Abstract
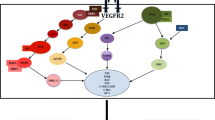
Ramucirumab (Cyramza®), a fully human anti-VEGFR-2 monoclonal antibody, has been approved as monotherapy for the treatment of patients with hepatocellular carcinoma (HCC) and α-fetoprotein levels ≥ 400 ng/mL who have been treated with sorafenib. Ramucirumab significantly prolonged overall survival (OS) and progression-free survival (PFS) relative to placebo in this population in the randomized, double-blind phase 3 REACH 2 trial. These benefits were seen in key prespecified subgroups based on demographic and disease characteristics. Ramucirumab had an acceptable tolerability profile and manageable safety profile in these patients, with the majority of treatment-related adverse events being mild or moderate in severity. The safety profile of ramucirumab was consistent with that expected for agents targeting the VEGF/VEGFR axis. Currently, ramucirumab is the only therapy specifically tested in patients with α-fetoprotein levels ≥ 400 ng/mL, which is associated with an aggressive disease and poor prognosis. Therefore, ramucirumab is an important treatment option for patients with HCC and α-fetoprotein levels ≥ 400 ng/mL who have been treated with sorafenib.

Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424.
Villanueva A. Hepatocellular carcinoma. N Engl J Med. 2019;380(15):1450–62.
Galle PR, Foerster F, Kudo M, et al. Biology and significance of alpha-fetoprotein in hepatocellular carcinoma. Liver Int. 2019;39:2214–29.
National Comprehensive Cancer Network. NCCN clinical practice guidelines in oncology: hepatobiliary cancers (version 3.2019). 2019. https://www.nccn.org. Accessed 17 Jan 2020.
EASL clinical practice guidelines. management of hepatocellular carcinoma. J Hepatol. 2018;69(1):182–236.
Vogel A, Cervantes A, Chau I, et al. Hepatocellular carcinoma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2018;29(Suppl 4):iv238–55.
Marrero JA, Kulik LM, Sirlin CB, et al. Diagnosis, staging, and management of hepatocellular carcinoma: 2018 practice guidance by the American Association for the Study of Liver Diseases. Hepatology. 2018;68(2):723–50.
Omata M, Cheng AL, Kokudo N, et al. Asia-Pacific clinical practice guidelines on the management of hepatocellular carcinoma: a 2017 update. Hepatol Int. 2017;11(4):317–70.
Vogel A, Cervantes A, Chau I, et al. Hepatocellular carcinoma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2019;30(5):871–3.
European Medicines Agency. Cyramza 10 mg/ml concentrate for solution for infusion: EU summary of product characteristics; 2015. https://www.ema.europa.eu. Accessed 17 Jan 2020.
Eli Lilly. Cyramza (ramucirumab) injection, for intravenous use: US prescribing information; 2019. https://www.cyramza.com/. Accessed 17 Jan 2020.
Eli Lilly. Cyramza intravenous infusion 100 mg/500 mg: Japanese prescribing information; 2019. http://www.pmda.go.jp/PmdaSearch/iyakuDetail/530471_4291429A1023_1_13#WARNINGS. Accessed 17 Jan 2020.
Miao HQ, Hu K, Jimenez X, et al. Potent neutralization of VEGF biological activities with a fully human antibody Fab fragment directed against VEGF receptor 2. Biochem Biophys Res Commun. 2006;345(1):438–45.
European Medicines Agency. Cyramza (ramucirumab): Committee for Medicinal Products for Human Use assessment report; 2014. https://www.ema.europa.eu. Accessed 17 Jan 2020.
Lu D, Shen J, Vil MD, et al. Tailoring in vitro selection for a picomolar affinity human antibody directed against vascular endothelial growth factor receptor 2 for enhanced neutralizing activity. J Biol Chem. 2003;278(44):43496–507.
Zhu Z, Hattori K, Zhang H, et al. Inhibition of human leukemia in an animal model with human antibodies directed against vascular endothelial growth factor receptor 2. Correlation between antibody affinity and biological activity. Leukemia. 2003;17(3):604–11.
Prewett M, Huber J, Li Y, et al. Antivascular endothelial growth factor receptor (fetal liver kinase 1) monoclonal antibody inhibits tumor angiogenesis and growth of several mouse and human tumors. Cancer Res. 1999;59(20):5209–18.
Chiorean EG, Hurwitz HI, Cohen RB, et al. Phase I study of every 2- or 3-week dosing of ramucirumab, a human immunoglobulin G1 monoclonal antibody targeting the vascular endothelial growth factor receptor-2 in patients with advanced solid tumors. Ann Oncol. 2015;26(6):1230–7.
Spratlin JL, Cohen RB, Eadens M, et al. Phase I pharmacologic and biologic study of ramucirumab (IMC-1121B), a fully human immunoglobulin G1 monoclonal antibody targeting the vascular endothelial growth factor receptor-2. J Clin Oncol. 2010;28(5):780–7.
Nokihara H, Yamamoto N, Yamada Y, et al. A phase 1 study of ramucirumab in Japanese patients with advanced solid tumors. Jpn J Clin Oncol. 2017;47(4):298–305.
Zhu AX, Finn RS, Mulcahy M, et al. A phase II and biomarker study of ramucirumab, a human monoclonal antibody targeting the VEGF receptor-2, as first-line monotherapy in patients with advanced hepatocellular cancer. Clin Cancer Res. 2013;19(23):6614–23.
Cao J, Ji D, Chen Z, et al. Phase I dose-escalation study of ramucirumab in Chinese patients with advanced solid tumors. Oncologist. 2017;22(6):638-e56.
Llovet J, Kudo M, Kang Y-K, et al. Ramucirumab in patients with advanced hepatocellular carcinoma (HCC) and elevated alpha fetoprotein (AFP): an exposure-response analysis [abstract no. 758P]. Ann Oncol. 2019;30(Suppl 5):v293–4.
Zhu AX, Kang YK, Yen CJ, et al. Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased alpha-fetoprotein concentrations (REACH-2): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2019;20(2):282–96.
Zhu AX, Park JO, Ryoo BY, et al. Ramucirumab versus placebo as second-line treatment in patients with advanced hepatocellular carcinoma following first-line therapy with sorafenib (REACH): a randomised, double-blind, multicentre, phase 3 trial. Lancet Oncol. 2015;16(7):859–70.
Galle P, Kudo M, Llovet JM, et al. Ramucirumab for patients with advanced hepatocellular carcinoma and elevated alpha-fetoprotein following sorafenib: outcomes by liver disease aetiology from two randomised, placebo-controlled phase 3 studies (REACH-2 and REACH) [abstract no. GS-09 plus poster]. J Hepatol. 2019;70(Suppl 1):e46.
Kang YK, Kudo M, Lim HY, et al. Efficacy and safety of ramucirumab (RAM) in Asian and non-Asian patients with advanced hepatocellular carcinoma (HCC) and elevated alpha-fetoprotein (AFP): subgroup analysis from two randomized studies [abstract no. 149O]. Ann Oncol. 2018;29(Suppl 9).
Kudo M, Okusaka T, Motomura K, et al. Ramucirumab as second-line treatment in patients with advanced hepatocellular carcinoma (HCC) and elevated alpha-fetoprotein (AFP) following first-line sorafenib: pooled efficacy and safety in Japanese patients across two global randomized phase III studies (REACH-2 and REACH) [abstract no. 320]. J Clin Oncol. 2019;37(Suppl 4):320.
Llovet JM, Yen CJ, Finn RS, et al. Ramucirumab (RAM) for sorafenib intolerant patients with hepatocellular carcinoma (HCC) and elevated baseline alpha fetoprotein (AFP): outcomes from two randomized phase 3 studies (REACH, REACH2) [abstract no. 4073]. J Clin Oncol. 2019;37(Suppl 15):4073.
Meyer T, Finn R, Kudo M, et al. Ramucirumab in advanced hepatocellular carcinoma and elevated alpha-fetoprotein following sorafenib: outcomes by prior transarterial chemoembolisation from two randomised, double-blind, placebo-controlled phase 3 studies (REACH-2 and REACH) [abstract no. O-021]. Ann Oncol. 2019;30(Suppl 4):iv133.
Zhu AX, Finn RS, Galle PR, et al. Ramucirumab as second-line treatment in patients with advanced hepatocellular carcinoma (HCC) and elevated alpha-fetoprotein (AFP) following first-line sorafenib: patient reported outcome results across two phase III studies (REACH-2 and REACH) [abstract no. 622PD plus poster]. Ann Oncol. 2018;29(Suppl 8):viii208.
Brandi G, Kudo M, Kang Y, et al. Ramucirumab for patients with hepatocellular carcinoma and elevated alpha-fetoprotein following sorafenib treatment: exploratory analysis of REACH-2 trial results by albumin-bilirubin grade and Child-Pugh score [abstract no. OP-7]. In: European Association for the Study of the Liver HCC Summit; 2019.
Kudo M, Galle PR, Brandi G, et al. Effect of ramucirumab on albumin-bilirubin grade during treatment of patients with hepatocellular carcinoma and elevated alpha-fetoprotein following sorafenib: outcomes from two randomized phase 3 studies (REACH, REACH-2) [abstract no. P-066]. In: 13th Annual Conference of the International Liver Cancer Association; 2019.
Kudo M, Galle PR, Motomura K, et al. Efficacy and safety of ramucirumab for advanced hepatocellular carcinoma with elevated alpha-fetoprotein following sorafenib across age subgroups in two global phase 3 trials (REACH, REACH-2) [abstract no. 757P]. Ann Oncol. 2019;30(Suppl 5).
Llovet JM, Montal R, Sia D, et al. Molecular therapies and precision medicine for hepatocellular carcinoma. Nat Rev Clin Oncol. 2018;15(10):599–616.
Zhu AX, Galle PR, Llovet JM, et al. Prognostic and predictive value of baseline alpha-fetoprotein (AFP) in patients with advanced hepatocellular carcinoma (HCC) treated with ramucirumab from two phase III studies (REACH, REACH-2) [abstract no. 753P]. Ann Oncol. 2019;30(Suppl 5):v289–90.
Montal R, Andreu-Oller C, Bassaganyas L, et al. Molecular portrait of high alpha-fetoprotein in hepatocellular carcinoma: implications for biomarker-driven clinical trials. Br J Cancer. 2019;121(4):340–3.
Zhu RX, Seto WK, Lai CL, et al. Epidemiology of hepatocellular carcinoma in the Asia-Pacific region. Gut Liver. 2016;10(3):332–9.
Zhu AX, Galle PR, Kudo M, et al. A study of ramucirumab (LY3009806) versus placebo in patients with hepatocellular carcinoma and elevated baseline alphafetoprotein (REACH-2) [abstract no. TPS538]. J Clin Oncol. 2018;36(Suppl 4).
Bruix J, Qin S, Merle P, et al. Regorafenib for patients with hepatocellular carcinoma who progressed on sorafenib treatment (RESORCE): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2017;389(10064):56–66.
Kuzuya T, Ishigami M, Ito T, et al. Clinical characteristics and outcomes of candidates for second-line therapy, including regorafenib and ramucirumab, for advanced hepatocellular carcinoma after sorafenib treatment. Hepatol Res. 2019;49(9):1054–65.
Acknowledgements
During the peer review process, the manufacturer of ramucirumab was also offered an opportunity to review this article. Changes resulting from comments received were made on the basis of scientific and editorial merit.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The preparation of this review was not supported by any external funding.
Conflict of interest
Yahiya Syed is a salaried employee of Adis International Ltd/Springer Nature, is responsible for the article content and declares no relevant conflicts of interest.
Additional information
Enhanced material for this Adis Drug Evaluation can be found at https://doi.org/10.6084/m9.figshare.11374896.
The manuscript was reviewed by:G. G. Di Costanzo, Department of Transplantation, Liver Unit, Cardarelli Hospital, Naples, Italy; J. Edeline, Medical Oncology Department, Centre Eugène Marquis, Rennes, France; M. Fukudo, Department of Hospital Pharmacy and Pharmacology, Asahikawa Medical University, Hokkaido, Japan; M. Nakano, Division of Gastroenterology, Department of Medicine, Kurume University School of Medicine, Kurume, Fukuoka, Japan; M. Peck-Radosavljevic, Department of Internal Medicine & Gastroenterology (IMuG), Hepatology, Endocrinology, Rheumatology and Nephrology with Centralized Emergency Department (ZAE), Klinikum Klagenfurt am Wörthersee, Klagenfurt, Austria; L. Rimassa, Department of Biomedical Sciences, Humanitas University, Milan, Italy; Humanitas Cancer Center, Humanitas Clinical and Research Center-IRCCS, Milan, Italy.
Rights and permissions
About this article
Cite this article
Syed, Y.Y. Ramucirumab: A Review in Hepatocellular Carcinoma. Drugs 80, 315–322 (2020). https://doi.org/10.1007/s40265-020-01263-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-020-01263-6