Abstract
Background
Sarcopenic elderly present low muscle mass and strength, however, it is not clear if the inflammatory and metabolic profile is more related to low lean mass or high fat mass in sarcopenic and non-sarcopenic overfat elderly.
Aim
To verify the difference in inflammatory and metabolic responses in sarcopenic and non-sarcopenic overfat elderly and the relationship between these markers, body composition, and strength in this population.
Methods
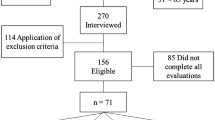
Fifty-seven elderly were divided into two groups: sarcopenic (n = 30) and non-sarcopenic (n = 27). Body composition was evaluated with octopolar bioimpedance. Total cholesterol, high-density lipoprotein cholesterol, triacylglycerol, glucose, cortisol, leptin, adiponectin, Plasminogen activator inhibitor-1 (PAI-1), TNF-α, IL-6, IL-8, and IL-10 were assessed. The handgrip test was used to evaluate strength.
Results
When comparing the inflammatory profile, sarcopenic individuals showed greater adiponectin concentration (p = 0.019), adiponectin/fat mass ratio (p < 0.001), adiponectin/visceral fat (p < 0.001), and higher PAI-1 (p = 0.019) than non-sarcopenic overfat elderly. After adjusting the inflammatory profile by skeletal muscle mass the significant differences between groups were maintained (p < 0.05) but no significant differences between groups were observed when adjusting by fat mass, despite a tendency to a significant difference for adiponectin concentration (p = 0.06). In addition, after adjusting leptin by fat mass there was a statistically significant lower concentration in the sarcopenic compared to non-sarcopenic overfat elderly.
Conclusion
Non-sarcopenic overfat elderly presented lower anti-inflammatory and anti-atherogenic responses than sarcopenic elderly. Furthermore, fat mass but not skeletal muscle mass seem to change these responses.

Similar content being viewed by others
References
Bonnefoy M, Gilbert T (2015) Body composition and comorbidity in the elderly. Geriatrie et psychologie neuropsychiatrie du vieillissement 13:29–36. https://doi.org/10.1684/pnv.2015.0528
Landi F, Calvani R, Cesari M et al (2015) Sarcopenia as the biological substrate of physical frailty. Clin Geriatr Med 31:367–374. https://doi.org/10.1016/j.cger.2015.04.005
Ali NA, O’Brien JM Jr, Hoffmann SP et al (2008) Acquired weakness, handgrip strength, and mortality in critically ill patients. Am J Respir Crit Care Med 178:261–268. https://doi.org/10.1164/rccm.200712-1829OC
Pedersen BK, Febbraio M (2005) Muscle-derived interleukin-6–a possible link between skeletal muscle, adipose tissue, liver, and brain. Brain Behav Immun 19:371–376. https://doi.org/10.1016/j.bbi.2005.04.008
Brandt C, Pedersen BK (2010) The role of exercise-induced myokines in muscle homeostasis and the defense against chronic diseases. J Biomed Biotechnol 2010:520258. https://doi.org/10.1155/2010/520258
Serrano AL, Baeza-Raja B, Perdiguero E et al (2008) Interleukin-6 is an essential regulator of satellite cell-mediated skeletal muscle hypertrophy. Cell Metab 7:33–44. https://doi.org/10.1016/j.cmet.2007.11.011
Visser M, Pahor M, Taaffe DR et al (2002) Relationship of interleukin-6 and tumor necrosis factor-alpha with muscle mass and muscle strength in elderly men and women: the Health ABC Study. J Gerontol Ser A Biol Sci Med Sci 57:M326-332
Aleman H, Esparza J, Ramirez FA et al (2011) Longitudinal evidence on the association between interleukin-6 and C-reactive protein with the loss of total appendicular skeletal muscle in free-living older men and women. Age Ageing 40:469–475. https://doi.org/10.1093/ageing/afr040
Schaap LA, Pluijm SM, Deeg DJ et al (2006) Inflammatory markers and loss of muscle mass (sarcopenia) and strength. Am J Med 119:526.e529–526.e517. https://doi.org/10.1016/j.amjmed.2005.10.049
Bouchard DR, Dionne IJ, Brochu M (2009) Sarcopenic/obesity and physical capacity in older men and women: data from the Nutrition as a Determinant of Successful Aging (NuAge)-the Quebec longitudinal Study. Obesity (Silver Spring Md) 17:2082–2088. https://doi.org/10.1038/oby.2009.109
Yang CW, Li CI, Li TC et al (2015) Correction: association of sarcopenic obesity with higher serum high-sensitivity C-reactive protein levels in Chinese older males-a community-based study (Taichung Community Health Study-Elderly, TCHS-E). PLoS One 10:e0136069. https://doi.org/10.1371/journal.pone.0136069
Zoico E, Corzato F, Bambace C et al (2013) Myosteatosis and myofibrosis: relationship with aging, inflammation and insulin resistance. Arch Gerontol Geriatr 57:411–416. https://doi.org/10.1016/j.archger.2013.06.001
Scuteri A, Orru M, Morrell C et al (2011) Independent and additive effects of cytokine patterns and the metabolic syndrome on arterial aging in the SardiNIA Study. Atherosclerosis 215:459–464. https://doi.org/10.1016/j.atherosclerosis.2010.12.023
Scuteri A, Orru M, Morrell CH et al (2012) Associations of large artery structure and function with adiposity: effects of age, gender, and hypertension. The SardiNIA Study. Atherosclerosis 221:189–197. https://doi.org/10.1016/j.atherosclerosis.2011.11.045
Kelly TL, Wilson KE, Heymsfield SB (2009) Dual energy X-Ray absorptiometry body composition reference values from NHANES. PloS One 4:e7038. https://doi.org/10.1371/journal.pone.0007038
Lohman TG, Houtkooper L, Going SB (1997) Body fat measurement goes hightech: not all are created equal. ACSM’S Health Fit J 1:30–35
Zhu M, Miura J, Lu LX et al (2004) Circulating adiponectin levels increase in rats on caloric restriction: the potential for insulin sensitization. Exp Gerontol 39:1049–1059. https://doi.org/10.1016/j.exger.2004.03.024
Vidal J (2002) Updated review on the benefits of weight loss. Int J Obes Relat Metab Disord J Int Assoc Study Obes 26:S25–S28. https://doi.org/10.1038/sj.ijo.0802215
Hotta K, Funahashi T, Arita Y et al (2000) Plasma concentrations of a novel, adipose-specific protein, adiponectin, in type 2 diabetic patients. Arterioscler Thromb Vasc Biol 20:1595–1599
Fatouros IG, Tournis S, Leontsini D et al (2005) Leptin and adiponectin responses in overweight inactive elderly following resistance training and detraining are intensity related. J Clin Endocrinol Metab 90:5970–5977. https://doi.org/10.1210/jc.2005-0261
Hsieh CJ, Wang PW (2005) Effectiveness of weight loss in the elderly with type 2 diabetes mellitus. J Endocrinol Investig 28:973–977
Lalic K, Jotic A, Rajkovic N, Singh S et al (2015) Altered daytime fluctuation pattern of plasminogen activator inhibitor 1 in type 2 diabetes patients with coronary artery disease: a strong association with persistently elevated plasma insulin, increased insulin resistance, and abdominal obesity. Int J Endocrinol 2015:390185. https://doi.org/10.1155/2015/390185
Liang X, Kanjanabuch T, Mao SL et al (2006) Plasminogen activator inhibitor-1 modulates adipocyte differentiation. Am J Physiol Endocrinol Metab 290:E103–E113. https://doi.org/10.1152/ajpendo.00605.2004
Chou YY, Sheu WH, Tang YJ et al (2009) Plasminogen activator inhibitor type 1 (PAI-1) is a valuable biomarker for predicting the metabolic syndrome (MS) in institutionalized elderly residents in Taiwan. Arch Gerontol Geriatr 49:S41–S45. https://doi.org/10.1016/s0167-4943(09)70012-3
Peverill RE, Teede HJ, Malan E et al (2007) Relationship of waist and hip circumference with coagulation and fibrinolysis in postmenopausal women. Clin Sci (Lond, Engl 1979) 113:383–391. https://doi.org/10.1042/cs20070084
Kim HK, Park HR, Lee JS et al (2007) Down-regulation of iNOS and TNF-alpha expression by kaempferol via NF-kappaB inactivation in aged rat gingival tissues. Biogerontology 8:399–408. https://doi.org/10.1007/s10522-007-9083-9
Li YP, Reid MB (2000) NF-kappaB mediates the protein loss induced by TNF-alpha in differentiated skeletal muscle myotubes. Am J Physiol Regul Integr Comp Physiol 279:R1165–R1170
Li YP, Chen Y, John J et al (2005) TNF-alpha acts via p38 MAPK to stimulate expression of the ubiquitin ligase atrogin1/MAFbx in skeletal muscle. FASEB J 19:362–370. https://doi.org/10.1096/fj.04-2364com
Clavel S, Coldefy AS, Kurkdjian E et al (2006) Atrophy-related ubiquitin ligases, atrogin-1 and MuRF1 are up-regulated in aged rat Tibialis Anterior muscle. Mech Ageing Dev 127:794–801. https://doi.org/10.1016/j.mad.2006.07.005
Biolo G, Di Girolamo FG, Breglia A et al (2015) Inverse relationship between “a body shape index” (ABSI) and fat-free mass in women and men: Insights into mechanisms of sarcopenic obesity. Clin Nutr (Edinb Scotl) 34:323–327. https://doi.org/10.1016/j.clnu.2014.03.015
Dutra MT, Avelar BP, Souza VC et al (2015) Relationship between sarcopenic obesity-related phenotypes and inflammatory markers in postmenopausal women. Clin Physiol Funct Imaging 37:205–210. https://doi.org/10.1111/cpf.12287
Lubkowska A, Radecka A, Bryczkowska I et al (2015) Serum adiponectin and leptin concentrations in relation to body fat distribution, hematological indices and lipid profile in humans. Int J Environ Res Public Health 12:11528–11548. https://doi.org/10.3390/ijerph120911528
Kilgour AH, Firth C, Harrison R et al (2013) Seropositivity for CMV and IL-6 levels are associated with grip strength and muscle size in the elderly. Immun Ageing I & A 10:33. https://doi.org/10.1186/1742-4933-10-33
Schaap LA, Pluijm SM, Deeg DJ et al (2009) Higher inflammatory marker levels in older persons: associations with 5-year change in muscle mass and muscle strength. J Gerontol Ser A Biol Sci Med Sci 64:1183–1189. https://doi.org/10.1093/gerona/glp097
Legrand D, Adriaensen W, Vaes B et al (2013) The relationship between grip strength and muscle mass (MM), inflammatory biomarkers and physical performance in community-dwelling very old persons. Arch Gerontol Geriatr 57:345–351. https://doi.org/10.1016/j.archger.2013.06.003
Acknowledgements
The authors would like to thank CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico) for the financial support (Edital Universal Proc. No. 483966/2013-4).
Funding
This study was funded by the Edital Universal Proc. No. 483966/2013-4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was reviewed and approved by the Research Ethics Committee of the São Paulo State University (Protocol nº: 15995113.8.0000.5402).
Informed consent
The present study complied with ethical standards and informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Rossi, F.E., Lira, F.S., Silva, B.S.A. et al. Influence of skeletal muscle mass and fat mass on the metabolic and inflammatory profile in sarcopenic and non-sarcopenic overfat elderly. Aging Clin Exp Res 31, 629–635 (2019). https://doi.org/10.1007/s40520-018-1029-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-018-1029-3