Abstract
Purpose
In a poor resource country where screening for adverse pregnancy outcomes using maternal biomarkers seems unattainable, there is a need to search for credible alternatives. This study is, therefore, aimed at determining the sensitivity of uterine artery Doppler pulsatility index (UtAD-PI) in predicting pregnancy outcomes in the first and second trimesters and to establish any statistical difference in mean UtAD-PI in first and second trimesters screening of women with normal and abnormal pregnancy outcomes respectively.
Methods
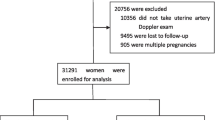
This clinical-based, longitudinal, and unpaired cohort study involved 500 pregnant women, who were screened for adverse outcomes using UtAD-PI and delivered in the hospital. These were divided into two groups, each having a training set and a test set. The training set was used to generate the receiver operator characteristic curve and cut-off point while the test set was used to test for sensitivity and specificity of the Ut-ADI in each trimester.
Results
The sensitivity and specificity of UtAD-PI in first-trimester screening are 97% and 76.5% while second-trimester gave sensitivity and specificity of 57.5% and 63.3% respectively. The uterine artery Doppler pulsatility index shows statistically significant differences between normal pregnancy and pregnancy with adverse outcomes (p-value = 0.000).
Conclusion
The uterine artery Doppler pulsatility index is a good screening tool for adverse pregnancy outcomes. First-trimester screening of patients for adverse outcomes is more sensitive than the second-trimester screening using UtAD-PI. There is also a statistically significant difference between mean UtAD-PI between normal pregnancy and pregnancy with adverse pregnancy outcomes.



Similar content being viewed by others
Data availability
Data are available with the corresponding author and can be made available when needed.
References
WHO (2021) New global targets to prevent maternal death. https://www.who.int/news/item/05-10-2021-new-global-targets-to-prevent-maternal-deaths. Accessed 5 Oct 2021
Central Intelligent Agency (CIA) (2021) Country Comparisons- Maternal mortality ratio. https://www.cia.gov/the-world-factbook/field/maternal-mortality-ratio/country-comparison. Accessed 30 Dec 2021
Ope BW (2020) Reducing maternal mortality in Nigeria: addressing maternal health services’ perception and experience. J Glob Health Rep 4:e20200028. https://doi.org/10.29392/001c.12733
UNICEF Nigeria (2020) Hidden tragedy: Nigeria accounts for one of the highest stillbirth rates in Africa. https://www.unicef.org/nigeria/stories/hidden-tragedy-nigeria-accounts-one-highest-stillbirth-rates-africa. Accessed 23 Nov 2020
WHO (2019) Maternal mortality. https://www.who.int/news-room/fact-sheets/detail/maternal-mortality. Accessed 19 Sep 2019
WHO (2021) Maternal health. https://www.who.int/health-topics/maternal-health#tab=tab_1. Accessed 5 Oct 2021
Packer AS (2005) Biochemical markers and physiological parameters as indices for identifying patients at risk of developing pre-eclampsia. J Hypertens 23(1):45–46
Magnussen EB, Vatten LJ, Lund-Nilsen TI, Salvesen KA, Smith GD, Romundstad PR (2007) Prepregnancy cardiovascular risk factors as predictors of pre-eclampsia: population-based cohort study. Br Medl J 335(7627):978–981
Papageorghiou AT, Yu CK, Erasmus IE, Cuckle HS, Nicolaides KH (2005) Assessment of risk for the development of pre-eclampsia by maternal characteristics and uterine artery Doppler. BJOG An Intl J Obstet Gynaecol 112(6):703–709
Al-Rubaie ZT, Hudson HM, Jenkins G, Mahmoud I, Ray JG, Askie LM et al (2020) Prediction of pre-eclampsia in nulliparous women using routinely collected maternal characteristics: model development and validation study. BMC Pregnancy Childbirth 20(1):1–14
Ilekis JV, Tsilou E, Fisher S, Abrahams VM, Soares MJ, Cross JC et al (2016) Placental origins of adverse pregnancy outcomes: potential molecular targets: an Executive Workshop Summary of the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Am J Obstet Gynecol 215(1):S1–S46
Hazra KK, Dash KK, Chaudhuri A, Ghosh MK, Banerjee D, Guha S (2013) A prospective study of Doppler velocimetry in pregnancy-induced Hypertension in a Rural Population of a Developing Country. J Basic Clin Reprode Scis 2(2):127–131
Ochi H, Suginami H, Matsubara K, Taniguchi H, Yano J, Matsuura S (1995) Micro-bead embolization of uterine spiral arteries and changes in uterine arterial flow velocity waveforms in the pregnant ewe. Ultrasound Obstet Gynecol 1995(6):272–276
Lakshmy SR, Praveenkumar M, Shobana U, Thasleem Z (2018) Uterine artery Doppler: changing concepts in prediction and prevention of PE and FGR. J Fetal Med 5(2):93–105
Afrakhteh M, Moeini A, Taheri MS, Haghighatkhah HR, Fakhri M, Masoom N (2014) Uterine Doppler velocimetry of the uterine arteries in the second and third trimesters for the prediction of gestational outcome. Rev Bras Ginecol Obstet 36:35–39
Awuah SP, Okai I, Ntim EA, Bedu-Addo K (2020) Prevalence, placenta development, and perinatal outcomes of women with hypertensive disorders of pregnancy at Komfo Anokye Teaching Hospital. PLoS ONE 15(10):e0233817
Oloyede OA, Iketubosin F (2013) Uterine artery Doppler study in the second trimester. Pan Afr Medl Jl 15:87
Li J, Fine J (2004) On sample size for sensitivity and specificity in prospective diagnostic accuracy studies. Stat Med 23(16):2537–2550
Ebrashy A, Ibrahim M, Marzook A, Yousef D (2005) The usefulness of aspirin therapy in high-risk pregnant women with abnormal uterine artery Doppler ultrasound at 14–16 weeks pregnancy: a randomized controlled clinical trial. Croat Med J 46(5):826–831
Groom KM, North RA, Stone PR, Chan EH, Taylor RS, Dekker GA et al (2009) Patterns of change in uterine artery Doppler studies between 20 and 24 weeks of gestation and pregnancy outcomes. Obstet Gynecol 113(2):332–338
Marangoni F, Cetin I, Verduci E, Canzone G, Giovannini M, Scollo P, Corsello G et al (2016) Maternal diet and nutrient requirement in pregnancy and breastfeeding. An Italian Consensus Document. Nutrient 8(10):629
Wardinger JE, Ambati S (2021) Placental Insufficiency. StatPearls. [Internet]
Girum T, Wasie A (2017) Correlates of maternal mortality in developing countries: an ecological study in 82 countries. Matern Health Neonatal Perinatol 3(1):1–6
Rodríguez M, Couve-Pérez C, San Martín S, Martínez F, Lozano C, Sepúlveda-Martínez A (2018) Perinatal outcome and placental apoptosis in patients with late-onset pre-eclampsia and abnormal uterine artery Doppler at diagnosis. Ultrasound Obstet Gynecol 51(6):775–782
Mandrekar JN (2010) Receiver operating characteristic curve in diagnostic test assessment. J Thorac Oncol 5(9):1315–1316
Velauthar L, Plana MN, Kalidindi M, Zamora J, Thilaganathan B, Illanes SE et al (2014) First-trimester uterine artery Doppler and adverse pregnancy outcome: a meta-analysis involving 55 974 women. Ultrasound Obstet Gynecol 43(5):500–507
Pongrojpaw D, Chanthasenanont A, Nanthakomon T (2010) Second-trimester uterine artery Doppler screening in the prediction of adverse pregnancy outcomes in high-risk women. J Med Assoc Thai 93(7):S127–S130
Mariana N, Chowdhury T, Choudhury T (2020) Uterine artery Doppler screening in 2nd trimester of pregnancy for prediction of pre-eclampsia and fetal growth restriction. J Adv Med Med Res 20:7–22
Barati M, Shahbazian N, Ahmadi L, Masihi S (2014) Diagnostic evaluation of uterine artery Doppler sonography for the prediction of adverse pregnancy outcomes. J Res Med Sci 19(6):515
Cavoretto PI, Salmeri N, Candiani M, Farina A (2022) Reference ranges of uterine arteries pulsatility index from first to third trimester based on serial Doppler measurements: longitudinal cohort study. Ultrasound Obstet Gynecol. https://doi.org/10.1002/uog.26092
Funding
The authors declared that no funds, grants, or other support were received from any agency as regards this study.
Author information
Authors and Affiliations
Contributions
Each of us participated actively in the course of this study. EOA and FUI designed the study. EOA performed the ultrasound scanning. JAA drafted the manuscript while A.C. Anakwue revised the manuscript for intellectual content. ACA and EOA analyzed the data.
Corresponding author
Ethics declarations
Competing interest
The authors declare no conflict of interest.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Enugu state ministry of Health on 11/10/2018 with the number MH/MSD/REC18/037.
Consent to participate
Written informed consent was obtained from all individual participants included in the study.
Consent to publish
Not applicable here as no participant personal information was published here.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Abonyi, E.O., Idigo, F.U., Anakwue, AM.C. et al. Sensitivity of uterine artery Doppler pulsatility index in screening for adverse pregnancy outcome in first and second trimesters. J Ultrasound 26, 517–523 (2023). https://doi.org/10.1007/s40477-022-00766-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-022-00766-0