Abstract
Background and aims
We aimed to test the hypothesis that central blood pressure (BP) would be lower in healthy older adults with greater daily ambulatory activity.
Methods
Forty-three (24 women, 19 men) older adults wore a triaxial accelerometer at the hip for 1 week. The volume of ambulatory activity was estimated by average steps per day. As a proxy of intensity of ambulatory activity, 1-min peak step accumulation, or the maximum number of steps taken within a minute was averaged from each day. Participants were considered “active” if they had >7500 steps per day or >105 steps per min. Radial arterial tonometry was used to estimate central (aortic) BP from pulse wave analysis.
Results
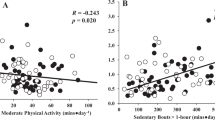
After adjusting for age and sex, adults with higher steps per day (n = 18) tended to have lower central pulse pressure (p = 0.08). Interestingly, adults with higher peak step accumulation (n = 25) had significantly lower central pulse pressure (40.4 ± 1.6 vs. 46.8 ± 2.0 mmHg; p = 0.02) after adjusting for age and sex. Stepwise regression including age, sex, body mass index, and peak step accumulation found body mass index to be the strongest predictor of central systolic BP [β = 0.42, 95 % CI (0.13, 0.70), p = 0.004] while peak step accumulation was the strongest predictor of central pulse pressure [β = −0.31, 95 % CI (−0.01, −0.60), p = 0.043].
Conclusions
These results find older adults with an “active” daily walking pattern, particularly having a higher number of maximal steps in a minute, have lower central pulse pressure than older adults with lower daily ambulatory activity.

Similar content being viewed by others
References
Ham SA, Kruger J, Tudor-Locke C (2009) Participation by US adults in sports, exercise, and recreational physical activities. J Phys Act Health 6:6–14
Aoyagi Y, Park H, Kakiyama T, Park S, Yoshiuchi K, Shephard RJ (2010) Yearlong physical activity and regional stiffness of arteries in older adults: the Nakanojo Study. Eur J Appl Physiol 109:455–464
Ayabe M, Park S, Shephard RJ, Aoyagi Y (2015) Associations of activity monitor output and an estimate of aerobic fitness with pulse wave velocities: the Nakanojo Study. J Phys Act Health 12:139–144
Kaess BM, Rong J, Larson MG, Hamburg NM, Vita JA, Levy D, Benjamin EJ, Vasan RS, Mitchell GF (2012) Aortic stiffness, blood pressure progression, and incident hypertension. JAMA 308:875–881
Najjar SS, Scuteri A, Shetty V, Wright JG, Muller DC, Fleg JL, Spurgeon HP, Ferrucci L, Lakatta EG (2008) Pulse wave velocity is an independent predictor of the longitudinal increase in systolic blood pressure and of incident hypertension in the Baltimore Longitudinal Study of Aging. J Am Coll Cardiol 51:1377–1383
Mitchell GF, Wang N, Palmisano JN, Larson MG, Hamburg NM, Vita JA, Levy D, Benjamin EJ, Vasan RS (2010) Hemodynamic correlates of blood pressure across the adult age spectrum/clinical perspective. Circ 122:1379–1386
Hashimoto J, Ito S (2009) Some mechanical aspects of arterial aging: physiological overview based on pulse wave analysis. Ther Adv Cardiovasc Dis 3:367–378
Roman MJ, Devereux RB, Kizer JR, Lee ET, Galloway JM, Ali T, Umans JG, Howard BV (2007) Central pressure more strongly relates to vascular disease and outcome than does brachial pressure: the strong heart study. Hypertension 50:197–203
McDonnell BJ, Maki-Petaja KM, Munnery M, Yasmin Wilkinson IB, Cockcroft JR, McEniery CM (2013) Habitual exercise and blood pressure: age dependency and underlying mechanisms. Am J Hypertens 26:334–341
Nualnim N, Barnes JN, Tarumi T, Renzi CP, Tanaka H (2011) Comparison of central artery elasticity in swimmers, runners, and the sedentary. Am J Cardiol 107:783–787
Dall PM, McCrorie PRW, Granat MH, Stansfield BW (2013) Step accumulation per minute epoch is not the same as cadence for free-living adults. Med Sci Sports Exerc 45:1995–2001
Tudor-Locke C, Brashear MM, Katzmarzyk PT, Johnson WD (2012) Peak stepping cadence in free-living adults: 2005-2006 NHANES. J Phys Act Health 9:1125–1129
Schuna JMJ, Brouillette RM, Foil HC, Fontenot SL, Keller JN, Tudor-Locke C (2013) Steps per day, peak cadence, body mass index, and age in community-dwelling older adults. Med Sci Sports Exerc 45:914–919
Gonzales JU, Kumar P, Shephard J, Means A (2014) Peak stepping cadence is associated with leg vascular compliance in young adults. J Sci Med Sport 17:683–687
Gonzales JU, Wiberg M, Defferari E, Proctor DN (2015) Arterial stiffness is higher in older adults with increased perceived fatigue and fatigability during walking. Exp Gerontol 61:92–97
Choi L, Liu Z, Matthews CE, Buchowski MS (2011) Validation of accelerometer wear and nonwear time classification algorithm. Med Sci Sports Exerc 43:357–364
Tudor-Locke C, Bassett DR (2004) How many steps/day are enough? Preliminary pedometer indices for public health. Sports Med 34:1–8
García-Ortiz L, Recio-Rodríguez JI, Trucksäss AS, Puigdomenech-Puig E, Martínez-Vizcaíno V, Fernández-Alonso C, Rubio-Galan J, Agudo-Conde C, Patino-Alonso MC, Rodríguez-Sánchez E, Gómez-Marcos MA, EVIDENT Group (2014) Relationship between objectively measured physical activity and cardiovascular aging in the general population—the EVIDENT trial. Atherosclerosis 233:434–440
Brook RD, Appel LJ, Rubenfire M, Ogedegbe G, Bisognano JD, Elliott WJ, Fuchs FD, Hughes JW, Lackland DT, Staffileno BA, Townsend RR, Rajagopalan S (2013) Beyond medications and diet: alternative approaches to lowering blood pressure: a scientific statement from the American Heart Association. Hypertension 61:1360–1383
van Dijk S, van den Meiracker A, van der Cammen T, Mattace Raso F, van der Velde N (2012) Central but not peripheral fat mass percentage is associated with blood pressure components in the elderly. Age Ageing 41:534–540
Carlyle M, Jones OB, Kuo JJ, Hall JE (2002) Chronic cardiovascular and renal actions of leptin: role of adrenergic activity. Hypertension 39:496–501
Korda M, Kubant R, Patton S, Malinski T (2008) Leptin-induced endothelial dysfunction in obesity. Am J Physiol Heart Circ Physiol 295:H1514–H1521
Nemoto K, Gen-no H, Masuki S, Okazaki K, Nose H (2007) Effects of high-intensity interval walking training on physical fitness and blood pressure in middle-aged and older people. Mayo Clin Proc 82:803–811
Tudor-Locke C, Schuna JM, Barreira TV, Mire EF, Broyles ST, Katzmarzyk PT, Johnson WD (2013) Normative steps/day values for older adults: NHANES 2005–2006. J Gerontol Series A Biol Sci Med Sci 68:1426–1432
Marshall SJ, Levy SS, Tudor-Locke CE, Kolkhorst FW, Wooten KM, Ji M, Macera CA, Ainsworth BE (2009) Translating physical activity recommendations into a pedometer-based step goal: 3000 Steps in 30 Minutes. Am J Prev Med 36:410–415
Ward DS, Evenson KR, Vaughn A, Rodgers AB, Troiano RP (2005) Accelerometer use in physical activity: best practices and research recommendations. Med Sci Sports Exerc 37:S582–S588
Acknowledgments
The authors would like to thank the participants for their time and effort. We also thank Ramona Harwell for her valuable administrative assistance. This study was funded by institutional startup funds.
Conflict of interest
The author has no real or perceived conflicts of interest arising from intellectual, personal, or financial circumstances of this research.
Compliance with ethical standards
This study was approved by an institutional review board for human privacy and protection, and follows ethical standards set by the Declaration of Helsinki.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gonzales, J.U. Do older adults with higher daily ambulatory activity have lower central blood pressure?. Aging Clin Exp Res 28, 965–971 (2016). https://doi.org/10.1007/s40520-015-0384-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-015-0384-6