Abstract
Aim
To determine if age is a factor influencing the type of breast cancer surgery (radical versus conservative) in Italy and to investigate the regional differences in breast cancer surgery clinical practice.
Methods
Retrospective study is based on national hospital discharge records. The study draws on routinely collected data from hospital discharge records in Italy in 2010. The following exclusion criteria were applied: day hospital stays, patients younger than 17 years, males, patients without an ICD-9CM code indicating breast cancer and breast surgery, and repeated hospital admission of the same patient. Overall, 49,058 patient records were selected for the analysis.
Results
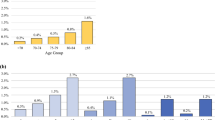
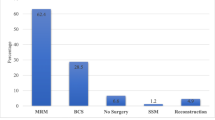
The proportion of conservative breast cancer operations was 70.9%. A greater number of women younger than 70 had undergone a breast-conserving operation compared to older women. There were regional variations ranging from a minimum in Basilicata to a maximum in Val d’Aosta. Multivariate analysis revealed that older patients with lower clinical severity were more likely to have undergone a radical operation than younger women. In addition, radical surgery was approximately twice as likely to occur in a private hospital that performed at least 50 breast cancer operations annually than in a public hospital that performed <50 breast surgeries.
Conclusion
Notwithstanding increases in life expectancy and the lack of clinical evidence to support the use of age as a surrogate for co-morbid conditions and frailty, our data on breast cancer operations in Italy are consistent with the hypothesis suggesting the persistence of ageistic practice in the healthcare system.
Similar content being viewed by others
References
Bouchardy C, Rapiti E, Fioretta G, Laissue P, Neyroud-Caspar I, Schafer P et al (2003) Undertreatment strongly decreases prognosis of breast cancer in elderly women. J Clin Oncol Off J Am Soc Clin Oncol 21:3580–3587. doi:10.1200/jco.2003.02.046
Wanebo HJ, Cole B, Chung M, Vezeridis M, Schepps B, Fulton J et al (1997) Is surgical management compromised in elderly patients with breast cancer? Ann Surg 225:579–586 (discussion 86–89)
Veronesi U, Cascinelli N, Mariani L, Greco M, Saccozzi R, Luini A et al (2002) Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med 347:1227–1232. doi:10.1056/NEJMoa020989
Fisher B, Anderson S, Bryant J, Margolese RG, Deutsch M, Fisher ER et al (2002) Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med 347:1233–1241. doi:10.1056/NEJMoa022152
Mandelblatt JS, Hadley J, Kerner JF, Schulman KA, Gold K, Dunmore-Griffith J et al (2000) Patterns of breast carcinoma treatment in older women: patient preference and clinical and physical influences. Cancer 89:561–573
Smith GL, Xu Y, Shih YC, Giordano SH, Smith BD, Hunt KK et al (2009) Breast-conserving surgery in older patients with invasive breast cancer: current patterns of treatment across the United States. J Am Coll Surg 209:425–433. doi:10.1016/j.jamcollsurg.2009.06.363
Wang J, Kollias J, Boult M, Babidge W, Zorbas HN, Roder D et al (2010) Patterns of surgical treatment for women with breast cancer in relation to age. Breast J 16:60–65. doi:10.1111/j.1524-4741.2009.00828.x
Bates T, Kearins O, Monypenny I, Lagord C, Lawrence G (2009) Clinical outcome data for symptomatic breast cancer: the Breast Cancer Clinical Outcome Measures (BCCOM) Project. Br J Cancer 101:395–402. doi:10.1038/sj.bjc.6605155
Barchielli A, Gini R, Roti L (2004) Indicatori di qualità dell’assistenza agli anziani. Agenzia Regional Sanità, Toscana
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
White H (1980) A heteroscedasticity-consistent covariance matrix estimator and a direct test for heteroscedasticity. Econometrica 48:817–838
User guide for age discrimination benchmarking tool (2002) Department of Health, UK
Chapter 17 Cancer (2010) Achieving age equality in health and social care, NHS pratice guide. NHS, UK
A literature review of the likely costs and benefits of legislation to prohibit age discrimination in health (2007) social care and mental health services and definitions of age discrimination that might be operationalised for measurement. Centre for Policy on Ageing, UK
Hind D, Wyld L, Reed MW (2007) Surgery, with or without tamoxifen, vs tamoxifen alone for older women with operable breast cancer: cochrane review. Br J Cancer 96:1025–1029. doi:10.1038/sj.bjc.6603600
Pritchard KI (2007) Have we been guilty of ageism in the primary treatment of breast cancer? Br J Cancer 96:1011–1012. doi:10.1038/sj.bjc.6603697
Lawler M, Selby P, Aapro MS, Duffy S (2014) Ageism in cancer care. BMJ 348:g1614. doi:10.1136/bmj.g1614
Chan DSY, Johnson RC, Shering SG (2010) Management of breast cancer in older women: factors which influence patients’ decision. The Open Breast. Cancer J 2:42–45
Siesling S, van de Poll-Franse LV, Jobsen JJ, Repelaer van Driel OJ, Voogd AC (2007) Explanatory factors for variation in the use of breast conserving surgery and radiotherapy in the Netherlands, 1990–2001. Breast (Edinburgh, Scotland) 16:606–614. doi:10.1016/j.breast.2007.05.004
Brunello A, Basso U, Pogliani C, Jirillo A, Ghiotto C, Koussis H et al (2005) Adjuvant chemotherapy for elderly patients (> or =70 years) with early high-risk breast cancer: a retrospective analysis of 260 patients. Ann Oncol 16:1276–1282. doi:10.1093/annonc/mdi257
Solej M, Ferronato M, Nano M (2005) Locally advanced breast cancer in the elderly: curettage mastectomy. Tumori 91:321–324
Sanguinetti A, Ragusa M, De Falco M, Sperlongano P, Calzolari F, Parmeggiani D et al (2007) Locally advanced breast cancer in elderly patients: treatment standardised or tailored to individual needs? Chir Ital 59:829–833
Schonberg MA, Marcantonio ER, Ngo L, Li D, Silliman RA, McCarthy EP (2011) Causes of death and relative survival of older women after a breast cancer diagnosis. J Clin Oncol Off J Am Soc Clin Oncol 29:1570–1577. doi:10.1200/JCO.2010.33.0472
Darby SC, Ewertz M, McGale P, Bennet AM, Blom-Goldman U, Bronnum D et al (2013) Risk of ischemic heart disease in women after radiotherapy for breast cancer. N Engl J Med 368:987–998. doi:10.1056/NEJMoa1209825
Acknowledgements
We want to thank the “Agenzia Nazionale per i Servizi Sanitari Regionali” for providing the national database on Hospital Discharge Forms.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest has been declared by the authors.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Di Rosa, M., Chiatti, C., Rimland, J.M. et al. Ageism and surgical treatment of breast cancer in Italian hospitals. Aging Clin Exp Res 30, 139–144 (2018). https://doi.org/10.1007/s40520-017-0757-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-017-0757-0