Abstract
Purpose
Concerns remain on different alveolar deposition of surfactant between LISA and INSURE methods. Ultrasound evaluation of diaphragm kinetics may provide clinical evidence on this issue, as indirect representation of the respiratory system compliance.
Methods
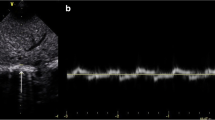
This was a prospective-observational pilot study. The inclusion criterion was CPAP-supported infants ≤ 32 weeks with RDS receiving surfactant via minimally invasive technique. 52 patients randomized for surfactant administration via LISA or INSURE methods were enrolled. Right diaphragm (RD) global mean peak velocity (MPV) by Pulsed-Wave Tissue Doppler Imaging (PTDI) was recorded before and two hours after surfactant administration with simultaneous measurements of oxygen saturation (SpO2)/fraction of inspired oxygen (FiO2) (SF ratio). Mechanical ventilation ≤ 72 h from birth represented treatment failure.
Results
LISA infants had significantly higher gestational age (p = 0.029) and birth weight (p = 0.030) with lower CRIB-II scores (p = 0.030) than INSURE infants. LISA infants showed higher median MPV at baseline RD-PTDI US assessment (p = 0.024), but post-surfactant median MPV and other the investigated variables were similar at the adjusted analysis for gestational age and sedation. 8/52 (15%) infants who failed treatment had a significantly lower SF ratio (p = 0.002) and higher median MPV at RD-PTDI US (p = 0.004) after surfactant administration, despite the higher CPAP support level before (p = 0.007) and after (p = 0.001) surfactant administration. A full course of antenatal steroids was protective against mechanical ventilation (p = 0.038).
Conclusions
Different minimally invasive surfactant administration techniques do not appear to influence diaphragm kinetics evaluated by RD-PTDI US.

Similar content being viewed by others
Data availability
The data that support the findings of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request. Data are located in controlled access data storage at: https://docs.google.com/spreadsheets/d/1z3Gil-uTw5rPDAwlTnWaL_I4Mr_ggwNh/edit?usp=sharing&ouid=108672324634995930721&rtpof=true&sd=true.
References
Mahmoud RA, Schmalisch G, Oswal A, Christoph RC (2022) Non-invasive ventilatory support in neonates: an evidence-based update. Paediatr Respir Rev 44:11–18
Ho JJ, Subramaniam P, Davis PG (2020) Continuous positive airway pressure (CPAP) for respiratory distress in preterm infants. Cochrane Database Syst Rev 10:CD002271
Solevåg AL, Cheung PY, Schmölzer GM (2021) Bi-level noninvasive ventilation in neonatal respiratory distress syndrome. A systematic review and meta-analysis. Neonatology 118:264–273
Bahadue FL, Soll R (2012) Early versus delayed selective surfactant treatment for neonatal respiratory distress syndrome. Cochrane Database Syst Rev 11:CD001456
Abdel-Latif ME, Davis PG, Wheeler KI, De Paoli AG, Dargaville PA (2021) Surfactant therapy via thin catheter in preterm infants with or at risk of respiratory distress syndrome. Cochrane Database Syst Rev 5:CD011672
Anand R, Nangia S, Kumar G, Mohan MV, Dudeja A (2022) Less invasive surfactant administration via infant feeding tube versus INSURE method in preterm infants: a randomized control trial. Sci Rep 12:21955
De Luca D, Shankar-Aguilera S, Bancalari E (2021) LISA/MIST: complex clinical problems almost never have easy solutions. Semin Fetal Neonatal Med 26(2):101230. https://doi.org/10.1016/j.siny.2021.101230
Janssen LC, Van Der Spil J, van Kaam AH, Dieleman JP, Andriessen P, Onland W, Niemarkt HJ (2019) Minimally invasive surfactant therapy failure: risk factors and outcome. Arch Dis Child Fetal Neonatal Ed 104:F636–F642
De Bisschop B, Derriks F, Cools F (2020) Early predictors for INtubation-SURfactant-extubation failure in preterm infants with neonatal respiratory distress syndrome: a systematic review. Neonatolog 117:33–45
Miller LE, Stoller JZ, Fraga MV (2020) Point-of-care ultrasound in the neonatal ICU. Curr Opin Pediatr 32:216–227
Zambon M, Greco M, Bocchino S, Cabrini L, Beccaria PF, Zangrillo A (2017) Assessment of diaphragmatic dysfunction in the critically ill patient with ultrasound: a systematic review. Intensive Care Med 43:29–38
Weber MD, Lim JKB, Glau C, Conlon T, James R, Lee JH (2021) A narrative review of diaphragmatic ultrasound in pediatric critical care. Pediatr Pulmonol 56:2471–2483
Rehan VK, McCool FD (2003) Diaphragm dimensions of the healthy term infant. Acta Paediatr 92:1062–1067
Rehan VK, Nakashima JM, Gutman A, Rubin LP, McCool FD (2000) Effects of the supine and prone position on diaphragm thickness in healthy term infants. Arch Dis Child 83:234–238
Rehan VK, Laiprasert J, Wallach M, Rubin LP, McCool FD (2001) Diaphragm dimensions of the healthy preterm infant. Pediatrics 108:E91
Rehan VK, Laiprasert J, Nakashima JM, Wallach M, McCool FD (2001) Effects of continuous positive airway pressure on diaphragm dimensions in preterm infants. J Perinatol 21:521–524
Yeung T, Mohsen N, Ghanem M, Ibrahim J, Shah J, Kajal D, Shah PS, Mohamed A (2023) Diaphragmatic thickness and excursion in preterm infants with bronchopulmonary dysplasia compared with term or near term infants: a prospective observational study. Chest 163:324–331
El-Mogy M, El-Halaby H, Attia G, Abdel-Hady H (2018) Comparative study of the effects of continuous positive airway pressure and nasal high-flow therapy on diaphragmatic dimensions in preterm infants. Am J Perinatol 35:448–454
Dassios T, Vervenioti A, Dimitriou G (2022) Respiratory muscle function in the newborn: a narrative review. Pediatr Res 91:795–803
Alonso-Ojembarrena A, Ruiz-González E, Estepa-Pedregosa L, Armenteros-López AI, Segado-Arenas A, Lubián-López SP (2020) Reproducibility and reference values of diaphragmatic shortening fraction for term and premature infants. Pediatr Pulmonol 55:1963–1968
Radicioni M, Rinaldi VE, Camerini PG, Salvatori C, Leonardi A, Bini V (2019) Right diaphragmatic peak motion velocities on pulsed wave tissue doppler imaging in neonates: method, reproducibility, and reference values. J Ultrasound Med 38:2695–2701
Soilemezi E, Savvidou S, Sotiriou P, Smyrniotis D, Tsagourias M, Matamis D (2020) Tissue doppler imaging of the diaphragm in healthy subjects and critically ill patients. Am J Respir Crit Care Med 202:1005–1012
Cammarota G, Boniolo E, Santangelo E, De Vita N, Verdina F, Crudo S, Sguazzotti I, Perucca R, Messina A, Zanoni M et al (2021) Diaphragmatic kinetics assessment by tissue doppler imaging and extubation outcome. Respir Care 66:983–993
Radicioni M, Leonardi A, Lanciotti L, Rinaldi VE, Bini V, Camerini PG (2021) How to improve CPAP failure prediction in preterm infants with RDS: a pilot study. Eur J Pediatr 180:709–716
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, Saugstad OD, Simeoni U, Speer CP, Vento M et al (2017) European consensus guidelines on the management of respiratory distress syndrome - 2016 update. Neonatology 111(2):107–125
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Lawrence Erlbaum Associates Inc., Hillsdale, NJ
Whitehead A, Julious S, Cooper C, Campbell MJ (2016) Estimating the sample size for a pilot randomised trial to minimise the overall trial sample size for the external pilot and main trial for a continuous outcome variable. Stat Methods Med Res 25(3):1057–1073
Knief U, Forstmeier W (2021) Violating the normality assumption may be the lesser of two evils. Behav Res Methods 53:2576–2590
Johnston R, Jones K, Manley D (2018) Confounding and collinearity in regression analysis: a cautionary tale and an alternative procedure, illustrated by studies of British voting behaviour. Qual Quant 52(4):1957–1976
Ali E, Abdel Wahed M, Alsalami Z, Abouseif H, Gottschalk T, Rabbani R, Zarychanski R, Abou-Setta AM (2016) New modalities to deliver surfactant in premature infants: a systematic review and meta-analysis. J Matern Fetal Neonatal Med 29:3519–3524
Niemarkt HJ, Kuypers E, Jellema R, Ophelders D, Hütten M, Nikiforou M, Kribs A, Kramer BW (2014) Effects of less-invasive surfactant administration on oxygenation, pulmonary surfactant distribution, and lung compliance in spontaneously breathing preterm lambs. Pediatr Res 76:166–170
Ricci F, Bresesti I, LaVerde PAM, Salomone F, Casiraghi C, Mersanne A, Storti M, Catozzi C, Tigli L, Zecchi R et al (2021) Surfactant lung delivery with LISA and INSURE in adult rabbits with respiratory distress. Pediatr Res 90:576–583
Laghi FA Jr, Saad M, Shaikh H (2021) Ultrasound and non-ultrasound imaging techniques in the assessment of diaphragmatic dysfunction. BMC Pulm Med 21:85
Supinski GS, Morris PE, Dhar S, Callahan LA (2018) Diaphragm dysfunction in critical illness. Chest 153:1040–1051
Singh Y, Tissot C, Fraga MV, Yousef N, Cortes RG, Lopez J, Sanchez-de-Toledo J, Brierley J, Colunga JM, Raffaj D et al (2020) International evidence-based guidelines on point of care ultrasound (POCUS) for critically ill neonates and children issued by the POCUS working group of the European society of paediatric and neonatal intensive care (ESPNIC). Crit Care 24:65
Herting E, Härtel C, Göpel W (2019) Less invasive surfactant administration (LISA): chances and limitations. Arch Dis Child Fetal Neonatal Ed 104:F655–F659
Roberts D, Brown J, Medley N, Dalziel SR (2020) Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Update in: Cochrane Database Syst Rev 25;12:CD004454
Klotz D, Porcaro U, Fleck T, Fuchs H (2017) European perspective on less invasive surfactant administration-a survey. Eur J Pediatr 176:147–154
Peterson J, den Boer MC, Roehr CC (2021) To sedate or not to sedate for less invasive surfactant administration: an ethical approach. Neonatology 118:639–646
Acknowledgements
We thank the neonatal intensive care unit staff for their valuable contribution.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Authors did not receive any funds for this study.
Author information
Authors and Affiliations
Contributions
All authors made a substantial contribution to the concept and design of the work. MR, SP and PC drafted the manuscript, designed the data collection instruments, performed exams, collected as well as interpreted data, and critically revised the manuscript for important intellectual content. AF helped in the collection and interpretation of data, gave administrative, technical, and material support, and critically revised the manuscript for important intellectual content. MR and VB conceptualized, designed, coordinated, and supervised the study, performed the data analysis and interpretation, and critically reviewed. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article to disclose.
Ethical approval
This study was conducted following the ethical standards of the Ethical Committee of the Health Authorities of the Umbria Region—CER [study code: MOV PG-04; CER registration number: 3800/19] and with the Helsinki Declaration of 1975.
Consent to participate
All patients’ parents/caregivers and healthcare professionals have signed a written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Radicioni, M., Pennoni, S., Fantauzzi, A. et al. Ultrasound evaluation of diaphragm kinetics after minimally invasive surfactant administration. J Ultrasound 27, 87–96 (2024). https://doi.org/10.1007/s40477-023-00820-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-023-00820-5