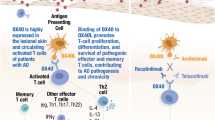
Abstract
Introduction
Several case studies have reported an association between antifungal drug use and psoriasis risk.
Objective
The objective of this study was to investigate the association between terbinafine/itraconazole exposure and psoriasis incidence.
Methods
Among patients with onychomycosis in the Taiwan National Health Insurance Research Database, 3831 incident psoriasis cases were identified during 2004–2010 and compared with 3831 age- and sex-matched controls with the same look-back period. Multivariate conditional logistic regression was used for the analysis.
Results
The psoriasis cases were significantly more likely than matched controls to have used terbinafine or itraconazole (59.85 vs. 42.70%, respectively; p < 0.0001). After adjusting for potential confounders and cumulative duration of antifungal drug prescription, terbinafine/itraconazole use was associated with an increased psoriasis risk (adjusted odds ratio 1.33, 95% confidence interval 1.15–1.54). The association was stronger for more recent drug exposure (adjusted odds ratio 2.96, 95% confidence interval 2.25–3.90 for ≤ 90 days before the sampling date; adjusted odds ratio 1.04, 95% confidence interval 0.89–1.22 for > 360 days). In a comparison of patients receiving terbinafine or itraconazole only, psoriasis risk was higher for itraconazole (adjusted odds ratio 1.21, 95% confidence interval 1.05–1.40).
Conclusion
This large population-based case-control analysis showed that exposure to terbinafine or itraconazole is associated with an increased risk of incident psoriasis. The finding of an increased psoriasis risk for antifungal drug users, particularly for itraconazole, deserves attention in clinical practice although further prospective studies are necessary to confirm our findings and clarify the biological mechanisms that underlie these associations.



Similar content being viewed by others
References
Boehncke WH, Schon MP. Psoriasis. Lancet. 2015;386(9997):983–94.
Chiu HY, Cheng YP, Tsai TF. T helper type 17 in psoriasis: from basic immunology to clinical practice. Dermatol Sin. 2012;30(4):136–41.
Nestle FO, Kaplan DH, Barker J. Psoriasis. N Engl J Med. 2009;361(5):496–509.
Kim GK, Del Rosso JQ. Drug-provoked psoriasis: is it drug induced or drug aggravated?: understanding pathophysiology and clinical relevance. J Clin Aesthet Dermatol. 2010;3(1):32–8.
Fry L, Baker BS. Triggering psoriasis: the role of infections and medications. Clin Dermatol. 2007;25(6):606–15.
Armstrong AW. Psoriasis provoked or exacerbated by medications: identifying culprit drugs. JAMA Dermatol. 2014;150(9):963.
Brauchli YB, Jick SS, Curtin F, Meier CR. Association between beta-blockers, other antihypertensive drugs and psoriasis: population-based case-control study. Br J Dermatol. 2008;158(6):1299–307.
Brauchli YB, Jick SS, Meier CR. Statin use and risk of first-time psoriasis diagnosis. J Am Acad Dermatol. 2011;65(1):77–83.
Basavaraj KH, Ashok NM, Rashmi R, Praveen TK. The role of drugs in the induction and/or exacerbation of psoriasis. Int J Dermatol. 2010;49(12):1351–61.
Szepietowski JC. Terbinafine exacerbates psoriasis: case report with a literature review. Acta Dermatovenerol Croat. 2003;11(1):17–21.
Wilson NJ, Evans S. Severe pustular psoriasis provoked by oral terbinafine. Br J Dermatol. 1998;139(1):168.
Gupta AK, Sibbald RG, Knowles SR, Lynde CW, Shear NH. Terbinafine therapy may be associated with the development of psoriasis de novo or its exacerbation: four case reports and a review of drug-induced psoriasis. J Am Acad Dermatol. 1997;36(5 Pt 2):858–62.
Mizuno K, Fukami T, Toyoda Y, Nakajima M, Yokoi T. Terbinafine stimulates the pro-inflammatory responses in human monocytic THP-1 cells through an ERK signaling pathway. Life Sci. 2010;87(17–18):537–44.
Mihu MR, Pattabhi R, Nosanchuk JD. The impact of antifungals on toll-like receptors. Front Microbiol. 2014;5:99.
Kanda N, Kano R, Ishikawa T, Watanabe S. The antimycotic drugs itraconazole and terbinafine hydrochloride induce the production of human beta-defensin-3 in human keratinocytes. Immunobiology. 2011;216(4):497–504.
Sweeney CM, Russell SE, Malara A, Kelly G, Hughes R, Tobin AM, et al. Human ß-defensin 3 and its mouse ortholog murine ß-defensin 14 activate Langerhans cells and exacerbate psoriasis-like skin inflammation in mice. J Investig Dermatol. 2016;136(3):723–7.
Kasperkiewicz M, Anemuller W, Angelova-Fischer I, Rose C, Zillikens D, Fischer TW. Subacute cutaneous lupus erythematosus associated with terbinafine. Clin Exp Dermatol. 2009;34(7):e403–4.
McKellar G, Porter D, Burden D. Terbinafine as a cause of cutaneous lupus erythematosus. Rheumatology (Oxford). 2004;43(2):249.
Magro CM, Schaefer JT, Waldman J, Knight D, Seilstad K, Hearne D. Terbinafine-induced dermatomyositis: a case report and literature review of drug-induced dermatomyositis. J Cutan Pathol. 2008;35(1):74–81.
Kanda N, Enomoto U, Watanabe S. Anti-mycotics suppress interleukin-4 and interleukin-5 production in anti-CD3 plus anti-CD28-stimulated T cells from patients with atopic dermatitis. J Investig Dermatol. 2001;117(6):1635–46.
Gimenes VM, Criado PR, Martins JE, Almeida SR. Cellular immune response of patients with chromoblastomycosis undergoing antifungal therapy. Mycopathologia. 2006;162(2):97–101.
Chiu HY, Huang HL, Li CH, Yin YJ, Chen HA, Hsu ST, et al. Increased risk of glomerulonephritis and chronic kidney disease in relation to the severity of psoriasis, concomitant medication, and comorbidity: a nationwide population-based cohort study. Br J Dermatol. 2015;173(1):146–54.
Chang YT, Chen TJ, Liu PC, Chen YC, Chen YJ, Huang YL, et al. Epidemiological study of psoriasis in the national health insurance database in Taiwan. Acta Derm Venereol. 2009;89(3):262–6.
Tsai TF, Wang TS, Hung ST, Tsai PI, Schenkel B, Zhang M, et al. Epidemiology and comorbidities of psoriasis patients in a national database in Taiwan. J Dermatol Sci. 2011;63(1):40–6.
Chiu HY, Huang HL, Li CH, Chen HA, Yeh CL, Chiu SH, et al. Increased risk of chronic kidney disease in rheumatoid arthritis associated with cardiovascular complications: a national population-based cohort study. PLoS One. 2015;10(9):e0136508.
Kim ES, Han K, Kim MK, Park YM, Baek KH, Moon SD, et al. Impact of metabolic status on the incidence of psoriasis: a Korean nationwide cohort study. Sci Rep. 2017;7(1):1989.
Picard D, Benichou J, Sin C, Abasq C, Houivet E, Koning R, et al. Increased prevalence of psoriasis in patients with coronary artery disease: results from a case-control study. Br J Dermatol. 2014;171(3):580–7.
Wu S, Han J, Li WQ, Qureshi AA. Hypertension, antihypertensive medication use, and risk of psoriasis. JAMA Dermatol. 2014;150(9):957–63.
Kim BS, Jang HS, Jwa SW, Jang BS, Kim MB, Oh CK, et al. Generalized pustular psoriasis and hepatic dysfunction associated with oral terbinafine therapy. J Korean Med Sci. 2007;22(1):167–9.
Gupta AK, Lynde CW, Lauzon GJ, Mehlmauer MA, Braddock SW, Miller CA, et al. Cutaneous adverse effects associated with terbinafine therapy: 10 case reports and a review of the literature. Br J Dermatol. 1998;138(3):529–32.
Bowcock AM, Krueger JG. Getting under the skin: the immunogenetics of psoriasis. Nat Rev Immunol. 2005;5(9):699–711.
Stuart PE, Nair RP, Ellinghaus E, Ding J, Tejasvi T, Gudjonsson JE, et al. Genome-wide association analysis identifies three psoriasis susceptibility loci. Nat Genet. 2010;42(11):1000–4.
Hsieh YJ, Chang YC, Huang YH, Chung WH, Tsai HY, Hsu LA. A lack of association between genetic polymorphisms in beta-defensins and susceptibility of psoriasis in Taiwanese: a case-control study. Dermatol Sin. 2016;34(2):78–82.
Chiu HY, Huang PY, Jee SH, Hu CY, Chou CT, Chang YT, et al. HLA polymorphism among Chinese patients with chronic plaque psoriasis: subgroup analysis. Br J Dermatol. 2012;166(2):288–97.
Duffy DL, Spelman LS, Martin NG. Psoriasis in Australian twins. J Am Acad Dermatol. 1993;29(3):428–34.
Lin HY, Hsu CH, Cheng ST, Chang CH. Imatinib-induced exacerbation of psoriasis in a patient with recurrent dermatofibrosarcoma protuberans: a case report and review of the literature. Dermatol Sin. 2016;34(1):26–8.
Hsu MC, Chen CC. Psoriasis flare-ups following sorafenib therapy: a rare case. Dermatol Sin. 2016;34(3):148–50.
Tsankov N, Angelova I, Kazandjieva J. Drug-induced psoriasis: recognition and management. Am J Clin Dermatol. 2000;1(3):159–65.
Imafuku S, Nakayama J. Profile of patients with psoriasis associated with hepatitis C virus infection. J Dermatol. 2013;40(6):428–33.
Nestle FO, Conrad C, Tun-Kyi A, Homey B, Gombert M, Boyman O, et al. Plasmacytoid predendritic cells initiate psoriasis through interferon-alpha production. J Exp Med. 2005;202(1):135–43.
Kelly R, Marsden RA, Bevan D. Exacerbation of psoriasis with GM-CSF therapy. Br J Dermatol. 1993;128(4):468–9.
Cho SG, Park YM, Moon H, Kim KM, Bae SS, Kim GB, et al. Psoriasiform eruption triggered by recombinant granulocyte-macrophage colony stimulating factor (rGM-CSF) and exacerbated by granulocyte colony stimulating factor (rG-CSF) in a patient with breast cancer. J Korean Med Sci. 1998;13(6):685–8.
Feliu J, Diaz R, Contreras F, Casado M, Espinosa E, Baron MG. Worsening psoriasis after treatment with G-CSF in a patient with small-cell lung cancer. J Natl Cancer Inst. 1997;89(17):1315–6.
Wollina U, Hansel G, Koch A, Schonlebe J, Kostler E, Haroske G. Tumor necrosis factor-alpha inhibitor-induced psoriasis or psoriasiform exanthemata: first 120 cases from the literature including a series of six new patients. Am J Clin Dermatol. 2008;9(1):1–14.
Sfikakis PP, Iliopoulos A, Elezoglou A, Kittas C, Stratigos A. Psoriasis induced by anti-tumor necrosis factor therapy: a paradoxical adverse reaction. Arthritis Rheum. 2005;52(8):2513–8.
Sari I, Akar S, Birlik M, Sis B, Onen F, Akkoc N. Anti-tumor necrosis factor-alpha-induced psoriasis. J Rheumatol. 2006;33(7):1411–4.
Hampton PJ, Jans R, Flockhart RJ, Parker G, Reynolds NJ. Lithium regulates keratinocyte proliferation via glycogen synthase kinase 3 and NFAT2 (nuclear factor of activated T cells 2). J Cell Physiol. 2012;227(4):1529–37.
Chiu HY, Chang WL, Huang WF, Wen YW, Tsai YW, Tsai TF. Increased risk of arrhythmia in patients with psoriatic disease: a nationwide population-based matched cohort study. J Am Acad Dermatol. 2015;73(3):429–38.
Chiu HY, Lo PC, Huang WF, Tsai YW, Tsai TF. Increased risk of aortic aneurysm (AA) in relation to the severity of psoriasis: a national population-based matched-cohort study. J Am Acad Dermatol. 2016;75(4):747–54.
Hari A, Flach TL, Shi Y, Mydlarski PR. Toll-like receptors: role in dermatological disease. Mediat Inflamm. 2010;2010:437246.
Seung NR, Park EJ, Kim CW, Kim KH, Kim KJ, Cho HJ, et al. Comparison of expression of heat-shock protein 60, Toll-like receptors 2 and 4, and T-cell receptor gammadelta in plaque and guttate psoriasis. J Cutan Pathol. 2007;34(12):903–11.
Gupta AK, Lynde CW, Jain HC, Sibbald RG, Elewski BE, Daniel CR 3rd, et al. A higher prevalence of onychomycosis in psoriatics compared with non-psoriatics: a multicentre study. Br J Dermatol. 1997;136(5):786–9.
Rigopoulos D, Papanagiotou V, Daniel R 3rd, Piraccini BM. Onychomycosis in patients with nail psoriasis: a point to point discussion. Mycoses. 2017;60(1):6–10.
Rizzo D, Alaimo R, Tilotta G, Dinotta F, Bongiorno MR. Incidence of onychomycosis among psoriatic patients with nail involvement: a descriptive study. Mycoses. 2013;56(4):498–9.
Martini K, Muller H, Huemer HP, Hopfl R. Nail psoriasis masqueraded by secondary infection with Rhodotorula mucilaginosa. Mycoses. 2013;56(6):690–2.
Lin CC, Lai MS, Syu CY, Chang SC, Tseng FY. Accuracy of diabetes diagnosis in health insurance claims data in Taiwan. J Formos Med Assoc. 2005;104(3):157–63.
Cheng CL, Kao YH, Lin SJ, Lee CH, Lai ML. Validation of the National Health Insurance Research Database with ischemic stroke cases in Taiwan. Pharmacoepidemiol Drug Saf. 2011;20(3):236–42.
Asgari MM, Wu JJ, Gelfand JM, Salman C, Curtis JR, Harrold LR, et al. Validity of diagnostic codes and prevalence of psoriasis and psoriatic arthritis in a managed care population, 1996–2009. Pharmacoepidemiol Drug Saf. 2013;22(8):842–9.
Kao WY, Su CW, Huang YS, Chou YC, Chen YC, Chung WH, et al. Risk of oral antifungal agent-induced liver injury in Taiwanese. Br J Clin Pharmacol. 2014;77(1):180–9.
Chen YJ, Wu CY, Chen TJ, Shen JL, Chu SY, Wang CB, et al. The risk of cancer in patients with psoriasis: a population-based cohort study in Taiwan. J Am Acad Dermatol. 2011;65(1):84–91.
Horwitz RI, Feinstein AR. The problem of “protopathic bias” in case-control studies. Am J Med. 1980;68(2):255–8.
Faillie JL. Indication bias or protopathic bias? Br J Clin Pharmacol. 2015;80(4):779–80.
Acknowledgements
We thank Prof. Weng-Foung Huang and the National Health Research Institutes for providing data. This study is based in part on data from the National Health Insurance Research Database provided by the National Health Insurance Administration, Ministry of Health and Welfare and managed by National Health Research Institutes. The interpretation and conclusions contained herein do not represent those of the National Health Insurance Administration, Ministry of Health and Welfare or National Health Research Institutes.
Author information
Authors and Affiliations
Contributions
Conception and design: H-YC, W-LC, T-FT, Y-WT, M-NS. Acquisition of data: W-LC, Y-WT, M-NS. Analysis and interpretation of the data: H-YC, W-LC, T-FT, Y-WT, M-NS. Drafting of the article: H-YC, W-LC, T-FT. Critical revision of the article for important intellectual content: T-FT, Y-WT, M-NS. Obtaining of funding: H-YC, T-FT. Final approval of the article: H-YC, W-LC, T-FT, Y-WT, M-NS.
Corresponding author
Ethics declarations
Funding
This study was funded in part by grants from National Taiwan University Hospital (105-S3196), National Taiwan University Hospital Hsin-Chu branch (106-HCH002), and the Ministry of Science and Technology, Taiwan (formerly, the National Science Council; grant numbers, MOST104-2314-B-002-117-MY3). The researchers were independent of the funders in designing the study, collecting and analyzing the data, interpreting the results, writing the manuscript, and deciding to submit the article for publication.
Conflict of interest
Wei-Lun Chang, Yi-Wen Tsai, and Ming-Neng Shiu have no conflicts of interest directly relevant to the content of this study. Hsien-Yi Chiu has received speaking fees from AbbVie, Janssen-Cilag Pharmaceutical, Novartis, and Pfizer. Tsen-Fang Tsai has conducted clinical trials or received honoraria for serving as a consultant for Pfizer, Eli Lilly, Galderma, Celgene, Novartis, and Janssen-Cilag Pharmaceutical and has received speaking fees from AbbVie.
Ethics approval
The study protocol was reviewed and approved by the local Institutional Review Board of National Taiwan University Hospital, Hsin-Chu, Taiwan (No. 103-024-E).
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chiu, HY., Chang, WL., Tsai, TF. et al. Risk of Psoriasis Following Terbinafine or Itraconazole Treatment for Onychomycosis: A Population-Based Case-Control Comparative Study. Drug Saf 41, 285–295 (2018). https://doi.org/10.1007/s40264-017-0614-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-017-0614-2