Abstract
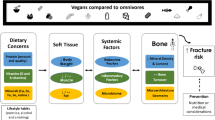
Uncountable health care organizations, clinicians, and individuals are striving to prevent obesity and the many chronic medical conditions linked to it by advocating a healthy lifestyle that includes measures such as reducing dietary calorie intake (i.e., calorie restriction = CR and intermittent fasting = IF) or limiting/abolishing animal source foods (i.e., practices termed vegetarianism and veganism). Although these regimens are traditionally considered healthy, their real impact on bone health has yet to be established, and some studies have reported that they have negative effects on bone outcomes. The current work provides an overview of the studies carried out to examine the effect/s of CR, IF and vegetarian/vegan diets on bone health, and, in particular, on bone mineral density (BMD) and fracture risk. Although data on this subject are limited to small studies and there is no information specifically referring to fractures, CR, but not IF, seems to reduce BMD but does not seem to affect bone quality. Vegetarian diets (particularly vegan ones) are associated with significantly lower BMD values with respect to omnivorous ones and could, potentially, increase the risk of fractures. Given these considerations, individuals who decide to follow these diets should be aware of the risk of osteoporosis and of bone fractures and should introduce dietary sources of calcium and Vitamin D and/or supplementation. Future studies examining fracture/osteoporosis incidence in selected populations will be able expand our knowledge about the safety of these diets and the risks linked to them.
Similar content being viewed by others
References
Waxman A, World HA (2004) WHO global strategy on diet, physical activity and health. Food Nutr Bull 25:292
Liao Q, Zheng Z, Xiu S et al (2018) Waist circumference is a better predictor of risk for frailty than BMI in the community-dwelling elderly in Beijing. Aging Clin Exp Res 30(11):1319–1325
Barnes AS (2012) Obesity and sedentary lifestyles: risk for cardiovascular disease in women. Tex Heart Inst J 39:224–227
Forouhi NG, Wareham NJ (2014) Epidemiology of diabetes. Medicine 42:698–702
Kyrgiou M, Kalliala I, Markozannes G et al (2017) Adiposity and cancer at major anatomical sites: umbrella review of the literature. BMJ 356:j477
Fontana L, Partridge L, Longo VD (2010) Extending healthy life span—from yeast to humans. Science 328:321–326
Fontana L, Mitchell SE, Wang B et al (2018) The effects of graded caloric restriction: XII. Comparison of mouse to human impact on cellular senescence in the colon. Aging Cell 17:e12746
Mattison JA, Colman RJ, Beasley TM et al (2017) Caloric restriction improves health and survival of rhesus monkeys. Nat Commun 8:14063
Shanley DP, Kirkwood TB (2000) Calorie restriction and aging: a life-history analysis. Evolution 54:740–750
Most J, Tosti V, Redman LM et al (2017) Calorie restriction in humans: an update. Ageing Res Rev 39:36–45
Veronese N, Facchini S, Stubbs B et al (2017) Weight loss is associated with improvements in cognitive function among overweight and obese people: a systematic review and meta-analysis. Neurosci Biobehav Rev 72:87–94
Colman RJ, Anderson RM, Johnson SC et al (2009) Caloric restriction delays disease onset and mortality in rhesus monkeys. Science 325:201–204
Yang L, Licastro D, Cava E et al (2016) Long-term calorie restriction enhances cellular quality-control processes in human skeletal muscle. Cell Rep 14:422–428
Rizza W, Veronese N, Fontana L (2014) What are the roles of calorie restriction and diet quality in promoting healthy longevity? Ageing Res Rev 13:38–45
Fontana L, Meyer TE, Klein S et al (2004) Long-term calorie restriction is highly effective in reducing the risk for atherosclerosis in humans. Proc Natl Acad Sci 101:6659–6663
Barbour KE, Lui LY, Ensrud KE et al (2014) Inflammatory markers and risk of hip fracture in older white women: the study of osteoporotic fractures. J Bone Miner Res 29:2057–2064
Ding C, Parameswaran V, Udayan R et al (2008) Circulating levels of inflammatory markers predict change in bone mineral density and resorption in older adults: a longitudinal study. J Clin Endocrinol Metab 93:1952–1958
Veronese N, Shivappa N, Hebert J et al (2018) Pro-inflammatory dietary pattern is associated with fractures in women: an eight year longitudinal cohort study. Osteoporos Int 29:S71–S72
Dennison E, Syddall H, Sayer AA et al (2004) Type 2 diabetes mellitus is associated with increased axial bone density in men and women from the Hertfordshire Cohort Study: evidence for an indirect effect of insulin resistance? Diabetologia 47:1963–1968
Veronese N, Stubbs B, Crepaldi G et al (2017) Relationship between low bone mineral density and fractures with incident cardiovascular disease: a systematic review and meta-analysis. J Bone Miner Res 32(5):1126–1135
Huang T, Ables GP (2016) Dietary restrictions, bone density, and bone quality. Ann N Y Acad Sci 1363:26–39
Soltani S, Hunter G, Kazemi A et al (2016) The effects of weight loss approaches on bone mineral density in adults: a systematic review and meta-analysis of randomized controlled trials. Osteoporos Int 27:2655–2671
Ensrud K, Vo T, Burghardt A et al (2018) Weight loss in men in late life and bone strength and microarchitecture: a prospective study. Osteoporosis Int 29(7):1549–1558
Villareal DT, Fontana L, Weiss EP et al (2006) Bone mineral density response to caloric restriction-induced weight loss or exercise-induced weight loss: a randomized controlled trial. Arch Intern Med 166:2502–2510
Villareal DT, Fontana L, Das SK et al (2016) Effect of two-year caloric restriction on bone metabolism and bone mineral density in non-obese younger adults: a randomized clinical trial. J Bone Miner Res 31:40–51
Villareal DT, Kotyk JJ, Armamento-Villareal RC et al (2011) Reduced bone mineral density is not associated with significantly reduced bone quality in men and women practicing long-term calorie restriction with adequate nutrition. Aging Cell 10:96–102
Schoell S, Weaver A, Beavers D et al (2018) Development of subject-specific proximal femur finite element models of older adults with obesity to evaluate the effects of weight loss on bone strength. J Osteoporosis Phys Act. https://doi.org/10.4172/2329-9509.1000213
Davis CS, Clarke RE, Coulter SN et al (2016) Intermittent energy restriction and weight loss: a systematic review. Eur J Clin Nutr 70:292–299
Patterson RE, Sears DD (2017) Metabolic effects of intermittent fasting. Annu Rev Nutr 37:371–393
Bahijri SM, Ajabnoor GM, Borai A et al (2015) Effect of Ramadan fasting in Saudi Arabia on serum bone profile and immunoglobulins. Ther Adv Endocrinol Metab 6:223–232
Barnosky A, Kroeger CM, Trepanowski JF et al (2017) Effect of alternate day fasting on markers of bone metabolism: an exploratory analysis of a 6-month randomized controlled trial. Nutr Healthy Aging 4:255–263
Pilis W, Stec K, Zych M et al (2014) Health benefits and risk associated with adopting a vegetarian diet. Rocz Panstw Zakl Hig 65(1):9–14
Sabaté J, Wien M (2010) Vegetarian diets and childhood obesity prevention. Am J Clin Nutr 91:1525S–1529S
Rizzo NS, Sabaté J, Jaceldo-Siegl K et al (2011) Vegetarian dietary patterns are associated with a lower risk of metabolic syndrome: the adventist health study 2. Diabetes Care 34:1225–1227
Snowdon DA, Phillips RL (1985) Does a vegetarian diet reduce the occurrence of diabetes? Am J Public Health 75:507–512
Kwok CS, Umar S, Myint PK et al (2014) Vegetarian diet, seventh day adventists and risk of cardiovascular mortality: a systematic review and meta-analysis. Int J Cardiol 176:680–686
Fraser GE (1999) Associations between diet and cancer, ischemic heart disease, and all-cause mortality in non-Hispanic white California seventh-day adventists. Am J Clin Nutr 70:532 s–538 s
Craig WJ (2009) Health effects of vegan diets. Am J Clin Nutr 89:1627S–1633S
Veronese N, Solmi M, Caruso MG et al (2018) Dietary fiber and health outcomes: an umbrella review of systematic reviews and meta-analyses. Am J Clin Nutr 107:436–444
Abid Z, Cross AJ, Sinha R (2014) Meat, dairy, and cancer. Am J Clin Nutr 100:386S–393S
Institute of Medicine (US) Standing Committee on the Scientific Evaluation of Dietary Reference Intakes (1997) Dietary reference intakes for calcium, phosphorus, magnesium, vitamin D, and fluoride. National Academies Press (US), Washington (DC)
Tucker KL (2014) Vegetarian diets and bone status. Am J Clin Nutr 100:329S–335S
Ho-Pham LT, Nguyen ND, Nguyen TV (2009) Effect of vegetarian diets on bone mineral density: a Bayesian meta-analysis. Am J Clin Nutr 90:943–950
Iguacel I, Miguel-Berges ML, Gómez-Bruton A et al (2018) Veganism, vegetarianism, bone mineral density, and fracture risk: a systematic review and meta-analysis. Nutr Rev 77:1–18
Shams-White MM, Chung M, Du M et al (2017) Dietary protein and bone health: a systematic review and meta-analysis from the National Osteoporosis Foundation, 2. Am J Clin Nutr 105:1528–1543
Weaver CM, Proulx WR, Heaney R (1999) Choices for achieving adequate dietary calcium with a vegetarian diet. Am J Clin Nutr 70:543 s–548 s
Tai V, Leung W, Grey A et al (2015) Calcium intake and bone mineral density: systematic review and meta-analysis. BMJ 351:h4183
Roman-Garcia P, Quiros-Gonzalez I, Mottram L et al (2014) Vitamin B 12-dependent taurine synthesis regulates growth and bone mass. J Clin Investig 124:2988–3002
Burckhardt P (2016) The role of low acid load in vegetarian diet on bone health: a narrative review. Swiss Med Wkly 146:w14277
Kanis J, Johnell O, Odén A et al (2008) FRAX™ and the assessment of fracture probability in men and women from the UK. Osteoporos Int 19:385–397
Theodoratou E, Tzoulaki I, Zgaga L et al (2014) Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials. BMJ 348:g2035. https://doi.org/10.1136/bmj.g2035
Blain H, Masud T, Dargent-Molina P et al (2016) A comprehensive fracture prevention strategy in older adults: the European Union Geriatric Medicine Society (EUGMS) statement. J Nutr Health Aging 20:647–652
Orces CH (2018) Association between leisure-time aerobic physical activity and vitamin D concentrations among US older adults: the NHANES 2007–2012. Aging Clin Exp Res. https://doi.org/10.1007/s40520-018-1031-9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human and animal rights
No human being or animal was involved in this study.
Informed consent
Being a review of previously published material, no informed consent was asked.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Veronese, N., Reginster, JY. The effects of calorie restriction, intermittent fasting and vegetarian diets on bone health. Aging Clin Exp Res 31, 753–758 (2019). https://doi.org/10.1007/s40520-019-01174-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-019-01174-x