4 and Coronis Neurosciences. He sits on the advisory board of the Phelan-McDermid Syndrome Foundation. Dr. Stevens reports funding support from the National Institutes of Health, the Nellie Ball Trust and the Roy J. Carver Trust. Drs. Glowinski, Kolevzon and Stevens sit on the advisory board of the Klingenstein Third Generation Foundation. The other authors have no conflicts to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Himmelstein, R., Guth, S., Enenbach, M. et al. Psychiatry Match Rates Increase After Exposure to a Medical Student Mentorship Program: A Multisite Retrospective Cohort Analysis. Acad Psychiatry 46, 40–44 (2022). https://doi.org/10.1007/s40596-020-01210-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40596-020-01210-3