Abstract
Purpose
This study was carried out to evaluate the effects of probiotics administration on clinical status and metabolic profiles in diabetic retinopathy (DR) patients.
Methods
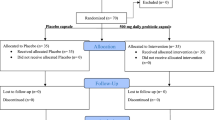
This randomized, double-blind, placebo-controlled trial was conducted among 72 DR patients. Subjects received probiotics including Lactobacillus acidophilus, Bifidobacterium bifidum, Bifidobacterium langum, Bifidobacterium lactis daily (2 × 109 CFU/each strain) (n = 36) or placebo (starch) (n = 36) and were instructed to take one capsule daily for 12 weeks. Finally, 55 participants [probiotic group (n = 30) and placebo group (n = 25)] completed the study. Fasting blood samples were obtained at baseline and after the 12-week intervention to determine metabolic profiles. To determine the effects of probiotic supplementation on clinical symptoms and biochemical variables, we used one-way repeated measures analysis of variance.
Results
After the 12-week intervention, compared with the placebo, probiotic supplementation significantly decreased means serum insulin concentrations (Probiotic group: -4.9 ± 6.5vs. Placebo group: 3.0 ± 7.7 µIU/mL, Ptime×group<0.001), homeostatic model assessment for insulin resistance (Probiotic group: -2.5 ± 3.8 vs. Placebo group: 1.1 ± 2.7, Ptime×group<0.001) and hemoglobin A1c (HbA1C) (Probiotic group: -0.4 ± 0.7 vs. Placebo group: -0.02 ± 0.2%, Ptime×group=0.01), and significantly increased the quantitative insulin sensitivity check index (QUICKI) (Probiotic group: 0.02 ± 0.03 vs. Placebo group: -0.03 ± 0.04, Ptime×group<0.001). There was no significant effect of probiotic administration on other metabolic profiles and clinical symptoms.
Conclusions
Overall, probiotic supplementation after 12 weeks in DR patients had beneficial effects on few metabolic profiles. This study was registered under the Iranian website for clinical trials as http://www.irct.ir: IRCT20130211012438N29.

Similar content being viewed by others
Data availability
The primary data for this study is available from the authors on direct request.
References
Fong DS, Aiello L, Gardner TW, King GL, Blankenship G, Cavallerano JD, et al. Retinopathy in diabetes. Diabetes Care. 2004;27:84–s7.
Williams R, Airey M, Baxter H, Forrester J, kennedy-martin, Kennedy-Martin T, et al. Epidemiology of diabetic retinopathy and macular oedema: a systematic review. Eye. 2004;18:963–83.
Knudsen ST, Bek T, Poulsen PL, Hove MN, Rehling M, Mogensen CE. Macular edema reflects generalized vascular hyperpermeability in type 2 diabetic patients with retinopathy. Diabetes Care. 2002;25:2328–34.
West AL, Oren GA, Moroi SE. Evidence for the use of nutritional supplements and herbal medicines in common eye diseases. Am J Ophthalmol. 2006;141:157–66.
Bloomgarden ZT. Screening for and managing diabetic retinopathy: current approaches. Am J health-system Pharm. 2007;64:8–S14.
García C, Aranda J, Arnold E, Thébault S, Macotela Y, López-Casillas F, et al. Vasoinhibins prevent retinal vasopermeability associated with diabetic retinopathy in rats via protein phosphatase 2A–dependent eNOS inactivation. J Clin Investig. 2008;118:2291–300.
Schwartz SG, Flynn HW. Pharmacotherapies for diabetic retinopathy: present and future. Experimental diabetes research. 2007;2007.
Lian F, Wu L, Tian J, Jin M, Zhou S, Zhao M, et al. The effectiveness and safety of a danshen-containing Chinese herbal medicine for diabetic retinopathy: a randomized, double-blind, placebo-controlled multicenter clinical trial. J Ethnopharmacol. 2015;164:71–7.
Ioannidou E, Tseriotis V-S, Tziomalos K. Role of lipid-lowering agents in the management of diabetic retinopathy. World J Diabetes. 2017;8:1.
Pramanik S, Banerjee K, Mondal LK. The amelioration of detrimental biochemical anomalies by supplementing B, C, and E vitamins in subjects with type 2 diabetes Mellitus May reduce the rate of Development of Diabetic Retinopathy. J Diabetes Res. 2022;2022:3886710.
Gardner TW, Antonetti DA, Barber AJ, LaNoue KF, Levison SW, Group PSRR. Diabetic retinopathy: more than meets the eye. Surv Ophthalmol. 2002;47:253–S62.
Akbari V, Hendijani F. Effects of probiotic supplementation in patients with type 2 diabetes: systematic review and meta-analysis. Nutr Rev. 2016;74:774–84.
Karamali M, Dadkhah F, Sadrkhanlou M, Jamilian M, Ahmadi S, Tajabadi-Ebrahimi M, et al. Effects of probiotic supplementation on glycaemic control and lipid profiles in gestational diabetes: a randomized, double-blind, placebo-controlled trial. Diabetes Metab. 2016;42:234–41.
Ahmadi S, Jamilian M, Karamali M, Tajabadi-Ebrahimi M, Jafari P, Taghizadeh M, et al. Probiotic supplementation and the effects on weight loss, glycaemia and lipid profiles in women with polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. Hum Fertil (Camb). 2017;20:254–61.
Asemi Z, Jazayeri S, Najafi M, Samimi M, Mofid V, Shidfar F, et al. Effect of daily consumption of probiotic yogurt on oxidative stress in pregnant women: a randomized controlled clinical trial. Ann Nutr Metab. 2012;60:62–8.
Li C, Li X, Han H, Cui H, Peng M, Wang G et al. Effect of probiotics on metabolic profiles in type 2 diabetes mellitus: a meta-analysis of randomized, controlled trials. Medicine. 2016;95.
Pisprasert V, Ingram KH, Lopez-Davila MF, Munoz AJ, Garvey WT. Limitations in the use of indices using glucose and insulin levels to predict insulin sensitivity: impact of race and gender and superiority of the indices derived from oral glucose tolerance test in African americans. Diabetes Care. 2013;36:845–53.
Firouzi S, Majid HA, Ismail A, Kamaruddin NA, Barakatun-Nisak MY. Effect of multi-strain probiotics (multi-strain microbial cell preparation) on glycemic control and other diabetes-related outcomes in people with type 2 diabetes: a randomized controlled trial. Eur J Nutr. 2017;56:1535–50.
Benzie IF, Strain JJ. The ferric reducing ability of plasma (FRAP) as a measure of antioxidant power: the FRAP assay. Anal Biochem. 1996;239:70–6.
Beutler E, Gelbart T. Plasma glutathione in health and in patients with malignant disease. J Lab Clin Med. 1985;105:581–4.
Devasagayam T, Boloor K, Ramasarma T. Methods for estimating lipid peroxidation: an analysis of merits and demerits. 2003.
Asemi Z, Zare Z, Shakeri H, Sabihi S-s, Esmaillzadeh A. Effect of multispecies probiotic supplements on metabolic profiles, hs-CRP, and oxidative stress in patients with type 2 diabetes. Annals Nutr Metabolism. 2013;63:1–9.
Hammes HP. Diabetic retinopathy: hyperglycaemia, oxidative stress and beyond. Diabetologia. 2018;61:29–38.
Ostadmohammadi V, Jamilian M, Bahmani F, Asemi Z. Vitamin D and probiotic co-supplementation affects mental health, hormonal, inflammatory and oxidative stress parameters in women with polycystic ovary syndrome. J Ovarian Res. 2019;12:5.
Hajifaraji M, Jahanjou F, Abbasalizadeh F, Aghamohammadzadeh N, Abbasi MM, Dolatkhah N. Effect of probiotic supplements in women with gestational diabetes mellitus on inflammation and oxidative stress biomarkers: a randomized clinical trial. Asia Pac J Clin Nutr. 2018;27:581–91.
Amaretti A, di Nunzio M, Pompei A, Raimondi S, Rossi M, Bordoni A. Antioxidant properties of potentially probiotic bacteria: in vitro and in vivo activities. Appl Microbiol Biotechnol. 2013;97:809–17.
Badehnoosh B, Karamali M, Zarrati M, Jamilian M, Bahmani F, Tajabadi-Ebrahimi M, et al. The effects of probiotic supplementation on biomarkers of inflammation, oxidative stress and pregnancy outcomes in gestational diabetes. J Matern Fetal Neonatal Med. 2018;31:1128–36.
Lin MY, Yen CL. Antioxidative ability of lactic acid bacteria. J Agric Food Chem. 1999;47:1460–6.
Forsyth CB, Farhadi A, Jakate SM, Tang Y, Shaikh M, Keshavarzian A. Lactobacillus GG treatment ameliorates alcohol-induced intestinal oxidative stress, gut leakiness, and liver injury in a rat model of alcoholic steatohepatitis. Alcohol. 2009;43:163–72.
Azcarate-Peril MA, Sikes M, Bruno-Barcena JM. The intestinal microbiota, gastrointestinal environment and colorectal cancer: a putative role for probiotics in prevention of colorectal cancer? Am J Physiol Gastrointest Liver Physiol. 2011;301:G401–24.
Borthakur A, Anbazhagan AN, Kumar A, Raheja G, Singh V, Ramaswamy K, et al. The probiotic Lactobacillus plantarum counteracts TNF-{alpha}-induced downregulation of SMCT1 expression and function. Am J Physiol Gastrointest Liver Physiol. 2010;299:G928–34.
Kijmanawat A, Panburana P, Reutrakul S, Tangshewinsirikul C. Effects of probiotic supplements on insulin resistance in gestational diabetes mellitus: a double-blind randomized controlled trial. J Diabetes Investig. 2019;10:163–70.
Rajkumar H, Mahmood N, Kumar M, Varikuti SR, Challa HR, Myakala SP. Effect of probiotic (VSL#3) and omega-3 on lipid profile, insulin sensitivity, inflammatory markers, and gut colonization in overweight adults: a randomized, controlled trial. Mediators Inflamm. 2014;2014:348959.
Kobyliak N, Falalyeyeva T, Mykhalchyshyn G, Kyriienko D, Komissarenko I. Effect of alive probiotic on insulin resistance in type 2 diabetes patients: randomized clinical trial. Diabetes Metab Syndr. 2018;12:617–24.
Gobel RJ, Larsen N, Jakobsen M, Molgaard C, Michaelsen KF. Probiotics to adolescents with obesity: effects on inflammation and metabolic syndrome. J Pediatr Gastroenterol Nutr. 2012;55:673–8.
Manzhalii E, Virchenko O, Falalyeyeva T, Beregova T, Stremmel W. Treatment efficacy of a probiotic preparation for non-alcoholic steatohepatitis: a pilot trial. J Dig Dis. 2017;18:698–703.
Carding SR, Davis N, Hoyles L. Review article: the human intestinal virome in health and disease. Aliment Pharmacol Ther. 2017;46:800–15.
Torres-Leal FL, Fonseca-Alaniz MH, Rogero MM, Tirapegui J. The role of inflamed adipose tissue in the insulin resistance. Cell Biochem Funct. 2010;28:623–31.
Bischoff SC, Barbara G, Buurman W, Ockhuizen T, Schulzke JD, Serino M, et al. Intestinal permeability–a new target for disease prevention and therapy. BMC Gastroenterol. 2014;14:189.
Neri-Rosario D, Martínez-López YE, Esquivel-Hernández DA, Sánchez-Castañeda JP, Padron-Manrique C, Vázquez-Jiménez A, et al. Dysbiosis signatures of gut microbiota and the progression of type 2 diabetes: a machine learning approach in a Mexican cohort. Front Endocrinol (Lausanne). 2023;14:1170459.
Soccol CR, Vandenberghe LPS, Spier MR, Medeiros ABP, Yamaguishi CT, Lindner JDD, et al. The potential of probiotics: a review. Food Technol Biotechnol. 2010;48:413–34.
Funding
The Research Deputy of Kashan University of Medical Sciences (KAUMS) gave this study grant.
Author information
Authors and Affiliations
Contributions
MT and HM: Concept, statistical analysis, design, drafting the paper, and supervising the research. HF, HM, ZA, SS, MT-E, NSH, and ZB: Collecting the data and drafting the trial.
Corresponding authors
Ethics declarations
Consent for publication
Not applicable.
Competing interests
The authors declare no conflict of interest.
Registration number of the clinical trial
http://www.irct.ir: IRCT20130211012438N29.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Farajipour, H., Matin, H.R., Asemi, Z. et al. The effects of probiotics supplements on metabolic indices and clinical signs in patients with diabetic retinopathy, a randomized double blind clinical trial. J Diabetes Metab Disord (2024). https://doi.org/10.1007/s40200-024-01399-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40200-024-01399-2