Abstract
Background
Renal transplant recipients (RTRs) remain at an increased risk of fatal and non-fatal cardiovascular (CV) events compared to the general population. Death is most commonly due to cardiovascular diseases.
Purpose
The primary outcome of this work is the determination of adverse CV events and their risk factors in the RTR population and their effect on mortality.
Methods
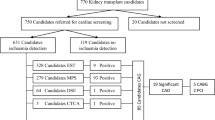
A retrospective analysis has been performed on data from 500 patients at the Cairo Kidney Center, Cairo, Egypt, who underwent kidney transplantation with a graft from a living donor. Data was collected for RTR starting from 1992 till 2014.
Results
The mean age of patients was 41.90 ± 9.67 years. 63.8% of them were males. CV complications (stable angina pectoris, acute coronary syndrome, new left ventricular hypertrophy (LVH), positive myocardial perfusion scan, elevated cardiac enzymes, and invasive coronary angiography) occurred in (22.6%, 2.4%, 49.8%, 13.6%, 1.8%, and 7.6%) of patients, respectively. Other CV complications occurred in (24.0%, 11.2%, and 40.8%), including Congestive Heart Failure (CHF), cardiomyopathy, and arrhythmias.The main causes of mortality were CV diseases, infections, cancer, surgical complications, and liver disease (19.0%, 13.4%, 1.6%, 1.4%, and 1.2%), respectively.
Conclusion
RTR are at an extremely high risk of adverse CV events. CV complications (CHF, ischemic heart diseases, LVH, and arrhythmias) are the leading causes of death in RTR.

Similar content being viewed by others
References
Abecassis M, Bartlett ST. Kidney transplantation as primary therapy for end-stage renal disease: a National Kidney Foundation/Kidney Disease Outcomes Quality Initiative (NKF/KDOQITM) conference. Clin J Am Soc Nephrol. 2008;3(2):471–80. https://doi.org/10.2215/CJN.05021107.
Lentine KL, Rocca Rey LA, Kolli S, et al. Variations in the risk for cerebrovascular events after kidney transplant compared with experience on the waiting list and after graft failure. Clin J Am SocNephrol. 2008;3:1090.
Yeo FE, Villines TC, Bucci JR, et al. Cardiovascular risk in stage 4 and 5nephropathy. Adv Chronic Kidney Dis. 2004;11:116.
Abbott KC, Reynolds JC, Taylor AJ, et al. Hospitalized atrial fibrillation after renal transplantation in the United States. Am J Transplant. 2003;3:471–6.
Ojo AO. Cardiovascular complications after renal transplantation and their prevention. Transplantation. 2006;82:603.
Meier-Kriesche HU, Schold JD, Srinivas TR, et al. Kidney transplantation halts cardiovascular disease progression in patients with end-stage renal disease. Am J Transplant. 2004;4:1662.
Mccullough PA, Bouchard J, Waikar SS et al. Implementation of novel biomarkers in the diagnosis, prognosis, and management of acute kidney injury: executive summary from the tenth consensus conference of the Acute Dialysis Quality Initiative (ADQI). ADQI Consensus on AKI Biomarkers and Cardiorenal Syndromes. Karger Publishers. Contrib Nephrol. 2013;182:5–12.https://doi.org/10.1159/000349962
Matas AJ, Smith JM, Skeans MA, et al. OPTN/SRTR 2013 Annual Data Report: kidney. Am J Transplant. 2015;15(Suppl 2):1–34.
Kramer A, Pippias M, Noordzij M, et al. The european renal association–european dialysis and transplant association (ERA-EDTA) registry annual report 2015: a summary. Clinicalkidney journal. 2018;11:108–22.
Fernandez-Prado R, Fernandez-Fernandez B, Ortiz A. Women and renal replacement therapy in Europe: lower incidence, equal access to transplantation, longer survival than men. Clin Kidney J. 2018;11:1–6.
El-Ballat M, El-Sayed MA, Emam HK. Epidemiology of end stage renal disease patients on regular hemodialysis in El-Beheira governorate, Egypt. Egyptian J Hos Med. 2019;76:3618–25.
Devine PA, Courtney AE, Maxwell AP. Cardiovascular risk in renal transplant recipients. J Nephrol. 2019;32:389–99.
Kasiske BL, Klinger D. Cigarette smoking in renal transplant recipients. J Am SocNephrol. 2000;11:753–9.
Glicklich D, Vohra P. Cardiovascular risk assessment before and after kidney transplantation. Cardiol Rev. 2014;22:153–62.
Crosland W, Aggarwal H, Farag A, et al. The effect of renal transplantation on left ventricular function, electrocardiography, and mechanical synchrony by gated myocardial perfusion imaging. J Nucl Cardiol. 2019;26:1962–70.
Slubowska K, Lichodziejewska B, Pruszczyk P, Szmidt J, Durlik M. Left ventricular hypertrophy in renal transplant recipients in the first year after transplantation. Transplant Proc. 2014;46(8):2719–23. https://doi.org/10.1016/j.transproceed.2014.08.019.
Alhaj E, Alhaj N, Rahman I, et al. Uremic cardiomyopathy: an underdiagnosed disease. Congest Heart Fail. 2013;19:E40–5.
Murkamilov IT, Sabirov IS, Fomin VV, et al. Myocardial infarction in hemodialysis patients. Int Heart Vasc Dis J. 2021;9(29):27–32.
Jardine AG, Fellström B, Logan JO, et al. Cardiovascular risk and renal transplantation: post hoc analyses of the Assessment of Lescol in Renal Transplantation (ALERT) Study. Am J Kidney Dis. 2005;46:529–36.
Israni A, Snyder J, Skeans M, et al. Predicting coronary heart disease after kidney transplantation: Patient Outcomes in Renal Transplantation (PORT) Study. Am J Transplant. 2010;10:338–53.
Didier R, Yao H, Legendre M, et al. Myocardial Infarction after Kidney Transplantation: A Risk and Specific Profile Analysis from a Nationwide French Medical Information Database. J Clin Med. 2020;9:3356.
Rigatto C, Parfrey P, Foley R, et al. Congestive heart failure in renal transplant recipients: risk factors, outcomes, and relationship with ischemic heart disease. J Am Soc Nephrol. 2002;13:1084–90.
Abbott KC, Hypolite IO, Hshieh P, et al. Hospitalized congestive heart failure after renal transplantation in the United States. Ann Epidemiol. 2002;12:115–22.
Lentine KL, Costa SP, Weir MR, et al. Cardiac disease evaluation and management among kidney and liver transplantation candidates: a scientific statement from the American Heart Association and the American College of Cardiology Foundation. J Am Coll Cardiol. 2012;60:434–80.
– Małyszko J, Musiałowska D, Tomaszuk-Kazberuk A et al. Cardiovascular disease in patients qualified to kidney transplantation. Borgis - Postępy Nauk Medycznych 9/2016; 672–676
Delville M, Sabbah L, Girard D, et al. Prevalence and predictors of early cardiovascular events after kidney transplantation: evaluation of pre-transplant cardiovascular work-up. PLoS ONE. 2015;10:e0131237.
Abedini S, Holme I, Fellström B, et al. Cerebrovascular events in renal transplant recipients. Transplantation. 2009;87:112–7.
Aull-Watschinger S, Konstantin H, Demetriou D, et al. Pre-transplant predictors of cerebrovascular events after kidney transplantation. Nephrol Dial Transplant. 2008;23:1429–35.
Davidson J, Wilkinson A, Dantal J, et al. New-onsetdiabetesafter transplantation: 2003 international consensus GUIDELINES1. Transplantation. 2003;75:SS3–24.
Choudhury PS, Mukhopadhyay P, Roychowdhary A, et al. Prevalence and Predictors of “New-onset Diabetes after Transplantation” (NODAT) in Renal Transplant Recipients: An Observational Study. Indian J Endocrinol Metab. 2019;23:273–7.
Tsampalieros A, Knoll GA. Evaluation and management of proteinuria after kidney transplantation. Transplantation. 2015;99:2049–60.
Borrego Hinojosa J, GentilGovantes MA, Cabello Díaz M, et al. Progression of urinary protein excretion after kidney transplantation: A marker for poor long-term prognosis. Nefrologia. 2015;35:374–84.
Vella J. Kidney transplantation in adults: Patient survival after kidney transplantation. Literature review current through: Mar 2023. 2019.
Howard RJ, Patton PR, Reed AI, et al. The changing causes of graft loss and death after kidney transplantation. Transplantation. 2002;73:1923–8.
Awan AA, Niu J, Pan JS, et al. Trends in the causes of death among kidney transplant recipients in the United States (1996–2014). Am J Nephrol. 2018;48:472–81.
Siedlecki A, Foushee M, Curtis JJ, et al. The impact of left ventricular systolic dysfunction on survival after renal transplantation. Transplantation. 2007;84:1610.
Acknowledgements
We are grateful for the word clerk team who present a lot of help in bringing and collecting all data from the filing system and old files.
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Soliman, M., Eskander, A., Effat, H. et al. Adverse Cardiovascular Events in Post-Renal Transplant Patients, a Retrospective Study of Five Hundred Cases Over Twenty-Two Years. Curr Transpl Rep 10, 89–99 (2023). https://doi.org/10.1007/s40472-023-00399-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40472-023-00399-0