Abstract
Background
With the launch of the “Global Age-Friendly Cities project”, increasing emphasis has been placed on the effects of green spaces on health in the elderly. The previous literature has shown that green spaces are beneficial to a range of health-related outcomes in adults. However, associations of greenness with mortality and cardiovascular outcomes are less certain, which may differ depending on the age class. This review aimed to synthesize current evidence from observational studies to assess relationships of green space exposure with mortality and cardiovascular outcomes in older individuals.
Methods
Five databases were searched. Qualitative evaluation and meta-analyses of included studies were conducted. This review is registered with PROSPERO, CRD42020160366.
Results
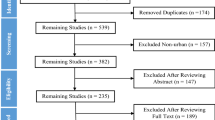
Of the 8,143 records identified, we finally included 22 studies. In a narrative systematic review, we observed that the majority of studies showed reductions in the risk of all-cause mortality and total cardiovascular disease. Further meta-analyses which included eight cohort studies, indicated that greater greenness exposure (per 0.1 unit increase of normalized difference vegetation index (NDVI)) was associated with a reduced risk of all-cause mortality (pooled hazard ratios (HR) (95% confidence interval (CI) = 0.99 (0.97, 1.00)) and stroke mortality (pooled HR (95% CI) = 0.77 (0.59, 1.00)) in older individuals.
Conclusions
This review supports increasing green space exposure in terms of the prevention of death and cardiovascular outcomes in older individuals. Effective measures to increase or preserve greenspaces should therefore be considered as important public health interventions.



Similar content being viewed by others
References
Marston HR, van Hoof J (2019) “Who doesn’t think about technology when designing urban environments for older people?” a case study approach to a proposed extension of the who’s age-friendly cities model. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph16193525
Jeste DV, Blazer DN, Buckwalter KC et al (2016) Age-friendly communities initiative: public health approach to promoting successful aging. Am J Geriatr Psychiatry 24:1158–1170. https://doi.org/10.1016/j.jagp.2016.07.021
Centres of Disease Control. Public Health Terms for Planners & Planning Terms for Public Health Professionals. http://www.cdc.gov/healthyplaces/terminology.htm
Colom A, Fiol M, Ruiz M et al (2018) Association between access to public open spaces and physical activity in a mediterranean population at high cardiovascular risk. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph15061285
Hawkesworth S, Silverwood RJ, Armstrong B et al (2018) Investigating associations between the built environment and physical activity among older people in 20 UK towns. J Epidemiol Community Health 72:121–131. https://doi.org/10.1136/jech-2017-209440
Triguero-Mas M, Donaire-Gonzalez D, Seto E et al (2017) Natural outdoor environments and mental health: stress as a possible mechanism. Environ Res 159:629–638. https://doi.org/10.1016/j.envres.2017.08.048
Dadvand P, Bartoll X, Basagana X et al (2016) Green spaces and general health: roles of mental health status, social support, and physical activity. Environ Int 91:161–167. https://doi.org/10.1016/j.envint.2016.02.029
van den Berg M, van Poppel M, van Kamp I et al (2016) Visiting green space is associated with mental health and vitality: a cross-sectional study in four european cities. Health Place 38:8–15. https://doi.org/10.1016/j.healthplace.2016.01.003
Paquet C, Coffee NT, Haren MT et al (2014) Food environment, walkability, and public open spaces are associated with incident development of cardio-metabolic risk factors in a biomedical cohort. Health Place 28:173–176. https://doi.org/10.1016/j.healthplace.2014.05.001
Michael YL, Nagel CL, Gold R, Hillier TA (2014) Does change in the neighborhood environment prevent obesity in older women? Soc Sci Med 102:129–137. https://doi.org/10.1016/j.socscimed.2013.11.047
Camargo DM, Ramirez PC, Fermino RC (2017) Individual and environmental correlates to quality of life in park users in Colombia. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph14101250
Pearce J, Shortt N, Rind E, Mitchell R (2016) Life course, green space and health: incorporating place into life course epidemiology. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph13030331
Cusack L, Larkin A, Carozza S, Hystad P (2017) Associations between residential greenness and birth outcomes across Texas. Environ Res 152:88–95. https://doi.org/10.1016/j.envres.2016.10.003
Fong KC, Hart JE, James P (2018) A Review of epidemiologic studies on greenness and health: updated literature through 2017. Curr Environ Health Rep 5:77–87. https://doi.org/10.1007/s40572-018-0179-y
Nieuwenhuijsen MJ, Khreis H, Triguero-Mas M, Gascon M, Dadvand P (2017) Fifty shades of green: pathway to healthy urban living. Epidemiology 28:63–71. https://doi.org/10.1097/EDE.0000000000000549
Gascon M, Triguero-Mas M, Martinez D et al (2016) Residential green spaces and mortality: a systematic review. Environ Int 86:60–67. https://doi.org/10.1016/j.envint.2015.10.013
Yitshak-Sade M, Kloog I, Novack V (2017) Do air pollution and neighborhood greenness exposures improve the predicted cardiovascular risk? Environ Int 107:147–153. https://doi.org/10.1016/j.envint.2017.07.011
James P, Hart JE, Banay RF, Laden F (2016) Exposure to greenness and mortality in a nationwide prospective cohort study of women. Environ Health Perspect 124:1344–1352. https://doi.org/10.1289/ehp.1510363
Klompmaker JO, Hoek G, Bloemsma LD et al (2020) Surrounding green, air pollution, traffic noise exposure and non-accidental and cause-specific mortality. Environ Int 134:105341. https://doi.org/10.1016/j.envint.2019.105341
Lanki T, Siponen T, Ojala A (2017) Acute effects of visits to urban green environments on cardiovascular physiology in women: a field experiment. Environ Res 159:176–185. https://doi.org/10.1016/j.envres.2017.07.039
Yang BY, Markevych I, Heinrich J et al (2019) Residential greenness and blood lipids in urban-dwelling adults: the 33 Communities Chinese Health Study. Environ Pollut 250:14–22. https://doi.org/10.1016/j.envpol.2019.03.128
Nieuwenhuijsen MJ, Gascon M, Martinez D et al (2018) Air pollution, noise, blue space, and green space and premature mortality in barcelona: a mega cohort. Int J Environ Res Public Health 15:2405. https://doi.org/10.3390/ijerph15112405
Vienneau D, de Hoogh K, Faeh D, Kaufmann M, Wunderli JM, Roosli M (2017) More than clean air and tranquillity: residential green is independently associated with decreasing mortality. Environ Int 108:176–184. https://doi.org/10.1016/j.envint.2017.08.012
Mitchell R, Popham F (2008) Effect of exposure to natural environment on health inequalities: an observational population study. Lancet 372:1655–1660. https://doi.org/10.1016/S0140-6736(08)61689-X
Orioli R, Antonucci C, Scortichini M et al (2019) Exposure to residential greenness as a predictor of cause-specific mortality and stroke incidence in the rome longitudinal study. Environ Health Perspect 127:27002. https://doi.org/10.1289/EHP2854
Villeneuve PJ, Jerrett M, Su JG et al (2012) A cohort study relating urban green space with mortality in Ontario, Canada. Environ Res 115:51–58. https://doi.org/10.1016/j.envres.2012.03.003
Crouse DL, Pinault L, Balram A et al (2017) Urban greenness and mortality in Canada’s largest cities: a national cohort study. The Lancet Planetary Health 1:e289–e297. https://doi.org/10.1016/S2542-5196(17)30118-3
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Plos Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605. https://doi.org/10.1007/s10654-010-9491-z
Atkins D, Fink K, Slutsky J (2005) Better information for better health care: the Evidence-based Practice Center program and the Agency for Healthcare Research and Quality. Ann Intern Med 142:1035–1041. https://doi.org/10.7326/0003-4819-142-12_part_2-200506211-00002
Lachowycz K, Jones AP (2011) Greenspace and obesity: a systematic review of the evidence. Obes Rev 12:e183–e189. https://doi.org/10.1111/j.1467-789X.2010.00827.x
Ji JS, Zhu A, Bai C et al (2019) Residential greenness and mortality in oldest-old women and men in China: a longitudinal cohort study. Lancet Planetary Health 3:e17–e25. https://doi.org/10.1016/S2542-5196(18)30264-X
Zijlema WL, Stasinska A, Blake D et al (2019) The longitudinal association between natural outdoor environments and mortality in 9218 older men from Perth, Western Australia. Environ Int 125:430–436. https://doi.org/10.1016/j.envint.2019.01.075
Paul LA, Hystad P, Burnett RT et al (2020) Urban green space and the risks of dementia and stroke. Environ Res 186:109520. https://doi.org/10.1016/j.envres.2020.109520
Xu Y, Zhu J, Gao L et al (2013) Hyperuricemia as an independent predictor of vascular complications and mortality in type 2 diabetes patients: a meta-analysis. PLoS ONE 8:e78206. https://doi.org/10.1371/journal.pone.0078206
Jiang Y, Ben Q, Shen H, Lu W, Zhang Y, Zhu J (2011) Diabetes mellitus and incidence and mortality of colorectal cancer: a systematic review and meta-analysis of cohort studies. Eur J Epidemiol 26:863–876. https://doi.org/10.1007/s10654-011-9617-y
Yang L, Wang G, Du Y, Ji B, Zheng Z (2014) Remote ischemic preconditioning reduces cardiac troponin I release in cardiac surgery: a meta-analysis. J Cardiothorac Vasc Anesth 28:682–689. https://doi.org/10.1053/j.jvca.2013.05.035
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13. https://doi.org/10.1186/1471-2288-5-13
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Takano T, Nakamura K, Watanabe M (2002) Urban residential environments and senior citizens’ longevity in megacity areas: the importance of walkable green spaces. J Epidemiol Commun H 56:913–918. https://doi.org/10.1136/jech.56.12.913
Sulander T, Karvinen E, Holopainen M (2016) Urban green space visits and mortality among older adults. Epidemiology 27:e34–e35. https://doi.org/10.1097/EDE.0000000000000511
Wang D, Lau KK, Yu R, Wong S, Kwok T, Woo J (2017) Neighbouring green space and mortality in community-dwelling elderly Hong Kong Chinese: a cohort study. BMJ Open 7:e015794. https://doi.org/10.1136/bmjopen-2016-015794
Massa KHC, Pabayo R, Lebrão ML, Filho ADPC (2016) Environmental factors and cardiovascular diseases: the association of income inequality and green spaces in elderly residents of São Paulo. BMJ Open 6:e011850. https://doi.org/10.1136/bmjopen-2016-011850
Jia X, Yu Y, Xia W et al (2018) Cardiovascular diseases in middle aged and older adults in China: the joint effects and mediation of different types of physical exercise and neighborhood greenness and walkability. Environ Res 167:175–183. https://doi.org/10.1016/j.envres.2018.07.003
Klompmaker JO, Janssen NAH, Bloenrsnur LD et al (2019) Associations of combined exposures to surrounding green, air pollution, and road traffic noise with cardiometabolic diseases. Environ Health Persp. https://doi.org/10.1289/EHP3857
Wang K, Lombard J, Rundek T et al (2019) Relationship of neighborhood greenness to heart disease in 249 405 US Medicare beneficiaries. J Am Heart Assoc 8:e010258. https://doi.org/10.1161/JAHA.118.010258
Aliyas Z (2019) Physical, mental, and physiological health benefits of green and blue outdoor spaces among elderly people. Int J Environ Health Res. https://doi.org/10.1080/09603123.2019.1681379
Seo S, Choi S, Kim K, Kim SM, Park SM (2019) Association between urban green space and the risk of cardiovascular disease: a longitudinal study in seven Korean metropolitan areas. Environ Int 125:51–57. https://doi.org/10.1016/j.envint.2019.01.038
Donovan GH, Michael YL, Gatziolis D, Prestemon JP, Whitsel EA (2015) Is tree loss associated with cardiovascular-disease risk in the Women’s Health Initiative? A natural experiment. Health Place 36:1–7. https://doi.org/10.1016/j.healthplace.2015.08.007
Tamosiunas A, Grazuleviciene R, Luksiene D et al (2014) Accessibility and use of urban green spaces, and cardiovascular health: findings from a Kaunas cohort study. Environ Health 13:20. https://doi.org/10.1186/1476-069X-13-20
Dalton AM, Jones AP (2020) Residential neighbourhood greenspace is associated with reduced risk of cardiovascular disease: a prospective cohort study. PLoS ONE 15:e226524. https://doi.org/10.1371/journal.pone.0226524
Astell-Burt T, Feng X (2019) Urban green space, tree canopy and prevention of cardiometabolic diseases: a multilevel longitudinal study of 46 786 Australians. Int J Epidemiol 49:926–933. https://doi.org/10.1093/ije/dyz239
Rojas-Rueda D, Nieuwenhuijsen MJ, Gascon M, Perez-Leon D, Mudu P (2019) Green spaces and mortality: a systematic review and meta-analysis of cohort studies. Lancet Planet Health 3:e469–e477. https://doi.org/10.1016/S2542-5196(19)30215-3
Twohig-Bennett C, Jones A (2018) The health benefits of the great outdoors: a systematic review and meta-analysis of greenspace exposure and health outcomes. Environ Res 166:628–637. https://doi.org/10.1016/j.envres.2018.06.030
Chandrabose M, Rachele JN, Gunn L et al (2019) Built environment and cardio-metabolic health: systematic review and meta-analysis of longitudinal studies. Obes Rev 20:41–54. https://doi.org/10.1111/obr.12759
Markevych I, Schoierer J, Hartig T et al (2017) Exploring pathways linking greenspace to health: theoretical and methodological guidance. Environ Res 158:301–317. https://doi.org/10.1016/j.envres.2017.06.028
James P, Banay RF, Hart JE, Laden F (2015) A review of the health benefits of greenness. Curr Epidemiol Rep 2:131–142. https://doi.org/10.1007/s40471-015-0043-7
Rhew IC, Vander SA, Kearney A, Smith NL, Dunbar MD (2011) Validation of the normalized difference vegetation index as a measure of neighborhood greenness. Ann Epidemiol 21:946–952. https://doi.org/10.1016/j.annepidem.2011.09.001
Funding
This review was supported by the Fujian Major Projects on Science and Technology for Social Development (2016YZ0001) and Fujian Science and Technology Innovation Joint Major Project (2019Y9027).
Author information
Authors and Affiliations
Contributions
All authors contributed to the initial planning of the review. YY, HF and LF developed the search strategy. YY and HF screened articles and extracted data, which was then cross-checked by LF and ZPL. ZPY mediated the discrepancies in article screening. YY and HF assessed study quality and performed meta-analyses. YY drafted the manuscript. All authors contributed to reviewing and revising the manuscript, read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
All reported studies with human subjects performed by the authors have been previously published and complied with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Statement of human and animal rights
This review does not contain any experiments involving human participants or animals.
Informed consent
We confirm that the present study is based on the analysis of other studies which had obtained informed consent for all included individuals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yuan, Y., Huang, F., Lin, F. et al. Green space exposure on mortality and cardiovascular outcomes in older adults: a systematic review and meta-analysis of observational studies. Aging Clin Exp Res 33, 1783–1797 (2021). https://doi.org/10.1007/s40520-020-01710-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-020-01710-0