Abstract
Objectives
To investigate whether a liberal blood transfusion strategy [Hb levels ≥11.3 g/dL (7 mmol/L)] reduces the risk of postoperative delirium (POD) on day 10, among nursing home residents with hip fracture, compared to a restrictive transfusion strategy [Hb levels ≥9.7 g/dL (6 mmol/L)]. Furthermore, to investigate whether POD influences mortality within 90 days after hip surgery.
Methods
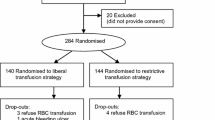
This is a post hoc analysis based on The TRIFE - a randomized controlled trial. Frail anemic patients from the Orthopedic Surgical Ward at Aarhus University Hospital were enrolled consecutively between January 18, 2010 and June 6, 2013. These patients (aged ≥65 years) had been admitted from nursing homes for unilateral hip fracture surgery. After surgery, 179 patients were included in this study. On the first day of hospitalization, all enrolled patients were examined for cognitive impairment (assessed by MMSE) and delirium (assessed by CAM). Delirium was also assessed on the tenth postoperative day.
Results
The prevalence of delirium was 10 % in patients allocated to a liberal blood transfusion strategy (LB) and 21 % in the group with a restrictive blood transfusion strategy (RB). LB prevents development of delirium on day 10, compared to RB, odds ratio 0.41 (95 % CI 0.17–0.96), p = 0.04. Development of POD on day 10 increased the risk of 90-day death, hazard ratio 3.14 (95 % CI 1.72–5.78), p < 0.001.
Conclusion
In nursing home residents undergoing surgery for hip fracture, maintaining hemoglobin level above 11.3 g/dL reduces the rate of POD on day 10 compared to a RB. Development of POD is associated with increased mortality.


Similar content being viewed by others
References
Rudolph JL, Marcantonio ER (2011) Review articles: postoperative delirium: acute change with long-term implications. Anesth Analg 112:1202–1211
Bitsch M, Foss N, Kristensen B et al (2004) Pathogenesis of and management strategies for postoperative delirium after hip fracture: a review. Acta Orthop Scand 75:378–389
Olofsson B, Lundström M, Borssén B et al (2005) Delirium is associated with poor rehabilitation outcome in elderly patients treated for femoral neck fractures. Scand J Caring Sci 19:119–127
Caplan GA, Coconis J, Board N et al (2006) Does home treatment affect delirium? A randomised controlled trial of rehabilitation of elderly and care at home or usual treatment (The REACH-OUT trial). Age Ageing 35:53
Lee K, Ha Y, Lee Y et al (2011) Frequency, risk factors, and prognosis of prolonged delirium in elderly patients after hip fracture surgery. Clin Orthop Relat Res 469:2612–2620
Brown CA, Boling J, Manson M et al (2012) Relation between prefracture characteristics and perioperative complications in the elderly adult patient with hip fracture. South Med J 105:306–310
Engedal K (2007) Tværfaglig geriatri. In: Bondevik M, Nygaard HA (eds). 1. bogklubudgave (2. udgave) ed. Kbh.: Gyldendals Bogklubber. pp 317–333
Kumar D, Mbako AN, Riddick A et al (2011) On admission haemoglobin in patients with hip fracture. Injury 42:167–170
Gruber-Baldini AL, Marcantonio E, Orwig D et al (2013) Delirium outcomes in a randomized trial of blood transfusion thresholds in hospitalized older adults with hip fracture. J Am Geriatr Soc 61:1286–1295
Behrends M, DePalma G, Sands L et al (2013) Association between intraoperative blood transfusions and early postoperative delirium in older adults. J Am Geriatr Soc 61:365–370
Marcantonio ER, Goldman L, Orav EJ et al (1998) The association of intraoperative factors with the development of postoperative delirium. Am J Med 105:380–384
Vochteloo AJ, van der Burg BLB, Mertens B et al (2011) Outcome in hip fracture patients related to anemia at admission and allogeneic blood transfusion: an analysis of 1262 surgically treated patients. BMC Musculoskelet Disord 12:262
WHO (2011) Haemoglobin concentrations for diagnosis of anemia and assessment of severity. http://www.who.int/vmnis/indicators/haemoglobin.pdf. Accessed on 01 July 2015
Danish Health and Medicine Authority (2015) Guidelines no. 9038. Blood transfusion
Gregersen M, Damsgaard EM, Borris LC (2015) Blood transfusion and risk of infection in frail elderly after hip fracture surgery: the TRIFE randomized controlled trial. Eur J Orthop Surg Traumatol 25:1031–1038
Gregersen M, Zintchouk D, Borris LC et al (2011) A geriatric multidisciplinary and tailor-made hospital-at-home method in nursing home residents with hip fracture. Geriatr Orthop Surg Rehabil 2:148–154
Danish Health and Medicine Authority (2008) Guidelines no. 10333. Blood transfusion
Gregersen M, Borris LC, Damsgaard EM (2015) Postoperative blood transfusion strategy in frail, anemic elderly patients with hip fracture. Acta Orthop 14:1–10
Inouye SK, van Dyck CH, Alessi CA et al (1990) Clarifying confusion: the confusion assessment method—a new method for detection of delirium. Ann Intern Med 113:941–948
National Institute for Health and Clinical Excellence (2010) NICE clinical guideline. Delirium: Diagnosis, prevention and management. http://www.nice.org.uk/nicemedia/live/13060/49909/49909.pdf. Accessed on 04 Dec 2014
Dansk Multidisciplinær Cancer Gruppe for Palliativ Indsats (2013) Klinisk retningslinje om delirium. CFKR. www.cfkr.dk
Hestermann U, Backenstrass M, Gekle I et al (2009) Validation of a German version of the confusion assessment method for delirium detection in a sample of acute geriatric patients with a high prevalence of dementia. Psychopathology 42:270–276
Wei LA, Fearing MA, Sternberg EJ et al (2008) The confusion assessment method: a systematic review of current usage. J Am Geriatr Soc 56:823–830
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Korner EA, Lauritzen L, Nilsson FM et al (2008) Mini mental state examination. Validation of new Danish version. Ugeskr Laeger 170:745–749
Juliebø V, Bjøro K, Krogseth M et al (2009) Risk factors for preoperative and postoperative delirium in elderly patients with hip fracture. J Am Geriatr Soc 57:1354–1361
de Lange E, Verhaak PF, van der Meer K (2013) Prevalence, presentation and prognosis of delirium in older people in the population, at home and in long term care: a review. Int J Geriatr Psychiatry 28:127–134
Lundstrom M, Edlund A, Bucht G et al (2003) Dementia after delirium in patients with femoral neck fractures. J Am Geriatr Soc 51:1002–1006
Krogseth M, Wyller TB, Engedal K et al (2011) Delirium is an important predictor of incident dementia among elderly hip fracture patients. Dement Geriatr Cognit Disord 31:63–70
Fan YX, Liu FF, Jia M et al (2014) Comparison of restrictive and liberal transfusion strategy on postoperative delirium in aged patients following total hip replacement: a preliminary study. Arch Gerontol Geriatr 59:181–185
Witlox J, Eurelings LS, de Jonghe JF et al (2010) Delirium in elderly patients and the risk of postdischarge mortality, institutionalization, and dementia: a meta-analysis. JAMA 304:443–451
Bellelli G, Mazzola P, Morandi A et al (2014) Duration of postoperative delirium is an independent predictor of 6-month mortality in older adults after hip fracture. J Am Geriatr Soc 62:1335–1340
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
The TRIFE study was conducted in accordance with the ethical principles of the Declaration of Helsinki and approved by the Central Denmark Region Ethical Committee. The study protocol was approved by the Danish Data Protection Agency on November 4, 2014. Data were stored according to good research practice. The TRIFE study is registered at ClinicalTrials.gov (Identifier NCT01102010).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Blandfort, S., Gregersen, M., Borris, L.C. et al. Blood transfusion strategy and risk of postoperative delirium in nursing homes residents with hip fracture. A post hoc analysis based on the TRIFE randomized controlled trial. Aging Clin Exp Res 29, 459–466 (2017). https://doi.org/10.1007/s40520-016-0587-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-016-0587-5