Abstract
Background
Physical activity (PA) interventions in people with spinal cord injury (SCI) have been limited by a shortage of (1) evidence for sufficient increases in unsupervised PA to improve aerobic fitness and (2) stakeholder involvement in intervention design.
Objectives
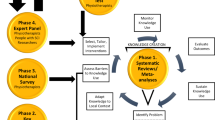
This study examined the effects of a theory-based PA intervention, developed in collaboration with nearly 300 stakeholders, on PA levels, aerobic fitness, and psychosocial predictors of PA among individuals with SCI.
Methods
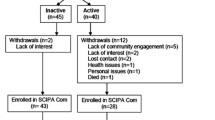
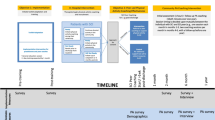
A randomized controlled trial (RCT) was conducted with 28 men and women with chronic SCI (age 45.0 ± 11.5 years, years post-injury 16.4 ± 12.4). Participants randomized to the intervention group (n = 14) received an introductory personal training session followed by eight weekly 15-min PA behavioral coaching sessions per week. PA was assessed using self-report and accelerometers. Aerobic fitness and psychosocial predictors of exercise were evaluated using an incremental exercise test and survey methods, respectively.
Results
At post-intervention, controlling for baseline, the intervention group showed fivefold greater self-reported moderate to vigorous physical activity [mean difference 247.9 min/day; 95% confidence interval (CI) 92.8–403.1; p = 0.026, d = 1.04], 17% greater accelerometer-measured PA (mean difference 3.9 × 105 vector magnitude counts; 95% CI 1.1 × 104–7.7 × 105; p = 0.014, d = 0.31), and 19% higher peak oxygen uptake (VO2Peak; mean difference 0.23 L/min; 95% CI 0.12–0.33; p < 0.001, d = 0.54) compared with the control group. Mean values of psychosocial predictors of PA were also significantly improved in the intervention group compared with controls.
Conclusion
To our knowledge, this co-created behavioral intervention produced the largest effect size to date for change in self-reported PA in an RCT involving people with physical disability. This is also the first RCT in people with SCI to demonstrate that a behavioral intervention can sufficiently increase unsupervised PA to improve aerobic fitness.
Trial Registration
ClinicalTrials.gov, NCT03111030, 12 April 2017, https://clinicaltrials.gov/ct2/show/NCT03111030?term=NCT03111030&rank=1.

Similar content being viewed by others
References
Van Den Berg-Emons RJ, Bussmann JB, Stam HJ. Accelerometry-based activity spectrum in persons with chronic physical conditions. Arch Phys Med Rehabil. 2010;91:1856–61.
Noreau L, Shephard RJ, Simard C, Pare G, Pomerleau P. Relationship of impairment and functional ability to habitual activity and fitness following spinal cord injury. Int J Rehabil Res. 1993;16:265–75.
Hicks AL, Martin Ginis KA, Pelletier CA, Ditor DS, Foulon B, Wolfe DL. The effects of exercise training on physical capacity, strength, body composition and functional performance among adults with spinal cord injury: a systematic review. Spinal Cord. 2011;49:1103–27. https://doi.org/10.1038/sc.2011.62.
van der Scheer JW, Martin Ginis KA, Ditor DS, Goosey-Tolfrey V, Hicks AL, West C, et al. Effects of exercise on fitness and health of adults with spinal cord injury: a systematic review. Neurology. 2017;89:736–45.
Lugo LH, Salinas F, García HI. Out-patient rehabilitation programme for spinal cord injured patients: evaluation of the results on motor FIM score. Disabil Rehabil. 2009;29:873–81.
Duran FS, Lugo L, Ramirez L, Eusse E. Effects of an exercise program on the rehabilitation of patients with spinal cord injury. Arch Phys Med Rehabil. 2001;82:1349–54.
Miller LE, Herbert G. Health and economic benefits of physical activity for patients with spinal cord injury. Clin Outcomes Res. 2016;8:551.
Martin Ginis KA, Ma JK, Latimer-Cheung AE, Rimmer J. A systematic review of review articles addressing factors related to physical activity participation among children and adults with physical disabilities. Health Psychol Rev. 2016;10:478–94.
Fekete C, Rauch A. Correlates and determinants of physical activity in persons with spinal cord injury: a review using the International Classification of Functioning, Disability and Health as reference framework. Disabil Health J. 2012;5:140–50. http://www.ncbi.nlm.nih.gov/pubmed/22726854. Accessed 21 Oct 2014.
Ma JK, Martin Ginis KA. A meta-analysis of physical activity interventions in people with physical disabilities: content, characteristics, and effects on behaviour. Psychol Sport Exerc. 2018;37:262–73.
Webb TL, Joseph J, Yardley L, Michie S. Using the internet to promote health behavior change: a systematic review and meta-analysis of the impact of theoretical basis, use of behavior change techniques, and mode of delivery on efficacy. J Med Internet Res. 2010;12:1–18.
Taylor N, Conner M, Lawton R. The impact of theory on the effectiveness of worksite physical activity interventions: a meta-analysis and meta-regression. Health Psychol Rev. 2012;6:33–73.
Schwarzer R, Lippke S, Luszczynska A. Mechanisms of health behavior change in persons with chronic illness or disability: The Health Action Process Approach (HAPA). Rehabil Psychol. 2011;56:161–70. http://doi.apa.org/getdoi.cfm?doi=10.1037/a0024509. Accessed 14 Aug 2018.
Latimer AE, Martin Ginis KA, Arbour KP. The efficacy of an implementation intention intervention for promoting physical activity among individuals with spinal cord injury: a randomized controlled trial. Rehabil Psychol. 2006;51:273–80.
Martin Ginis KA, Arbour-Nicitopoulos KP, Latimer AE, Buchholz AC, Bray SR, Craven BC, et al. Leisure time physical activity in a population-based sample of people with spinal cord injury part II: activity types, intensities, and durations. Arch Phys Med Rehabil. 2010;91:729–33. https://doi.org/10.1016/j.apmr.2009.12.028.
Radomski MV, Finkelstein M, Hagel S, Masemer S, Theis J, Thompson M. A pilot wellness and weight management program for individuals with spinal cord injury: participants’ goals and outcomes. Top Spinal Cord Inj Rehabil. 2011;17:59–69.
Froehlich-Grobe K, Lee J, Aaronson L, Nary DE, Washburn RA, Little TD. Exercise for everyone: a randomized controlled trial of project workout on wheels in promoting exercise among wheelchair users. Arch Phys Med Rehabil. 2014;95:20–8. https://doi.org/10.1016/j.apmr.2013.07.006.
Froehlich-Grobe K, White GW. Promoting physical activity among women with mobility impairments: a randomized controlled trial to assess a home- and community-based intervention. Arch Phys Med Rehabil. 2004;85:640–8.
Nooijen CFJ, Stam HJ, Sluis T, Valent L, Twisk J, Van Den Berg-Emons RJG. A behavioral intervention promoting physical activity in people with subacute spinal cord injury: secondary effects on health, social participation and quality of life. Clin Rehabil. 2017;31:772–80.
Allin S, Shepherd J, Tomasone J, Munce S, Linassi G, Hossain SN, et al. Participatory design of an online self-management tool for users with spinal cord injury: qualitative study. JMIR Rehabil Assist Technol. 2018;5:1–14.
Nosek MA, Robinson-Whelen S, Ledoux TA, Hughes RB, O’Connor DP, Lee RE, et al. A pilot test of the GoWoman weight management intervention for women with mobility impairments in the online virtual world of Second Life. Disabil Rehabil. 2018;40:1–12.
Graham ID, Logan J, Harrison MB, Straus SE, Tetroe J, Caswell W, et al. Lost in knowledge translation: time for a map? J Contin Educ Health Prof. 2006;26:13–24.
Ma JK, Cheifetz O, Todd KR, Chebaro C, Phang SH, Shaw RB, et al. Advancing intervention development: Engagement of physiotherapists and patients in the co-creation of a physical activity intervention for adults with spinal cord injury (under rev).
Latimer-Cheung AE, Arbour-Nicitopoulos KP, Brawley LR, Gray C, Justine Wilson A, Prapavessis H, et al. Developing physical activity interventions for adults with spinal cord injury. Part 2: Motivational counseling and peer-mediated interventions for people intending to be active. Rehabil Psychol. 2013;58:307–15. http://www.ncbi.nlm.nih.gov/pubmed/23978086. Accessed 1 May 2018.
Faul F, Erdfelder E, Lang A-G, Buchner A. G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39:175–91.
Canadian Society for Exercise Physiologists. Participaction. Toronto: Canadian Society for Exercise Physiologists; 2010.
Maynard FM, Bracken MB, Creasey G, Ditunno JF, Donovan WH, Ducker B, et al. International standards for neurological and functional classification of spinal cord injury: American Spinal Injury Association. Spinal Cord. 1997;35:266–74.
Troiano RP, Berrigan D, Dodd KW, Masse LC, Tilert T, Mcdowell M. Physical activity in the United States measured by accelerometer. Med Sci Sport Exerc. 2007;40:181–8.
Hart TL, Swartz AM, Cashin SE, Strath SJ. How many days of monitoring predict physical activity and sedentary behaviour in older adults? Int J Behav Nutr Phys Act. 2011;8:1–7.
Conger SA, Scott SN, Fitzhugh EC, Thompson DL, Bassett DR. Validity of physical activity monitors for estimating energy expenditure during wheelchair propulsion. J Phys Act Health. 2015;12:1520–6.
Warms CA, Belza BL. Actigraphy as a measure of physical activity for wheelchair users with spinal cord injury. Nurs Res. 2004;53:136–43.
McCracken LA, Ma JK, Voss C, Martin Ginis KA, West CR. Individual physical activity cut-points for wrist accelerometry in spinal cord injury. Arch Phys Med Rehabil. 2018;99(4):684–9.
Ma JK, McCracken LA, Voss C, Chan FHN, West CR, Martin Ginis KA. Physical activity measurement in people with spinal cord injury: comparison of accelerometry and the physical activity recall assessment for people with spinal cord injury. Disabil Rehabil. 2018;40:1–7. https://doi.org/10.1080/09638288.2018.1494213.
Bouchard C, Shephard RJ. Physical activity, fitness, and health: the model and key concepts. Phys Act Fitness, Heal Int Proc Consens Statement. In: International proceedings and consensus statement. InInternational Consensus Symposium on Physical Activity, Fitness, and Health, 2nd, May, 1992, Toronto, ON, Canada ,1994, p. 77–88.
Martin Ginis KA, Latimer AE, Hicks AL, Craven BC. Development and evaluation of an activity measure for people with spinal cord injury. Med Sci Sports Exerc. 2005;37:1099–111.
Martin Ginis KA, Phang SH, Latimer AE, Arbour-Nicitopoulos KP. Reliability and validity tests of the leisure time physical activity questionnaire for people with spinal cord injury. Arch Phys Med Rehabil. 2012;93:677–82. https://doi.org/10.1016/j.apmr.2011.11.005.
Claydon VE, Hol AT, Eng JJ, Krassioukov AV. Cardiovascular responses and postexercise hypotension after arm cycling exercise in subjects with spinal cord injury. Arch Phys Med Rehabil. 2006;87:1106–14.
Borg G. Perceived exertion as an indicator of somatic stress. Scand J Rehabil Med. 1970;2:92–8.
Bandura A. Self-efficacy: the exercise of control. New York: W.H. Freeman & Co.; 1997.
Scholz U, Sniehotta FF, Schwarzer R. Predicting physical exercise in cardiac rehabilitation: the role of phase-specific self-efficacy beliefs. J Sport Exerc Psychol. 2005;27:135–51.
Sniehotta F, Scholz U, Lippke S, Ziegelmann J, Luszczynska A. Scale for the assessment of phase-specific self-efficacy of physical activity. Meas Instrum. https://userpage.fu-berlin.de/health/healself.pdf.
Sniehotta FF, Scholz U, Schwarzer R. Bridging the intention–behaviour gap: planning, self-efficacy, and action control in the adoption and maintenance of physical exercise. Psychol Health. 2005;20:143–60. http://www.tandfonline.com/doi/abs/10.1080/08870440512331317670. Accessed 4 Jan 2016.
Martin Ginis KA, Hicks AL, Latimer AE, Warburton DER, Bourne C, Ditor DS, et al. The development of evidence-informed physical activity guidelines for adults with spinal cord injury. Spinal Cord. 2011;49:1088–96. https://doi.org/10.1038/sc.2011.63.
Cowan RE, Nash MS, Anderson KD. Exercise participation barrier prevalence and association with exercise participation status in individuals with spinal cord injury. Spinal Cord. 2013;51:27–32. http://www.ncbi.nlm.nih.gov/pubmed/22584283. Accessed 21 June 2019.
Sallis JF, Grossman RM, Pinski RB, Patterson TL, Nader PR. The development of scales to measure social support for diet and exercise behaviours. Prev Med (Baltim). 1987;16:825–36.
Arbour-Nicitopoulos KP, Martin Ginis KA, Latimer AE. Planning, leisure-time physical activity, and coping self-efficacy in persons with spinal cord injury: a randomized controlled trial. Arch Phys Med Rehabil. 2009;90:2003–11. https://doi.org/10.1016/j.apmr.2009.06.019.
Martin Ginis KA, Tomasone JR, Latimer-Cheung AE, Arbour-Nicitopoulos KP, Bassett-Gunter RL, Wolfe DL. Developing physical activity interventions for adults with spinal cord injury. Part 1: a comparison of social cognitions across actors, intenders, and nonintenders. Rehabil Psychol. 2013;58:299–306. http://www.scopus.com/inward/record.url?eid=2-s2.0-84883144796&partnerID=tZOtx3y1. Accessed 22 Feb 2018.
Marcus B, Simkin L. The stages of exercise behavior. J Sports Med Phys Fitness. 1993;33:83–8.
Tomasone JR, Flood SM, Ma JK, Scime NV, Burke SM, Sleeth L, et al. Physical activity self-management interventions for adults with spinal cord injury: part 1—a systematic review of the use and effectiveness of behavior change techniques. Psychol Sport Exerc. 2018;37:274–85.
Michie S, Richardson M, Johnston M, Abraham C, Francis J, Hardeman W, et al. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: building an international consensus for the reporting of behavior change interventions. Ann Behav Med. 2013;46:81–95.
Lorencatto F, West R, Bruguera C, Michie S. A method for assessing fidelity of delivery of telephone behavioural support for smoking cessation. J Consult Clin Psychol. 2014;82:482–91.
Burkett LN, Chisum J, Stone W, Femhall B. Exercise capacity of untrained spinal cord injured individuals and the relationship of peak oxygen uptake to level of injury. Paraplegia. 1990;28:512–21.
Astrand P. Human physical fitness with special reference to sex and age. Physiol Rev. 2019;36:307–35.
Martin Ginis KA, Latimer AE, Arbour-Nicitopoulos KP, Buchholz AC, Bray SR, Craven BC, et al. Leisure time physical activity in a population-based sample of people with spinal cord injury part I: demographic and injury-related correlates. Arch Phys Med Rehabil. 2010;91:722–8. http://www.ncbi.nlm.nih.gov/pubmed/20434609. Accessed 10 Jan 2015.
Cohen J. A Power Primer. Psychol Bull. 1992;112(1):155.
Cohen J. Weighted kappa: nominal scale agreement with provision for scaled disagreement or partial credit. Psychol Bull. 1968;70:213–20.
Kooijmans H, Moremans H, Stam H, Bussman J. Valid detection of self-propelled wheelchair driving with two accelerometers. Physiol Meas. 2014;35:2297–306.
Bassett DR, Ainsworth BE, Swartz AM, Strath SJ, Brien WLO, King GA. Validity of four motion sensors in measuring moderate intensity physical activity. Med Sci Sport Exerc. 2000;2:471–80.
Shephard RJ. Normal levels of activity in Canadian city dwellers. Can Med Assoc J. 1967;97:313–8.
Wise HH, Jackson Thomas K, Nietert PJ, Brown DD, Sword DO, Diehl N. Home physical activity programs for the promotion of health and wellness in individuals with spinal cord injury. Top Spinal Cord Inj Rehabil. 2009;14:122–32.
Nooijen CFJ, Stam HJ, Bergen MP, Bongers-Janssen HMH, Valent L, van Lageveld S, et al. A behavioural intervention increases physical activity in people with subacute spinal cord injury: a randomised trial. J Physiother. 2016;62:35–41.
Pelletier CA, De Totosy Zepetnek JO, Macdonald MJ, Hicks AL. A 16-week randomized controlled trial evaluating the physical activity guidelines for adults with spinal cord injury. Spinal Cord. 2015;53:363–7.
Scelza WM, Kalpakjian CZ, Zemper ED, Tate DG. Perceived barriers to exercise in people with spinal cord injury. Am J Phys Med Rehabil. 2005;84:576–83.
Sniehotta FF, Scholz U, Schwarzer R, Fuhrmann B, Kiwus U, Völler H. Long-term effects of two psychological interventions on physical exercise and self-regulation following coronary rehabilitation. Int J Behav Med. 2005;12:244–55. http://www.ncbi.nlm.nih.gov/pubmed/16262543. Accessed 19 Aug 2018.
Adams SA, Matthews CE, Ebbeling CB, Moore CG, Joan E, Fulton J, et al. The effects of social desirability and social approval on self-reports of physical activity. Am J Epidemiol. 2010;161:389–98.
Martin Ginis KA, Van Der Scheer JW, Andy AEL, Chris B, Carruthers P, Bernardi M, et al. Evidence-based scientific exercise guidelines for adults with spinal cord injury: an update and a new guideline. Spinal Cord: US; 2017. p. 1–13.
Acknowledgements
The authors thank all the participants for their time and effort in designing and completing the trial.
Author information
Authors and Affiliations
Contributions
JM contributed to study conceptualization, data collection, analysis, and writing of the manuscript. CW contributed to study conceptualization, analysis, and review of the manuscript. KMG contributed to study conceptualization, analysis, writing and review of the manuscript.
Corresponding author
Ethics declarations
Funding
This work was supported by an Ontario Neurotrauma Foundation/Rick Hansen Institute grant (2015-RHI-PEPA-998). The funding body did not contribute to the design of the project, collection, analysis, and interpretation of data, or in writing the manuscript.
Conflict of Interest
Dr. Jasmin Ma, Dr. Christopher West, and Dr. Kathleen Martin Ginis have no conflicts of interest that are directly relevant to the content of this article.
Ethics approval and consent to participate
Ethics approval for the protocol was granted by the Clinical Research Ethics Board at the University of British Columbia. Written informed consent was obtained from each of the participants. This study was performed in accordance with the standards of ethics outlined in the Declaration of Helsinki.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ma, J.K., West, C.R. & Martin Ginis, K.A. The Effects of a Patient and Provider Co-Developed, Behavioral Physical Activity Intervention on Physical Activity, Psychosocial Predictors, and Fitness in Individuals with Spinal Cord Injury: A Randomized Controlled Trial. Sports Med 49, 1117–1131 (2019). https://doi.org/10.1007/s40279-019-01118-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-019-01118-5