Abstract
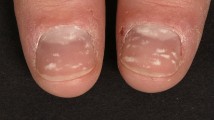
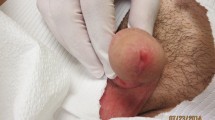
The majority of patients with Sézary syndrome (SS) present with classic symptoms of erythroderma, lymphadenopathy, and pruritus. However, there have been numerous reports of patients with SS who have non-classic signs. In this review, we report the less common clinical presentations of SS and discuss their relevant treatments. Our search included all literature on SS since 2008, the year the World Health Organization (WHO) incorporated the diagnostic criteria for SS into the WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. We reviewed 896 articles and identified 505 patients with non-classic presentations of SS. Of these 505 patients, the most common non-classic signs of SS were keratoderma, onychodystrophy, alopecia, leonine facies, and ectropion. Given the aggressive and highly symptomatic nature of SS, it is imperative that clinicians recognize the less common signs of the disease to prevent delays in diagnosis and treatment. To our knowledge, this is the first review of the clinical variations of SS with a focus on non-classic signs and symptoms.


Similar content being viewed by others
References
Vonderheid EC, Bernengo MG, Burg G, Duvic M, Heald P, Laroche L, et al. Update on erythrodermic cutaneous T-cell lymphoma: report of the international society for cutaneous lymphomas. J Am Acad Dermatol. 2002;46(1):95–106. https://doi.org/10.1067/mjd.2002.118538.
Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, et al. (eds). WHO classification of tumours of haematopoietic and lymphoid tissues. World Health Organization Classification of Tumours, 4th edn. Lyon: International Agency for Research on Cancer (IARC); 2008.
Thompson AK, Killian JM, Weaver AL, Pittelkow MR, Davis MDP. Sézary syndrome without erythroderma: a review of 16 cases at Mayo Clinic. J Am Acad Dermatol. 2017;76(4):683–8. https://doi.org/10.1016/j.jaad.2016.10.029.
Booken N, Nicolay JP, Weiss C, Klemke CD. Cutaneous tumor cell load correlates with survival in patients with Sezary syndrome. J Dtsch Dermatol Ges. 2013;11(1):67–79. https://doi.org/10.1111/j.1610-0387.2012.08027.x.
Vij A, Duvic M. Prevalence and severity of pruritus in cutaneous T cell lymphoma. Int J Dermatol. 2012;51(8):930–4. https://doi.org/10.1111/j.1365-4632.2011.05188.x.
Boonk SE, Zoutman WH, Marie-Cardine A, van der Fits L, Out-Luiting JJ, Mitchell TJ, et al. Evaluation of immunophenotypic and molecular biomarkers for Sezary syndrome using standard operating procedures: a multicenter study of 59 patients. J Invest Dermatol. 2016;136(7):1364–72. https://doi.org/10.1016/j.jid.2016.01.038.
Gru A, Schaffer A. Hematopathology of the skin: a clinical and pathologic approach. 1st ed. Philadelphia: Wolters Kluwer; 2017.
Talpur R, Bassett R, Duvic M. Prevalence and treatment of Staphylococcus aureus colonization in patients with mycosis fungoides and Sezary syndrome. Br J Dermatol. 2008;159(1):105–12. https://doi.org/10.1111/j.1365-2133.2008.08612.x.
Mangold AR, Thompson AK, Davis MD, Saulite I, Cozzio A, Guenova E, et al. Early clinical manifestations of Sézary syndrome: a multicenter retrospective cohort study. J Am Acad Dermatol. 2017;77(4):719–27. https://doi.org/10.1016/j.jaad.2017.05.036.
Bi MY, Curry JL, Christiano AM, Hordinsky MK, Norris DA, Price VH, et al. The spectrum of hair loss in patients with mycosis fungoides and Sezary syndrome. J Am Acad Dermatol. 2011;64(1):53–63. https://doi.org/10.1016/j.jaad.2009.12.056.
Martin SJ, Duvic M. Prevalence and treatment of palmoplantar keratoderma and tinea pedis in patients with Sezary syndrome. Int J Dermatol. 2012;51(10):1195–8. https://doi.org/10.1111/j.1365-4632.2011.05204.x.
Molloy K, Jonak C, Woei AJF, Guenova E, Busschots AM, Bervoets A, et al. Characteristics associated with significantly worse quality of life in mycosis fungoides/Sezary syndrome from the Prospective Cutaneous Lymphoma International Prognostic Index (PROCLIPI) study. Br J Dermatol. 2019. https://doi.org/10.1111/bjd.18089(Epub 2019 May 2).
Vidulich KA, Talpur R, Bassett RL, Duvic M. Overall survival in erythrodermic cutaneous T-cell lymphoma: an analysis of prognostic factors in a cohort of patients with erythrodermic cutaneous T-cell lymphoma. Int J Dermatol. 2009;48(3):243–52. https://doi.org/10.1111/j.1365-4632.2009.03771.x.
Brown DN, Wieser I, Wang C, Dabaja BS, Duvic M. Leonine facies (LF) and mycosis fungoides (MF): a single-center study and systematic review of the literature. J Am Acad Dermatol. 2015;73(6):976–86. https://doi.org/10.1016/j.jaad.2015.09.017.
Fragkos KC. Plantar keratoderma of Sézary syndrome. Clin Case Rep. 2017;5(10):1726–7. https://doi.org/10.1002/ccr3.1168.
Bishop BE, Wulkan A, Kerdel F, El-Shabrawi-Caelen L, Tosti A. Nail alterations in cutaneous T-cell lymphoma: a case series and review of nail manifestations. Skin Appendage Disord. 2015;1(2):82–6. https://doi.org/10.1159/000433474.
Polansky M, Talpur R, Daulat S, Hosing C, Dabaja B, Duvic M. Long-term complete responses to combination therapies and allogeneic stem cell transplants in patients with Sezary syndrome. Clin Lymphoma Myeloma Leuk. 2015;15(5):e83–93. https://doi.org/10.1016/j.clml.2014.09.013.
Al-Niaimi F, Cox NH, Taylor WD. Follicular hyperkeratosis as a manifestation of Sezary syndrome. Br J Dermatol. 2010;162(3):695–6. https://doi.org/10.1111/j.1365-2133.2009.09599.x.
Ogilvie C, Jackson R, Leach M, McKay P. Sezary syndrome: diagnosis and management. J R Coll Phys Edinb. 2012;42:317–21. https://doi.org/10.4997/JRCPE.2012.408.
Rasmussen TA, McMahon J, Chang JJ, Symons J, Roche M, Dantanarayana A, et al. Impact of alemtuzumab on HIV persistence in an HIV-infected individual on antiretroviral therapy with Sezary syndrome. AIDS. 2017;31(13):1839–45. https://doi.org/10.1097/QAD.0000000000001540.
Park K, Reed J, Talpur R, Duvic M. Nail irregularities associated with Sezary syndrome. Cutis. 2019;103(4):E11–E16.
Mackie RM. Onycholysis occurring during PUVA therapy. Clin Exp Dermatol. 1979;4(1):111–3. https://doi.org/10.1111/j.1365-2230.1979.tb01599.x.
Jones GW, Kacinski BM, Wilson LD, Willemze R, Spittle M, Hohenberg G, et al. Total skin electron radiation in the management of mycosis fungoides: consensus of the European Organization for Research and Treatment of Cancer (EORTC) Cutaneous Lymphoma Project Group. J Am Acad Dermatol. 2002;47(3):364–70. https://doi.org/10.1067/mjd.2002.123482.
Ehsani AH, Nasimi M, Azizpour A, Noormohammadpoor P, Kamyab K, Seirafi H, et al. Nail changes in early mycosis fungoides. Skin Appendage Disord. 2018;4(1):55–9. https://doi.org/10.1159/000478946.
Haneke E. Advanced nail surgery. J Cutan Aesthet Surg. 2011;4(3):167–75. https://doi.org/10.4103/0974-2077.91247.
Sonnex TS, Dawber RP, Zachary CB, Millard PR, Griffiths AD. The nails in adult type 1 pityriasis rubra pilaris. A comparison with Sezary syndrome and psoriasis. J Am Acad Dermatol. 1986;15(5 Pt 1):956–60. https://doi.org/10.1016/s0190-9622(86)70256-9.
Parmentier L, Durr C, Vassella E, Beltraminelli H, Borradori L, Haneke E. Specific nail alterations in cutaneous T-cell lymphoma: successful treatment with topical mechlorethamine. Arch Dermatol. 2010;146(11):1287–91. https://doi.org/10.1001/archdermatol.2010.325.
Tomsick RS. Hyperkeratosis in mycosis fungoides. Cutis. 1982;29(6):621–3.
Damasco FM, Geskin L, Akilov OE. Onychodystrophy in Sézary syndrome. J Am Acad Dermatol. 2018;79(5):972–3. https://doi.org/10.1016/j.jaad.2018.06.023.
Oliveira A, Lobo I, Alves R, Lima M, Selores M. Sezary syndrome presenting with leonine facies and treated with low-dose subcutaneous alemtuzumab. Dermatol Online J. 2011;17(11):6.
Kho B, Wong HHN, Sin C-F, Leung RYY, Kwong Y-L. Leonine facies due to sezary syndrome: complete clinical, radiologic, and molecular remission with alemtuzumab. Ann Hematol. 2017;96(12):2121–3. https://doi.org/10.1007/s00277-017-3113-8.
Corey K, Cook D, Bekker J, Mugnaini E, Lin JH. A case of refractory Sézary syndrome with large-cell transformation responsive to brentuximab vedotin. JAMA Dermatol. 2014;150(2):210–2. https://doi.org/10.1001/jamadermatol.2013.5741.
Chattopadhyay M, Rytina E, Follows G, Meligonis G, Meyer P, Norris P. Acute scleritis and nonerythrodermic skin rash: an unusual presentation of Sézary syndrome [poster no. P6697]. J Am Acad Dermatol. 2013;68(4 Suppl. 1):AB143. https://doi.org/10.1016/j.jaad.2012.12.595.
Livingstone I, Ramamurthi S, Drummond S, Kemp E, Roberts F. Corneal perforation due to limbal involvement in Sezary syndrome. Graefes Arch Clin Exp Ophthalmol. 2011;249(7):1091–4. https://doi.org/10.1007/s00417-010-1611-7.
LaMattina KC, Becker NM. Bilateral hypopyon uveitis secondary to mycosis fungoides with Sezary syndrome. Ocul Immunol Inflamm. 2014;22(3):246–7. https://doi.org/10.3109/09273948.2013.841488.
Kotz E, Anderson D, Thiers B. Cutaneous T-cell lymphoma. J Eur Acad Dermatol Venereol. 2003;17(2):131–7. https://doi.org/10.1046/j.1468-3083.2003.00635.x.
Cedeno-Laurent F, Kim EJ, Rook AH, Vittorio CC, Rubin AI. Polydactylous longitudinal melanonychia acquired following total skin electron beam radiation therapy for Sézary syndrome. Skin Appendage Disord. 2015;1(2):60–1. https://doi.org/10.1159/000398817.
DeSesa CR, Appugounder S, Haberland C, Johnson MP. Osteonecrosis of the jaw in association with chemotherapy in the setting of cutaneous T-cell lymphoma. J Oral Maxillofac Surg. 2016;74(2):292–301. https://doi.org/10.1016/j.joms.2015.07.019.
Gardner JM, Introcaso CE, Nasta SD, Kim EJ, Vittorio CC, Rook AH. A novel regimen of vorinostat with interferon gamma for refractory Sezary syndrome. J Am Acad Dermatol. 2009;61(1):112–6. https://doi.org/10.1016/j.jaad.2008.11.889.
Ortonne N, Le Gouvello S, Mansour H, Poillet C, Martin N, Delfau-Larue MH, et al. CD158K/KIR3DL2 transcript detection in lesional skin of patients with erythroderma is a tool for the diagnosis of Sezary syndrome. J Invest Dermatol. 2008;128(2):465–72. https://doi.org/10.1038/sj.jid.5701013.
van Doorn R, Slieker RC, Boonk SE, Zoutman WH, Goeman JJ, Bagot M, et al. Epigenomic analysis of Sézary syndrome defines patterns of aberrant DNA methylation and identifies diagnostic markers. J Invest Dermatol. 2016;136(9):1876–84. https://doi.org/10.1016/j.jid.2016.03.042.
Alberti-Violetti S, Vezzoli P, Corti L, Fanoni D, Merlo V, Venegoni L, et al. Sézary syndrome in a 17-year-old boy: clinicopathologic features and genomic profile. Pediatr Dermatol. 2016;33(5):e318–e321321. https://doi.org/10.1111/pde.12930.
Brugiere C, Stefan A, Salaun V, Comoz F, Campbell K, Chantepie S, et al. An unusual Sezary syndrome with concomitant pulmonary localization: aggressiveness of folliculotropic form. Int J Dermatol. 2016;55(1):81–4. https://doi.org/10.1111/ijd.12371.
Emadi SN, Babamahmoodi F, Poursaleh Z, Sayad-Noori SS, Soroush MR, Maleki AR, et al. Sezary syndrome, Kaposi sarcoma and generalized dermatophytosis 15 years after sulfur mustard gas exposure. J Dermatol Case Rep. 2012;6(3):86–9. https://doi.org/10.3315/jdcr.2012.1109.
Jang MS, Kang DY, Han SH, Park JB, Kim ST, Suh KS. CD25+ folliculotropic Sezary syndrome with CD30+ large cell transformation. Aust J Dermatol. 2014;55(1):e4–8. https://doi.org/10.1111/ajd.12000.
Miyashiro D, Torrealba MP, Manfrere KC, Pereira J, Sato MN, Sanches JA. Double-positive CD4 and CD8 Sézary syndrome. JAAD Case Rep. 2017;3(6):485–8. https://doi.org/10.1016/j.jdcr.2017.06.036.
Tilakaratne D, Sidhu S. Heavy metal (monoclonal) bands: a link between cutaneous T-cell lymphoma and contact allergy to potassium dichromate, nickel and cobalt? Aust J Dermatol. 2015;56(1):59–63. https://doi.org/10.1111/ajd.12182.
Bagazgoitia L, Perez-Carmona L, Rios L, Munoz E, Harto A, Jaen P. Acute hyperkeratotic and desquamative reaction in a patient with Sezary syndrome treated with bexarotene. J Eur Acad Dermatol Venereol. 2008;22(3):389–90. https://doi.org/10.1111/j.1468-3083.2007.02341.x.
Damasco FM, Geskin LJ, Akilov OE. Nail changes in Sezary syndrome: a single-center study and review of the literature. J Cutan Med Surg. 2019;23(4):380–7. https://doi.org/10.1177/1203475419839937.
Wu R, Zippin JH, Magro C. Double-positive CD4(+)CD8(+) Sezary syndrome: an unusual phenotype with an aggressive clinical course. Cutis. 2014;93(2):E18–25.
Bi MY, Curry JL, Christiano AM, Hordinsky MK, Norris DA, Price VH, et al. The spectrum of hair loss in patients with mycosis fungoides and Sézary syndrome. J Am Acad Dermatol. 2011;64(1):53–63. https://doi.org/10.1016/j.jaad.2009.12.056.
Carter JB, Barnes JA, Niell BL, Nardi V. Case records of the Massachusetts General Hospital. Case 24-2013. A 53-year-old woman with erythroderma, pruritus, and lymphadenopathy. N Engl J Med. 2013;369(6):559–69. https://doi.org/10.1056/NEJMcpc1201415.
Crandon S, Yancey MA. Sezary syndrome: a case study of cutaneous T-cell lymphoma. Clin J Oncol Nurs. 2009;13(2):157–9. https://doi.org/10.1188/09.Cjon.157-159.
Lehloenya RJ, Shebe K, Hlela C, Dlamini S, Mankahla A, Lapiner V, et al. Aggressive worsening of Sezary syndrome during early antiretroviral therapy. AIDS. 2013;27(6):1035–6. https://doi.org/10.1097/QAD.0b013e32835ecb62.
Nassem S, Kashyap R, Awasthi NP, Krishnani N, Kumari N. Sezary syndrome presenting with ‘leonine facies’. Aust J Dermatol. 2009;50(4):285–8. https://doi.org/10.1111/j.1440-0960.2009.00560.x.
Alexandroff AB, Shpadaruk V, Bamford WM, Kennedy DB, Burd R, Dyer MJ. Alemtuzumab-resistant Sezary syndrome responding to zanolimumab. Br J Haematol. 2011;154(3):419–21. https://doi.org/10.1111/j.1365-2141.2011.08620.x.
Torocsik D, Gergely L, Veres I, Remenyik E, Begany A. Cutaneous cryptococcosis mimicking basal cell carcinoma in a patient with Sezary syndrome. Acta Derm Venereol. 2012;92(3):286–7. https://doi.org/10.2340/00015555-1326.
Bezier M, Reguiai Z, Delaby P, Laroche L, Said G, Bernard P, et al. Neurolymphomatosis associated with Sezary syndrome. Arch Dermatol. 2009;145(3):294–6. https://doi.org/10.1001/archdermatol.2008.584.
Gottesman SP, Rosen JR, Geller JD, Freeman BB. Atypical varicella-zoster Kaposi varicelliform eruption in Sézary syndrome. Am J Dermatopathol. 2018;40(12):920–3. https://doi.org/10.1097/dad.0000000000001264.
Karadag YS, Gulunay A, Oztekin N, Ak F, Kilickap S. Peripheral neuropathy in sezary syndrome: coincidence or a part of the syndrome? Turk J Haematol. 2013;30(4):420–1. https://doi.org/10.4274/Tjh.2012.0163.
Zeng YP, Wang HW, Wang Z, Sun QN, Jin HZ. Sezary syndrome: a rare form of cutaneous T-cell lymphoma. Chin Med J (Engl). 2010;123(14):1945–7.
Kuzumi A, Takahashi-Shishido N, Mukogawa S, Miyagaki T, Sato S. Paraneoplastic arthritis in a patient with Sézary syndrome. Int J Dermatol. 2018;57(8):e57–e5858. https://doi.org/10.1111/ijd.14020.
Maher AM, Ward CE, Glassman S, Litvinov IV. The importance of excluding cutaneous T-cell lymphomas in patients with a working diagnosis of papuloerythroderma of Ofuji: a case series. Case Rep Dermatol. 2018;10(1):46–544. https://doi.org/10.1159/000487473.
Shimauchi T, Sugita K, Nakamura M, Tokura Y. Leukaemic cutaneous T-cell lymphoma-manifesting papuloerythroderma with CD3(−) CD4(+) phenotype. Acta Derm Venereol. 2010;90(1):68–72. https://doi.org/10.2340/00015555-0786.
Acknowledgements
Dr. Madeleine Duvic is the Blanche Bender Professor in Cancer Research and an honoree of the Stanton CTCL Research Fund.
Funding
No external funding was used in the preparation of this review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Lisa Morris, Jessica Tran, and Madeleine Duvic declare that they have no conflicts of interest that might be relevant to the contents of this review.
Rights and permissions
About this article
Cite this article
Morris, L., Tran, J. & Duvic, M. Non-Classic Signs of Sézary Syndrome: A Review. Am J Clin Dermatol 21, 383–391 (2020). https://doi.org/10.1007/s40257-020-00501-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-020-00501-7