Abstract
Purpose
A large percentage of side effects and problems associated with diabetes including social stigma interfere with health promotion behaviors in people with diabetes, minimize their social interactions, and indeed prevent them from asking for help regarding treatments and follow-up care services. Therefore, the present study was to elucidate the relationship between perceived social stigma (PSS) and diabetes self-care (DSC) activities in Iranian participants with type 1 diabetes (T1D).
Methods
This correlational study was fulfilled on 135 participants with T1D in the city of Tabriz, Iran, selected through the convenience sampling method. The data were collected via the Demographic and Clinical Data Collection Form, the Type 1 Diabetes Stigma Assessment Scale (DSAS-1), and the Summary of Diabetes Self-Care Activities Questionnaire (SDSCAQ). The data were analyzed using the SPSS Statistics software (Version 16) incorporating descriptive and analytical statistics.
Results
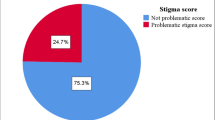
The results revealed that the total score mean of PSS in the study participants was 51.43±12.16, which was at a moderate level. As well, the mean score of the DSC activities was 37.93±11.26. As a whole, no significant relationship was observed between the PSS and the DSC activities.
Conclusion
According to the study findings, the PSS was not significantly correlated with the DSC activities; however, both variables in most study participants were at moderate levels. Therefore, further studies on the factors associated with the social stigma of diabetes are necessary. Knowing these factors can help treatment team plan to reduce the diabetes stigma and improve people with diabetes' self-care.
Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
AlSalhi MS, Devanesan S, E AlZahrani K, AlShebly M, Al-Qahtani F, Farhat K, et al. 2018. Impact of Diabetes Mellitus on Human Erythrocytes: Atomic Force Microscopy and Spectral Investigations. International journal of environmental research and public health. 2018; 15(11): 2368.
Protheroe J, Rowlands G, Bartlam B, Levin-Zamir D. Health literacy, diabetes prevention, and self-management. Journal of Diabetes Research. 2017; Open Access: 3 Pages.
Castensøe-Seidenfaden P, Husted GR, Jensen AK, Hommel E, Olsen B, Pedersen-Bjergaard U, et al. Testing a smartphone app (Young with Diabetes) to improve self-management of diabetes over 12 months: randomized controlled trial. JMIR mHealth and uHealth. 2018;6(6):e141.
Mousavi SI, Alizadeh Chaharborj T, Sheikh MR. Frequency of Psychiatric Disorder Symptoms in Diabetic Patients of Yasuj City in 2014. J Neyshabur Univ Med Sci. 2016;4(1):65–71.
Liu NF, Brown AS, Folias AE, Younge MF, Guzman SJ, Close KL, et al. Stigma in people with type 1 or type 2 diabetes. Clinical Diabetes. 2017;35(1):27–34.
Nishio I, Chujo M. Self-stigma of patients with type 1 diabetes and their coping strategies. Yonago Acta Med. 2017;60(3):167–73.
Ohlsson Nevo E, Karlsson J. Impact of health-related stigma on psychosocial functioning in the general population: construct validity of the Stigma-related Social Problems scale. In Nordic Conference in Nursing Research: Methods and Networks for the future, Oslo, Norway, 13–15 June, 2018.
Tsai W, Lu Q. Ambivalence over emotional expression and intrusive thoughts as moderators of the link between self-stigma and depressive symptoms among Chinese American breast cancer survivors. J Behav Med. 2019;42(3):452–60.
Hofstraat K, van Brakel WH. Social stigma towards neglected tropical diseases: a systematic review. International health. 2016; 8(suppl_1): i53-i70.
Mokaya J, McNaughton AL, Burbridge L, Maponga T, O’Hara G, Andersson M, et al. A blind spot? Confronting the stigma of hepatitis B virus (HBV) infection-A systematic review. Welcome Open Res. 2018;3:29.
Ciftci A, Jones N, Corrigan PW. Mental Health Stigma in the Muslim Community. J Muslim Mental Health. 2013;7(1):17–32.
Cohen J. Statistical power analysis for the behavioral sciences. Second edition. 12 Lawrence Erlbaum Associates Inc. Hillsdale, New Jersey. 1988;13.
Browne JL, Ventura AD, Mosely K, Speight J. Measuring Type 1 diabetes stigma: development and validation of the Type 1 Diabetes Stigma Assessment Scale (DSAS-1). Diabet Med. 2017;34(12):1773–82.
Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943–50.
Shabibi P, Mansourian M, Abedzadehzavareh M, Sayehmiri K. The status of self-care behaviors in patients with type 2 diabetes in the city of Ilam in 2014. Scie J Ilam Univ Med Scie. 2016;24(2):63–71.
Holmes-Truscott E, Ventura AD, Thuraisingam S, Pouwer F, Speight J. Psychosocial Moderators of the Impact of Diabetes Stigma: Results from the Second Diabetes MILES–Australia (MILES-2) Study. Diabetes Care. 2020;43(11):2651–9.
Gredig D, Bartelsen-Raemy A. Diabetes-related stigma affects the quality of life of people living with diabetes mellitus in S witzerland: implications for healthcare providers. Health Soc Care Commun. 2017;25(5):1620–33.
Olesen K, Cleal B, Willaing I. Discrimination and stigma among people with type 2 diabetes in the workplace: prejudice against illness or obesity? Public Health. 2020;180:100–1.
Vasli P, Eshghbaz F. Survey condition regarding self-caring of children suffering from diabetes type 1 and It’s relation with family reaction. J Mazandaran Univ Med Sci. 2009;19(69):38–44.
Khezerloo S, Feizi A. A survey of relationship between perceived self-efficacy and self-care performance in diabetic patients referring to Urmia Diabetes Center. J Urmia Nurs Midwifery Faculty. 2012;10(3):369–75.
Rajasekharan D, Kulkarni V, Unnikrishnan B, Kumar N, Holla R, Thapar R. Self care activities among patients with diabetes attending a tertiary care hospital in Mangalore Karnataka, India. Ann Med Health Sci Res. 2015;5(1):59–64.
Mahdi H, Maddah SMB, Mahammadi F. The effectiveness of self-care training on quality of life among elderlies with diabetes. Iran J Rehabil Res. 2016;2(4):32–9.
Shrivastava A, Shah N, De Sousa A, Sonavane S. Clinical consequences of stigma (suicide, non-compliance and rehospitalisation). Indian J Appl Res. 2013;3(9):410–3.
Kato A, Fujimaki Y, Fujimori S, Isogawa A, Onishi Y, Suzuki R, et al. Association between self-stigma and self-care behaviors in patients with type 2 diabetes: a cross-sectional study. BMJ Open Diabetes Res Care. 2016;4(1):1–7.
Kato A, Fujimaki Y, Fujimori S, Isogawa A, Onishi Y, Suzuki R, Ueki K, Yamauchi T, Kadowaki T, Hashimoto H. How self-stigma affects patient activation in persons with type 2 diabetes: a cross-sectional study. BMJ open. 2020;10(5):e034757.
Puhl RM, Himmelstein MS, Hateley-Browne JL, Speight J. Weight stigma and diabetes stigma in US adults with type 2 diabetes: Associations with diabetes self-care behaviors and perceptions of health care. Diabetes Res Clin Pract. 2020;168:108387.
Lee SM, Lim LC, Koh D. Stigma among workers attending a hospital specialist diabetes clinic. Occup Med. 2015;65(1):67–71.
Jaacks LM, Liu W, Ji L, Mayer-Davis EJ. Type 1 diabetes stigma in China: a call to end the devaluation of individuals living with a manageable chronic disease. Diabetes Res Clin Pract. 2015;107(2):306–7.
Kato A, Fujimaki Y, Fujimori S, Isogawa A, Onishi Y, Suzuki R, Yamauchi T, Ueki K, Kadowaki T, Hashimoto H. Psychological and behavioral patterns of stigma among patients with type 2 diabetes: a cross-sectional study. BMJ Open. 2017;7(3):e013425.
Soylar P, Kadioglu BU, Kilic K. Investigation of the barriers about insulin therapy in patients with type 2 diabetes. Niger J Clin Pract. 2020;23(1):98.
Acknowledgements
The authors of this article appreciate the Research Deputy of Islamic Azad University, Isfahan (Khorasgan) Branch, all dear participants as well as the respectable personnel of Tabriz Health Center who helped us in conducting this study.
Funding
This study was supported by the vice chancellor for research at Islamic Azad University, Isfahan (Khorasgan) Branch.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Nothing to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mahdilouy, P., Ziaeirad, M. Relationship between perceived social stigma and diabetes self-care activities in Iranian participants with type 1 diabetes. J Diabetes Metab Disord 20, 1505–1511 (2021). https://doi.org/10.1007/s40200-021-00893-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-021-00893-1