Abstract
Introduction
Preemptive and multi-variant genotyping is suggested to improve the safety of patient drug therapy. The number of South Koreans who would benefit from this approach is unknown.
Objective
We aimed to quantify the number of patients who may experience serious adverse drug events (ADEs) due to high-risk pharmacogenetic variants and who may benefit from preemptive genotyping.
Methods
The health claims dataset of the Korean Health Insurance Review and Assessment service for 3 % of the South Korean population for year 2011 was used to calculate the number of patients exposed to 84 drugs covered by National Health Insurance with pharmacogenomic biomarkers. The product of ADE risk-conferring genotype prevalence, ADE prevalence rates, and genotype effect sizes in South Koreans or East Asians derived from published literature and the 1000 Genomes Project, and the drug exposure data were solved to estimate the number of South Koreans in whom preemptive genotyping may prevent serious ADEs.
Results
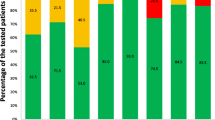
Among 1,341,077 patients in the dataset with prescriptions, 47.4 % were prescribed a drug whose response was affected by genetic variants and 31.9 % were prescribed at least one drug with serious ADEs modulated by these variants. Without genetic testing, the number of South Korean patients predicted to experience serious ADEs due to their higher ADE risk genotypes was estimated at 729. Extrapolating this to the total South Korean population indicated that approximately 24,300 patients in 2011 might have benefitted from preemptive genotyping.
Conclusions
This study quantified the number of South Korean patients predicted to have serious ADEs and demonstrated the need for preemptive genotyping to assist safer drug therapy in South Korea.



Similar content being viewed by others
References
Abul-Husn NS, Obeng AO, Sanderson SC, Gottesman O, Scott SA. Implementation and utilization of genetic testing in personalized medicine. Pharmgenomics Pers Med. 2014. doi:10.2147/PGPM.S48887.
Scott SA. Personalizing medicine with clinical pharmacogenetics. Genet Med. 2011;13(12):987–95. doi:10.1097/GIM.0b013e318238b38c.
Hoffman JM, Haidar CE, Wilkinson MR, Crews KR, Baker DK, Kornegay NM, et al. PG4KDS: a model for the clinical implementation of pre-emptive pharmacogenetics. Am J Med Genet C Semin Med Genet. 2014;166C(1):45–55. doi:10.1002/ajmg.c.31391.
Pulley JM, Denny JC, Peterson JF, Bernard GR, Vnencak-Jones CL, Ramirez AH, et al. Operational implementation of prospective genotyping for personalized medicine: the design of the Vanderbilt PREDICT project. Clin Pharmacol Ther. 2012;92(1):87–95. doi:10.1038/clpt.2011.371.
Anon. National action plan for adverse drug event prevention. Inhealth.gov. Office of Disease Prevention and Health Promotion. 2016. http://health.gov/hcq/ade.asp. Accessed 2 Jun 2016.
Bates DW, Cullen DJ, Laird N, Petersen LA, Small SD, Servi D, et al. Incidence of adverse drug events and potential adverse drug events. Implications for prevention. ADE Prevention Study Group. JAMA. 1995;274(1):29–34.
Yoo TW, Kim BI, Kim JB, Kim DJ, Kim JW, Baik SK, et al. The survey for the actual condition of drug medication and development of health care cost associated with toxic liver injury in Korean: a multicenter study for the detection and the development of nationwide reporting system of toxic liver injury. Korean J Hepatol. 2007;13(1):34–43.
Park J, Jeong J, Hwang S. Cost-effectiveness analysis of linezolid versus vancomycin in hospital-acquired pneumonia caused by methicillin-resistant Staphylococcus aureus. JoHTA. 2015;3(2):99–106.
Schildcrout JS, Denny JC, Bowton E, Gregg W, Pulley JM, Basford MA, et al. Optimizing drug outcomes through pharmacogenetics: a case for preemptive genotyping. Clin Pharmacol Ther. 2012;92(2):235–42. doi:10.1038/clpt.2012.66.
Dunnenberger HM, Crews KR, Hoffman JM, Caudle KE, Broeckel U, Howard SC, et al. Preemptive clinical pharmacogenetics implementation: current programs in five US medical centers. Annu Rev Pharmacol Toxicol. 2015;55:89–106. doi:10.1146/annurev-pharmtox-010814-124835.
Bielinski SJ, Olson JE, Pathak J, Weinshilboum RM, Wang L, Lyke KJ, et al. Preemptive genotyping for personalized medicine: design of the right drug, right dose, right time-using genomic data to individualize treatment protocol. Mayo Clin Proc. 2014;89(1):25–33. doi:10.1016/j.mayocp.2013.10.021.
Van Driest SL, Shi Y, Bowton EA, Schildcrout JS, Peterson JF, Pulley J, et al. Clinically actionable genotypes among 10,000 patients with preemptive pharmacogenomic testing. Clin Pharmacol Ther. 2014;95(4):423–31. doi:10.1038/clpt.2013.229.
Vanderbilt University Medical Center. Using genetics to personalize medication treatment. In. My DRUG GENOME. n.d. http://www.mydruggenome.org/overview.php. Accessed 28 Jun 2016.
Kim L, Kim JA, Kim S. A guide for the utilization of health insurance review and assessment service national patient samples. Epidemiol Health. 2014;36:e2014008. doi:10.4178/epih/e2014008.
Kim L, Jin S, Kim Y, Kim S, Kim S, Tchoe B, et al. Developing the inpatient sample for the National Health Insurance claims data. Health Policy Manag. 2013;23(2):152–61. doi:10.4332/KJHPA.2013.23.2.152.
Food and Drug Administration. Table of pharmacogenomic biomarkers in drug labeling. In: US Food and Drug Administration. 2015. http://www.fda.gov/Drugs/ScienceResearch/ResearchAreas/Pharmacogenetics/ucm083378.htm. Accessed 28 Jun 2016.
Yang JJ, Lim JY, Huang J, Bass J, Wu J, Wang C, Fang J, Stewart E, Harstead EH, Robinson GW, Evans WE, Pappo A, Zuo J, Relling MV, Onar-Thomas A, Gajjar A, Stewart CF. The role of inherited TPMT and COMT genetic variation in cisplatin-induced ototoxicity in children with cancer. Clin Pharmacol Ther. 2013;94(2):252–9. doi:10.1038/clpt.2013.121.
Hagleitner MM, Coenen MJ, Patino-Garcia A, de Bont ES, Gonzalez-Neira A, Vos HI, van Leeuwen FN, Gelderblom H, Hoogerbrugge PM, Guchelaar HJ, Te Loo MW. Influence of genetic variants in TPMT and COMT associated with cisplatin induced hearing loss in patients with cancer: two new cohorts and a meta-analysis reveal significant heterogeneity between cohorts. PLoS One. 2014. 31;9(12):e115869. doi:10.1371/journal.pone.0115869.
Yagi M, Nakamura T, Okizuka Y, Oyazato Y, Kawasaki Y, Tsuneishi S, Sakaeda T, Matsuo M, Okumura K, Okamura N. Effect of CPS14217C > A genotype on valproic-acid-induced hyperammonemia. Pediatr Int. 2010;52(5):744–8. doi:10.1111/j.1442-200X.2010.03157.x.
Inoue K, Suzuki E, Takahashi T, Yamamoto Y, Yazawa R, Takahashi Y, Imai K, Miyakawa K, Inoue Y, Tsuji D, Hayashi H, Itoh K. 4217C > A polymorphism in carbamoyl-phosphate synthase 1 gene may not associate with hyperammonemia development during valproic acid-based therapy. Epilepsy Res. 2014;108(6):1046–51. doi:10.1016/j.eplepsyres.2014.04.008.
Food and Drug Administration. What is a serious adverse event? In US food and drug administration. 2016. http://www.fda.gov/Safety/MedWatch/HowToReport/ucm053087.htm. Accessed 28 Jun 2016.
Genomes. The 1000 Genomes Browser. In 1000 Genomes. 2015. http://browser.1000genomes.org/index.html. Accessed 28 Jun 2016.
Beutler E, Gelbart T, Demina A. Racial variability in the UDP-glucuronosyltransferase 1 (UGT1A1) promoter: a balanced polymorphism for regulation of bilirubin metabolism? Proc Natl Acad Sci USA. 1998;95(14):8170–4.
Park IH, Ro J, Park S, Lim HS, Lee KS, Kang HS, Jung SY, Lee S. Lack of any association between functionally significant CYP2D6 polymorphisms and clinical outcomes in early breast cancer patients receiving adjuvant tamoxifen treatment. Breast Cancer Res Treat. 2012;131(2):455–61. doi:10.1007/s10549-011-1425-2.
Premji Z, Umeh RE, Owusu-Agyei S, Esamai F, Ezedinachi EU, Oguche S, et al. Chlorproguanil-dapsone-artesunate versus artemether-lumefantrine: a randomized, double-blind phase III trial in African children and adolescents with uncomplicated Plasmodium falciparum malaria. PLoS One. 2009;4(8):e6682. doi:10.1371/journal.pone.0006682.
Bancone G, Chowwiwat N, Somsakchaicharoen R, Poodpanya L, Moo PK, Gornsawun G, Kajeechiwa L, Thwin MM, Rakthinthong S, Nosten S, Thinraow S, Nyo SN, Ling CL, Wiladphaingern J, Kiricharoen NL, Moore KA, White NJ, Nosten F. Single low dose primaquine (0.25 mg/kg) does not cause clinically significant haemolysis in G6PD deficient subjects. PLoS One. 2016;11(3):e0151898. doi:10.1371/journal.pone.0151898.
Vannaprasaht S, Angsuthum S, Avihingsanon Y, Sirivongs D, Pongskul C, Makarawate P, Praditpornsilpa K, Tassaneeyakul W, Tassaneeyakul W. Impact of the heterozygous TPMT*1/*3C genotype on azathioprine-induced myelosuppression in kidney transplant recipients in Thailand. Clin Ther. 2009;31(7):1524–33. doi:10.1016/j.clinthera.2009.07.008.
Higgs JE, Payne K, Roberts C, Newman WG. Are patients with intermediate TPMT activity at increased risk of myelosuppression when taking thiopurine medications? Pharmacogenomics. 2010;11(2):177–88. doi:10.2217/pgs.09.155.
Peregud-Pogorzelski J, Tetera-Rudnicka E, Kurzawski M, Brodkiewicz A, Adrianowska N, Mlynarski W, et al. Thiopurine S-methyltransferase (TPMT) polymorphisms in children with acute lymphoblastic leukemia, and the need for reduction or cessation of 6-mercaptopurine doses during maintenance therapy: the Polish multicenter analysis. Pediatr Blood Cancer. 2011;57(4):578–82. doi:10.1002/pbc.23013.
Sorich MJ, Rowland A, McKinnon RA, Wiese MD. CYP2C19 genotype has a greater effect on adverse cardiovascular outcomes following percutaneous coronary intervention and in Asian populations treated with clopidogrel: a meta-analysis. Circ Cardiovasc Genet. 2014;7(6):895–902. doi:10.1161/CIRCGENETICS.114.000669.
Teh LK, Hamzah S, Hashim H, Bannur Z, Zakaria ZA, Hasbullani Z, Shia JK, Fijeraid H, Md Nor A, Zailani M, Ramasamy P, Ngow H, Sood S, Salleh MZ. Potential of dihydropyrimidine dehydrogenase genotypes in personalizing 5-fluorouracil therapy among colorectal cancer patients. Ther Drug Monit. 2013;35(5):624–30. doi:10.1097/FTD.0b013e318290acd2.
Meta-Analysis Group In C, Levy E, Piedbois P, Buyse M, Pignon JP, Rougier P, et al. Toxicity of fluorouracil in patients with advanced colorectal cancer: effect of administration schedule and prognostic factors. J Clin Oncol. 1998;16(11):3537–41.
Bloch KM, Sills GJ, Pirmohamed M, Alfirevic A. Pharmacogenetics of antiepileptic drug-induced hypersensitivity. Pharmacogenomics. 2014;15(6):857–68. doi:10.2217/pgs.14.65.
Martin-Merino E, de Abajo FJ, Gil M. Risk of toxic epidermal necrolysis and Stevens–Johnson syndrome associated with benzodiazepines: a population-based cohort study. Eur J Clin Pharmacol. 2015;71(6):759–66. doi:10.1007/s00228-015-1850-y.
Ozeki T, Mushiroda T, Yowang A, Takahashi A, Kubo M, Shirakata Y, et al. Genome-wide association study identifies HLA-A*3101 allele as a genetic risk factor for carbamazepine-induced cutaneous adverse drug reactions in Japanese population. Hum Mol Genet. 2011;20(5):1034–41. doi:10.1093/hmg/ddq537.
Tangamornsuksan W, Lohitnavy O, Kongkaew C, Chaiyakunapruk N, Reisfeld B, Scholfield NC, Lohitnavy M. Association of HLA-B*5701 genotypes and abacavir-induced hypersensitivity reaction: a systematic review and meta-analysis. J Pharm Pharm Sci. 2015;18(1):68–76.
Sun HY, Hung CC, Lin PH, Chang SF, Yang CY, Chang SY, et al. Incidence of abacavir hypersensitivity and its relationship with HLAB*5701 in HIV-infected patients in Taiwan. J Antimicrob Chemother. 2007;60(3):599–604.
Grover S, Kukreti R. HLA alleles and hypersensitivity to carbamazepine: an updated systematic review with meta-analysis. Pharmacogenet Genomics. 2014;24(2):94–112. doi:10.1097/FPC.0000000000000021 (Review. Erratum in: Pharmacogenet Genomics. 2014;24(4):230).
Wang Y, Shen L, Xu N, Wang JW, Jiao SC, Liu ZY, Xu JM. UGT1A1 predicts outcome in colorectal cancer treated with irinotecan and fluorouracil. World J Gastroenterol. 2012;18(45):6635–44. doi:10.3748/wjg.v18.i45.6635.
Singer JB, Shou Y, Giles F, Kantarjian HM, Hsu Y, Robeva AS, et al. UGT1A1 promoter polymorphism increases risk of nilotinib-induced hyperbilirubinemia. Leukemia. 2007;21(11):2311–5. doi:10.1038/sj.leu.2404827.
Xu CF, Reck BH, Xue Z, Huang L, Baker KL, Chen M, et al. Pazopanib-induced hyperbilirubinemia is associated with Gilbert’s syndrome UGT1A1 polymorphism. Br J Cancer. 2010;102(9):1371–7. doi:10.1038/sj.bjc.6605653.
Yang J, Chen Y, Li X, Wei X, Chen X, Zhang L, Zhang Y, Xu Q, Wang H, Li Y, Lu C, Chen W, Zeng C, Yin T. Influence of CYP2C9 and VKORC1 genotypes on the risk of hemorrhagic complications in warfarin-treated patients: a systematic review and meta-analysis. Int J Cardiol. 2013;168(4):4234–43. doi:10.1016/j.ijcard.2013.07.151.
Hou Q, Li S, Li L, Li Y, Sun X, Tian H. Association between SLCO1B1 gene T521C polymorphism and statin-related myopathy risk: a meta-analysis of case-control studies. Medicine (Baltimore). 2015;94(37):e1268. doi:10.1097/MD.0000000000001268.
Acknowledgments
The authors would like to acknowledge the Korean Health Insurance Review and Assessment service for providing the National Patient Sample dataset used in our study (dataset serial number HIRA-NPS-2011-0133) and educational support provided by the Education and Research Encouragement Fund of Seoul National University Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by Grants from the Korean Health Technology R&D Project, Ministry of Health and Welfare (HI13C2164, HI16C11280000).
Conflicts of interest
Ju Han Kim, Grace Juyun Kim, Soo Youn Lee, Ji Hye Park, and Brian Y. Ryu have no conflict of interest directly relevant to the content of this study. The results of this study do not reflect the views of the Ministry of Health and Welfare or the South Korean Health Insurance Review and Assessment service.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Additional information
G. J. Kim and S. Y. Lee contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, G.J., Lee, S.Y., Park, J.H. et al. Role of Preemptive Genotyping in Preventing Serious Adverse Drug Events in South Korean Patients. Drug Saf 40, 65–80 (2017). https://doi.org/10.1007/s40264-016-0454-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-016-0454-5