Abstract
Purpose of Review
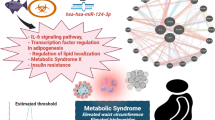
Metabolic syndrome (MS) describes the co-occurrence of conditions that increase one’s risk for heart disease and other disorders such as diabetes and stroke. The worldwide increase in the prevalence of MS cannot be fully explained by lifestyle factors such as sedentary behavior and caloric intake alone. Environmental exposures, such as heavy metals, have been implicated, but results are conflicting and possible mechanisms remain unclear. To assess recent progress in determining a possible role between heavy metal exposure and MS, we reviewed epidemiological and model system data for cadmium (Cd), lead (Pb), and mercury (Hg) from the last decade.
Recent Findings
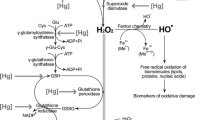
Data from 36 epidemiological studies involving 17 unique countries/regions and 13 studies leveraging model systems are included in this review. Epidemiological and model system studies support a possible association between heavy metal exposure and MS or comorbid conditions; however, results remain conflicting. Epidemiological studies were predominantly cross-sectional and collectively, they highlight a global interest in this question and reveal evidence of differential susceptibility by sex and age to heavy metal exposures. In vivo studies in rats and mice and in vitro cell-based assays provide insights into potential mechanisms of action relevant to MS including altered regulation of lipid and glucose homeostasis, adipogenesis, and oxidative stress.
Summary
Heavy metal exposure may contribute to MS or comorbid conditions; however, available data are conflicting. Causal inference remains challenging as epidemiological data are largely cross-sectional; and variation in study design, including samples used for heavy metal measurements, age of subjects at which MS outcomes are measured; the scope and treatment of confounding factors; and the population demographics vary widely. Prospective studies, standardization or increased consistency across study designs and reporting, and consideration of molecular mechanisms informed by model system studies are needed to better assess potential causal links between heavy metal exposure and MS.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Kaur J. A comprehensive review on metabolic syndrome. Cardiol Res Pract. 2014;2014:943162.
Aguilar M, Bhuket T, Torres S, Liu B, Wong RJ. Prevalence of the metabolic syndrome in the United States, 2003-2012. JAMA. 2015;313(19):1973–4.
Ogden CL, Carroll MD, Fryar CD, Flegal KM. Prevalence of obesity among adults and youth: United States, 2011-2014. NCHS Data Brief. 2015;219:1–8.
De Long NE, Holloway AC. Early-life chemical exposures and risk of metabolic syndrome. Diabetes Metab Syndr Obes. 2017;10:101–9. https://doi.org/10.2147/DMSO.S95296.
Thayer KA, Heindel JJ, Bucher JR, Gallo MA. Role of environmental chemicals in diabetes and obesity: a National Toxicology Program workshop review. Environ Health Perspect. 2012;120(6):779–89. https://doi.org/10.1289/ehp.1104597.
Roy C, Tremblay PY, Ayotte P. Is mercury exposure causing diabetes, metabolic syndrome and insulin resistance? A systematic review of the literature. Environ Res. 2017;156:747–60. https://doi.org/10.1016/j.envres.2017.04.038.
Tinkov AA, Filippini T, Ajsuvakova OP, Aaseth J, Gluhcheva YG, Ivanova JM, et al. The role of cadmium in obesity and diabetes. Sci Total Environ. 2017;601–602:741–55.
Li Y, Zhang Y, Wang W, Wu Y. Association of urinary cadmium with risk of diabetes: a meta-analysis. Environ Sci Pollut Res Int. 2017;24(11):10083–90.
Kuo CC, Moon K, Thayer KA, Navas-Acien A. Environmental chemicals and type 2 diabetes: an updated systematic review of the epidemiologic evidence. Curr Diabetes Rep. 2013;13(6):831–49. https://doi.org/10.1007/s11892-013-0432-6.
Borne Y, Fagerberg B, Persson M, Sallsten G, Forsgard N, Hedblad B, et al. Cadmium exposure and incidence of diabetes mellitus—results from the Malmo diet and cancer study. PLoS One. 2014;9(11):e112277. https://doi.org/10.1371/journal.pone.0112277.
Menai M, Heude B, Slama R, Forhan A, Sahuquillo J, Charles MA, et al. Association between maternal blood cadmium during pregnancy and birth weight and the risk of fetal growth restriction: the EDEN mother-child cohort study. Reprod Toxicol. 2012;34(4):622–7. https://doi.org/10.1016/j.reprotox.2012.09.002.
• Swaddiwudhipong W, Limpatanachote P, Mahasakpan P, Krintratun S, Punta B, Funkhiew T. Progress in cadmium-related health effects in persons with high environmental exposure in northwestern Thailand: a five-year follow-up. Environ Res. 2012;112:194–8. Prospective study with significant associations between Cd exposure and T2D and HT.
Virtanen JK, Mursu J, Voutilainen S, Uusitupa M, Tuomainen TP. Serum omega-3 polyunsaturated fatty acids and risk of incident type 2 diabetes in men: the Kuopio ischemic heart disease risk factor study. Diabetes Care. 2014;37(1):189–96. https://doi.org/10.2337/dc13-1504.
Mozaffarian D, Shi P, Morris JS, Grandjean P, Siscovick DS, Spiegelman D, et al. Methylmercury exposure and incident diabetes in U.S. men and women in two prospective cohorts. Diabetes Care. 2013;36(11):3578–84. https://doi.org/10.2337/dc13-0894.
Drouillet-Pinard P, Huel G, Slama R, Forhan A, Sahuquillo J, Goua V, et al. Prenatal mercury contamination: relationship with maternal seafood consumption during pregnancy and fetal growth in the ‘EDEN mother-child’ cohort. Br J Nutr. 2010;104(8):1096–100. https://doi.org/10.1017/S0007114510001947.
He K, Xun P, Liu K, Morris S, Reis J, Guallar E. Mercury exposure in young adulthood and incidence of diabetes later in life: the CARDIA trace element study. Diabetes Care. 2013;36(6):1584–9. https://doi.org/10.2337/dc12-1842.
Singh PK, Baxi D, Diwedi R, Ramachandran AV. Prior cadmium exposure improves glucoregulation in diabetic rats but exacerbates effects on metabolic dysregulation, oxidative stress, and hepatic and renal toxicity. Drug Chem Toxicol. 2012;35(2):167–77.
Treviño S, Waalkes MP, Flores Hernández JA, León-Chavez BA, Aguilar-Alonso P, Brambila E. Chronic cadmium exposure in rats produces pancreatic impairment and insulin resistance in multiple peripheral tissues. Arch Biochem Biophys. 2015;583:27–35.
• Kawakami T, Nishiyama K, Kadota Y, Sato M, Inoue M, Suzuki S. Cadmium modulates adipocyte functions in metallothionein-null mice. Toxicol Appl Pharmacol. 2013;272(3):625–36. In vivo and in vitro study identifying Cd-mediated alterations in molecular markers of metabolism and adiposity.
Gong P, Chang X, Chen X, Bai X, Wen H, Pi S, et al. Metabolomics study of cadmium-induced diabetic nephropathy and protective effect of caffeic acid phenethyl ester using UPLC-Q-TOF-MS combined with pattern recognition. Environ Toxicol Pharmacol. 2017;54:80–92.
El Muayed M, Raja MR, Zhang X, MacRenaris KW, Bhatt S, Chen X, et al. Accumulation of cadmium in insulin-producing β cells. Islets. 2012;4(6):405–16.
Chang K-C, Hsu C-C, Liu S-H, Su C-C, Yen C-C, Lee M-J, et al. Cadmium induces apoptosis in pancreatic β-cells through a mitochondria-dependent pathway: the role of oxidative stress-mediated c-Jun N-terminal kinase activation. PLoS One. 2013;8(2):e54374.
Tyrrell JB, Hafida S, Stemmer P, Adhami A, Leff T. Lead (Pb) exposure promotes diabetes in obese rodents. J Trace Elem Med Biol. 2017;39:221–6.
Mostafalou S, Baeeri M, Bahadar H, Soltany-Rezaee-Rad M, Gholami M, Abdollahi M. Molecular mechanisms involved in lead induced disruption of hepatic and pancreatic glucose metabolism. Environ Toxicol Pharmacol. 2015;39(1):16–26. https://doi.org/10.1016/j.etap.2014.11.001.
Sun H, Wang N, Nie X, Zhao L, Li Q, Cang Z, et al. Lead exposure induces weight gain in adult rats, Accompanied by DNA Hypermethylation. PLoS One. 2017;12(1):e0169958. https://doi.org/10.1371/journal.pone.0169958.
Beier EE, Inzana JA, Sheu T-J, Shu L, Puzas JE, Mooney RA. Effects of combined exposure to lead and high-fat diet on bone quality in juvenile male mice. Environ Health Perspect. 2015;123(10):935–43.
Faulk C, Barks A, Sánchez BN, Zhang Z, Anderson OS, Peterson KE, et al. Perinatal lead (Pb) exposure results in sex-specific effects on food intake, fat, weight, and insulin response across the murine life-course. PLoS One. 2014;9(8):e104273.
Chen YW, Huang CF, Tsai KS, Yang RS, Yen CC, Yang CY, et al. The role of phosphoinositide 3-kinase/Akt signaling in low-dose mercury-induced mouse pancreatic beta-cell dysfunction in vitro and in vivo. Diabetes. 2006;55(6):1614–24.
Kawakami T, Hanao N, Nishiyama K, Kadota Y, Inoue M, Sato M, et al. Differential effects of cobalt and mercury on lipid metabolism in the white adipose tissue of high-fat diet-induced obesity mice. Toxicol Appl Pharmacol. 2012;258(1):32–42.
Thevenod F, Lee WK. Toxicology of cadmium and its damage to mammalian organs. Met Ions Life Sci. 2013;11:415–90. https://doi.org/10.1007/978-94-007-5179-8_14.
Jomova K, Valko M. Advances in metal-induced oxidative stress and human disease. Toxicology. 2011;283(2–3):65–87. https://doi.org/10.1016/j.tox.2011.03.001.
Gundacker C, Gencik M, Hengstschlager M. The relevance of the individual genetic background for the toxicokinetics of two significant neurodevelopmental toxicants: mercury and lead. Mutat Res. 2010;705(2):130–40.
Moon SS. Association of lead, mercury and cadmium with diabetes in the Korean population: the Korea National Health and Nutrition Examination Survey (KNHANES) 2009-2010. Diabet Med. 2013;30(4):e143–8. https://doi.org/10.1111/dme.12103.
Simic A, Hansen AF, Asvold BO, Romundstad PR, Midthjell K, Syversen T, et al. Trace element status in patients with type 2 diabetes in Norway: the HUNT3 survey. J Trace Elem Med Biol. 2017;41:91–8.
Feng W, Cui X, Liu B, Liu C, Xiao Y, Lu W, et al. Association of urinary metal profiles with altered glucose levels and diabetes risk: a population-based study in China. PLoS One. 2015;10(4):e0123742. https://doi.org/10.1371/journal.pone.0123742.
Menke A, Guallar E, Cowie CC. Metals in urine and diabetes in U.S. adults. Diabetes. 2016;65(1):164–71. https://doi.org/10.2337/db15-0316.
Ettinger AS, Bovet P, Plange-Rhule J, Forrester TE, Lambert EV, Lupoli N, et al. Distribution of metals exposure and associations with cardiometabolic risk factors in the “modeling the epidemiologic transition study”. Environ Health. 2014;13(1):90. https://doi.org/10.1186/1476-069X-13-90.
Yang A, Liu S, Cheng N, Pu H, Dai M, Ding J, et al. Multiple metals exposure, elevated blood glucose and dysglycemia among Chinese occupational workers. J Diabetes Complicat. 2017;31(1):101–7. https://doi.org/10.1016/j.jdiacomp.2016.07.022.
Park SB, Choi SW, Nam AY. Hair tissue mineral analysis and metabolic syndrome. Biol Trace Elem Res. 2009;130(3):218–28. https://doi.org/10.1007/s12011-009-8336-7.
Rhee SY, Hwang YC, Woo JT, Sinn DH, Chin SO, Chon S, et al. Blood lead is significantly associated with metabolic syndrome in Korean adults: an analysis based on the Korea National Health and Nutrition Examination Survey (KNHANES), 2008. Cardiovasc Diabetol. 2013;12(1):9. https://doi.org/10.1186/1475-2840-12-9.
Moon SS. Additive effect of heavy metals on metabolic syndrome in the Korean population: the Korea National Health and Nutrition Examination Survey (KNHANES) 2009-2010. Endocrine. 2014;46(2):263–71. https://doi.org/10.1007/s12020-013-0061-5.
Barregard L, Bergstrom G, Fagerberg B. Cadmium exposure in relation to insulin production, insulin sensitivity and type 2 diabetes: a cross-sectional and prospective study in women. Environ Res. 2013;121:104–9. https://doi.org/10.1016/j.envres.2012.11.005.
Kelishadi R, Askarieh A, Motlagh ME, Tajadini M, Heshmat R, Ardalan G, et al. Association of blood cadmium level with cardiometabolic risk factors and liver enzymes in a nationally representative sample of adolescents: the CASPIAN-III study. J Environ Public Health. 2013;2013:142856.
Padilla MA, Elobeid M, Ruden DM, Allison DB. An examination of the association of selected toxic metals with total and central obesity indices: NHANES 99-02. Int J Environ Res Public Health. 2010;7(9):3332–47. https://doi.org/10.3390/ijerph7093332.
Shao W, Liu Q, He X, Liu H, Gu A, Jiang Z. Association between level of urinary trace heavy metals and obesity among children aged 6-19 years: NHANES 1999-2011. Environ Sci Pollut Res Int. 2017;24(12):11573–81. https://doi.org/10.1007/s11356-017-8803-1.
Jornayvaz FR, Vollenweider P, Bochud M, Mooser V, Waeber G, Marques-Vidal P. Low birth weight leads to obesity, diabetes and increased leptin levels in adults: the CoLaus study. Cardiovasc Diabetol. 2016;15(1):73. https://doi.org/10.1186/s12933-016-0389-2.
Schellong K, Schulz S, Harder T, Plagemann A. Birth weight and long-term overweight risk: systematic review and a meta-analysis including 643,902 persons from 66 studies and 26 countries globally. PLoS One. 2012;7(10):e47776. https://doi.org/10.1371/journal.pone.0047776.
Rotter I, Kosik-Bogacka D, Dolegowska B, Safranow K, Lubkowska A, Laszczynska M. Relationship between the concentrations of heavy metals and bioelements in aging men with metabolic syndrome. Int J Environ Res Public Health. 2015;12(4):3944–61. https://doi.org/10.3390/ijerph120403944.
Swaddiwudhipong W, Mahasakpan P, Limpatanachote P, Krintratun S. Correlations of urinary cadmium with hypertension and diabetes in persons living in cadmium-contaminated villages in northwestern Thailand: a population study. Environ Res. 2010;110(6):612–6. https://doi.org/10.1016/j.envres.2010.06.002.
Everett CJ, Frithsen IL. Association of urinary cadmium and myocardial infarction. Environ Res. 2008;106(2):284–6. https://doi.org/10.1016/j.envres.2007.10.009.
Hecht EM, Arheart KL, Lee DJ, Hennekens CH, Hlaing WM. Interrelation of cadmium, smoking, and cardiovascular disease (from the National Health and Nutrition Examination Survey). Am J Cardiol. 2016;118(2):204–9. https://doi.org/10.1016/j.amjcard.2016.04.038.
Hansen AF, Simic A, Asvold BO, Romundstad PR, Midthjell K, Syversen T, et al. Trace elements in early phase type 2 diabetes mellitus—a population-based study. The HUNT study in Norway. J Trace Elem Med Biol. 2017;40:46–53.
Afridi HI, Kazi TG, Kazi N, Jamali MK, Arain MB, Jalbani N, et al. Evaluation of status of toxic metals in biological samples of diabetes mellitus patients. Diabetes Res Clin Pract. 2008;80(2):280–8. https://doi.org/10.1016/j.diabres.2007.12.021.
Liu B, Feng W, Wang J, Li Y, Han X, Hu H, et al. Association of urinary metals levels with type 2 diabetes risk in coke oven workers. Environ Pollut. 2016;210:1–8.
Son HS, Kim SG, Suh BS, Park DU, Kim DS, Yu SD, et al. Association of cadmium with diabetes in middle-aged residents of abandoned metal mines: the first health effect surveillance for residents in abandoned metal mines. Ann Occup Environ Med. 2015;27(1):20. https://doi.org/10.1186/s40557-015-0071-2.
Nie X, Wang N, Chen Y, Chen C, Han B, Zhu C, et al. Blood cadmium in Chinese adults and its relationships with diabetes and obesity. Environ Sci Pollut Res Int. 2016;23(18):18714–23. https://doi.org/10.1007/s11356-016-7078-2.
Lee BK, Kim Y. Association of blood cadmium level with metabolic syndrome after adjustment for confounding by serum ferritin and other factors: 2008-2012 Korean National Health and Nutrition Examination Survey. Biol Trace Elem Res. 2016;171(1):6–16. https://doi.org/10.1007/s12011-015-0499-9.
Lee BK, Kim Y. Blood cadmium, mercury, and lead and metabolic syndrome in South Korea: 2005-2010 Korean National Health and Nutrition Examination Survey. Am J Ind Med. 2013;56(6):682–92. https://doi.org/10.1002/ajim.22107.
Cummings BP, Digitale EK, Stanhope KL, Graham JL, Baskin DG, Reed BJ, et al. Development and characterization of a novel rat model of type 2 diabetes mellitus: the UC Davis type 2 diabetes mellitus UCD-T2DM rat. AJP: Regul Integr Comp Physiol. 2008;295(6):R1782–R93.
Zhang H, Yan C, Yang Z, Zhang W, Niu Y, Li X, et al. Alterations of serum trace elements in patients with type 2 diabetes. J Trace Elem Med Biol. 2017;40:91–6.
CDC. CDC’s childhood lead poisoning prevention program/what do parents need to know to protect their children? 2017 [cited 2017 November 2017]. Available from: https://www.cdc.gov/nceh/lead/acclpp/blood_lead_levels.htm.
Jeppesen C, Valera B, Nielsen NO, Bjerregaard P, Jorgensen ME. Association between whole blood mercury and glucose intolerance among adult Inuit in Greenland. Environ Res. 2015;143(Pt A):192–7.
Eom SY, Choi SH, Ahn SJ, Kim DK, Kim DW, Lim JA, et al. Reference levels of blood mercury and association with metabolic syndrome in Korean adults. Int Arch Occup Environ Health. 2014;87(5):501–13. https://doi.org/10.1007/s00420-013-0891-8.
Park K, Seo E. Association between toenail mercury and metabolic syndrome is modified by selenium. Nutrients. 2016;8(7) https://doi.org/10.3390/nu8070424.
Park JS, Ha KH, He K, Kim DJ. Association between blood mercury level and visceral adiposity in adults. Diabetes Metab J. 2017;41(2):113–20. https://doi.org/10.4093/dmj.2017.41.2.113.
Barnes DM, Hanlon PR, Kircher EA. Effects of inorganic HgCl2 on adipogenesis. Toxicol Sci. 2003;75(2):368–77.
Wang RY, Caldwell KL, Jones RL. Analytical considerations in the clinical laboratory assessment of metals. J Med Toxicol. 2014;10(2):232–9. https://doi.org/10.1007/s13181-014-0381-8.
Akerstrom M, Barregard L, Lundh T, Sallsten G. The relationship between cadmium in kidney and cadmium in urine and blood in an environmentally exposed population. Toxicol Appl Pharmacol. 2013;268(3):286–93. https://doi.org/10.1016/j.taap.2013.02.009.
Satarug S, Moore MR. Emerging roles of cadmium and heme oxygenase in type-2 diabetes and cancer susceptibility. Tohoku J Exp Med. 2012;228(4):267–88. https://doi.org/10.1620/tjem.228.267.
King KE, Darrah TH, Money E, Meentemeyer R, Maguire RL, Nye MD, et al. Geographic clustering of elevated blood heavy metal levels in pregnant women. BMC Public Health. 2015;15(1):1035. https://doi.org/10.1186/s12889-015-2379-9.
Acknowledgments
The authors would like to acknowledge the outstanding team at the Comparative Toxicogenomics Database for helpful discussions and for curating and providing access to additional information about the articles reviewed in this manuscript as well as the Center for Human Health and the Environment, which helped to facilitate collaborations such as this review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Mechanisms of Toxicity
Electronic supplementary material
Supplemental Table 1
(DOCX 97 kb)
Rights and permissions
About this article
Cite this article
Planchart, A., Green, A., Hoyo, C. et al. Heavy Metal Exposure and Metabolic Syndrome: Evidence from Human and Model System Studies. Curr Envir Health Rpt 5, 110–124 (2018). https://doi.org/10.1007/s40572-018-0182-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-018-0182-3