Abstract
Purpose of Review
The ability of viruses to infect host cells is dependent on several factors including the availability of cell-surface receptors, antiviral state of cells, and presence of host factors needed for viral replication. Here, we review findings from in vitro and in vivo studies using mammalian orthoreovirus (reovirus) that have identified an intricate group of molecules and mechanisms used by the virus to attach and enter cells.
Recent Findings
Recent findings provide an improved mechanistic understanding of reovirus cell entry. Of special note is the identification of a cellular mediator of cell entry in neuronal and non-neuronal cells, the effect of cell entry on the outcome of infection and cytopathic effects on the host cell, and an improved understanding of the components that promote viral penetration of cellular membranes.
Summary
A mechanistic understanding of the interplay between host and viral factors has enhanced our view of how viruses usurp cellular processes during infection.
Similar content being viewed by others
Introduction
As obligate intracellular parasites, viruses depend on their host to replicate and spread. Viral tropism for specific cells, tissues, and hosts is determined by the presence and accessibility of host factors the virus needs to replicate. The outcome of infection is also influenced by the ability of the host to mount an antiviral response to infection. Viruses differ in the specific host molecules used to infect cells and how they evade host immune pathways. However, general principles used by viruses to take over host cells are conserved: viruses attach and enter cells, cross the cellular lipid bilayer, deliver viral nucleic acid to an intracellular site, usurp cellular factors for replication, and exit. Understanding the host and viral factors that promote or mitigate viral infection is essential for the development of efficacious antiviral therapeutics and the engineering of improved viral vectors for gene delivery and oncolytic purposes.
The Reoviridae are a family of non-enveloped, double-stranded RNA (dsRNA), segmented viruses initially isolated from the stools of children in the 1950s [1, 2]. Reovirus is an acronym for respiratory enteric orphan virus [3]. Members of the Reoviridae include rotavirus, the most common cause of pediatric gastroenteritis [4], bluetongue virus, an economically important arthropod-transmitted virus that causes disease in ruminants [5], and mammalian orthoreovirus (reovirus), which infects humans, although disease is restricted to the very young [3, 6]. Serological studies have shown that most humans are exposed to reovirus during childhood, with 35% of children under a year old and approximately 60% of children aged 11–19 years being seropositive for reovirus antibodies [7]. Despite the presence of reovirus-specific antibodies, the majority of reovirus infections in humans are asymptomatic. Reovirus-associated symptoms include coryza, pharyngitis, cough, and gastroenteritis [8, 9] and virus infection has been associated with neonatal biliary atresia [10]. Reovirus is also associated with the development of celiac disease by promoting loss of tolerance to dietary antigens [11••]. Reovirus studies in mice have enhanced our understanding of how the virus disseminates from primary sites of replication [12, 13, 14•, 15, 16], illustrate the importance of the innate and adaptive immune responses in controlling infection [17,18,19,20], and revealed the importance of the gut microbiota in reovirus infection of the gastrointestinal tract [21].
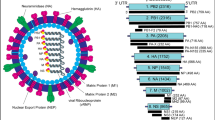
The reovirus particle is 85 nm in diameter and is composed of two concentric capsid shells that contain 10 dsRNA gene segments [22, 23]. Reoviruses contain three large segments (L1, L2, and L3), three medium segments (M1, M2, and M3), and four small segments (S1, S2, S3, and S4) that encode 11 viral proteins, with the S1 gene segment encoding two viral proteins [3]. Three reovirus serotypes have been identified (T1, T2, and T3) based on antibody-mediated neutralization and hemagglutination inhibition (HAI) assays [3]. Four parental viruses isolated in the 1950s from human stool samples [2], type 1 Lang (T1L), type 2 Jones (T2J), type 3 Abney (T3A), and type 3 Dearing (T3D) are commonly used as parental strains. A plasmid-based reverse genetics system for T1L and T3D reoviruses allows facile manipulation of their genome and has enabled studies to understand the contribution of specific viral components to reovirus biology [24].
In neonatal murine animal models, reovirus infection via oral or respiratory routes results in primary infection of the gut or lungs followed by dissemination to secondary sites of replication [3, 16]. The brain, heart, liver, and spleen all support viral replication and are sites of secondary viral replication [3, 12, 16]. Dissemination from the intestine occurs via neural and hematogenous routes, depending on the viral strain [13, 16]. Following oral inoculation, T1L spreads via hematogenous routes, infects ependymal cells in the brain, and causes nonlethal hydrocephalus [15]. T3D spreads via hematogenous and neural routes, infects neurons, and causes lethal encephalitis [13, 15, 16]. These serotype-dependent differences in tropism are linked to the S1 gene segment-encoded σ1 protein [25, 26]. Viral-induced disease is limited to neonatal mice. Reovirus replication in the brains of 7–10-day-old mice is limited and these mice have decreased mortality. Reovirus infection of adult mice results in poor viral replication at primary sites of infection, little dissemination to secondary sites, and little to no mortality [27, 28]. Adult mice with an impaired type I interferon response or those lacking B and T cells are susceptible to reovirus-induced disease, suggesting that these components of the immune system are important to limit reovirus-induced pathogenesis in adult animals [18, 29, 30]. In this review, the focus is on how host and viral molecules interact during virus cell entry and how modulation of these steps affects the outcome of reovirus infection.
Attachment to the Cell Surface
The process of reovirus cell entry involves attachment to target cells via a strength-adhesion mechanism whereby the virus attaches to cells by low-affinity interactions with cell-surface carbohydrate followed by strong-affinity interactions with cell-surface proteinaceous receptors. Virions are then internalized via receptor-mediated endocytosis, uncoated by endosomal proteases, resulting in the release of the transcriptionally active viral core into the cytoplasm where viral nucleic acid is delivered. Successful viral entry requires an intricate interplay of host and viral factors. Host innate and adaptive antiviral factors target specific steps in the cell entry process to inhibit infection (Fig. 1).
Cell entry pathways used by reovirus. Three distinct cell entry pathways have been described for reovirus: 1 JAM-A dependent, 2 NgR1 dependent, and 3 ISVP cell entry. 1 Following attachment to the surface via cell-surface carbohydrate, reovirus binds JAM-A with high affinity and is internalized in a β1 integrin-dependent manner via clathrin-mediated endocytosis. Activation of Src kinase targets reovirus to Rab5-marked early endosomes. Transport to Rab7- and Rab9-marked late endosomes and acidification in this compartment (depicted by white circles) promotes cathepsin-mediated disassembly of the viral particle, cellular membrane penetration, and release of the transcriptionally active core into the cytoplasm. 2 In cortical neurons and cells devoid of JAM-A, reovirus engages NgR1 and is internalized into cells. Reovirus may engage NgR1 through outer capsid protein σ3. The endocytic pathway used by the virus following NgR1 binding is not known but is presumed to be similar to that used following JAM-A binding. 3 ISVPs bind JAM-A and may be internalized in a β1 integrin-dependent manner. ISVPs traffic to Rab5-positive early endosomes where they induce membrane penetration in a cathepsin-independent mechanism and release of the transcriptionally active core into the cytoplasm. 4 Impairment of endocytosis results in abortive cell entry. The presence of IFITM3 in endosomes, inhibition of cathepsin activity, disruption of Rab GTPase function, inhibition of Src kinase activity, or genetic disruption of NPXY motifs in β1 integrin affect the endocytic sorting of reovirus and inhibit infection
Reovirus attachment to cells occurs via interactions of the S1-encoded reovirus attachment fiber σ1 to cell-surface carbohydrates [31]. Both T1 and T3 reoviruses bind sialic acid, although they do so through different regions of the σ1 protein [32••, 33, 34]. T1 reovirus agglutinates human and non-human primate erythrocytes, whereas T3 reovirus agglutinates erythrocytes from various mammalian species [35, 36], suggesting these serotypes engage different glycans. Glycan array screening revealed that T1 reovirus binds GM2 glycan, whereas T3 reovirus binds various sialylated glycans [32••, 33, 34]. Glycan binding by reovirus dictates viral tropism and spread in vivo. T1 reovirus that is deficient in GM2 binding does not infect ependymal cells as efficiently and induces substantially less hydrocephalus in infected animals than wild-type reovirus [37•]. T3 reoviruses that are deficient on sialic acid binding are impaired in their ability to disseminate from the intestines to secondary sites of viral replication and replicate to lower titers in the spinal cord and brains of infected animals [38, 39]. Monoclonal antibodies that neutralize T1 and T3 reovirus infection by binding sites on σ1 also impair T1 and T3 hemagglutination of erythrocytes, suggesting they impair T1 and T3 glycan binding [40]. Together, these studies highlight the role of low affinity binding of cell-surface carbohydrates to reovirus infection and reovirus-mediated pathogenesis in small animal models.
Junctional Adhesion Molecule-A, a Reovirus Proteinaceous Receptor
Following attachment to carbohydrate, reovirus engages a proteinaceous receptor, junctional adhesion molecule-A (JAM-A) [41]. JAM-A is an immunoglobulin superfamily protein that localizes mainly to cellular tight junctions [42]. All three reovirus serotypes bind JAM-A through the head domain of attachment fiber σ1 and reovirus structural protein μ2 affects the efficiency of the interaction between the virion and JAM-A through an unknown mechanism [41, 43,44,45]. Also, some rotavirus strains also use JAM-A and other tight junction proteins as co-receptors for cell entry [46]. Whereas engagement of cell-surface carbohydrates is of low affinity, binding to JAM-A is of high affinity [44]. JAM-A binding does not mediate viral internalization, as deletion of the cytoplasmic tail of JAM-A, which includes a PDZ-binding domain that promotes binding of JAM-A to scaffolding proteins within tight junctions is dispensable for reovirus infection [47,48,49]. It is not known how reovirus gains access to JAM-A in tight junctions as reovirus infection does not appear to disrupt tight junction integrity during infection of polarized cells [50]. This is in contrast to group B coxsackieviruses, which enter cells by attaching to decay-accelerating factor (DAF) on the apical surface, promoting the disruption of tight junctions that allows virus access to the tight junction-resident coxsackievirus and adenovirus receptor (CAR) [51]. It is possible that reovirus engages pools of JAM-A not found in tight junctions or is transported to tight junctions without substantial disruption of cellular barrier integrity.
The role of JAM-A in reovirus infection in vivo has been determined through pan JAM-A and tissue-specific JAM-A knockout mice [12, 14•]. Although JAM-A is necessary for reovirus dissemination from the intestines and reovirus-induced disease, reovirus infection of the gastrointestinal tract is unaltered in JAM-A knockout animals [12, 14•]. Intracranial inoculation of JAM-A knockout animals does not affect virus replication in the central nervous system (CNS) [12]. The role of JAM-A in reovirus dissemination to secondary sites of infection was defined through the use of endothelial-specific and hematogenous-specific JAM-A knockout mice [14•]. Eliminating JAM-A expression from endothelial cells impaired reovirus dissemination from the gut. In contrast, lack of expression of JAM-A in hematopoietic cells did not alter reovirus dissemination. These data suggest that JAM-A is not required for infection of the gut or CNS, but essential for reovirus dissemination from the gut into the bloodstream through reovirus infection of JAM-A-expressing endothelial cells.
During reovirus infection of the gut, the virus binds and is taken up by microfold (M) cells [52•, 53]. Interestingly, during respiratory infection, reovirus also uses M cells to gain access to the lungs [54]. The virus does not actively replicate in M cells, but transits through these cells and infects M cell-adjacent enterocytes through the basolateral surface [52•, 53]. Reovirus antigen is also detected in the villus tips of infected animals [12, 13], although it is unclear if this represents primary infection or sites of replication after the virus has trafficked through intestinal M cells. Moreover, the presence of host bacterial microbiota positively influences reovirus infection of the gut [21]. Although there is no direct evidence to show if JAM-A expression is necessary for reovirus infection of specific sites within the gut, the lack of an impairment on reovirus replication within the gastrointestinal tract in JAM-A knockout animals strongly suggests that infection of intestinal cells is JAM-A independent. The identity of the cellular receptor that promotes reovirus infection of the gut is unknown.
Nogo Receptor 1
Reovirus infection of the CNS is JAM-A independent [12]. Through genome-wide RNAi screening, nogo receptor 1 (NgR1), a glycosylphosphatidylinositol (GPI)-anchored protein that is expressed on the cell surface of neurons, was shown to mediate infection of primary murine cortical neurons as well as HeLa cells and Chinese hamster ovary (CHO) cells [55••]. Expression of NgR1 in trans enhances reovirus attachment to cells and NgR1-specific antibodies impair reovirus attachment and infectivity of CHO cells. Reovirus infection of primary murine cortical neurons lacking NgR1 and infection in the presence of NgR1-specific antibodies is severely impaired, suggesting that NgR1 is key for productive infection of neurons. Interestingly, in vitro-generated infectious subvirion particles (ISVPs) that lack the σ3 structural protein but contain the σ1 attachment fiber are unable to infect NgR1-expressing CHO cells. These data indicate that NgR1 mediates reovirus infection of a subset of cells in the CNS and that engagement of NgR1 by reovirus occurs either through the σ3 structural protein or a specific conformation of the σ1 attachment fiber found in virions. NgR1 expression in the CNS mirror sites that are susceptible to T3 reovirus infection, including the thalamus, middle and outer layers of the cerebral cortex, the CA3 region of the hippocampus, and cerebellar Purkinje cells [12, 56]. Whether NgR1 is essential for infection of the CNS in vivo, how it affects reovirus pathogenesis by T1 and T3 reoviruses, and how it affects reovirus infection at other sites besides the CNS remain to be determined.
Reovirus Internalization
Following attachment to cell-surface carbohydrate, JAM-A, and NgR1, reovirus is internalized by receptor-mediated endocytosis. Endocytosis in some cells is dependent on β1 integrin [48, 57], although it is unclear if the virus directly or indirectly engages β1 integrin or if the virus utilizes signaling from β1 integrin to promote endocytosis. The viral core protein λ2 has conserved RGD and KGE integrin-binding motifs that are solvent exposed in the virion [56, 58]. However, it is not known if these motifs mediate direct interaction with β1 integrin or if they have another function during reovirus infection. Although the cytoplasmic tail of JAM-A is dispensable for reovirus internalization [47], NPXY motifs found in the cytoplasmic tail of β1 integrin are necessary for efficient infection and internalization [57]. NPXY motifs have been shown to mediate the association of β1 integrin with the actin cytoskeleton and regulate integrin signaling [59]. Several rotavirus strains use integrins to infect cells [60], suggesting a conserved mechanism exploited by the Reoviridae. The exact signaling events and molecules recruited to the site of viral entry triggered by the engagement of integrins by reovirus are not well defined.
Reovirus endocytosis is primarily dependent on clathrin [57, 61]. However, there is mounting evidence that other mechanisms are involved in the cellular uptake of the virus, including dynamin-dependent and dynamin-independent mechanisms [57, 62]. Following internalization, the virus is transported through Rab5-positive early endosomes to Rab7- and Rab9-positive late endosomes where cathepsin proteases perform acid-dependent proteolysis of the viral particle [63,64,65,66,67]. JAM-A is observed in the same endosomal compartments as reovirus during cell entry [67]. Viral particles are also observed in slow and fast recycling compartments, but impairment of these compartments does not diminish reovirus infectivity [67]. It is unclear if virus present in recycling compartments is recycled to the cell surface where it may re-initiate cell entry or if this compartment is a non-productive cell entry route. It is possible that virions that end up in the recycling compartment define a subset of viral particles that failed to induce the necessary molecules or signaling events needed for productive cell entry.
Different reovirus particle types use distinct endocytic entry routes which affect the fate of the infected cell. Whereas virions must traverse through early and late endosomes to productively infect cells, in vitro-generated ISVPs enter cells by engaging cell-surface carbohydrate and JAM-A, followed by receptor mediated endocytosis, and transport to early, but not late, endosomes [41, 62, 66, 68]. During the natural course of infection, ISVPs are generated during the endocytic transport of virions through the endosomal system by cathepsin cleavage of the viral particle presumably in late endosomes [64, 69]. As ISVPs have been proteolytically digested, infection with extracellularly-produced ISVPs is able to bypass the need for cathepsin-mediated digestion of the virion to promote membrane penetration. In vivo, ISVPs are generated in the intestinal lumen by resident proteases and are thought to be the type of viral particle that enters M cells in the gut [70]. In intestinal epithelial cells, the alternate endocytic transport route taken by ISVPs yields a dampened innate immune response and induction of a pro-survival state through TGF-β production [71•]. In contrast, infection of intestinal epithelial cells with virions strongly activates the innate immune response and results in significant levels of cell death [71•]. These data indicate that the route of infection can greatly affect not only the fate of the incoming virion, but also the ultimate outcome of infection. It remains to be determined if ISVPs infect other cells beyond those in the gut during in vivo infection and whether pro-survival pathways are induced following reovirus infection of the intestines.
Engagement of several host factors beyond cell-surface carbohydrate, JAM-A, NgR1, and β1 integrin are important for efficient reovirus cell entry. Src kinase, the prototype member of the Src family of kinases, is activated and colocalizes with reovirus virions during cell entry [72]. Infection in the presence of a Src kinase inhibitor or infection of cells that are devoid of Src kinase results in the aberrant transport of reovirus to lysosomes [72]. The activation of Src family kinases is also used by coxsackievirus B following engagement of DAF [51], suggesting this is a conserved mechanism used by viruses to productively enter cells. In the context of coxsackievirus infection, Fyn kinase activation promotes actin rearrangement that is needed for the transport of virions to tight junctions and subsequent internalization by caveolin-mediated endocytosis [51]. In contrast to coxsackievirus, Src activity does not affect the overall internalization of reovirus. How reovirus activates Src and the downstream factors modified by Src that promote reovirus infection are not known.
Other molecules that modulate reovirus infection at the cell entry step include serotonin receptors (5-HTR) and the interferon-inducible transmembrane protein 3 (IFITM3) [73, 74]. Inducing 5-HTR signaling with the agonist 5-nonyloxytrymptamine (5-NT) impairs reovirus infection, whereas antagonizing 5-HTRs enhance infectivity [74]. Treatment of cells with 5-NT impairs reovirus infection by affecting cell entry kinetics through disruption of early endosome localization [74]. The effect of 5-NT is not reovirus specific, as infection with the alphavirus chikungunya virus and the coronavirus murine hepatitis virus (MHV), both of which use early endosomes to enter cells, was impaired by 5-NT [43, 75, 76]. The interferon-inducible IFITM3, which localizes to late endosomes, restricts infection of reovirus virions but not ISVPs [73]. IFITM family of proteins has been shown to restrict infection of coronaviruses, filoviruses, and influenza virus at a step involving late endosomes [77, 78]. As such, the late endosomal compartment appears to be a bottleneck where the host has evolved mechanisms to antagonize virus infection by a variety of viruses.
Membrane Penetration
Reovirus access to the late endosomal compartment results in the proteolytic disassembly of virions by cathepsins B, L, and S [63, 65, 79, 80]. Cathepsin proteolysis is also used during Ebola virus entry [81, 82] and severe acute respiratory syndrome coronavirus (SARS-CoV) utilizes cathepsins to process its glycoprotein prior to fusion with the cell membrane [83, 84]. Cathepsin cleavage in late endosomes give rise to ISVPs, which are characterized by the loss of the outer capsid protein σ3, conformational changes in σ1, and cleavage of the major capsid protein μ1 [3]. Although the low pH environment of the late endosome is essential for cathepsin activity [69], artificially lowering endosomal pH is detrimental to reovirus infection [85]. These data suggest that reovirus disassembly kinetics are perfectly orchestrated to use both the lower pH environment of late endosomes and the proteolytic activity of cathepsins. Cleavage of the μ1 protein releases an N-terminally myristoylated fragment that associates with cellular membranes and is capable of pore formation [86, 87]. The interaction of the μ1 cleavage fragment with lipid membranes not only drives pore formation, but also affects the disassembly of the viral particle [88, 89]. Besides cathepsins, the cellular chaperone Hsp70 participates in reovirus cell entry by removing residual μ1 fragments from virions [90]. It is unclear if Hsp70 activity also promotes the transport of the virion across the endosomal membrane. The cell entry process culminates with endosomal membrane penetration by a transcriptionally active viral core that delivers viral transcripts in the cytoplasm of host cells [3].
Conclusions
Studies on reovirus cell entry have shown an intricate process used by the virus to attach to host cells, trigger endocytic events that culminate with membrane penetration by the viral particle, and release of viral nucleic acid into the cytoplasm of cells. It is revealing that a variety of viruses, from reovirus to coronaviruses, picornaviruses, and filoviruses, have evolved to use similar molecular mechanisms to gain entry into their host. This highlights the importance of studies of host and pathogen interactions, as they are likely to illuminate mechanisms used by several viruses and provide valuable insights for the development of antiviral therapeutics.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Rosen L. Serologic grouping of reoviruses by hemagglutination-inhibition. Am J Hyg. 1960;71:242–9.
Sabin AB. Reoviruses. A new group of respiratory and enteric viruses formerly classified as ECHO type 10 is described. Science. New York, NY. 1959;130(3386):1387–1389.
Dermody TS, Parker J, Sherry B. Orthoreoviruses. In: Knipe DM, Howley PM, editors. Fields virology. 2. Sixth ed. Philadelphia: Lippincott Williams & Wilkins; 2013. p. 1304–1346.
Parashar UD, Bresee JS, Gentsch JR, et al. Rotavirus. Emerg Infect Dis. 1998;4(4):561–70.
Maclachlan NJ. Bluetongue: history, global epidemiology, and pathogenesis. Prev Vet Med. 2011;102(2):107–11.
Ouattara LA, Barin F, Barthez MA, et al. Novel human reovirus isolated from children with acute necrotizing encephalopathy. Emerg Infect Dis. 2011;17(8):1436–44.
Selb B, Weber B. A study of human reovirus IgG and IgA antibodies by ELISA and western blot. J Virol Methods. 1994;47(1–2):15–25.
Giordano MO, Martinez LC, Isa MB, et al. Twenty year study of the occurrence of reovirus infection in hospitalized children with acute gastroenteritis in Argentina. Pediatr Infect Dis J. 2002;21(9):880–2.
Jackson GG, Muldoon RL. Viruses causing common respiratory infection in man. IV. Reoviruses and adenoviruses. J Infect Dis. 1973;128(6):811–66.
Tyler KL, Sokol RJ, Oberhaus SM, et al. Detection of reovirus RNA in hepatobiliary tissues from patients with extrahepatic biliary atresia and choledochal cysts. Hepatology. 1998;27(6):1475–82.
•• Bouziat R, Hinterleitner R, Brown JJ, et al. Reovirus infection triggers inflammatory responses to dietary antigens and development of celiac disease. Science (New York, NY. 2017;356(6333):44-50. First report of reovirus association with celiac disease through the promotion of loss of tolerance to dietary antigen.
Antar AA, Konopka JL, Campbell JA, et al. Junctional adhesion molecule-A is required for hematogenous dissemination of reovirus. Cell Host Microbe. 2009;5(1):59–71.
Boehme KW, Guglielmi KM, Dermody TS. Reovirus nonstructural protein sigma1s is required for establishment of viremia and systemic dissemination. Proc Natl Acad Sci U S A. 2009;106(47):19986–91.
• Lai CM, Boehme KW, Pruijssers AJ, et al. Endothelial JAM-A promotes reovirus viremia and bloodstream dissemination. J Infect Dis. 2015;211(3):383–93. Identification of hematogenous JAM-A in reovirus dissemination from the gut.
Tyler KL, McPhee DA, Fields BN. Distinct pathways of viral spread in the host determined by reovirus S1 gene segment. Science (New York, NY. 1986;233(4765):770–4.
Boehme KW, Lai CM, Dermody TS. Mechanisms of reovirus bloodstream dissemination. Adv Virus Res. 2013;87:1–35.
Baldridge MT, Lee S, Brown JJ, et al. Expression of Ifnlr1 on intestinal epithelial cells is critical to the antiviral effects of interferon lambda against norovirus and reovirus. J Virol. 2017;91(7).
Johansson C, Wetzel JD, He J, et al. Type I interferons produced by hematopoietic cells protect mice against lethal infection by mammalian reovirus. J Exp Med. 2007;204(6):1349–58.
Holm GH, Pruijssers AJ, Li L, et al. Interferon regulatory factor 3 attenuates reovirus myocarditis and contributes to viral clearance. J Virol. 2010;84(14):6900–8.
Irvin SC, Zurney J, Ooms LS, et al. A single-amino-acid polymorphism in reovirus protein mu2 determines repression of interferon signaling and modulates myocarditis. J Virol. 2012;86(4):2302–11.
Kuss SK, Best GT, Etheredge CA, et al. Intestinal microbiota promote enteric virus replication and systemic pathogenesis. Science (New York, NY. 2011;334(6053):249–52.
Shatkin AJ, Sipe JD, Loh P. Separation of ten reovirus genome segments by polyacrylamide gel electrophoresis. J Virol. 1968;2(10):986–91.
Ramig RF, Cross RK, Fields BN. Genome RNAs and polypeptides of reovirus serotypes 1, 2, and 3. J Virol. 1977;22(3):726–33.
Kobayashi T, Antar AA, Boehme KW, et al. A plasmid-based reverse genetics system for animal double-stranded RNA viruses. Cell Host Microbe. 2007;1(2):147–57.
Kauffman RS, Wolf JL, Finberg R, et al. The sigma 1 protein determines the extent of spread of reovirus from the gastrointestinal tract of mice. Virology. 1983;124(2):403–10.
Morin MJ, Warner A, Fields BN. Reovirus infection in rat lungs as a model to study the pathogenesis of viral pneumonia. J Virol. 1996;70(1):541–8.
Mann MA, Knipe DM, Fischbach GD, et al. Type 3 reovirus neuroinvasion after intramuscular inoculation: direct invasion of nerve terminals and age-dependent pathogenesis. Virology. 2002;303(2):222–31.
Tardieu M, Powers ML, Weiner HL. Age dependent susceptibility to Reovirus type 3 encephalitis: role of viral and host factors. Ann Neurol. 1983;13(6):602–7.
Haller BL, Barkon ML, Vogler GP, et al. Genetic mapping of reovirus virulence and organ tropism in severe combined immunodeficient mice: organ-specific virulence genes. J Virol. 1995;69(1):357–64.
George A, Kost SI, Witzleben CL, et al. Reovirus-induced liver disease in severe combined immunodeficient (SCID) mice. A model for the study of viral infection, pathogenesis, and clearance. J Exp Med. 1990;171(3):929–34.
Gentsch JR, Pacitti AF. Differential interaction of reovirus type 3 with sialylated receptor components on animal cells. Virology. 1987;161(1):245–8.
•• Reiss K, Stencel JE, Liu Y, et al. The GM2 glycan serves as a functional coreceptor for serotype 1 reovirus. PLoS Pathogens. 2012;8(12):e1003078. Identification of GM2 as the glycan used by T1 reoviruses.
Reiter DM, Frierson JM, Halvorson EE, et al. Crystal structure of reovirus attachment protein sigma1 in complex with sialylated oligosaccharides. PLoS Pathog. 2011;7(8):e1002166.
Stencel-Baerenwald JE, Reiss K, Reiter DM, et al. The sweet spot: defining virus-sialic acid interactions. Nat Rev Microbiol. 2014;12(11):739–49.
Eggers HJ, Gomatos PJ, Tamm I. Agglutination of bovine erythrocytes: a general characteristic of reovirus type 3. Proc Soc Exp Biol Med. 1962;110:879–81.
Weiner HL, Ramig RF, Mustoe TA, et al. Identification of the gene coding for the hemagglutinin of reovirus. Virology. 1978;86(2):581–4.
• Stencel-Baerenwald J, Reiss K, Blaum BS, et al. Glycan engagement dictates hydrocephalus induction by serotype 1 reovirus. mBio. 2015;6(2):e02356. Study showing the effects of glycan utilization in T1 reovirus-induced disease.
Barton ES, Youree BE, Ebert DH, et al. Utilization of sialic acid as a coreceptor is required for reovirus-induced biliary disease. J Clin Invest. 2003;111(12):1823–33.
Frierson JM, Pruijssers AJ, Konopka JL, et al. Utilization of sialylated glycans as coreceptors enhances the neurovirulence of serotype 3 reovirus. J Virol. 2012;86(24):13164–73.
Dietrich MH, Ogden KM, Katen SP, et al.. Structural insights into reovirus sigma1 interactions with two neutralizing antibodies. J Virol. 2017;91(4).
Barton ES, Forrest JC, Connolly JL, et al. Junction adhesion molecule is a receptor for reovirus. Cell. 2001;104(3):441–51.
Martin-Padura I, Lostaglio S, Schneemann M, et al. Junctional adhesion molecule, a novel member of the immunoglobulin superfamily that distributes at intercellular junctions and modulates monocyte transmigration. J Cell Biol. 1998;142(1):117–27.
Schelling P, Guglielmi KM, Kirchner E, et al. The reovirus sigma1 aspartic acid sandwich: a trimerization motif poised for conformational change. J Biol Chem. 2007;282(15):11582–9.
Barton ES, Connolly JL, Forrest JC, et al. Utilization of sialic acid as a coreceptor enhances reovirus attachment by multistep adhesion strengthening. J Biol Chem. 2001;276(3):2200–11.
Thete D, Snyder AJ, Mainou BA, et al. Reovirus mu1 protein affects infectivity by altering virus-receptor interactions. J Virol. 2016;90(23):10951–62.
Torres-Flores JM, Silva-Ayala D, Espinoza MA, et al. The tight junction protein JAM-A functions as coreceptor for rotavirus entry into MA104 cells. Virology. 2015;475:172–8.
Danthi P, Hansberger MW, Campbell JA, et al. JAM-A-independent, antibody-mediated uptake of reovirus into cells leads to apoptosis. J Virol. 2006;80(3):1261–70.
Maginnis MS, Forrest JC, Kopecky-Bromberg SA, et al. Beta1 integrin mediates internalization of mammalian reovirus. J Virol. 2006;80(6):2760–70.
Severson EA, Parkos CA. Structural determinants of Junctional Adhesion Molecule A (JAM-A) function and mechanisms of intracellular signaling. Curr Opin Cell Biol. 2009;21(5):701–7.
Lai CM, Mainou BA, Kim KS, et al. Directional release of reovirus from the apical surface of polarized endothelial cells. mBio. 2013;4(2):e00049–13.
Coyne CB, Bergelson JM. Virus-induced Abl and Fyn kinase signals permit coxsackievirus entry through epithelial tight junctions. Cell. 2006;124(1):119–31.
• Gonzalez-Hernandez MB, Liu T, Payne HC, et al. Efficient norovirus and reovirus replication in the mouse intestine requires microfold (M) cells. J Virol. 2014;88(12):6934–43. In vivo study showing importance of M cells in reovirus infection of the gut.
Wolf JL, Rubin DH, Finberg R, et al. Intestinal M cells: a pathway for entry of reovirus into the host. Science (New York, NY 1981;212(4493):471–2.
Morin MJ, Warner A, Fields BN. A pathway for entry of reoviruses into the host through M cells of the respiratory tract. J Exp Med. 1994;180(4):1523–7.
•• Konopka-Anstadt JL, Mainou BA, Sutherland DM, et al. The Nogo receptor NgR1 mediates infection by mammalian reovirus. Cell Host Microbe. 2014;15(6):681–91. Identification of NgR1 as a mediator of reovirus infection of neurons.
Wang X, Chun SJ, Treloar H, et al. Localization of Nogo-A and Nogo-66 receptor proteins at sites of axon-myelin and synaptic contact. J Neurosci. 2002;22(13):5505–15.
Maginnis MS, Mainou BA, Derdowski A, et al. NPXY motifs in the beta1 integrin cytoplasmic tail are required for functional reovirus entry. J Virol. 2008;82(7):3181–91.
Breun LA, Broering TJ, McCutcheon AM, et al. Mammalian reovirus L2 gene and lambda2 core spike protein sequences and whole-genome comparisons of reoviruses type 1 Lang, type 2 Jones, and type 3 Dearing. Virology. 2001;287(2):333–48.
Moser M, Legate KR, Zent R, et al. The tail of integrins, talin, and kindlins. Science (New York, NY. 2009;324(5929):895–899.
Lopez S, Arias CF. Early steps in rotavirus cell entry. Curr Top Microbiol Immunol. 2006;309:39–66.
Ehrlich M, Boll W, Van Oijen A, et al. Endocytosis by random initiation and stabilization of clathrin-coated pits. Cell. 2004;118(5):591–605.
Schulz WL, Haj AK, Schiff LA. Reovirus uses multiple endocytic pathways for cell entry. J Virol. 2012;86(23):12665–75.
Doyle JD, Danthi P, Kendall EA, et al. Molecular determinants of proteolytic disassembly of the reovirus outer capsid. J Biol Chem. 2012;287(11):8029–38.
Ebert DH, Deussing J, Peters C, et al. Cathepsin L and cathepsin B mediate reovirus disassembly in murine fibroblast cells. J Biol Chem. 2002;277(27):24609–17.
Johnson EM, Doyle JD, Wetzel JD, et al. Genetic and pharmacologic alteration of cathepsin expression influences reovirus pathogenesis. J Virol. 2009;83(19):9630–40.
Boulant S, Stanifer M, Kural C, et al. Similar uptake but different trafficking and escape routes of reovirus virions and infectious subvirion particles imaged in polarized Madin-Darby canine kidney cells. Mol Biol Cell. 2013;24(8):1196–207.
Mainou BA, Dermody TS. Transport to late endosomes is required for efficient reovirus infection. J Virol. 2012;86(16):8346–58.
Nibert ML, Chappell JD, Dermody TS. Infectious subvirion particles of reovirus type 3 Dearing exhibit a loss in infectivity and contain a cleaved sigma 1 protein. J Virol. 1995;69(8):5057–67.
Chapman HA, Riese RJ, Shi GP. Emerging roles for cysteine proteases in human biology. Annu Rev Physiol. 1997;59:63–88.
Amerongen HM, Wilson GA, Fields BN, et al. Proteolytic processing of reovirus is required for adherence to intestinal M cells. J Virol. 1994;68(12):8428–32.
• Stanifer ML, Rippert A, Kazakov A, et al. Reovirus intermediate subviral particles constitute a strategy to infect intestinal epithelial cells by exploiting TGF-beta dependent pro-survival signaling. Cellular Microbiol. 2016;18(12):1831–45. Study highlighting different outcomes of infection of intestinal epithelial cells between virions and ISVPs.
Mainou BA, Dermody TS. Src kinase mediates productive endocytic sorting of reovirus during cell entry. J Virol. 2011;85(7):3203–13.
Anafu AA, Bowen CH, Chin CR, et al. Interferon-inducible transmembrane protein 3 (IFITM3) restricts reovirus cell entry. J Biol Chem. 2013;288(24):17261–71.
Mainou BA, Ashbrook AW, Smith EC, et al. Serotonin receptor agonist 5-nonyloxytryptamine alters the kinetics of reovirus cell entry. J Virol. 2015;89(17):8701–12.
Bernard E, Solignat M, Gay B, et al. Endocytosis of chikungunya virus into mammalian cells: role of clathrin and early endosomal compartments. PLoS One. 2010;5(7):e11479.
Burkard C, Verheije MH, Wicht O, et al. Coronavirus cell entry occurs through the endo-/lysosomal pathway in a proteolysis-dependent manner. PLoS Pathog. 2014;10(11):e1004502.
Huang IC, Bailey CC, Weyer JL, et al. Distinct patterns of IFITM-mediated restriction of filoviruses, SARS coronavirus, and influenza A virus. PLoS Pathog. 2011;7(1):e1001258.
Feeley EM, Sims JS, John SP, et al. IFITM3 inhibits influenza A virus infection by preventing cytosolic entry. PLoS Pathog. 2011;7(10):e1002337.
Ebert DH, Wetzel JD, Brumbaugh DE, et al. Adaptation of reovirus to growth in the presence of protease inhibitor E64 segregates with a mutation in the carboxy terminus of viral outer-capsid protein sigma3. J Virol. 2001;75(7):3197–206.
Golden JW, Bahe JA, Lucas WT, et al. Cathepsin S supports acid-independent infection by some reoviruses. J Biol Chem. 2004;279(10):8547–57.
Chandran K, Sullivan NJ, Felbor U, et al. Endosomal proteolysis of the Ebola virus glycoprotein is necessary for infection. Science (New York, NY. 2005;308(5728):1643–1645.
Misasi J, Chandran K, Yang JY, et al. Filoviruses require endosomal cysteine proteases for entry but exhibit distinct protease preferences. J Virol. 2012;86(6):3284–92.
Huang IC, Bosch BJ, Li F, et al. SARS coronavirus, but not human coronavirus NL63, utilizes cathepsin L to infect ACE2-expressing cells. J Biol Chem. 2006;281(6):3198–203.
Simmons G, Gosalia DN, Rennekamp AJ, et al. Inhibitors of cathepsin L prevent severe acute respiratory syndrome coronavirus entry. Proc Natl Acad Sci U S A. 2005;102(33):11876–81.
Thete D, Danthi P. Conformational changes required for reovirus cell entry are sensitive to pH. Virology. 2015;483:291–301.
Agosto MA, Ivanovic T, Nibert ML. Mammalian reovirus, a nonfusogenic nonenveloped virus, forms size-selective pores in a model membrane. Proc Natl Acad Sci U S A. 2006;103(44):16496–501.
Ivanovic T, Agosto MA, Zhang L, et al. Peptides released from reovirus outer capsid form membrane pores that recruit virus particles. EMBO J. 2008;27(8):1289–98.
Snyder AJ, Danthi P. Lipids cooperate with the reovirus membrane penetration peptide to facilitate particle uncoating. J Biol Chem. 2016;291(52):26773–85.
Snyder AJ, Danthi P. Lipid membranes facilitate conformational changes required for reovirus cell entry. J Virol. 2015;90(5):2628–38.
Ivanovic T, Agosto MA, Chandran K, et al. A role for molecular chaperone Hsc70 in reovirus outer capsid disassembly. J Biol Chem. 2007;282(16):12210–9.
Acknowledgements
The author would like to thank Angela K. Berger for critical feedback on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The author declares that he has no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the author.
Additional information
This article is part of the Topical Collection on Virology
Rights and permissions
About this article
Cite this article
Mainou, B.A. The Orchestra of Reovirus Cell Entry. Curr Clin Micro Rpt 4, 142–149 (2017). https://doi.org/10.1007/s40588-017-0067-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40588-017-0067-5