Abstract
Background
Skeletal muscle plays an important role in maintaining the stability of the lumbar region. However, there is conflicting evidence regarding the effects of exercise on trunk muscle morphology.
Objective
To systematically review the literature on the effects of exercise training on lower trunk muscle morphology to determine the comparative effectiveness of different exercise interventions.
Data Source and Study Selection
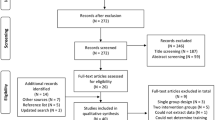
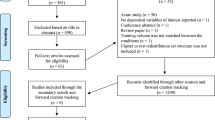
A systematic search strategy was conducted in the following databases: PubMed, SportDiscus, CINAHL, the Cochrane Library and PEDro. We included full, peer-reviewed, prospective longitudinal studies, including randomized controlled trials and single-group designs, such as pre- to post-intervention and crossover studies, reporting on the effect of exercise training on trunk muscle morphology.
Study Appraisal and Synthesis
Study quality was assessed with the Cochrane risk-of-bias tool. We classified each exercise intervention into four categories, based on the primary exercise approach: motor control, machine-based resistance, non-machine-based resistance or cardiovascular. Treatment effects were estimated using within-group standardized mean differences (SMDs).
Results
The systematic search identified 1,911 studies; of which 29 met our selection criteria: motor control (n = 12), machine-based resistance (n = 10), non-machine-based resistance (n = 5) and cardiovascular (n = 2). Fourteen studies (48 %) reported an increase in trunk muscle size following exercise training. Among positive trials, the largest effects were reported by studies testing combined motor control and non-machine-based resistance exercise (SMD [95 % CI] = 0.66 [0.06 to 1.27] to 3.39 [2.80 to 3.98]) and machine-based resistance exercise programmes (SMD [95 % CI] = 0.52 [0.01 to 1.03] to 1.79 [0.87 to 2.72]). Most studies investigating the effects of non-machine-based resistance exercise reported no change in trunk muscle morphology, with one study reporting a medium effect on trunk muscle size (SMD [95 % CI] = 0.60 [0.03 to 1.16]). Cardiovascular exercise interventions demonstrated no effect on trunk muscle morphology (SMD [95 % CI] = −0.16 [−1.14 to 0.81] to 0.09 [−0.83 to 1.01]).
Limitations
We excluded studies published in languages other than English, and therefore it is possible that the results of relevant studies are not represented in this review. There was large clinical heterogeneity between the included studies, which prevented data synthesis. Among the studies included in this review, common sources of potential bias were random sequence generation, allocation concealment and blinding. Finally, the details of the exercise parameters were poorly reported in most studies.
Conclusion
Approximately half of the included studies reported an increase in lower trunk muscle size following participation in an exercise programme. Among positive trials, studies involving motor control exercises combined with non-machine-based resistance exercise, as well as machine-based resistance exercises, demonstrated medium to large effects on trunk muscle size. Most studies examining the effect of non-machine-based resistance exercise and all studies investigating cardiovascular exercise reported no effect on trunk muscle morphology. However, these results should be interpreted with caution because of the substantial risk of bias and suboptimal reporting of exercise details in the included studies. Additional research, using methods ensuring a low risk of bias, are required to further elucidate the effects of exercise on trunk muscle morphology.







Similar content being viewed by others
References
Cholewicki J, McGill SM. Mechanical stability of the in vivo lumbar spine: implications for injury and chronic low back pain. Clin Biomech. 1996;11(1):1–15.
d’Hemecourt PA, Luke A. Sport-specific biomechanics of spinal injuries in aesthetic athletes (dancers, gymnasts, and figure skaters). Clin Sports Med. 2012;31(3):397–408. doi:10.1016/j.csm.2012.03.010.
Donatelli R, Dimond D, Holland M. Sport-specific biomechanics of spinal injuries in the athlete (throwing athletes, rotational sports, and contact-collision sports). Clin Sports Med. 2012;31(3):381–96. doi:10.1016/j.csm.2012.03.003.
Alexander MJ. Biomechanical aspects of lumbar spine injuries in athletes: a review. Can J Appl Sport Sci. 1985;10(1):1–20.
Panjabi MM. The stabilizing system of the spine. Part I. Function, dysfunction, adaptation, and enhancement. J Spinal Disord. 1992;5(4):383–9 (discussion 397).
Panjabi MM. Clinical spinal instability and low back pain. J Electromyogr Kinesiol. 2003;13(4):371–9.
Cholewicki J, Panjabi MM, Khachatryan A. Stabilizing function of trunk flexor-extensor muscles around a neutral spine posture. Spine (Phila Pa 1976). 1997;22(19):2207–12.
Bergmark A. Stability of the lumbar spine. A study in mechanical engineering. Acta Orthop Scand Suppl. 1989;230:1–54.
Stevens VK, Vleeming A, Bouche KG, et al. Electromyographic activity of trunk and hip muscles during stabilization exercises in four-point kneeling in healthy volunteers. Eur Spine J. 2007;16(5):711–8. doi:10.1007/s00586-006-0181-1.
McGill SM. Low back stability: from formal description to issues for performance and rehabilitation. Exerc Sport Sci Rev. 2001;29(1):26–31.
Crisco JJ III, Panjabi MM. Euler stability of the human ligamentous lumbar spine. Part I: theory. Clin Biomech. 1992;7(1):19–26.
Hodges PW, Richardson CA. Inefficient muscular stabilization of the lumbar spine associated with low back pain. A motor control evaluation of transversus abdominis. Spine (Phila Pa 1976). 1996;21(22):2640–50.
Chilibeck PD, Calder AW, Sale DG, et al. A comparison of strength and muscle mass increases during resistance training in young women. Eur J Appl Physiol Occup Physiol. 1998;77(1–2):170–5.
Choi G, Raiturker PP, Kim MJ, et al. The effect of early isolated lumbar extension exercise program for patients with herniated disc undergoing lumbar discectomy. Neurosurgery. 2005;57(4):764–72.
Evans WJ. Reversing sarcopenia: how weight training can build strength and vitality. Geriatrics. 1996;51(5):46–7, 51–3; quiz 54.
Klizienė I, Sipavičienė S, Imbrasienė D, et al. Effect of core stability exercise on cross sectional area of lumbar multifidus muscle and physical capacity. Educ Phys Train Sport. 2011;83:9–15.
Singh DK, Bailey M, Lee RY. Ageing modifies the fibre angle and biomechanical function of the lumbar extensor muscles. Clin Biomech. 2011;26(6):543–7. doi:10.1016/j.clinbiomech.2011.02.002.
Hides JA, Richardson CA, Jull GA. Multifidus muscle recovery is not automatic after resolution of acute, first-episode low back pain. Spine (Phila Pa 1976). 1996;21(23):2763-9.
Parkkola R, Rytokoski U, Kormano M. Magnetic resonance imaging of the discs and trunk muscles in patients with chronic low back pain and healthy control subjects. Spine (Phila Pa 1976). 1993;18(7):830–6.
Beneck GJ, Kulig K. Multifidus atrophy is localized and bilateral in active persons with chronic unilateral low back pain. Arch Phys Med Rehabil. 2012;93(2):300–6.
Hicks GE, Simonsick EM, Harris TB, et al. Trunk muscle composition as a predictor of reduced functional capacity in the health, aging and body composition study: the moderating role of back pain. Gerontol A Biol Sci Med Sci. 2005;60(11):1420–4.
Hicks GE, Simonsick EM, Harris TB, et al. Cross-sectional associations between trunk muscle composition, back pain, and physical function in the health, aging and body composition study. Gerontol A Biol Sci Med Sci. 2005;60(7):882–7.
Sihvonen T, Herno A, Paljarvi L, et al. Local denervation atrophy of paraspinal muscles in postoperative failed back syndrome. Spine (Phila Pa 1976). 1993;18(5):575–81.
Akbari A, Khorashadizadeh S, Abdi G. The effect of motor control exercise versus general exercise on lumbar local stabilizing muscles thickness: randomized controlled trial of patients with chronic low back pain. J Back Musculoskelet Rehabil. 2008;21(2):105–12.
Woohyung L, Yoonmi L, Wontae G. The effect of lumbar strengthening exercise on pain and the cross-sectional area change of lumbar muscles. J Phys Ther Sci. 2011;23(2):209–12.
Lescher S, Bender B, Eifler R, et al. Isometric non-machine-based prevention training program: effects on the cross-sectional area of the paravertebral muscles on magnetic resonance imaging. Clin Neuroradiol. 2011;21(4):217–22. doi:10.1007/s00062-011-0104-3.
Sokunbi O, Watt P, Moore A. A randomised controlled trial (RCT) on the effects of frequency of application of spinal stabilisation exercises on multifidus cross sectional area (MFCSA) in participants with chronic low back pain. Physiother Singap. 2008;11(2):9–16.
Critchley DJ, Pierson Z, Battersby G. Effect of Pilates mat exercises and conventional exercise programmes on transversus abdominis and obliquus internus abdominis activity: pilot randomised trial. Man Ther. 2011;16(2):183–9. doi:10.1016/j.math.2010.10.007.
Kuk JL, Church TS, Blair SN, et al. Associations between changes in abdominal and thigh muscle quantity and quality. Med Sci Sports Exerc. 2008;40(7):1277–81.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62(10):e1–34. doi:10.1016/j.jclinepi.2009.06.006.
Mayer J, Mooney V, Dagenais S. Evidence-informed management of chronic low back pain with lumbar extensor strengthening exercises. Spine J. 2008;8(1):96–113. doi:10.1016/j.spinee.2007.09.008.
Martuscello JM, Nuzzo JL, Ashley CD, et al. Systematic review of core muscle activity during physical fitness exercises. J Strength Cond Res. 2013;27(6):1684–98. doi:10.1519/JSC.0b013e318291b8da.
Macedo LG, Maher CG, Latimer J, et al. Motor control exercise for persistent, nonspecific low back pain: a systematic review. Phys Ther. 2009;89(1):9–25. doi:10.2522/ptj.20080103.
Kankaanpaa M, Taimela S, Airaksinen O, et al. The efficacy of active rehabilitation in chronic low back pain. Effect on pain intensity, self-experienced disability, and lumbar fatigability. Spine (Phila Pa 1976). 1999;24(10):1034–42.
Parkkola R, Kujala U, Rytokoski U. Response of the trunk muscles to training assessed by magnetic resonance imaging and muscle strength. Eur J Appl Physiol Occup Physiol. 1992;65(5):383–7.
Darden E. The Nautilus book. Chicago: Contemporary Books; 1990.
Thompson WR, Gordon NF, Pescatello LS, et al. ACSM’s guidelines for exercise testing and prescription. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2010.
Agarwal SK. Cardiovascular benefits of exercise. Int J Gen Med. 2012;5:541–5. doi:10.2147/IJGM.S30113.
Higgins JP, Altman DG, Gotzsche PC, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928. doi:10.1136/bmj.d5928.
Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. Hillsdale: L. Erlbaum Associates; 1988.
Storheim K, Holm I, Gunderson R, et al. The effect of comprehensive group training on cross-sectional area, density, and strength of paraspinal muscles in patients sick-listed for subacute low back pain. J Spinal Disord Tech. 2003 Jun;16(3):271-9.
Hides JA, Stanton WR, Wilson SJ, et al. Retraining motor control of abdominal muscles among elite cricketers with low back pain. Scand J Med Sci Sports. 2010;20(6):834–42.
Sakamaki M, Bemben MG, Abe T. Legs and trunk muscle hypertrophy following walk training with restricted leg muscle blood flow. J Sports Sci Med. 2011;10(2):338–40.
Danneels LA, Cools AM, Vanderstraeten GG et al. The effects of three different training modalities on the cross-sectional area of the paravertebral muscles. Scand J Med Sci Sports. 2001;11(6):335–41.
Teyhen DS, Childs JD, Dugan JL, et al. Effect of two different exercise regimens on trunk muscle morphometry and endurance in soldiers in training. Phys Ther. 2013;93(9):1211–24.
Danneels L, Vanderstraeten G, Cambier D, et al. Effects of three different training modalities on the cross sectional area of the lumbar multifidus muscle in patients with chronic low back pain. Br J Sports Med. 2001;35(3):186–91. doi:10.1136/bjsm.35.3.186.
Hides JA, Stanton WR, Mendis MD, et al. Effect of motor control training on muscle size and football games missed from injury. Med Sci Sport Exerc. 2012;44(6):1141–9. doi:10.1249/Mss.0b013e318244a321.
Dorado C, Calbet JA, Lopez-Gordillo A, et al. Marked effects of Pilates on the abdominal muscles: a longitudinal magnetic resonance imaging study. Med Sci Sport Exerc. 2012;44(8):1589–94. doi:10.1249/MSS.0b013e31824fb6ae.
Hides J, Stanton W, McMahon S, et al. Effects of stabilization training on multifidus muscle cross-sectional area among young elite cricketers with low back pain. J Orthop Sports Phys Ther. 2008;38(3):101–8.
Jansen JA, Mens JM, Backx FJ, et al. Changes in abdominal muscle thickness measured by ultrasound are not associated with recovery in athletes with longstanding groin pain associated with resisted hip adduction. J Orthop Sports Phys Ther. 2009;39(10):724–32. doi:10.2519/jospt.2009.3068 2354 [pii].
Jongwoo KIM, Wontae G, Byeongjun H. The effects of resistivity and stability-combined exercise for lumbar muscles on strength, cross-sectional area and balance ability: exercises for prevention of lower back pain. J Phys Ther Sci. 2011;23(2):247–50.
Kaser L, Mannion AF, Rhyner A, et al. Active therapy for chronic low back pain: part 2. Effects on paraspinal muscle cross-sectional area, fiber type size, and distribution. Spine (Phila Pa 1976). 2001;26(8):909–19.
Kramer M, Dehner C, Katzmaier P, et al. Device-assisted muscle strengthening in the rehabilitation of patients after surgically stabilized vertebral fractures. Arch Phys Med Rehabil. 2005;86(3):558–64. doi:10.1016/j.apmr.2004.09.008.
Lee N-G, Jung J-H, You JH, et al. Novel augmented ADIM training using ultrasound imaging and electromyography in adults with core instability. J Back Musculoskelet Rehabil. 2011;24(4):233–40.
Mooney V, Gulick J, Perlman M, et al. Relationships between myoelectric activity, strength, and MRI of lumbar extensor muscles in back pain patients and normal subjects. J Spinal Disord. 1997;10(4):348–56.
Rissanen A, Kalimo H, Alaranta H. Effect of intensive training on the isokinetic strength and structure of lumbar muscles in patients with chronic low back pain. Spine (Phila Pa 1976). 1995;20(3):333–40.
Willemink MJ, van Es HW, Helmhout PH, et al. The effects of dynamic isolated lumbar extensor training on lumbar multifidus functional cross-sectional area and functional status of patients with chronic non-specific low back pain. Spine (Phila Pa 1976). 2012;37(26):E1651–8.
Hoshikawa Y, Iida T, Muramatsu M, et al. Effects of stabilization training on trunk muscularity and physical performances in youth soccer players. J Strength Cond Res. 2013;27(11):3142–9. doi:10.1519/JSC.0b013e31828bed36.
Fortin M, Macedo LG. Multifidus and paraspinal muscle group cross-sectional areas of patients with low back pain and control patients: a systematic review with a focus on blinding. Phys Ther. 2013;. doi:10.2522/ptj.20120457.
Narici MV, Hoppeler H, Kayser B, et al. Human quadriceps cross-sectional area, torque and neural activation during 6 months strength training. Acta Physiol Scand. 1996;157(2):175–86. doi:10.1046/j.1365-201X.1996.483230000.x.
Hebert JJ, Kjaer P, Fritz JM, et al. The relationship of lumbar multifidus muscle morphology to previous, current, and future low back pain: a nine-year population-based prospective cohort study. Spine (Phila Pa 1976). 2014. doi:10.1097/BRS.0000000000000424.
Timson BF. Evaluation of animal models for the study of exercise-induced muscle enlargement. J Appl Physiol. 1990;69(6):1935–45.
Staron RS, Karapondo DL, Kraemer WJ, et al. Skeletal muscle adaptations during early phase of heavy-resistance training in men and women. J Appl Physiol. 1994;76(3):1247–55.
Fry AC. The role of resistance exercise intensity on muscle fibre adaptations. Sports Med. 2004;34(10):663–79.
Campos GE, Luecke TJ, Wendeln HK, et al. Muscular adaptations in response to three different resistance-training regimens: specificity of repetition maximum training zones. Eur J Appl Physiol. 2002;88(1–2):50–60. doi:10.1007/s00421-002-0681-6.
Cardinale M, Newton R, Nosaka K. Strength and conditioning biological principles and practical applications. Chichester: Wiley; 2011.
McGill SM. Low back exercises: evidence for improving exercise regimens. Phys Ther. 1998;78(7):754–65.
Slade SC, Keating JL. Exercise prescription: a case for standardised reporting. Br J Sports Med. 2012;46(16):1110–3. doi:10.1136/bjsports-2011-090290.
Acknowledgments
The authors would like to thank Ms Margaret Solosy for assistance with developing the search strategy, Dr Golnaz Shahtahmassebi for statistical advice and Mr Andrew Schechter (A.S.) for assisting with study selection. The contributions of the authors are as follows: B.S.—study conception and design, data acquisition, analysis and interpretation, drafting and final approval of the manuscript; J.J.H.—study conception and design, data interpretation, critical revision and approval of the final manuscript; N.J.S.—data acquisition, critical revision and final approval of the manuscript; M.H.—study conception, critical revision and final approval of the manuscript; T.J.F.—study conception and design, data interpretation, critical revision and final approval of the manuscript.
Conflicts of interest
The authors have no conflicts of interest that are directly relevant to the content of this review. No sources of funding were used in the preparation of this review.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Below is the link to the Electronic Supplementary Material.
Rights and permissions
About this article
Cite this article
Shahtahmassebi, B., Hebert, J.J., Stomski, N.J. et al. The Effect of Exercise Training on Lower Trunk Muscle Morphology. Sports Med 44, 1439–1458 (2014). https://doi.org/10.1007/s40279-014-0213-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-014-0213-7