Abstract
Aim
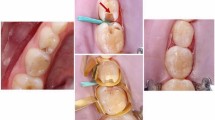
Aim of this randomised clinical trial was to compare the outcome of direct pulp capping (DPC) versus pulpotomy, both with MTA, for carious primary molars.
Methods
Healthy, cooperative children aged 3–9 years with at least one deep carious primary molar requiring vital pulp therapy were included. Data on the primary outcome (all-cause failure) and secondary outcomes (clinical or radiographic failure) were collected blindly semi-annually for a minimum of 1 year up to 3 years and analysed with survival analysis and generalised linear regression at alpha = 5%.
Results
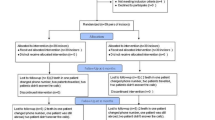
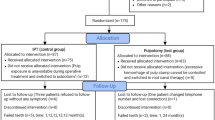
A total of 74 children were randomly allocated on 1:1 basis to DPC (35 children; 40 teeth) or pulpotomy (39 children; 57 teeth). Survival from all-cause failure was 79.7% [95% confidence interval (CI) 69.3–86.9%] at 12 months and 66.0% (95% CI 53.4–76.0%) at 24 months which remained stable up to 36 months, with no differences between groups (P > 0.05). No significant difference was found in the survival rate of the two groups for all-cause [hazard ratio (HR) = 0.95; 95% CI 0.45–2.01; P = 0.88], clinical (HR = 0.74; 95% CI 0.0.19–2.92; P = 0.66), or radiographic failure (HR = 0.80; 95% CI 0.0.36–1.82; P = 0.60) throughout the 3-year follow-up. Regression analysis indicated that needing a second attempt for haemorrhage control was associated with higher clinical failure rate. All-case failure was significantly different for class II versus occlusal cavities and in the latter cavities pulpotomy performed better (P < 0.001).
Conclusion
The results of the current trial indicate that both DPC and pulpotomy can be reliable options for the treatment of deep carious primary molars in cooperative children, in carefully selected cases.


Similar content being viewed by others
References
Agamy HA, Bakry NS, Mounir MMF, Avery DR. Comparison of mineral trioxide aggregate and formocresol as pulp-capping agents in pulpotomized primary teeth. Pediatr Dent. 2004;26:302–9.
Agary S, Shirvani A, Fazlyab M. MTA and ferric sulfate in pulpotomy outcomes of primary molars: a systematic review and meta-analysis. J Clin Pediatr Dent. 2014;39:1–8.
American Academy of Pediatric Dentistry. Guideline on pulp therapy for primary and immature permanent teeth, Revised 2014. Pediatric Dentistry. Reference Manual 2014–2015; p. 242–50. http://www.aapd.org/media/policies_guidelines/g_pulp.pdf. Accessed 21 Sept 2018
Asl Aminabadi N, Maljaei E, Erfanparast L, et al. Simvastatin versus calcium hydroxide direct pulp capping of human primary molars: a randomized clinical trial. J Dent Res Dent Clin Dent Prospects. 2013;7:8–14.
Bani M, Aktas N, Cinar C, Odabas ME. The clinical and radiographic success of primary molar pulpotomy using biodentine and mineral trioxide aggregate: a 24-month randomized clinical trial. Pediatr Dent. 2017;39:284–8.
Caicedo R, Abbott PV, Alongi DJ, Alarcon MY. Clinical, radiographic and histological analysis of the effects of mineral trioxide aggregate used in direct pulp capping and pulpotomies of primary teeth. Aust Dent J. 2006;51:297–305.
Cardoso-Silva C, Barberia E, Maroto M, Garcia-Godoy F. Clinical study of mineral trioxide aggregate in primary molars. Comparison between grey and white MTA—a long term follow-up (84 months). J Dent. 2011;39:187–93.
Coll JA, Seale NS, Vargas K, et al. Primary tooth vital pulp therapy: a systematic review and meta-analysis. Pediatr Dent. 2017;39:16–23.
Demir T, Cehreli ZC. Clinical and radiographic evaluation of adhesive pulp capping in primary molars following hemostasis with 1.25% sodium hypochlorite: 2-year results. Am J Dent. 2007;20:182–8.
Dhar V, Marghalani AA, Crystal YO, et al. Use of vital pulp therapies in primary teeth with deep caries lesions. Pediatr Dent. 2017;39:E146–59.
Dimitraki D, Papageorgiou SN, Kotsanos N. Direct pulp capping versus pulpotomy with MTA for carious primary molars: a 3-year randomised clinical trial. Zenodo. 2018. https://doi.org/10.5281/zenodo.1401124.
Duston B, Coll JA. A survey of primary tooth pulp therapy as taught in US dental schools and practiced by diplomats of an American board of pediatric dentistry. Pediatr Dent. 2008;30:42–8.
Dye B, Thornton-Evans G, Li X, Iafolla T. Dental caries and sealant prevalence in children and adolescents in the United States, 2011–2012. NCHS Data Brief. 2015;191:1–8.
Fallahinejad Ghajari M, Jeddi TA, Iri S, Asgary S. Direct pulp-capping with calcium enriched mixture in primary molar teeth: a randomized clinical trial. Iran Endod J. 2010;5:27–30.
Fallahinejad Ghajari M, Jeddi TA, Iri S, Asgary S. Treatment outcomes of primary molars direct pulp capping after 20 months: a randomized controlled trial. Iran Endod J. 2013;8:149–52.
Farooq NS, Coll JA, Kuwabara A, Shelton P. Success rates of formocresol pulpotomy and indirect pulp therapy in the treatment of deep dentinal caries in primary teeth. Pediatr Dent. 2000;22:278–86.
Fuks AB. Current concepts in vital pulp therapy. Eur J Paediatr Dent. 2002;2:115–20.
Fuks AB. Vital pulp therapy with new materials for primary teeth: new directions and treatment perspectives. J Endod. 2008;34:18–24.
Fuks AB, Papagiannoulis L. Pulpotomy in primary teeth: review of the literature according to standardized criteria. Eur Arch Paediatr Dent. 2006;7:64–71.
Garrocho-Rangel A, Flores H, Silva-Herzog D, et al. Efficacy of EMD versus calcium hydroxide in direct pulp capping of primary molars: a randomized controlled clinical trial. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107:733–8.
Haghgoo R, Naderi NJ. Comparison of calcium hydroxide and bioactive glass after direct pulp capping in primary teeth. J Dent Tehran Tehran Univ. 2007;4:155–9.
Haghgoo R, Asgary S, Abbas FM, Hedeshi RM. Nano-hydroxyapatite and calcium-enriched mixture for pulp capping of sound primary teeth: a randomized clinical trial. Iran Endod J. 2015;10:107–11.
Huth KC, Paschos E, Hajek-Al-Khatar N, et al. Effectiveness of 4 pulpotomy techniques—randomized controlled trial. J Dent Res. 2005;84:1144–8.
Innes N. Better outcomes in pulpotomies on primary molars with MTA. Evid Based Dent. 2007;8:11–2.
Kassa D, Day P, High A, Duggal M. Histological comparison of pulpal inflammation in primary teeth with occlusal or proximal caries. Int J Paediatr Dent. 2009;19:26–33.
Kotsanos N, Arapostathis KN, Arhakis A, Menexes G. Direct pulp capping of carious primary molars. A specialty practice based study. J Clin Pediatr Dent. 2014;38:307–12.
Malekafzali B, Shekarchi F, Asgary S. Treatment outcomes of pulpotomy in primary molars using two endodontic biomaterials. A 2-year randomised clinical trial. Eur J Paediatr Dent. 2011;12:189–93.
Ng FK, Messer LB. Mineral trioxide aggregate as a pulpotomy medicament: a narrative review. Eur Arch Paediatr Dent. 2008;9:4–11.
Noorollahian H. Comparison of mineral trioxide aggregate and formocresol as pulp medicaments for pulpotomies in primary molars. Br Dent J. 2008;204:E20.
Peng L, Ye L, Tan H, Zhou X. Evaluation of the formocresol versus mineral trioxide aggregate primary molar pulpotomy: a meta-analysis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;102:e40– e44.
Rodd HD, Waterhouse PJ, Fuks AB, Fayle SA, Moffat MA. Pulp therapy for primary molars. Int J Paediatr Dent. 2006;16(Suppl 1):15–23.
Rönnerman A. The effect of early loss of primary molars on tooth eruption and space conditions. A longitudinal study. Acta Odontol Scand. 1977;35:229–39.
Schwendicke F, Brouwer F, Schwendicke A, Paris S. Different materials for direct pulp capping: systematic review and meta-analysis and trial sequential analysis. Clin Oral Investig. 2016;20:1121–32.
Shayegan A, Atash R, Petein M, Abbeele AV. Nanohydroxyapatite used as a pulpotomy and direct pulp capping agent in primary pig teeth. J Dent Child (Chic). 2010;77:77–83.
Smaïl-Faugeron V, Glenny AM, Courson F, Durieux P, Muller-Bolla M, Fron Chabouis H. Pulp treatment for extensive decay in primary teeth. Cochrane Database Syst Rev. 2018;5:CD003220.
Sonmez D, Sari S, Cetinbas T. A comparison of four pulpotomy techniques in primary molars: a long-term follow-up. J Endod. 2008;34:950–5.
Subramaniam P, Konde S, Mathew S, Sugnami S. Mineral trioxide aggregate as pulp capping agent for primary teeth pulpotomy: 2 year follow up study. J Clin Pediatr Dent. 2009;33:311–4.
Sujlana A, Pannu PK. Direct pulp capping: a treatment option in primary teeth? Pediatr Dent J. 2017;27:1–7.
Tuna D, Olmez A. Clinical long-term evaluation of MTA as a direct pulp capping material in primary teeth. Int Endod J. 2008;41:273–8.
Tziafas D, Smith AJ, Lesot H. Designing new treatment strategies in vital pulp therapy. J Dent. 2000;28:77–92.
Ulusoy AT, Bayrak S, Bodrumlu EH. Clinical and radiological evaluation of calcium sulfate as direct pulp capping material in primary teeth. Eur J Paediatr Dent. 2014;15:127–31.
Vostatek S, Kanellis M, Weber-Gasparoni K, Gregorsok RL. Sodium hypochlorite pulpotomies in primary teeth: a retrospective assessment. Pediatr Dent. 2011;33:329–32.
Acknowledgements
The authors would like to thank all postgraduate residents and clinic supervisors for their assistance in this study. The MTA used in the study procedures was provided by Medcem GmbH, Weinfelden, Switzerland. Preliminary results of this study were published in the 13th EAPD Congress in Belgrade and were awarded with the “Young Scientist Research Award”.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Ethics Committee of the Aristotle University of Thessaloniki, Dental School (307/July 6, 2012).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dimitraki, D., Papageorgiou, S.N. & Kotsanos, N. Direct pulp capping versus pulpotomy with MTA for carious primary molars: a randomised clinical trial. Eur Arch Paediatr Dent 20, 431–440 (2019). https://doi.org/10.1007/s40368-019-00419-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-019-00419-7