Abstract
Objective
To externally validate the PALIAR index for patients with advanced, nononcologic chronic diseases.
Methods
We performed a prospective, multicenter cohort study that included patients with advanced, nononcologic chronic diseases hospitalized in internal medicine departments and treated consecutively by the researchers between July 1st and December 31st, 2014. Data were collected from each patient on age, sex, advanced disease, Charlson index, comorbidities, Barthel index, terminal illness symptoms, need for caregiver, hospitalization in the past 3 and 12 months and number of drugs. We calculated the PALIAR index and conducted a 6-month follow-up. To analyze the association between the variables and mortality, we constructed several multivariate logistic regression models.
Results
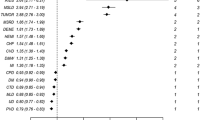
The study included 295 patients with a mean age of 82.7 (8.6) years, 148 (50.2%) of whom were women. Mortality at 6 months was associated with the albumin level (OR 0.52, 95% CI 0.30–0.85, p = 0.011), and the terminal illness (OR 2.75, 95% CI 1.55–4.89, p = 0.001). The PALIAR index showed good discrimination for predicting mortality (statistical C, 0.728, 95% CI 0.670–0.787). A reduced version of the PALIAR index showed similar mortality discriminatory power.
Conclusions
The PALIAR index is a reliable tool for predicting mortality in patients with advanced, nononcologic chronic diseases.



Similar content being viewed by others
References
OECD (2011) Health reform: meeting the challenge of ageing and multiple morbidities. OECD. https://doi.org/10.1787/9789264122314-en. Accessed 02 Feb 2018
WHO. Noncommunicable diseases. http://www.who.int/mediacentre/factsheets/fs355/en/. Accessed 02 Feb 2018
Lunney JR, Lynn J, Foley DJ et al (2003) Patterns of functional decline at the end of life. JAMA 289:2387–2392
Gill TM, Gahbauer EA, Han L et al (2010) Trajectories of disability in the last year of life. N Engl J Med 362:1173–1180
Murray SA, Kendall M, Boyd K et al (2005) Illness trajectories and palliative care. BMJ 330:1007–1011
Hole B, Salem J (2016) How long do patients with chronic diseases expect to live? A systematic review of the literature. BMJ Open 6:e012248
SUPPORT Principal Investigators (1995) A controlled trial to improve care for seriously ill hospitalized patients. JAMA 274:1591–1598
Christakis NA, Lamont EB (2000) Extent and determinants of error in doctors prognoses in terminally ill patients: prospective cohort study. BMJ 320:469–472
Brandt HE, Ooms ME, Ribbe NW et al (2006) Predicted survival vs. actual survival in terminally ill noncancer patients in Dutch nursing homes. J Pain Symptom Manag 32:560–566
Bernabeu-Witell M, Murcia Zaragoza J, Hernández Quiles C et al (2014) Development of a six-month prognostic index in patients with advanced chronic medical conditions: the PALIAR Score. J Pain Symptom Manag 47:551–565
Bestall JC, Paul EA, Garrod R et al (1999) Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax 54:581–586
Levey AS, Coresh J, Balk E et al (2003) National Kidney Foundation practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Ann Intern Med 139:137–147
Pugh RN, Murray-Lyon IM, Dawson JL et al (1973) Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 60:646–649
Pfeiffer E (1975) A short portable mental status questionnaire for the assessment of organic brain deficit in elderly patients. J Am Geriatr Soc 23:433–441
Mahoney FI, Barthel DW (1965) Functional evaluation: the Barthel index. Md State Med J 4:61–65
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Oken MM, Creech RH, Tormey DC et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
National Hospice Organisation (NHO) (1996) Medical guidelines for determining prognosis in selected noncancer diseases. Hospice J 11:47–59
Indice Nacional de Defunciones. https://www.msssi.gob.es/estadEstudios/estadisticas/estadisticas/estMinisterio/IND_TipoDifusion.htm. Accessed 02 Feb 2018
Aragonese Statistics Institute. Aragón basic data. http://www.aragon.es/DepartamentosOrganismosPublicos/Institutos/InstitutoAragonesEstadistica/AreasTematicas/02_Demografia_Y_Poblacion/02_Indicadores_demograficos/ci.01_Indicadores_estructura.detalleDepartamento?channelSelected=0#section1. Accessed 02 Feb 2018
Luppa M, Luck T, Weyerer S et al (2010) Prediction of institutionalization in elderly. A systematic review. Age Ageing 39:31–38
Yourman LC, Lee SJ, Schonberg MA et al (2012) Prognostic indices for older adults. A systematic review. JAMA 307:182–192
Celli BR, Cote CG, Marin JM et al (2004) The body-mass index, airflow obstruction, dyspnea and exercise capacity index in chronic obstructive pulmonary disease. N Engl J Med 350:1005–1012
Levy WC, Mozaffarian D, Linker DT et al (2006) The Seattle Heart Failure Model. Prediction of survival in heart failure. Circulation 113:1424–1433
Pilotto A, Sancalo D, Panza F et al (2009) The Multidimensional Prognostic Index (MPI), based on a comprehensive geriatric assessment, predicts short- and long-term mortality in hospitalized older patients with dementia. J Alzheimers Dis 18:191–199
Pilotto A, Addante F, D´Onofrio G et al (2009) The comprehensive geriatric assessment and the multidimensional approach. A new look at the older patient with gastroenterological disorders. Best Pract Res Clin Gastroenterol 23:829–837
Pilotto A, Sancarlo D, Aucella F et al (2012) Addition of the multidimensional prognostic index to the estimated glomerular filtration rate improves prediction of long-term all-cause mortality in older patients with chronic kidney disease. Rejuvenation Res 15:82–88
Acknowledgements
List of researchers of the PALIARAGON Study Jesús Díez-Manglano, José Velilla-Marco, Carmen Bueno-Castel, Alfonso García-Aranda, Ester Artajona-Rodrigo (Internal Medicine Department, Hospital Universitario Miguel Servet, Zaragoza), Carolina Clemente-Sarasa, Daniel Fuertes-Ruiz, Esperanza Bejarano-Tello, Eulalia Munilla-López, María-Pilar Lambán-Aranda (Internal Medicine Department, Hospital Royo Villanova, Zaragoza), Noelia Gómez-Aguirre (Internal Medicine Department, Hospital Ernest Lluch, Calatayud), Begoña De Escalante-Yangüela, Borja Gracia-Tello, Jorge Rubio-Gracia (Internal Medicine Department, Hospital Clínico Universitario Lozano Blesa, Zaragoza), José-Luis Cabrerizo-García, Sandra Yagüe-Vallejo (Internal Medicine Department, Hospital General de la Defensa, Zaragoza).
Funding
The Research Group on Comorbidity and Polypathology in Aragón is co-financed from the European Regional Development Fund.
Author information
Authors and Affiliations
Consortia
Contributions
We assure that all authors included on a paper fulfill the criteria of authorship. JD-M, JV-M and NG-A designed the study. All authors performed data collection. Data analysis was performed by JD-M. The manuscript was drafted by JD-M, and all authors helped with its revision and gave final approval of this version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Statement of human and animal rights
The study was approved by the Clinical Research Ethics Committee of Aragon, and was carried out in accordance with the principles of the Declaration of Helsinki. This article does not contain any studies with animal performed by any of the authors.
Informed consent
All patients (or their caregivers in the case of cognitive impairment) signed a written informed consent form.
Additional information
The list of researchers of the PALIARAGON Study are given in Acknowledgements.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gómez-Aguirre, N., Fuertes-Ruiz, D., Gracia-Tello, B. et al. External validation of the PALIAR index for patients with advanced, nononcologic chronic diseases. Aging Clin Exp Res 31, 393–402 (2019). https://doi.org/10.1007/s40520-018-0980-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-018-0980-3