Abstract
Purpose
To examine whether metabolic syndrome (MetS) is related to estimation of weight status and weight-loss efforts in Korean adults with non-obesity.
Methods
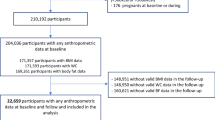
In 4345 men and 6387 women in non-obese Koreans (age 49.2 ± 16.7 years, BMI < 25 kg/m2) participating in the 2011–2013 Korean National Health and Nutrition Examination Survey, the presence/absence of MetS using the harmonized criteria, and weight perception and weight-loss efforts using questionnaires were assessed. Estimation of weight status was determined as underestimation, correct estimation, and overestimation based on differences between perceived weight categories and BMI-based categories.
Results
15.7% in men and 12.6% in women with BMI < 25 kg/m2 had the MetS. After adjusting for sociodemographic factors, health-related behaviors, treatment of cardiovascular diseases and cardiovascular risk factors, and BMI-based categories, correct estimation and overestimation of weight status in men [odds ratio (95% CI), 1.58 (1.29–1.92); 2.82 (1.48–5.38)], and women [1.53 (1.26–1.86); 1.59 (1.09–2.31)] were positively associated with the presence of MetS compared to those with underestimation of weight status. After adjusting for weight estimation, sociodemographic factors, health-related behaviors, and treatment of cardiovascular diseases and cardiovascular risk factors, weight-loss efforts were positively associated with the presence of MetS [1.66 (1.33–2.08) in men, 1.31 (1.07–1.61) in women] in all subjects, and number of MetS components [1.28 (1.02–1.62) per 1 more component] in those with MetS.
Conclusions
In non-obese individuals, correct estimation and overestimation of weight status may be more likely to identify individuals with MetS and concurrent MetS may increase weight-loss efforts regardless of weight estimation.
Level of evidence
Level III, evidence obtained from a case–control observational study.
Similar content being viewed by others
References
Lopez-Miranda J, Perez-Martinez P (2013) It is time to define metabolically obese but normal-weight (MONW) individuals. Clin Endocrinol (Oxf) 3:314–315
Conus F, Rabasa-Lhoret R, Peronnet F (2007) Characteristics of metabolically obese normal-weight (MONW) subjects. Appl Physiol Nutr Metab 1:4–12
Choi KM, Cho HJ, Choi HY, Yang SJ, Yoo HJ, Seo JA et al (2013) Higher mortality in metabolically obese normal-weight people than in metabolically healthy obese subjects in elderly Koreans. Clin Endocrinol (Oxf) 3:364–370
Fan J, Song Y, Chen Y, Hui R, Zhang W (2013) Combined effect of obesity and cardio-metabolic abnormality on the risk of cardiovascular disease: a meta-analysis of prospective cohort studies. Int J Cardiol 5:4761–4768
Lee K (2009) Metabolically obese but normal weight (MONW) and metabolically healthy but obese (MHO) phenotypes in Koreans: characteristics and health behaviors. Asia Pac J Clin Nutr 2:280–284
Choi J, Se-Young O, Lee D, Tak S, Hong M, Park SM et al (2005) Characteristics of diet patterns in metabolically obese, normal weight adults (Korean National Health and Nutrition Examination Survey III. Nutr Metab Cardiovasc Dis 2012;7:567–574
Choi JY, Ha HS, Kwon HS, Lee SH, Cho HH, Yim HW et al (2013) Characteristics of metabolically obese, normal-weight women differ by menopause status: the Fourth Korea National Health and Nutrition Examination Survey. Menopause 1:85–93
Dvorak RV, DeNino WF, Ades PA, Poehlman ET (1999) Phenotypic characteristics associated with insulin resistance in metabolically obese but normal-weight young women. Diabetes 11:2210–2214
Badoud F, Perreault M, Zulyniak MA, Mutch DM (2015) Molecular insights into the role of white adipose tissue in metabolically unhealthy normal weight and metabolically healthy obese individuals. FASEB J 3:748–758
Guglielmi V, Sbraccia P (2017) Obesity phenotypes: depot-differences in adipose tissue and their clinical implications. Eat Weight Disord
Mogre V, Abedandi R, Salifu ZS (2014) Distorted self-perceived weight status and underestimation of weight status in diabetes mellitus type 2 patients. PLoS One 4:e95165
Baur DM, Christophi CA, Tsismenakis AJ, Jahnke SA, Kales SN (2012) Weight-perception in male career firefighters and its association with cardiovascular risk factors. BMC Public Health 480-2458-12-480
Duncan DT, Wolin KY, Scharoun-Lee M, Ding EL, Warner ET, Bennett GG (2011) Does perception equal reality? Weight misperception in relation to weight-related attitudes and behaviors among overweight and obese US adults. Int J Behav Nutr Phys Act. 20-5868-8-20
Lee K (2016) Parental and offspring factors in offspring’s weight-loss efforts. Eat Weight Disord 4:679–685
Peltzer K, Pengpid S (2015) Trying to lose weight among non-overweight university students from 22 low, middle and emerging economy countries. Asia Pac J Clin Nutr 1:177–183
Yaemsiri S, Slining MM, Agarwal SK (2011) Perceived weight status, overweight diagnosis, and weight control among US adults: the NHANES 2003–2008 study. Int J Obes (Lond) 8:1063–1070
Montani JP, Schutz Y, Dulloo AG. Dieting and weight cycling as risk factors for cardiometabolic diseases: who is really at risk?. Obes Rev., 2015:7–18
Guidelines for heath survey (2013) The Sixth Korea National Health and Nutrition Examination Survey (KNHANES VI-1), 2013, Korea Centers for Disease Control and Prevention
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA et al (2009) Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 16:1640–1645
The International Association for the Study of Obesity and the International Obesity Task Force (2000) The Asia–Pacific perspective: redefining obesity and its treatment. IASO and IOTF, Australia
Gregory CO, Blanck HM, Gillespie C, Maynard LM, Serdula MK (2008) Perceived health risk of excess body weight among overweight and obese men and women: differences by sex. Prev Med 1:46–52
Gregory CO, Blanck HM, Gillespie C, Maynard LM, Serdula MK (2008) Health perceptions and demographic characteristics associated with underassessment of body weight. Obesity (Silver Spring) 5:979–986
Wardle J, Haase AM, Steptoe A (2006) Body image and weight control in young adults: international comparisons in university students from 22 countries. Int J Obes (Lond) 4:644–651
Wang B, Zhuang R, Luo X, Yin L, Pang C, Feng T et al (2015) Prevalence of metabolically healthy obese and metabolically obese but normal weight in adults worldwide: a meta-analysis. Horm Metab Res 11:839–845
Acevedo P, Lopez-Ejeda N, Alferez-Garcia I, Martinez-Alvarez JR, Villarino A, Cabanas MD et al (2014) Body mass index through self-reported data and body image perception in Spanish adults attending dietary consultation. Nutrition 6:679–684
Wang ML, Haughton CF, Frisard C, Pbert L, Geer C, Lemon SC (2017) Perceived weight status and weight change among a US adult sample. Obesity (Silver Spring) 1:223–228
Acknowledgements
This work was supported by the National Resarch Foundation of Korea Grant funded by the Korean Government (NRF-2017S1A5B8066096).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
This work was supported by the National Rsearch Foundation of Korea Grant funded by the Korean Government (NRF-2017S1A5B8066096).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Lee, K. Estimation of weight status and weight-loss efforts in Korean adults with non-obesity considering metabolic syndrome. Eat Weight Disord 24, 135–142 (2019). https://doi.org/10.1007/s40519-018-0484-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-018-0484-3