Abstract
Objective
The aim of this systematic review and meta-analysis was to compare the clinical outcomes between genotype-guided and conventional tacrolimus doses in kidney transplantation patients.
Materials and Methods
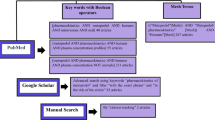
We performed a comprehensive literature search of the PubMed, EMBASE, and Cochrane databases from the date of inception to 26 February 2020. References of the retrieved articles were also reviewed and any further relevant studies were included. The search terms included ‘tacrolimus’, ‘cytochrome P-450 CYP3A’, ‘polymorphism, genetic’, ‘genomics’, ‘genome’, ‘genotype’, ‘genes’, ‘alleles’, and ‘pharmacogenetics’.
Results
Our study showed that the genotype-guided group included an increased proportion of patients with tacrolimus concentrations in the therapeutic range at steady state (risk ratio [RR] 1.40, 95% confidence interval [CI] 1.14–1.72, p = 0.001; high quality), with a trend for achieving therapeutic concentrations earlier compared with those in the conventional group. However, there was no statistical difference in the incidence of delayed graft function (RR 1.98, 95% CI 0.92–1.76, p = 0.12; moderate quality), incidence of acute rejection (RR 1.00, 95% CI 0.64–1.55, p = 1.00; moderate quality), incidence of graft survival censored for death (RR 1.02, 95% CI 0.98–1.06, p = 0.37; moderate quality), and incidence of adverse effects (AEs).
Conclusions
Although the genotype-guided group had a higher proportion of patients within the targeted concentration and less median time to achieve the therapeutic range, the clinical endpoints, including delayed graft function, acute rejection, graft survival censored for death, and AEs were similar in both groups. All in all, evidence suggested there was no utility in pharmacogenetics for tacrolimus based on the cytochrome P450 (CYP) 3A5 genotype. Studies with Chinese and African American populations are needed due to the frequency of genetic polymorphisms of CYP3A5. Furthermore, a dosing algorithm that includes demographic and clinical factors plus multiple genetic variants should be added for consideration, and may optimize early tacrolimus exposure.





Similar content being viewed by others
References
Thölking G, Gerth HU, Schuette-Nuetgen K, et al. Influence of tacrolimus metabolism rate on renal function after solid organ transplantation. World J Transplant. 2017;7(1):26–33.
Muraki Y. Factors affecting the pharmacokinetics after living donor liver transplant. Yakugaku Zasshi. 2012;132(9):1011–7.
Gonzalez D, Rao GG, Bailey SC, et al. Precision dosing: public health need, proposed framework, and anticipated impact. Clin Transl Sci. 2017;10(6):443–54.
Ferraris JR, Argibay PF, Costa L, et al. Influence of CYP3A5 polymorphism on tacrolimus maintenance doses and serum levels after renal transplantation: age dependency and pharmacological interaction with steroids. Pediatr Transplant. 2011;15(5):525–32.
Birdwell KA, Decker B, Barbarino JM, et al. Clinical Pharmacogenetics Implementation Consortium (CPIC) guidelines for CYP3A5 genotype and tacrolimus dosing. Clin Pharmacol Ther. 2015;98(1):19–24.
MacPhee I, Fredericks S, Tai T, et al. The influence of pharmacogenetics on the time to achieve target tacrolimus concentrations after kidney transplantation. Am J Transplant. 2004;4(6):914–9.
Thervet E, Loriot MA, Barbier S, et al. Optimization of initial tacrolimus dose using pharmacogenetic testing. Clin Pharmacol Ther. 2010;87(6):721–6.
Pallet N, Etienne I, Buchler M, et al. Long-term clinical impact of adaptation of initial tacrolimus dosing to CYP3A5 genotype. Am J Transplant. 2016;16(9):2670–5.
Chen SY, Li JL, Meng FH, et al. Individualization of tacrolimus dosage basing on cytochrome P450 3A5 polymorphism: a prospective, randomized controlled study. Clin Transplant. 2013;27(3):E272-281.
Shuker N, Bouamar R, van Schaik RHN, et al. A randomized controlled trial comparing the efficacy of Cyp3a5 genotype-based with body-weight-based tacrolimus dosing after living donor kidney transplantation. Am J Transplant. 2016;16(7):2085–96.
Min S, Papaz T, Lafreniere-Roula M, et al. A randomized clinical trial of age and genotype–guided tacrolimus dosing after pediatric solid organ transplantation. Pediatr Transplant. 2018;22(7):e13285.
Anutrakulchai S, Pongskul C, Kritmetapak K, et al. Therapeutic concentration achievement and allograft survival comparing usage of conventional tacrolimus doses and CYP3A5 genotype–guided doses in renal transplantation patients. Br J Clin Pharmacol. 2019;85(9):1964–73.
Hui Y, Xiangli C, Xin W, et al. Clinical outcomes with antiviral prophylaxis or preemptive therapy for cytomegalovirus disease after liver transplantation: a systematic review and meta-analysis. J Pharm Pharm Sci. 2017;20:15–27.
Venkataramanan R, Swaminathan A, Prasad T, et al. Clinical pharmacokinetics of tacrolimus. Clin Pharmacokinet. 1995;29:404.
Undre NA, van Hoof J, Christiaans M, et al. Low systemic exposure to tacrolimus correlates with acute rejection. Transplant Proc. 1999;31:296–8.
Hessenlink DA, van Schaik RH, van der Heiden IP, et al. Genetic polymorphisms of the CYP3A4, CYP3A5, and MDR–1 genes and pharmacokinetics of the calcineurin inhibitors cyclosporine and tacrolimus. Clin Pharmacol Ther. 2003;74(3):245–54.
Zhang X, Liu ZH, Zheng JM, et al. Influence of CYP3A5 and MDR1 polymorphisms on 6 tacrolimus concentration in the early stage after renal transplantation. Clin Transplant. 2005;19(5):638–43.
Renders L, Frisman M, Ufer M, et al. CYP3A5 genotype markedly influences the pharmacokinetics of tacrolimus and sirolimus in kidney transplant recipients. Clin Pharmacol Ther. 2007;81(2):228–34.
Haufroid V, Wallemacq P, VanKerckhove V, et al. CYP3A5 and ABCB1 polymorphisms and tacrolimus pharmacokinetics in renal transplant candidates: guidelines from an experimental study. Am J Transplant. 2006;6(11):2706–13.
Hustert E, Haberl M, Burk O, et al. The genetic determinants of the CYP3A5 polymorphism. Pharmacogenetics. 2001;11(9):773–9.
Xie HG, Wood AJ, Kim RB, et al. Genetic variability in CYP3A5 and its possible consequences. Pharmacogenomics. 2004;5(3):243–72.
Van Schaik RH, van der Heiden IP, van den Anker JN, et al. CYP3A5 variant allele frequencies in Dutch Caucasians. Clin Chem. 2002;48(10):1668–71.
Ruan V, Czer LS, Awad M, et al. Use of anti-thymocyte globulin for induction therapy in cardiac transplantation: a review. Transplant Proc. 2017;49(2):253–9.
Crowson CN, Reed RD, Shelton BA, et al. Lymphocyte–depleting induction therapy lowers the risk of acute rejection in African American pediatric kidney transplant recipients. Pediatr Transplant. 2017;21(1):10.
Passey C, Birnbaum AK, Brundage RC, et al. Dosing equation for tacrolimus using genetic variants and clinical factors. Br J Clin Pharmacol. 2011;72(6):948–57.
Elens L, Bouamar R, Shuker N, et al. Clinical implementation of pharmacogenetics in kidney transplantation: calcineurin inhibitors in the starting blocks. Br J Clin Pharmacol. 2014;77(4):715–28.
Bloch J, Hazzan M, Van der Hauwaert C, et al. Donor ABCB1 genetic polymorphisms influence epithelial-to-mesenchyme transition in tacrolimus-treated kidney recipients. Pharmacogenomics. 2014;15(16):2011–24.
Moore J, McKnight AJ, Dohler B, et al. Donor ABCB1 variant associates with increased risk for kidney allograft failure. J Am Soc Nephrol. 2012;23(11):1891–9.
Abdel-Kahaar E, Winter S, Tremmel R, et al. The impact of CYP3A4*22 on tacrolimus pharmacokinetics and outcome in clinical practice at a single kidney transplant center. Front Genet. 2019;10:871.
Lloberas N, Elens L, Llaudó I, et al. The combination of CYP3A4*22 and CYP3A5*3 single-nucleotide polymorphisms determines tacrolimus dose requirement after kidney transplantation. Pharmacogenet Genom. 2017;27(9):313–22.
Wang P, Mao Y, Razo J, et al. Using genetic and clinical factors to predict tacrolimus dose in renal transplant recipients. Pharmacogenomics. 2010;11(10):1389–402.
Acknowledgements
We thank all authors of the included studies for their wonderful work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of Interest
Hui Yang, Yiqi Sun, Xiaojia Yu, Xiaopeng Hu, Wei Wang, Xiaodong Zhang, and Lihong Liu declare no conflicts of interest.
Ethical Approval
This was a systematic review and meta-analysis based on previously published articles, therefore ethical approval was not required.
Consent to participate
This was a systematic review and meta-analysis based on previously published articles, therefore consent to participate was not required.
Consent for publication
This was a systematic review and meta-analysis based on previously published articles, therefore consent for publication was not required.
Availability of data and material
The datasets used or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Author Contributions
HY and LHL designed the experiments. HY, YS, XY, XH, WW, and XZ collected and analyzed the data. HY wrote the article, which was reviewed by all authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yang, H., Sun, Y., Yu, X. et al. Clinical Impact of the Adaptation of Initial Tacrolimus Dosing to the CYP3A5 Genotype After Kidney Transplantation: Systematic Review and Meta-Analysis of Randomized Controlled Trials. Clin Pharmacokinet 60, 877–885 (2021). https://doi.org/10.1007/s40262-020-00955-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-020-00955-2