Abstract
Ivosidenib (Tibsovo®), a first-in-class, small molecule inhibitor of mutant isocitrate dehydrogenase 1 (IDH1), is an important new therapeutic option in the USA for treating adults with relapsed or refractory acute myeloid leukemia who have a susceptible IDH1 gene mutation. In such patients, oral ivosidenib is effective and generally well tolerated, producing encouraging rates and durations of complete remission (CR), CR or CR with partial hematologic recovery (CR/CRh), overall response, and overall survival. CR/CRh rates are consistent across most baseline characteristics. Ivosidenib also provides additional clinical benefits, including transfusion independence, improvements in hematologic variables, and deep molecular responses as measured by IDH1 mutation clearance in patients who achieve CR/CRh.
Similar content being viewed by others
Reduces elevated levels of d-2-hydroxyglutarate and reverses the inhibition of myeloid blast differentiation imposed by mutant IDH1 enzymes |
Provides beneficial effects on rates and duration of CR, CR/CRh, overall response, and overall survival |
Improves transfusion dependence and hematologic variables |
Adverse events of special interest include QT interval prolongation, IDH-differentiation syndrome, and leukocytosis; are managed using standard-of-care measures and dosage modifications, where required |
Convenient once-daily oral administration regimen |
What is the rationale for using ivosidenib in relapsed or refractory AML?
Acute myeloid leukemia (AML) is a group of heterogeneous hematologic malignancies characterized by the clonal expansion of myeloid precursor cells (i.e. blasts) in the bone marrow, blood, and/or other tissues [1]. It typically arises from somatic mutations [e.g. isocitrate dehydrogenase 1 (IDH1) gene mutations] that alter the normal mechanisms of proliferation, survival, differentiation, and/or self-renewal of the blasts [2, 3]. The pathogenesis may also involve cytogenetic alterations and/or dysregulated epigenetic mechanisms [4, 5]. AML is diagnosed based on the presence of ≥ 20% of blasts in the bone marrow or blood; however, accurate classification requires multidisciplinary diagnostic studies [1]. AML is the most common type of acute leukemia in adults [1], with > 50% of patients being diagnosed aged ≥ 65 years [6].
Mutations in the IDH1 gene are found in ≈ 6–16% of patients with AML [7]. IDH1 encodes a key metabolic enzyme, IDH1, which is located in the cytoplasm and peroxisomes and catalyzes the reversible NADP+-dependent oxidative decarboxylation of isocitrate to yield α–ketoglutarate [8]. Other metabolic IDH enzymes, namely IDH2 and IDH3 (encoded by IDH2 and IDH3) are located in the mitochondria [8]. Mutations in IDH1 result in neomorphic enzymatic activity, leading to the conversion of NADH and α–ketoglutarate to NADP+ and d-2-hydroxyglutarate (d-2HG) [8,9,10]. Mutant IDH1 enzymes produce high levels of d-2HG in cells [10]; the cellular accumulation of d-2HG competitively inhibits α–ketoglutarate-dependent enzymes, which prevents normal hematopoietic differentiation and promotes tumorigenesis [11,12,13]. Patients with IDH1- or IDH2-mutated AML are associated with high rates of co-occurring NPM1 mutations, intermediate-risk cytogenetics, increased platelet counts, high numbers of bone marrow blasts at diagnosis, and older patient age [14]. The prognostic significance of IDH1 or IDH2 mutations in AML (i.e. compared with the wild-type IDH form of the disease) remains controversial [1].
Standard treatment protocols for AML typically comprise induction chemotherapy (e.g. cytarabine and an anthracycline in patients aged < 60 years) followed by post-remission therapy, as well as supportive care [1]. The induction therapy strategy is influenced by patient age, history of prior myelodysplasia or cytotoxic therapy, and the presence of comorbid conditions that may affect performance status [1]. In patients that are not eligible for standard induction therapy (e.g. elderly patients or those who cannot tolerate intensive chemotherapy), other therapeutic strategies may be implemented, such as single-agent chemotherapy, hypomethylating-agent based therapy (e.g. azacytidine), or best supportive care (e.g. hydroxyurea or transfusion support) [1]. Despite these methods, patient outcomes in AML are generally poor; the estimated survival rate of the disease is only 27.4% within 5 years of diagnosis [6]. The rates of achieving complete remission (CR) rarely exceed 70% in patients aged < 60 years and 50% in patients > 60 years [1]. Moreover, most patients who achieve CR will have a disease relapse within 3 years of diagnosis [15].
Substantial efforts have recently been made to develop novel cancer treatments that molecularly target the genomic profile of the individual, thereby improving clinical outcomes and preventing toxicities associated with standard chemotherapy [16, 17].
One such novel agent is oral ivosidenib (Tibsovo®), a first-in-class, potent, selective small molecule inhibitor of susceptible mutant IDH1 enzymes developed to treat patients with cancers harboring IDH1 mutations [18,19,20]. In vitro and in vivo, clinically relevant concentrations of ivosidenib inhibit the function of mutant, but not wild-type, IDH1 enzymes, thereby reducing elevated d-2HG levels, and reversing the inhibition of myeloid blast differentiation [18,19,20].
When is ivosidenib therapy indicated in the USA?
Oral ivosidenib is approved in the USA for the treatment of adults with relapsed or refractory AML who have a susceptible IDH1 mutation in their blood and bone marrow as detected by an FDA-approved test (e.g. the Abbott RealTime IDH1 test) [18]. Susceptible IDH1 mutations are defined as those that lead to the increase of d-2HG levels in leukemia cells, and where the efficacy of ivosidenib is predicted by clinically meaningful remissions and/or inhibition of the mutant IDH1 enzyme activity at concentrations that are sustainable at the recommended dosage, according to validated methods. The most common IDH1 mutations that are susceptible to ivosidenib are Arg132 to His or Cys substitutions (i.e. R132H or R132C). Notably, patients without IDH1 mutations at diagnosis should be retested at relapse as IDH1 mutations may emerge during treatment or relapse [18].
Table 1 provides an overview of the use of ivosidenib in the treatment of AML based on the US prescribing information [18]. Dosage adjustments may be required to manage some treatment-related adverse effects (Table 1), but are not required on the basis of age, race, sex, body weight, Eastern Cooperative Oncology Group performance status (ECOG-PS) score, mild or moderate renal impairment, or mild hepatic impairment (data in patients with severe renal and moderate and severe hepatic impairment are lacking) [18].
Pregnant women should be advised of the potential risk to the fetus with ivosidenib therapy (based on animal embryo-fetal toxicity studies); breast-feeding women should also be advised to avoid breast-feeding during ivosidenib treatment and for ≥ 1 month after the last dose. Consult local prescribing information for further details on the use of ivosidenib [18].
What are the clinically relevant effects of ivosidenib in relapsed or refractory AML?
An open-label, dose-escalation (n = 78) + expansion phase (n = 180), multicenter study of oral ivosidenib was conducted in a total of 258 adult patients with IDH1-mutated advanced hematological malignancies, including 179 patients with relapsed or refractory AML [21]. In the dose-escalation phase, patient cohorts received ivosidenib at dosages ranging from 100 mg twice daily to 300–1200 mg once daily. Based on the available data regarding the safety, pharmacokinetic, and efficacy profiles of ivosidenib, the dosage that was selected to be evaluated in the expansion phase was ivosidenib 500 mg once daily. Ivosidenib was administered in 28-day cycles [21].
Pharmacodynamic effects
d-2HG was maximally inhibited in plasma and bone marrow by day 14 in patients who received ivosidenib 500 mg once daily, and d-2HG suppression was subsequently maintained throughout treatment [21]. Of note, mean plasma d-2HG decreased to the extent that was comparable to those reported in healthy individuals. No additional d-2HG inhibition was observed at higher dosages of 800 or 1200 mg once daily. Although the suppression of d-2HG formation is indicative of pharmacologic inhibition of mutated IDH1, the degree of suppression and baseline levels of d-2HG do not predict the clinical response to ivosidenib [21].
Clinical efficacy
In the phase 1 trial [21], the clinical efficacy of oral ivosidenib 500 mg once daily was assessed in 125 patients with relapsed or refractory IDH1-mutated AML. To be eligible to be included in this primary efficacy population, patients were required to have [21]:
-
IDH1 mutation-positive AML that had relapsed (i.e. second or later relapse, a relapse following a stem-cell transplant, or a relapse ≤ 1 year after initial therapy) or was refractory (i.e. refractory to induction or re-induction chemotherapy);
-
received a starting dosage of ivosidenib 500 mg once daily, with the first dose being administered ≥ 6 months prior to the analysis cut-off date (12 May 2017);
-
a baseline ECOG-PS score of 0-2;
-
documented IDH1 mutation(s) based on prospective central testing (which were retrospectively confirmed using an FDA-approved test for ivosidenib treatment selection [18]).
In the primary efficacy population, the median patient age was 67 years (range 18–87), 52% were male, and 66% had primary AML. Patients had received a median of 2 previous therapies (range 1–6), had an intermediate (53%) or poor (30%) cytogenetic risk status (status unknown for the remaining patients), and had received ivosidenib for a median of 3.9 months (range 0.1–25.8 months) [21].
The clinical efficacy of ivosidenib was assessed using the modified 2003 International Working Group response criteria for AML [22], where the primary endpoint was the rate of CR (defined as < 5% bone marrow blasts combined with an absolute neutrophil count of > 1 × 109/L and platelet count of > 100 × 109/L) as assessed by the investigators, or CR with partial hematologic recovery (CRh; defined as < 5% bone marrow blasts combined with an absolute neutrophil count of > 0.5 × 109/L and a platelet count of > 50 × 109/L) as assessed by the sponsor [21] (hereafter referred to as a CR/CRh response). Other clinical endpoints were also assessed [21]. Unless otherwise stated, results discussed are in the primary efficacy population.
Clinical response
Ivosidenib 500 mg once daily provided encouraging rates and durations of CR/CRh, CR, and overall response (Table 2) [21]. Notably, out of the patients who achieved a best response of CR/CRh, all achieved their first CR/CRh response within 6 months of initiating ivosidenib therapy [18]. Subgroup analyses indicated that CR/CRh response rates were consistent across all baseline demographics and disease characteristics, except for the number of prior regimens: patients who had received one prior regimen had a higher CR/CRh response rate (46%) than those who had received ≥ 3 prior regimens (15%) [21].
CR and CRh response rates and durations in the 125 patients in the primary efficacy population were similar to those observed in the total population of 179 patients with relapsed or refractory AML (i.e. primary efficacy population plus those who did meet the above relapsed/refractory AML eligibility criteria) [21]. Moreover, in the 101 patients with ≥ 1 baseline co-mutations (e.g. DNMT3A, NPM1, and/or SRSF2) receiving ivosidenib 500 mg once daily in the expansion phase, the mean number of co-occurring mutations was significantly lower in patients with a CR/CRh response than in those without such a response (1.8 vs 2.6 co-mutations; p = 0.0017). Although mutations in receptor tyrosine kinase pathway genes (e.g. NRAS, KRAS, LT3, KIT, NF1, PTPN11, BRAF, MAP2K1, and RET) occurred significantly (p = 0.003) more frequently in patients who did not achieve CR or CRh than those who did achieve CR or CRh as a best response, no specific preexisting single gene mutation was deemed a significant predictor of clinical response or resistance following treatment with ivosidenib [21].
Overall survival
Treatment with once-daily ivosidenib 500 mg was associated with encouraging rates and duration of overall survival [21]. Median overall survival was 8.8 months with a median follow-up time of 14.8 months (range 0.2–30.3 months), and in patients who achieved a CR/CRh response, the survival rate was 50.1% after 18 months of ivosidenib therapy (median not reached by the cut-off date).
Estimates of the median overall survival were 9.3 months in patients who achieved non-CR/CRh responses (i.e. CR with incomplete hematologic or platelet recovery, a morphologic leukemia-free state that did not meet the criteria for CRh, and/or partial remission), and 3.9 months in patients who did not achieve a response (i.e. stable or progressive disease) [21].
Transfusion independence
In addition to the rate and duration of CR/CRh response, US approval of ivosidenib 500 mg once daily was also based on the rate of conversion from transfusion dependence to transfusion independence [18]. Following treatment with ivosidenib, the acquisition and maintenance of transfusion independence was observed across all response categories [21]. Of the 84 patients dependent on platelet and/or red blood cell transfusion at baseline, 35% became transfusion independent for ≥ 56 days during ivosidenib therapy. Of the 41 patients not dependent on transfusions at baseline, 56% remained transfusion independent for ≥ 56 days during ivosidenib therapy [21].
Ivosidenib 500 mg once daily reduced the mean percentage of bone marrow blasts over time (≈ 50% at baseline vs ≈ 10% after twelve 28-day cycles of ivosidenib), and induced myeloid differentiation and trilineage hematopoietic recovery without a period of bone marrow aplasia (consistent with the drug’s mechanism of action) [21]. Improvements from baseline in hematologic variables were also observed over time, where the mean platelet count increased from ≈ 60 to 130 × 109/L and the mean absolute neutrophil count increased from ≈ 0.5 to ≈ 3.3 × 109/L after ≤ 12 cycles of ivosidenib therapy [21]. Patients who achieved a CR/CRh response had lower rates of exposure-adjusted febrile neutropenia (any grade) and grade 3/4 infections during ivosidenib therapy than with other responses [21].
Mutation clearance
IDH1 mutation clearance was defined as the inability to detect a mutated IDH1 (mIDH1) variant allele [variant allele frequency (VAF) cutoff of 1% as assessed using the next-generation sequencing (NGS) FoundationOne™ Heme Panel] in bone marrow mononuclear cells (BMMCs) at ≥ 1 time point during the study, using highly sensitive digital polymerase-chain-reaction technology [21]. Of the 31 patients in the expansion phase who achieved a best response of CR or CRh and who had available longitudinal mIDH1 VAF data for BMMCs and neutrophils, 23% (7 patients) had clearance of IDH1 mutations in BMMCs following treatment with ivosidenib 500 mg once daily. Over time, mean levels of IDH1 mutations in bone marrow mononuclear cells and neutrophils decreased in these patients. Clearance of IDH1 mutations was not observed in any patient who did not achieve CR/CRh with ivosidenib 500 mg once daily (n = 33) [21].
Moreover, preliminary findings suggest that patients with clearance of IDH1 mutations in BMMCs may have longer durations of response and overall survival than those without clearance [21]. The median duration of CR/CRh and overall survival were 11.1 and 14.5 months in patients with IDH1 mutation clearance, whereas, in patients who did not have IDH1 mutation clearance, the corresponding values were 6.5 and 10.2 months [21].
What is the tolerability profile of ivosidenib?
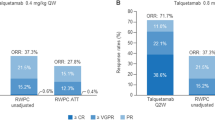
Oral ivosidenib 500 mg once daily had a generally manageable tolerability profile in the treatment of IDH1 mutation-positive relapsed or refractory AML in the phase 1 trial [21]. Out of the 179 patients who received a starting dosage of 500 mg once daily (safety population), 98.9% experienced treatment-emergent adverse events. The most common treatment-emergent adverse events were diarrhea, leukocytosis, febrile neutropenia, nausea, and fatigue (Fig. 1a).
Tolerability of ivosidenib in the treatment of IDH1 mutation-positive relapsed or refractory acute myeloid leukemia in the safety population of 179 patients receiving a starting dosage of 500 mg once daily in the phase 1 trial [21]: a treatment-emergent adverse events reported in ≥ 20% of patients; b grade 3/4 treatment-related adverse events as assessed by the investigator. IDH isocitrate dehydrogenase
Treatment-related adverse events
Treatment interruption, dosage modification, and/or permanent discontinuation may be required to manage some serious/severe adverse events related to treatment with ivosidenib (Table 1). Adverse events that have been associated with ivosidenib treatment include IDH differentiation syndrome (a boxed warning in the US prescribing information [18]), corrected QT (QTc) interval prolongation, non-infectious leukocytosis, Guillain-Barré syndrome, anemia, thrombocytopenia, diarrhea, decreased platelet counts, and hypoxia.
In the phase 1 trial, 20.7% of patients in the safety population experienced grade 3/4 events related to treatment with ivosidenib 500 mg once daily (Fig. 1b). All events were manageable with appropriate interventions [21]. Temporary treatment interruption was required by 35.2% of patients, with a median duration of interruption of 8 days (range 1–36 days). Dosage reductions to manage adverse events were uncommon, being required by only six (3.4%) patients [21]; there were two discontinuations for QTc prolongation (one serious), and one each for anemia, decreased platelet count, increased ALT, increased AST, neutropenia, thrombocytopenia, serious diarrhea, and serious nausea [21]. In the safety population, no patients permanently discontinued ivosidenib due to a treatment-related adverse event, and there were no treatment-related deaths.
Adverse events of special interest in the safety population of the phase 1 trial were as follows [21]:
-
QTc interval prolongation Treatment-emergent (any grade) reported in 24.6% of patients (Fig. 1a), and treatment-related grade 3/4 in 7.8% (Fig. 1b); 7.3% of patients required treatment interruption, and 1.1% required dosage reduction. Drugs that are known to increase the QTc interval (Table 1) were often used concomitantly with ivosidenib; 59.2% of patients received levofloxacin, 39.7% ondansetron, 35.8% voriconazole, 26.3% fluconazole, 24.6% ciprofloxacin, and 21.2% posaconazole.
-
Leukocytosis Treatment-emergent (any grade) reported in 29.6% of patients (Fig. 1a), and treatment-related grade 3/4 in 1.7% (Fig. 1b); 2.8% of patients required treatment interruption; none required dosage reduction. The time to the first onset was generally ≤ 30 days.
-
IDH differentiation syndrome Thought to be due to the rapid increase in differentiation of neutrophils following the removal of the differentiation block in the malignant myeloid clone [23], and may be life-threatening or fatal if not treated [18]. Treatment-emergent (any grade) differentiation syndrome was reported in 10.6% of patients, and treatment-related grade 3 in 3.9% (Fig. 1b), with no grade 4 events [21]. The median time to onset was 29 days (range 5–59 days). In 19 patients who required interventions (e.g. corticosteroids, diuretics, and hydroxyurea if concurrent leukocytosis), the syndrome had resolved in 17 (89.5%) by the cut-off date. Importantly, the approved US prescribing information cites a higher differentiation syndrome rate of 19% [18], which is derived from an algorithmic analysis of patient-level data from the clinical trial [24]. This analysis grouped adverse events and laboratory events using the Montesinos criteria [25].
What is the current clinical position of ivosidenib in relapsed or refractory AML?
Ivosidenib, a first-in-class small molecule inhibitor of mutant IDH1 with a convenient once-daily oral dosing regimen, is an important new option to treat adults with relapsed or refractory AML and a susceptible IDH1 mutation. At the recommended dosage of 500 mg once daily, ivosidenib produces encouraging rates and durations of CR/CRh, CR, overall response, and overall survival in adult patients with IDH1 mutation-positive relapsed or refractory AML. Additional clinical benefits are also observed in ivosidenib recipients in this patient population, including transfusion independence, improvements in hematologic variables, and deep molecular responses as measured by IDH1 mutation clearance in patients who achieved CR/CRh.
Ivosidenib 500 mg once daily has a generally manageable tolerability profile in adults with IDH1 mutation-positive relapsed or refractory AML, with the most common adverse events being diarrhea, leukocytosis, febrile neutropenia, nausea, and fatigue, and the most common grade 3/4 treatment-related events being QT interval prolongation, IDH differentiation syndrome, and anemia. Precautions should be followed to minimize the risk of potentially serious treatment-related adverse events, and to optimize the clinical response. Treatment interruption and, less frequently, dosage modification and/or treatment discontinuation may be required to manage serious/severe adverse effects.
Change history
10 June 2019
The original article has been corrected.
References
National Comprehensive Cancer Network®. NCCN clinical practice guidelines in oncology (NCCN guidelines®): acute myeloid leukemia (version 3.2018). Plymouth Meeting, PA: National Comprehensive Cancer Network®, Inc.; 2018.
Frohling S, Scholl C, Gilliland DG, et al. Genetics of myeloid malignancies: pathogenetic and clinical implications. J Clin Oncol. 2005;23(26):6285–95.
Marcucci G, Haferlach T, Dohner H. Molecular genetics of adult acute myeloid leukemia: prognostic and therapeutic implications. J Clin Oncol. 2011;29(5):475–86.
Wouters BJ, Delwel R. Epigenetics and approaches to targeted epigenetic therapy in acute myeloid leukemia. Blood. 2016;127(1):42–52.
Schoch C, Haferlach T. Cytogenetics in acute myeloid leukemia. Curr Oncol Rep. 2002;4(5):390–7.
National Cancer Institute: Surveillance, epidemiology, and End Results Program (SEER). Cancer stat facts: leukemia—acute myeloid leukemia (AML) https://seer.cancer.gov/statfacts/html/amyl.html. Accessed Feb 1 2019.
Im AP, Sehgal AR, Carroll MP, et al. DNMT3A and IDH mutations in acute myeloid leukemia and other myeloid malignancies: associations with prognosis and potential treatment strategies. Leukemia. 2014;28(9):1774–83.
Mondesir J, Willekens C, Touat M, et al. IDH1 and IDH2 mutations as novel therapeutic targets: current perspectives. J Blood Med. 2016;7:171–80.
Ward PS, Patel J, Wise DR, et al. The common feature of leukemia-associated IDH1 and IDH2 mutations is a neomorphic enzyme activity converting α-ketoglutarate to 2-hydroxyglutarate. Cancer Cell. 2010;17(3):225–34.
Dang L, White DW, Gross S, et al. Cancer-associated IDH1 mutations produce 2-hydroxyglutarate. Nature. 2009;462(7274):739–44.
Lu C, Ward PS, Kapoor GS, et al. IDH mutation impairs histone demethylation and results in a block to cell differentiation. Nature. 2012;483(7390):474–8.
Krell D, Mulholland P, Frampton AE, et al. IDH mutations in tumorigenesis and their potential role as novel therapeutic targets. Future Oncol. 2013;9(12):1923–35.
Figueroa ME, Abdel-Wahab O, Lu C, et al. Leukemic IDH1 and IDH2 mutations result in a hypermethylation phenotype, disrupt TET2 function, and impair hematopoietic differentiation. Cancer Cell. 2010;18(6):553–67.
DiNardo CD, Ravandi F, Agresta S, et al. Characteristics, clinical outcome, and prognostic significance of IDH mutations in AML. Am J Hematol. 2015;90(8):732–6.
Dohner H, Estey EH, Amadori S, et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood. 2010;115(3):453–74.
Bullinger L, Dohner K, Dohner H. Genomics of acute myeloid leukemia diagnosis and pathways. J Clin Oncol. 2017;35(9):934–46.
Schwaederle M, Zhao M, Lee JJ, et al. Impact of precision medicine in diverse cancers: a meta-analysis of phase II clinical trials. J Clin Oncol. 2015;33(32):3817–25.
Tibsovo® (ivosidenib) tablets, for oral use: US prescribing information. Cambridge: Agios Pharmaceuticals Inc.; 2018.
Popovici-Muller J, Lemieux RM, Artin E, et al. Discovery of AG-120 (ivosidenib): a first-in-class mutant IDH1 inhibitor for the treatment of IDH1 mutant cancers. ACS Med Chem Lett. 2018;9(4):300–5.
IDH program. Cambridge: Agios Pharmaceuticals Inc.; 2018. https://agios.com/pipeline/idh-program. Accessed 1 Feb 2019.
DiNardo CD, Stein EM, de Botton S, et al. Durable remissions with ivosidenib in IDH1-mutated relapsed or refractory AML. N Engl J Med. 2018;378(25):2386–98.
Cheson BD, Bennett JM, Kopecky KJ, et al. Revised recommendations of the International Working Group for diagnosis, standardization of response criteria, treatment outcomes, and reporting standards for therapeutic trials in acute myeloid leukemia. J Clin Oncol. 2003;21(24):4642–9.
Birendra KC, DiNardo CD. Evidence for clinical differentiation and differentiation syndrome in patients with acute myeloid leukemia and IDH1 mutations treated with the targeted mutant IDH1 inhibitor, AG-120. Clin Lymphoma Myeloma Leuk. 2016;16(8):460–5.
Norsworthy JK, Mulkey F, Ward AF, et al. Incidence of differentiation syndrome with ivosidenib (IVO) and enasidenib (ENA) for treatment of patients with relapsed or refractory (R/R) isocitrate dehydrogenase (IDH)1- or IDH2-mutated acute myeloid leukemia (AML): a systematic analysis by the U.S. Food and Drug Administration (FDA) [abstract no. 288]. In: 60th American Society of Hematology Annual Meeting. 2018.
Montesinos P, Bergua JM, Vellenga E, et al. Differentiation syndrome in patients with acute promyelocytic leukemia treated with all-trans retinoic acid and anthracycline chemotherapy: characteristics, outcome, and prognostic factors. Blood. 2009;113(4):775–83.
Acknowledgements
The manuscript was reviewed by: G. N. Mannis, Hematology/Blood and Marrow Transplant, Department of Medicine, University of California, San Francisco, CA, USA; A. S. Mims, Division of Hematology, Department of Medicine, Ohio State University, Columbus, OH, USA. During the peer review process, Agios Inc., the marketing-authorization holder of ivosidenib (Tibsovo®), was also offered an opportunity to provide a scientific accuracy review of their data. Changes resulting from comments received were made on the basis of scientific and editorial merit.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The preparation of this review was not supported by any external funding.
Conflicts of interest
E.H. McCafferty and K.A. Lyseng-Williamson are employees of Adis/Springer, are responsible for the article content and declare no conflicts of interest.
Additional information
The original version of this article was revised due to a retrospective Open Access request.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
About this article
Cite this article
McCafferty, E.H., Lyseng-Williamson, K.A. Ivosidenib in relapsed or refractory acute myeloid leukemia: a profile of its use in the USA. Drugs Ther Perspect 35, 160–166 (2019). https://doi.org/10.1007/s40267-019-00610-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40267-019-00610-2