Abstract
Background
Obstetric ultrasound is a non-invasive imaging modality that uses sound waves to provide a real-time image of the foetus. Women’s knowledge of and attitudes toward ultrasound are suggested to influence their responses, and a variety of barriers also influence their practices.
Objectives
This study aimed to assess the knowledge, attitude, barriers, and associated factors of obstetric ultrasound among pregnant women in public hospitals in Addis Ababa.
Methods and materials
An institution-based cross-sectional study was conducted on 422 pregnant women from July to August 2021 using systematic random sampling. A structured questionnaire was employed, entered into Epi Info 7.2, and analysed in SPSS 23. Bivariate and multivariate logistic regression was used to identify associated factors.
Result
The proportion with good knowledge of obstetric ultrasound was 51.4%, and that with positive attitudes was 70.1%. Women with a degree and above (AOR 2.70; 95% CI 0.21–35.23), government employment (AOR 3.901; 95% CI 1.92–7.90), and previous ultrasound exposure (AOR 1.966; 95% CI 1.24–3.12) were significantly associated with knowledge. Government-employed women (AOR 6.83; 95% CI 2.43–19.18), women with 1000–5000birr in household income (AOR 5.31; 95% CI 2.01–14.03), and women with a history of births with congenital anomalies (AOR 21.07; 95% CI 2.09–21.21) were significantly associated with the attitude toward obstetric ultrasound. Participants in the study expressed a variety of barriers that influenced their practices; long waiting time was the most common (77.3%).
Conclusion
Pregnant women’s levels of knowledge and attitudes towards obstetric ultrasound were moderately good. However, there were a variety of barriers, including patient privacy, waiting time, handling, and side effects, that influenced the utilisation of ultrasound.
Similar content being viewed by others
Introduction
Obstetric ultrasound (US) is a non-invasive imaging modality that uses sound waves to scan a pregnant mother’s abdominal and pelvic cavity and provides parents with a real-time image of the foetus [1,2,3]. Obstetricians/clinicians can utilise this technology to assure their patients about the health of their foetus in utero. It is particularly useful in the management of high-risk pregnancies, while it is also used routinely in low-risk pregnancies for the diagnosis of congenital deformities in the foetus, the location of the placenta, and the assessment of the foetal biometry and well-being [4].
This examination is considered standard for prenatal diagnosis in many countries, and US imaging during pregnancy has become a common element of antenatal care (ANC) [5] and helps to improve the quality of ANC and pregnancy outcome [6,7,8]. However, it may pose risks to pregnant women, namely diagnostic errors and possible biological effects [9, 10].
All pregnant women should get at least one obstetric ultrasonography before the 24th week of gestation (GA) according to the World Health Organisation [7]. The International Federation of Gynaecology and Obstetrics (FIGO) also recommends that all pregnant women get two US screens during the first and second trimesters to lower the risk of unfavourable perinatal outcomes [11]. Ultrasound has nearly universal coverage in obstetrics in Western medicine, where routine screening has become an integral part of every pregnant woman’s antenatal examination [12, 13]. However, most women in Sub-Saharan Africa (SSA) still go through pregnancy without the benefit of even a single ultrasound examination [14, 15] and its utilisation is limited by a number of barriers [12].
It has been demonstrated that women’s knowledge of and attitude toward obstetric ultrasonography are crucial, as they affect their decision to undergo a test, and obstetric US has an impact on their mental health, particularly where it is newly used [16]. Pregnant women who are unaware of the benefits of obstetric US scanning are less likely to have it performed, and some may reject the diagnosis [5]. It is critical to assess their knowledge of obstetric US [1].
Only a few studies have been conducted in Ethiopia to analyse pregnant women’s knowledge of and attitude toward obstetric ultrasound and barriers to using ultrasound that pregnant women face. Accordingly, the purpose of this study was to analyse pregnant women’s knowledge, attitude, barriers, and associated factors regarding obstetric ultrasound in Ethiopian public hospitals.
Methods
Study area, design, and period
A prospective cross-sectional study was conducted in four public hospitals in Addis Ababa from July 20 to September 25, 2022. Ethiopia’s main and largest city, Addis Ababa, has 11 sub-cities. According to the 2007 census, the city’s population is estimated to be 2,739,551 people [17]. There are 14 public hospitals in Addis Ababa and roughly 40 non-profit institutions [18]. The Ministry of Health, university hospitals, military forces hospitals, and police hospitals are all affiliated with governmental hospitals.
Source population
All pregnant women receiving antenatal care in public hospitals in Addis Ababa.
Study population
During the data collection period, all pregnant women attending antenatal care services in Addis Ababa’s public hospitals.
Study participants
During the data collection period, all pregnant women who attended their regular antenatal care in Addis Ababa public hospitals and met the inclusion criteria were included.
Inclusion criteria
Pregnant women who presented for antenatal care within the study period and were willing to participate in the research were included in the study.
Exclusion criteria
Pregnant women with severe emergency conditions, pain and discomfort during their interview, unwillingness to cooperate, and an inability to communicate were not included in the study.
Sample size determination
The sample size was calculated based on the single population proportion formula, n = (z(α/2))2 p (1− p)/d2, with a 5% margin of error in a 95% confidence interval. Because no study had been undertaken in Ethiopia to investigate the barriers to using obstetric ultrasound, and because the proportion was close to 50%, the maximum sample size was employed. A 10% non-response rate was estimated, resulting in a final sample size of 422.
Sampling techniques and procedures
Using a simple random sample technique, four public hospitals that deliver ANC were chosen: Zewditu Memorial Hospital, Tirunesh Beijing Hospital, Gandhi Memorial Hospital, and Abebech Gobena MCH Hospital.
The sample was proportionally assigned to health facilities based on the average number of clients receiving ANC at each hospital, and the previous month’s performance report was used as a reference to estimate the client load (ANC load) in each hospital. Accordingly, 129 of the samples were allocated to Zewditu Memorial hospital, 115 were allocated to Abebech Gobena MCH Hospital, 79 were allocated to Gandhi Memorial Hospital, and 99 were allocated to Tirunesh Beijing Hospital. To select study participants, a systematic random sampling technique was applied, and the first study participant was chosen at random.
Study variables
Dependent variables: knowledge of, attitudes toward, and barriers to obstetric ultrasound.
Independent variables:
-
Socio-demographic factors: age, educational status, marital status, monthly income, husband’s educational status, respondent’s occupation.
-
Obstetric and other factors: parity, gestational age, previous obstetrics-related complications, number of ANC visits, time of ANC initiation.
Operational definitions
Knowledge of obstetric ultrasound
Respondents who answered at least 50% of the knowledge questions correctly were regarded to have good knowledge. Those who gave answers to fewer than 50% had a poor understanding of obstetric ultrasonography [5].
Attitude towards obstetric ultrasound
The attitude questions were obtained from responses on a Likert-type scale including strongly disagree, disagree, neither agree nor disagree/neutral, agree, and strongly agree. Finally, neutral, disagree, and strongly disagree were combined to form a negative attitude, while agree and strongly agree formed a positive attitude.
Respondents who answered ‘agree’ to more than 50% of the questions about their attitude are regarded to have a positive attitude toward obstetric ultrasound, whereas those who answered ‘agree’ to 50% or fewer of the questions are regarded as having a negative attitude toward prenatal ultrasound [5].
Barriers to accessing obstetric ultrasound
Those factors that prohibit pregnant women from utilising ultrasound during their pregnancy period.
Data collection methods and instruments
Structured questionnaires developed by the investigator and adapted from previous literature were used to collect data. After the study participants received antenatal care services, information about socio-demographic factors, obstetric history, knowledge, attitude toward obstetric ultrasound, and barriers to accessing ultrasound were obtained via face-to-face interviews.
One week before the actual data collection, 5% of the sample size in similar areas completed a pre-test of the questionnaire to ensure clarity and consistency of the questions. The appropriate corrections were then made based on data collector comments. The principal investigator reviewed all acquired data for completeness, accuracy, and consistency before communicating it to the data collectors the next day. The tools were initially created in English and then translated into Amharic.
Data analysis
Following data collection, the data were reviewed for completeness and consistency. Data were entered into Epi Info version 7.2.31 software after coding and confirming completeness and exported to the Statistical Program for Social Science (SPSS) version 26.0 once the question number in the questionnaire was recognised and the proper variable name was given by data coding. To determine the relationship between the dependent and independent variables, binary logistic regression was utilised.
All factors with p-values of less than 0.25 in the bivariate analysis were transferred to multivariable logistic regression analysis to find variables related to the dependent variable.
The significance link in multivariable logistic regressions was declared at p-value < 0.05 and reported using an adjusted odds ratio. A confidence level of 95% and p-value < 0.05 were considered significant. Model fitness was checked using the Hosmer–Lemeshow test. Multicollinearity was checked using the variance inflation factor (VIF) and the tolerance test. Finally, the results are presented in the form of text, tables, and graphs.
Results
Respondents’ socio-demographics
A total of 422 pregnant women participated in this study. The majority of study participants (203, 48.1%) were between the ages of 20 and 29. The majority (400, 94.8%) were married, and 168 (39.8%) had completed high school. Table 1 discusses the socio-demographic characteristics of the respondents in greater depth.
Obstetric history of the study participants
The majority (72.7%) of the respondents were multigravidae, and 115 (27.3%) were primigravidae. One hundred fifty-seven of the respondents had obtained information about ultrasound from their obstetricians/midwives (Table 2).
Pregnant women’s knowledge of obstetric ultrasound
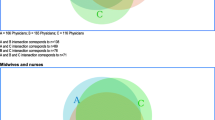
The study participants obtained information about obstetric ultrasound examination from different sources, and most of them obtained information from health professionals (Fig. 1).
An obstetric ultrasound scan can be performed between 4 and 6 months of pregnancy, according to the majority of participants (40.8%) (Fig. 2).
More than half (51.4%) of the respondents had good knowledge of obstetric ultrasound, while the remaining (48.6%) had poor knowledge of obstetric ultrasound. The most generally stated component of obstetric ultrasonography expertise by participants was the ability to confirm pregnancy, with around 403 (95.5%) women expressing it. The second most common reason for using ultrasound was to confirm the foetal position and cord and placental location, as stated by 379 women (89.8%). Only 96 respondents (22.7%) reported knowing how to determine the method of delivery during pregnancy (Table 3).
Attitude towards obstetric ultrasound
The majority of study participants 296 (70.1%) had a favourable opinion of obstetric ultrasound, while the remaining 126 (29.9%) had a negative attitude toward obstetric ultrasound. This demonstrates that more than a quarter of women have a negative attitude regarding obstetric ultrasound, which may result in refusal of the exam, thereby impacting the outcome of the pregnancy for both the baby and the mother.
The majority (82.2%) of the study participants did not agree that ultrasound can cause pain during the examination. More than 75% of the respondents considered obstetric ultrasound a safe examination during pregnancy, and few of them agreed that it caused deformity of the foetus. No pregnant women would terminate their pregnancy if the sex of the foetus were different from their preference; this may be because they had planned their pregnancies and were on regular pregnancy follow-up (Table 4).
Barriers to obstetric ultrasound utilisation
Participants in the study expressed a variety of issues that influenced their practice of obstetric ultrasound. Long waiting time for the examination was the most commonly stated barrier to utilising obstetric ultrasound according to the majority (77.3%) of the study participants. Being attended by a student was the second barrier to the use of ultrasound during the pregnancy period. According to this study, there was no culture that prohibited pregnant women from conducting ultrasound studies during their pregnancy (Fig. 3).
Factors associated with knowledge of obstetric ultrasound
In the bivariate logistic regression analysis, seven variables were associated with knowledge of obstetric ultrasound: age, educational level, parent/husband’s education, occupation, number of antenatal care visits, history of births with congenital anomalies, ultrasound exposure for a reason other than pregnancy, pregnancy experience, and knowledge of prenatal ultrasound. However, in the multivariate logistic regression analysis, women with a degree and above (AOR 2.70; 95% CI 0.21–35.23), government-employed women (AOR 3.901; 95% CI 1.92–7.90), and women with previous ultrasound exposure (AOR 1.966; 95% CI 1.24–3.12) were significantly associated with knowledge of obstetric ultrasound (Table 5).
Factors associated with attitude toward obstetric ultrasound
In the bivariate logistic regression analysis, occupation, monthly household income, time of ANC initiation, history of abortion, history of births with congenital anomalies, and ultrasound exposure for a reason other than pregnancy were associated with attitude toward obstetric ultrasound. However, in the multivariate logistic regression analysis, government employment (AOR 6.83; 95% CI 2.43–19.18), 1000–5000 in household income (AOR 5.31; 95% CI 2.01–14.03), and history of births with congenital anomalies (AOR 21.07; 95% CI 2.09–21.21) were significantly associated with pregnant women’s attitudes towards obstetric ultrasound, as shown in Table 6.
Discussion
Knowledge of obstetric ultrasound
In this study, 51.4% of study participants had good knowledge regarding the use of ultrasound during pregnancy. This finding was in line with a study conducted in Turkey, where half of pregnant women had a sufficient level of knowledge [21]. The finding of this study was higher than that of a study conducted in Gedeo zone, Ethiopia [2], and the study by Singh et al. in Lucknow, India [5]. This study’s finding is lower than that of a study in Nigeria [19]. This might be due to the pregnant women’s cultural background women regarding obstetric ultrasound use during pregnancy.
Most participants (95.5%) reported the importance of ultrasound in ANC was to confirm pregnancy. The awareness was least for estimating the expected date of delivery and predicting the way of delivery. This is contrary to the findings from a previous study [20], where estimating the date of delivery and managing ways of delivery were the most reported components.
Attitude towards prenatal ultrasound
The majority (296, 70.1%) of the study participants had a positive attitude towards obstetric ultrasound. This finding is in line with a study conducted in Nigeria (73.1%) [21]. This study’s finding was higher than that of a study conducted in Gedeo region [2] and a study conducted in Iran, where the majority of pregnant women had a negative attitude [10]. This may be because of socio-demographic factors.
In this study, 77% of pregnant women thought obstetric ultrasonography was safe. This finding is consistent with a study in Jeddah (78.9%) [10]. Similar research from Tanzania and India backed up the current finding [16, 22]. This may be because most of the study participants believed that the examination was safe for foetuses and women.
The majority of the women in this study (86.7%) agreed that obstetric ultrasonography was a vital pregnancy investigation. This finding is in line with studies conducted in Kano, Nigeria (93.8%) [23], and Puducherry, India (88%) [16]. The finding of this study is higher than that of a study conducted in Gedeo (71.8%) [2]. This may be because most of the respondents understood the benefit of the exam for the foetus and for women during pregnancy.
In this study, 7.8% of the study participants felt that ultrasound examination could cause cancer, which is lower than the finding in Mulago, Kampala (9%) [6]. The difference may be due to the time of the study period and the educational status of the pregnant women.
This study, consistent with research conducted in Gedeo, found that 17.3% of pregnant women believed that obstetric ultrasonography could cause congenital defects. This is higher than Jeddah’s finding (5.5%) [5] and lower than in Iran (53.3%) and Uganda (78%) [6, 24]. This may be a result of the study’s time and the sociodemographic characteristics of the participants.
Barriers towards utilisation of obstetric ultrasound
Generally, long waiting time for the examination and being attended by students were identified by the majority of the respondents as the main barriers to accessing ultrasound. This finding is higher than that of a study conducted in Kenya [25], where 49.5% of respondents mentioned the lack of skilled staff; this may be due to differences in the study areas.
According to the respondents in a study in the northern part of Nigeria, the distance to the service area, financial cost, and satisfaction with service were barriers to utilising obstetric ultrasound [26]. The findings are in line with this study, which identified privacy, service cost, and long distance to a health facility as important barriers to ultrasound service utilisation.
Factors associated with obstetric ultrasound
This finding shows that participants’ educational status, occupation, and exposure to ultrasound for reasons other than pregnancy were significantly associated with knowledge of obstetric ultrasound. It also showed that pregnant women with a history of births with congenital anomalies, occupation, and monthly household income were significantly associated with attitudes toward obstetric ultrasound.
Conclusions
In this study, 51.4% of pregnant women had knowledge of obstetric ultrasound. Educational status, occupation, and previous ultrasound exposure were significantly associated with knowledge of obstetric ultrasound. The majority (70.1%) of pregnant women had a positive attitude toward the use of obstetric ultrasound. Pregnant women’s attitudes toward obstetric ultrasound were significantly associated with women’s occupation, monthly household income, and history of births with congenital anomalies. Participants in the study expressed a variety of barriers that influenced their practice of obstetric ultrasound, with long waiting time for the examination being the most commonly stated.
Strengths and limitations
Strength of the study
This study addressed women from different hospitals in the study area and was the first research in this study area.
Limitations
Since the study design was an institution-based cross-sectional study, the study does not represent those women who had antenatal care visits at a private clinic. Moreover, the study shares the limitations of the cross-sectional study design.
Author contribution(s)
Zegeye Wubeshet: study conception, design, writing original draft preparation, analyze and interpreting the data. Almaz Gadisa: data curation, supervision, writing-reviewing and editing.
Availability of data and materials
All data included in this manuscript can be accessed from the corresponding author upon request through the email address.
Abbreviations
- ANC:
-
Antenatal care
- AOR:
-
Adjusted odd ratio
- CI:
-
Confidence interval
- COR:
-
Crude odd ratio
- ETB:
-
Ethiopian birr
- FIGO:
-
International Federation of Gynecology and Obstetrics
- GA:
-
Gestational age
- Sig:
-
Statistical significance
- SPSS:
-
Statistical package for social science
- SSA:
-
Sub-Saharan Africa
- US:
-
Ultrasound
- WHO:
-
World Health Organization
References
WHO. Recommendations on antenatal care for a positive pregnancy experience implementation considerations. Highlights and key messages from the World Health Organization’s 2016 global recommendations. Who [Internet]. 2018;1(November 2017):2013–6. http://apps.who.int/iris/bitstream/10665/259946/1/WHO-RHR-18.01-eng.pdf.
Molla W, Mengistu N, Wudneh A (2022) Pregnant women’s knowledge, attitude, and associated factors toward obstetric ultrasound in public hospitals, Ethiopia, 2021: multi-centered cross-sectional study. Womens Health 18:174550572210913
Nambile Cumber S, Nkeh NK (2017) Diagnostic medical ultrasound awareness among women in Cameroon. Int J Radiol Radiat Ther 4(4):397–398
Enakpene CA, Morhason-Bello IO, Marinho AO, Adedokun BO, Kalejaiye AO, Sogo K, Gbadamosi SA. BSA and OOE. Clients’ reasons for prenatal ultrasonography in Ibadan, South West of Nigeria [Internet]. BMC Women’s Health. 2009 [cited 2022 May 6]. https://www.ijars.net/article_fulltext.asp?issn=0973-709x&year=2016&month=October&volume=5&issue=4&page=-&id=2207.
Abduljabbar HS, Jabal NAB, Hussain FA, Alqabbaa RM, Marwani FA, Alghamdi SA et al (2020) Knowledge, attitudes and practice about obstetric ultrasonography among women attending a university hospital: a cross-sectional study. Open J Obstet Gynecol 10(12):1763–1775
Maniragena J, Murachi EJ. Knowledge, attitudes and practices of pregnant women towards obstetric ultrasound at Mulago Hospital: a cross-sectional survey. J Gynecol Reprod Med 2022;6(1).
Tunçalp Ӧ, Pena-Rosas JP, Lawrie T, Bucagu M, Oladapo OT, Portela A, Metin Gülmezoglu A (2017) WHO recommendations on antenatal care for a positive pregnancy experience-going beyond survival. BJOG 124(6):860-862. https://doi.org/10.1111/1471-0528.14599
Yetwale A, Kabeto T, Biyazin T, Fenta B (2022) Prenatal ultrasound utilization and its associated factors among pregnant women in Jimma town public health institutions. Ethiop Health Serv Res Manag Epidemiol 9:1–8
Abramowicz JS (2013) Benefits and risks of ultrasound in pregnancy. Semin Perinatol 37(5):295–300
Arvan M, Motlagh KM, Zare S, Gholami M (2019) Knowledge and attitude of pregnant women 15–49 years old about ultrasound examinations: a cross sectional study. J Res Med Dent Sci 7(2):177–181
Melamed N, Baschat A, Yinon Y, Athanasiadis A, Mecacci F, Figueras F, Berghella V, Nazareth A, Tahlak M, McIntyre HD, Da Silva Costa F, Kihara AB, Hadar E, McAuliffe F, Hanson M, Ma RC, Gooden R, Sheiner E, Kapur A, Divakar H, Ayres-de-Campos D, Hiersch L, Poon LC, Kingdom J, Romero R, Hod M (2021) FIGO (international Federation of Gynecology and obstetrics) initiative on fetal growth: best practice advice for screening, diagnosis, and management of fetal growth restriction. Int J Gynaecol Obstet. 152(1):3–57. https://doi.org/10.1002/ijgo.13522
Wanyonyi SZ, Mariara CM, Vinayak S, Stones W (2017) Opportunities and challenges in realizing universal access to obstetric ultrasound in Sub-Saharan Africa. Ultrasound Int Open 3(2):E52–E59
B P. Role of antenatal care in safe motherhood. JIndian Med Assoc. 1995. p. 53–52.
Sippel S, Muruganandan K, Levine A, Shah S (2011) Review article: use of ultrasound in the developing world. Int J Emerg Med 4(72):1–11
Ostensen H (2000) Developing countries. Ultrasound Med Biol 26(SUPPL. 1):159–161
Krishnamoorthy N, Kasinathan A (2016) Knowledge and attitude regarding obstetric ultrasound among pregnant women: a cross sectional study. Int J Reprod Contracept Obstet Gynecol 5(7):2192–2196
Service E statistical. Census 2007 [Internet]. 2007 [cited 2022 May 1]. https://www.statsethiopia.gov.et/census-2007-2/.
Ejegu T. Addis Ababa’s ailing state hospitals - Addis Standard [Internet]. Addis Standard. 2014 [cited 2022 May 1]. https://addisstandard.com/addis-ababas-ailing-state-hospitals-2/.
Sadiq Umar A, Raji M, Umar KA, Oche OM, Umar AS, Raji MO, et al. Knowledge of the use and indications for obstetric ultrasound scan among women attending a main Referral Hospital, Sokoto, Nigeria. Res Obstet Gynecol [Internet]. 2014;2013(5):55–62. https://www.researchgate.net/publication/259571365.
Maniragena J, Kasozi D, Mubuuke G, Murachi E (2022) Knowledge, attitudes and practices of pregnant women towards obstetric ultrasound at Mulago Hospital. J Gynecol Reprod Med 6(1):78–92
Ikeako L, Ezegwui H, Onwudiwe E, Enwereji J (2014) Attitude of expectant mothers on the use of ultrasound in pregnancy in a tertiary institution in South East of Nigeria. Ann Med Health Sci Res 4(6):949–953. https://doi.org/10.4103/2141-9248.144923
Firth ER, Mlay P, Walker R, Sill PR (2011) Pregnant women’s beliefs, expectations and experiences of antenatal ultrasound in Northern Tanzania. Afr J Reprod Health 15(June):91–107
Saleh, Idris G, Dare A, Yahuza M, Suwaid M, Idris S (2017) Awareness and perception of pregnant women about obstetrics ultrasound at Aminu Kano Teaching Hospital. Sahel Med J 20(1):38
Behzadmehr R, Keikhaie KR, Pour NS (2017) The Study of Pregnant Women’s Attitude toward Using Ultrasound in Pregnancy and its Diagnostic Value based on the Demographic Features in Amir-al-Momenin Hospital of Zabol, 2015–2016. Int J Adv Res Biol Sci 4:58–63
Matiang’i M, Joosse K, Ngunju P, Kiilu C, Harkx R, Hangelbroek M et al (2021) Barriers and enablers that influence utilization of ultrasound screening services among antenatal women in Kajiado and Kisii counties Kenya. Open J Clin Diagn 11(01):1–17
Ohagwu CC, Abu PO, Odo MC, Chiegwu HU (2010) Maternal perception of barriers to utilization of prenatal ultrasound in prenatal care in the northern part of Nigeria. Clin Mother Child Health 7(June):1–5
Acknowledgements
We are thankful to the study participants for giving their time to participate in this study. We would also want to thank the data collectors for their dedication and patience during the data collection period.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval and consent to participate
Ethical approval and clearance were obtained from Addis Ababa research and emergency management directorate Institutional Review Board. Permission was also obtained from the concerned bodies in the study area. Prior to data collection, written informed consent were obtained from each study participant and for those with no formal education the informed consent were obtained from legally authorized representative. Confidentiality of the information was assured and privacy of the respondents was maintained. The study was also carried out following relevant guidelines and regulations according to the Helsinki declaration. To prevent covid-19 transmissions while delivering questioner face masks also prepared.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Haile, Z.W., Gurmu, A.G. Knowledge, attitude, barriers, and associated factors of obstetric ultrasound among pregnant women in public hospitals, Ethiopia, 2022: a cross-sectional study. J Ultrasound 27, 31–40 (2024). https://doi.org/10.1007/s40477-023-00783-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-023-00783-7