Abstract
Aim
Swallowing is a vital activity. The difficulty while swallowing, referred to as swallowing disorder, is strongly associated with serious health problems in the elderly. The aim of this study is to enable early recognition of the swallowing function developing as an asymptomatic condition.
Method
Our study was conducted on elderly populations aged 65 years and over who met the exclusion criteria. Firstly, to be able to reach the number of sampling, “EAT-10 questionnaire”, which also has a Turkish validation, was used to eliminate those with symptomatic swallowing disorders. The number of patients we reached was 320, but 7 dropped out of the study and therefore the study was carried out with a total of 313 [reached as 97.8% (up 95% G-power)].
Result
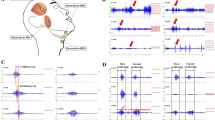
We used validated sEMG test in the quantitative (objective) detection of asymptomatic swallowing disorder. In this method, asymptomatic swallowing disorder was detected in 39 cases (12.4%).
Conclusion
Swallowing disorder without symptoms is frequent and the sEMG test is useful in detecting it in the elderly population.





Similar content being viewed by others
References
Fucile S, Wright PM, Chan I et al (1998) Functional oral-motor skills: do they change withage? Dysphagia 13:195–201
Di Carlo A, Lamassa M, Pracucci G et al (1999) Stroke in the very old: clinical presentation and determinants of 3-month functional outcome: a European perspective. Stroke 30:2313–2319
Leder SB, Suiter DM (2009) An epidemiologic study on aging and dysphagia in the acute care hospitalized population: 2000–2007. Gerontology 55:714–718
Crary MA, Groher ME (2003) Introduction to adult swallowing disorders. Butterworth-Heinemann an imprint of Elsevier Sciense, Missouri
Shioda S, Takenoya F, Yagi M et al (2007) Neurophysiology of swallowing. Physiol Behav 92:2226–2244
Jean A (2001) Brain stem control of swallowing: neuronal network and cellular mechanisms. Physiol Rev 81:929–969
Trate DM, Parkman HP, Fisher RS (1996) Dysphagia. Evaluation, diagnosis, and treatment. Prim Care 23:417–432
Robbins J, Hamilton JW, Lof GL, Kempster GB (1992) Oropharyngeal swallowing in normal adults of different ages. Gastroenterology 103:823–829
McCullough GH, Rosenbek JC, Wertz RT et al (2007) Defining swallowing function by age: promises and pitfalls of pigeonholing. Top Geriatr Rehabil 23:290–307
McCoy YM, Varindani Desai R (2018) Presbyphagia versus dysphagia: identifying age-related changes in swallow function. Perspect ASHA Spec Interest Gr. https://doi.org/10.1044/persp3.SIG15.15
Tracy JF, Logemann JA, Kahrilas PJ et al (1999) Preliminary observations on the effects of age on oropharyngeal deglutition. Dysphagia 4:90–94
Miller AJ (1972) Significance of sensory inflow to the swallowing reflex. Brain Res 43:147–159
Månsson I, Sandberg N (1975) Oro-pharyngeal sensitivity and elicitation of swallowing in man. Acta Otolaryngol 79:140–145
Clavé P, Terré R, de Kraa M, Serra M (2004) Approaching oropharyngeal dysphagia. Rev Esp Enferm Dig 96:119–131
Loeb MB, Becker M, Eady A et al (2003) Interventions to prevent aspiration pneumonia in older adults: a systematic review. J Am Geriatr Soc 51:1018–1022
Sura L, Madhavan A, Carnaby G et al (2012) Dysphagia in the elderly: management and nutritional considerations. Clin Interv Aging 7:287–298
Ortega O, Martín A, Clavé P (2017) Diagnosis and management of oropharyngeal dysphagia among older persons, state of the art. J Am Med Dir Assoc 18:576–582
Lindgren S, Janzon L (1991) Prevalence of swallowing complaints and clinical findings among 50–79-year-old men and women in an urban population. Dysphagia 6:187–192
Barczi SR, Sullivan PA, Robbins J (2000) How should dysphagia care of older adults differ? Establishing optimal practice patterns. Semin Speech Lang 21:347–361
Nicosia MA, Hind JA, Roecker EB et al (2000) Age effects on the temporal evolution of isometric and swallowing pressure. J Gerontol A Biol Sci Med Sci 55:634–640
Rao Poduri K (2017) Geriatric rehabilitation: from bedside to curbside. Taylor and Francis Group, London, p 535
Ekberg O, Hamdy S, Woisard V et al (2002) Social and psychological burden of dysphagia: its impact on diagnosis and treatment. Dysphagia 17:139–146
Logemann JA, Veis S, Colangelo L (1999) A screening procedure for oropharyngeal dysphagia. Dysphagia 14:44–51
Daniels SK, Anderson JA, Willson PC (2012) Valid items for screening dysphagia risk in patients with stroke: a systematic review. Stroke 43:892–897
Belafsky PC, Mouadeb DA, Rees CJ et al (2008) Validity and reliability of the Eating Assessment Tool (EAT-10). Ann Otol Rhinol Laryngol 117:919–924
Ertekin C, Aydogdu I, Yüceyar N et al (1998) Electrodiagnostic methods for neurogenic dysphagia. Electroencephalogr Clin Neurophysiol 109:331–340
Ertekin C, Aydoğdu I, Yüceyar N et al (1997) Effects of bolus volume on oropharyngeal swallowing: an electrophysiologic study in man. Am J Gastroenterol 92:2049–2053
Ertekin C, Aydoğdu I, Yüceyar N (1996) Piecemeal deglutition and dysphagia limit in normal subjects and in patients with swallowing disorders. J Neurol Neurosurg Psychiatry 61:491–496
Aydogdu I, Kiylioglu N, Tarlaci S et al (2015) Diagnostic value of “dysphagia limit” for neurogenic dysphagia: 17 years of experience in 1278 adults. Clin Neurophysiol 126:634–643
Ertekin C, Aydogdu I, Yüceyar N et al (1998) Electrodiagnostic methods for neurogenic dysphagia. Electroencephalogr Clin Neurophysiol Electromyogr Mot Control 109:331–340
Suiter DM, Leder SB (2008) Clinical utility of the 3-ounce water swallow test. Dysphagia 23:244–250
Ertekin C, Aydogdu I, Yüceyar N et al (1995) An electrophysiological investigation of deglutition in man. Muscle Nerve 18:1177–1186
Linden P, Kuhlemeier KV, Patterson C (1993) The probability of correctly predicting subglottic penetration from clinical observations. Dysphagia 8:170–179
Hughes TA, Wiles CM (1996) Clinical measurement of swallowing in health and in neurogenic dysphagia. QJM 89:109–116
Nathadwarawala KM, Nicklin J, Wiles CM (1992) A timed test of swallowing capacity for neurological patients. J Neurol Neurosurg Psychiatry 55:822–825
Palmer PM, McCulloch TM, Jaffe D et al (2005) Effects of a sour bolus on the intramuscular electromyographic (EMG) activity of muscles in the submental region. Dysphagia 20:210–217
McKeown MJ, Torpey DC, Gehm WC (2002) Non-invasive monitoring of functionally distinct muscle activations during swallowing. Clin Neurophysiol 113:354–366
Gürgör N, Arici Ş, Kurt Incesu T et al (2013) An electrophysiological study of the sequential water swallowing. J Electromyogr Kinesiol 23:619–626
Ertekin C, Palmer JB (2000) Physiology and electromyography of swallowing and its disorders. Suppl Clin Neurophysiol 53:148–154
Okamoto N, Tomioka K, Saeki K et al (2012) Relationship between swallowing problems and tooth loss in community-dwelling independent elderly adults: the Fujiwara-Kyo study. J Am Geriatr Soc 60:849–853
Inui A, Takahashi I, Kurauchi S et al (2017) Oral conditions and dysphagia in Japanese, community-dwelling middle- and older-aged adults, independent in daily living. Clin Interv Aging 12:515–521
Ertekin C, Aydogdu I, Yüceyar N et al (2000) Pathophysiological mechanisms of oropharyngeal dysphagia in amyotrophic lateral sclerosis. Brain 123:125–140
Ertekin C, Aydoğdu I, Yüceyar N et al (1997) Effects of bolus volume on oropharyngeal swallowing: an electrophysiologic study in man. Am J Gastroenterol 92:2049–2053
Groher ME, Crary MA (2010) Dysphagia : clinical management in adults and children, 2nd edn. Mosby Elsevier, Missouri, p 386
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the study were in accordance with the ethical standards of our Institution (Health Sciences University, Bozyaka Education and Research Hospital Ethical Commity Ref Number: 01 Date 06.12.2016 and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individuals participating the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yüksel, A., Kulan, C.A. & Akçiçek, F. The investigation of asymptomatic swallowing disorder through surface electromyography in the geriatric population. Aging Clin Exp Res 32, 1567–1576 (2020). https://doi.org/10.1007/s40520-019-01349-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-019-01349-6